Do You Need a Follow-Up STD Test After Treatment? What Each Infection Actually Requires
Last updated: April 2025
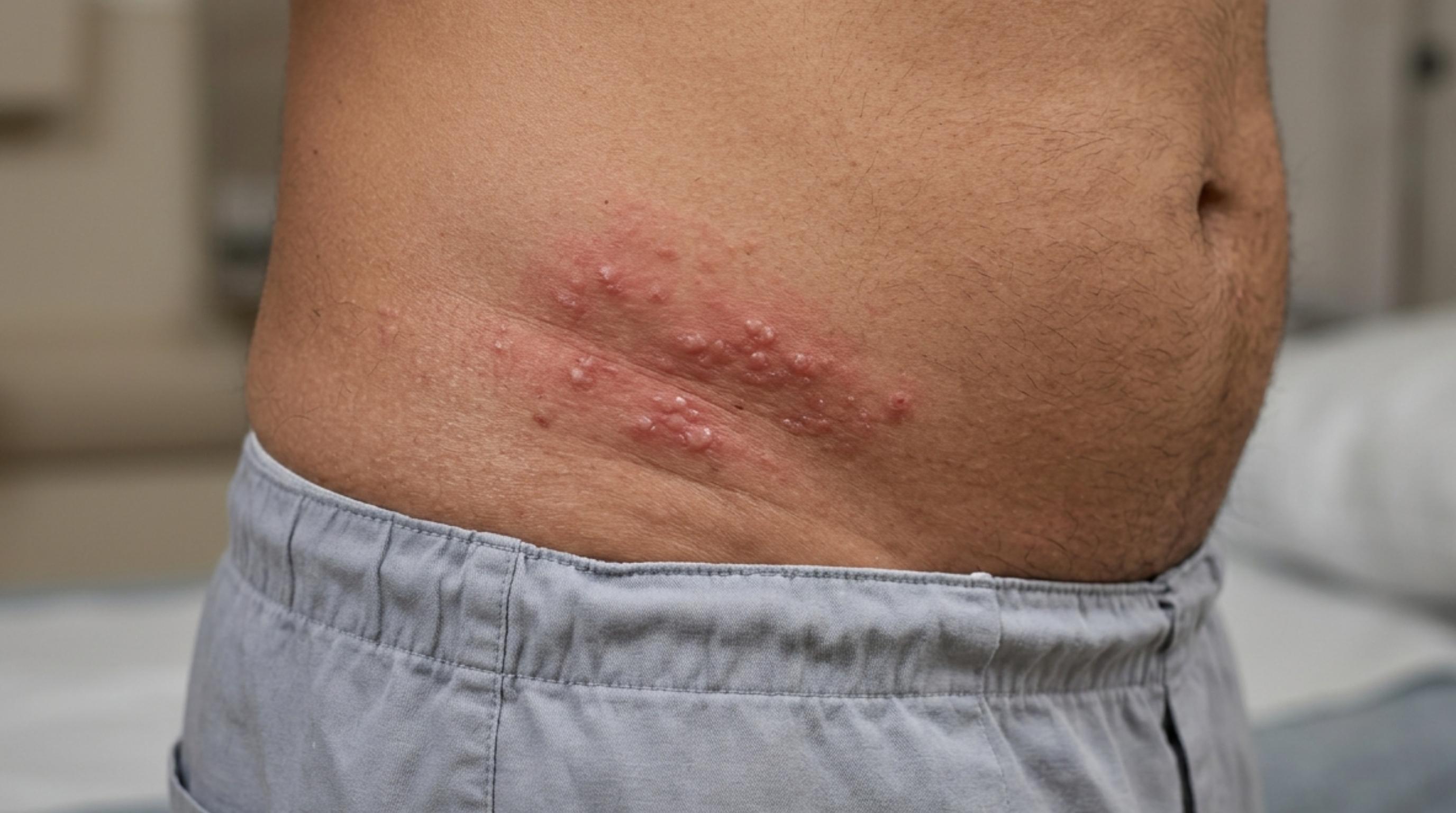
A rash that appears after a sexual encounter is one of the fastest routes to a 3 AM internet spiral. And while most rashes turn out to be something completely unrelated to HIV, the seroconversion rash is real, it's recognizable, and understanding it can help you decide whether what you're looking at warrants a test, or whether you can relax. Here's everything you actually need to know.
An HIV rash during the acute phase of infection appears as a widespread, flat or slightly raised discoloration, reddish or flushed on lighter skin tones, deep purple or brownish on darker skin. It typically spreads across the chest, back, and upper arms, and arrives roughly 2 to 4 weeks after exposure alongside fever, fatigue, swollen lymph nodes, and a sore throat. It almost never appears in isolation. No rash alone can confirm HIV, testing is the only tool that actually answers the question.
People are also reading: STD Myths and Facts: Common Misconceptions About Sexually Transmitted Infections
What Does an HIV Rash Actually Look Like, Colour, Texture, Location
The technical classification is a maculopapular exanthem: a mix of flat discoloured patches (macules) and slightly raised bumps (papules) spread across a wide area of skin. In plain terms, it looks like a diffuse reddish or purplish flush, not a cluster, not a single sore, not a blister. It covers broad areas of skin rather than concentrating in one spot, and it doesn't move or shift location the way hives do.
On fair to medium skin, the rash appears clearly red or pink, sometimes described as looking like a mild sunburn with uneven colouring. On medium to dark skin, the contrast with surrounding skin is much lower, and it presents as deeper purple or brownish discolouration that can be easy to miss in poor lighting or a quick glance. This disparity is clinically significant: according to the NIH, HIV-related skin changes are frequently overlooked in people with darker skin tones, which contributes to later diagnosis. It's not that the rash doesn't appear, it's that it's subtler and requires closer attention.
The rash is mildly itchy for some people and not itchy at all for others. It doesn't typically have the intense, unbearable itch of an allergic reaction or scabies. The skin in the affected area may feel slightly warm or tender. It spreads most commonly across the trunk, chest and back first, then to the upper arms, neck, and sometimes the face. It does not preferentially appear on the genitals, palms, or soles at the acute stage (those patterns belong to other conditions, as we'll get to).
| Feature | Detail |
|---|---|
| Appearance | Flat patches and slightly raised bumps (maculopapular); widespread, not clustered |
| Colour, fair skin | Red, pink, flushed, like uneven sunburn |
| Colour, dark skin | Deep purple or brownish; lower contrast, easier to miss |
| Primary location | Chest, back, upper arms; sometimes neck and face |
| Itching | Mild to absent, not intensely itchy |
| Timing | 2–4 weeks after exposure (not within the first few days) |
| Duration | 1–3 weeks, resolves on its own |
| Usually comes with | Fever, fatigue, sore throat, swollen lymph nodes |
| Can it confirm HIV? | No. Testing is the only confirmation |
Most Rashes After Sex Are Not HIV, Here's What They Usually Are
Before going further into what an HIV rash is, this needs to be said clearly: the vast majority of rashes that people worry might be HIV turn out to be something far more ordinary. This isn't dismissiveness, it's epidemiology. Most people who notice a rash after a sexual encounter are looking at an allergic reaction, friction irritation, heat rash, or a common viral skin condition that has nothing to do with HIV. If there were no meaningful exposure risk, a rash is almost certainly not the acute HIV presentation.
Allergic reactions and hives are probably the most frequent source of confusion. Hives appear as raised, welted patches that can spread quickly across the body and look alarming, but the behaviour is different. Individual welts from an allergic reaction typically appear and disappear within hours, shifting location across the skin. An HIV rash doesn't do that. It persists in the same areas, doesn't resolve in hours, and isn't triggered by a food, detergent, or new product. As explored in The 3 Rashes That Get Mistaken for HIV, the look-alikes are consistent and predictable, knowing them reduces a lot of unnecessary panic.
Pityriasis rosea is another extremely common misidentification. It's a benign viral rash that starts with one large "herald patch" and then spreads in a Christmas tree pattern across the trunk, exactly the location people associate with an HIV rash, and it looks similar in colour. The distinction is that pityriasis rosea is scaly rather than smooth, tends to follow that distinctive trunk pattern, and doesn't come with systemic flu-like illness. It also has nothing to do with sexual transmission. Seborrheic dermatitis, eczema, heat rash, and contact dermatitis from new products round out the list of rashes that commonly land someone in an anxious search.
The rash alone doesn't define risk. Exposure does. If the encounter was low risk or protected, the probability that any rash is HIV-related is very low. What changes the calculation is the combination: rash plus significant exposure risk plus flu-like illness appearing 2 to 4 weeks later. That constellation is worth taking seriously. A rash with no other symptoms and no clear exposure risk usually isn't.
People are also reading: Scared to Get Tested for an STD? Here's How to Actually Pull Through
What Else Comes With the HIV Rash, Acute Retroviral Syndrome
The reason the HIV seroconversion rash is called part of "acute retroviral syndrome" (ARS) is that it's almost always one symptom among several, not a standalone sign. The body's response to a new HIV infection looks remarkably like a bad flu or a bout of mono. In fact, it's so similar to other viral illnesses that many people assume they've caught a seasonal bug, feel terrible for a week or two, recover, and never connect what happened to HIV. That's one of the reasons the infection can go undetected for so long.
The typical ARS picture includes: fever (often significant, 38°C / 100.4°F or higher), profound fatigue, sore throat, swollen lymph nodes in the neck, armpits, or groin, muscle aches, and sometimes mouth ulcers or diarrhoea. The rash tends to appear a few days into this illness and resolve alongside it. According to the CDC, in 2023 over 39,000 people were newly diagnosed with HIV in the United States, and a significant portion had been living with the infection, unknowingly, for years. Missing the acute phase is extremely common. For a deeper look at what the first 30 days of HIV infection feel like, Acute HIV Symptoms: What to Expect in the First 30 Days covers the full timeline in detail.
If a rash appears completely on its own, no fever, no fatigue, no swollen glands, nothing, the probability that it's the HIV seroconversion rash drops significantly. That doesn't mean testing isn't worthwhile if there was a real exposure; it just means the rash alone is a weak signal compared to the full clinical picture. The presence of multiple ARS symptoms alongside the rash is what makes the picture clinically meaningful.
When to Test for HIV After a Possible Exposure
This is the section that actually matters most, and the one people most often get wrong. The instinct is to test immediately after noticing a rash or a worrying exposure. But testing too early produces a false negative, not because the test is faulty, but because the body hasn't yet produced enough antibodies for the test to detect. A negative result before the window period closes doesn't mean you're clear, it means you tested too soon.
For HIV, the reliable testing window opens at 6 weeks after exposure. At that point, the HIV 1&2 At-Home Rapid Test Kit (99.7% accuracy) gives a strongly reliable result from a simple finger-prick blood sample, no clinic, no lab, results in minutes. A negative at 6 weeks is highly reassuring. Retesting at 12 weeks gives you confirmed certainty and closes the window definitively. The 6-week result is your first real data point; 12 weeks is your final answer.
If the potential exposure also carries risk for other infections, which is common, since the same encounters that raise HIV concern often involve syphilis, herpes, chlamydia, or gonorrhea risk simultaneously, testing across a broader panel makes sense. The 7-in-1 Complete STD Home Test Kit (98.5% accuracy) covers HIV, herpes HSV-2, chlamydia, gonorrhea, syphilis, hepatitis B, and hepatitis C in one session. For everything including herpes HSV-1, the Complete 8-in-1 (99% accuracy) is the most comprehensive at-home option. For more on how these tests detect HIV specifically, How Do At-Home STD Test Kits Detect HIV? explains the antibody detection process in plain terms.
| Infection | Test From | Notes |
|---|---|---|
| HIV | 6 weeks after exposure | Retest at 12 weeks for confirmed certainty |
| Herpes HSV-1 & HSV-2 | 6 weeks after exposure | Antibody-based; earlier testing may miss it |
| Syphilis | 6 weeks after exposure | Rash appears at secondary stage, 4–10 weeks post-infection |
| Chlamydia | 14 days after exposure | Often no symptoms, worth testing even without them |
| Gonorrhea | 3 weeks after exposure | Can present with discharge; increasingly drug-resistant |
| Hepatitis B | 6 weeks after exposure | Vaccine-preventable; test if unvaccinated |
| Hepatitis C | 8–11 weeks after exposure | Longest window, patience required for accurate result |
Check Your STD Status in Minutes
Test at Home with RemediumHIV Rapid Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $33.99 $49.00
HIV Rash vs. Other STI-Related Skin Changes, How to Tell the Difference
More than one STI causes visible skin changes, and people with a recent high-risk exposure sometimes aren't sure which infection might be responsible for what they're seeing. The presentations are actually quite different, the problem is that photos online rarely show the full clinical context that helps tell them apart.
A syphilis rash, which appears during secondary syphilis (untreated primary infection), is one of the most distinctive: copper-coloured spots on the palms of the hands and soles of the feet, appearing 4 to 10 weeks after the initial sore. That palms-and-soles location is almost diagnostic on its own, it's uncommon with most other rashes and very characteristic of syphilis. The HIV seroconversion rash doesn't appear on palms or soles at the acute stage. Both infections can coexist, which is why co-infection testing is worth considering after any high-risk exposure, Co-Infection Risks: The Hidden Link Between STDs and HIV covers this relationship in detail.
Herpes outbreaks, whether oral HSV-1 or genital HSV-2, are localized clusters of blisters or sores, most commonly on the genitals, inner thighs, buttocks, or around the mouth. They are not a widespread body rash. They blister, crust, and resolve in a way that looks nothing like the diffuse maculopapular spread of an HIV seroconversion rash. However, herpes and HIV interact in an important way: having herpes increases susceptibility to HIV, and having HIV makes herpes outbreaks more frequent and more severe. How Ignoring Herpes Treatment Can Increase HIV Risk and Herpes vs. HIV: What Itches, What Stays, What You Need to Test For both break down that connection clearly.
The practical takeaway: the location and behaviour of a rash matter as much as its appearance. A rash on the palms and soles points toward syphilis. Blisters in one location point toward herpes. A widespread, flat, flu-associated body rash appearing 2 to 4 weeks after exposure points toward HIV seroconversion. None of these are confirmed by appearance alone, but the patterns are meaningfully different.
Rashes That Appear Later, When HIV Affects the Immune System Over Time
The seroconversion rash is not the only skin story in HIV. People living with HIV who aren't on effective treatment, or whose viral load is poorly controlled, can develop a range of skin conditions caused by the immune system's progressive weakening. These are secondary presentations, not acute infection signs, and they look completely different from the seroconversion rash.
Herpes zoster (shingles) is significantly more common and more severe in people with compromised immunity. It presents as a painful blistering rash following a single nerve pathway, a stripe along one side of the chest, back, or face. It doesn't spread diffusely; it stays in that nerve distribution. Molluscum contagiosum, normally a minor self-limiting viral infection, can become extensive and hard to control when the immune system can't suppress it. Seborrheic dermatitis, red, flaky patches around the nose, eyebrows, and scalp, is both extremely common generally and disproportionately severe in people with HIV. The Hidden Dangers of Untreated HIV covers the full cascade of what happens to the body without treatment, including skin complications.
Drug reactions are another category entirely. Some antiretroviral medications can cause rashes, usually mild and self-limiting, but occasionally more serious. The rare but severe Stevens-Johnson syndrome involves a rapidly spreading, blistering rash with fever and pain that requires immediate medical attention. Anyone on HIV medications who develops a rapidly progressing rash with blistering, fever, or difficulty breathing should seek emergency care immediately, and should never stop medication without medical guidance.
People are also reading: At-Home STD Testing: How It Works, How Accurate It Is, and What to Do With the Results
What to Do If You Think You Have an HIV Rash
You've noticed something on your skin, you're aware of a recent potential exposure, and the timeline fits. Here's what actually matters right now, in order of priority.
If it has been fewer than 72 hours since a high-risk exposure, contact a healthcare provider about PEP (post-exposure prophylaxis), a short course of medication that can prevent HIV from establishing infection if started quickly enough. The 72-hour window is hard: after that, PEP is no longer effective. If you're within the window, that's the thing to focus on before anything else. How PrEP and PEP Are Changing STD Prevention has more on how these medications work.
Once the PEP window has passed, the plan is straightforward: wait for the 6-week testing window, then test. Use the time between now and then wisely, avoid further high-risk exposures, and if you have significant flu-like symptoms alongside the rash, let a healthcare provider know. Conditions like mono produce a very similar picture and deserve direct evaluation. At the 6-week mark, the HIV 1&2 Rapid Test Kit gives you a 99.7% accurate result at home in minutes. If the result is negative, retest at 12 weeks to close the window definitively. Testing is the fastest way to stop the guessing game, and the only move that actually ends it.
For anyone thinking about their ongoing testing routine, not just this one exposure, Testing for HIV at Home: Benefits, Accuracy and Tips and Why Regular STD Testing Is So Important are worth reading. Regular testing removes the need for these anxiety spirals to begin with, and it takes about 15 minutes.
FAQs
1. How does an HIV rash feel?
Some people find it mildly itchy, while others don't find it itchy at all. It's not the intense itch that comes with an allergic reaction. The skin in the area that hurts may feel a little warm or sore. The rash itself usually doesn't hurt too much, but the flu-like symptoms that come with it, like fever, fatigue, and sore throat, are what people really feel.
2. Is it possible to have an HIV rash without any other signs?
Possible, but not very likely. The rash that comes with seroconversion is almost always part of a bigger acute illness, like fever, fatigue, swollen lymph nodes, and a sore throat. If a rash shows up with no other symptoms and there was no significant high-risk exposure, it's statistically much more likely that it's something else. That being said, testing is the only way to know for sure if someone has HIV or not; symptoms alone are not enough to make a diagnosis.
3. How soon after being exposed does an HIV rash show up?
The usual time frame is 2 to 4 weeks. If you get a rash within the first few days of being exposed, it's almost certainly not HIV. The viral load hasn't had time to rise high enough to cause the immune response that leads to the seroconversion rash. Rashes that happen early on (within the first week) are almost always caused by something else, like contact irritation, an allergic reaction, or timing that happens to be the same as an unrelated condition.
4. Does an HIV rash go away by itself?
Yes. Without treatment, the seroconversion rash usually goes away on its own in 1 to 3 weeks. The virus hasn't gone away; it just means that the acute phase is over and the infection has moved on to the next stage. HIV keeps getting worse even when symptoms go away if you don't get treatment.
5. Does an HIV rash look different on darker skin?
Yes, and it's an important point for doctors. On darker skin, the rash looks more like a deep purple or brownish discoloration than the bright red or pink that is seen on lighter skin. It's easier to miss or ignore because it doesn't stand out as much against the skin around it. This makes it harder to diagnose people with darker skin, which is one reason why HIV symptoms are sometimes not noticed until later stages.
6. Can someone with HIV not get a rash?
Of course. About 40–80% of people may have some form of acute retroviral syndrome, which may or may not include a rash. A lot of people get through the acute phase without any symptoms or with symptoms that aren't bad enough to worry about. This is exactly why you should get tested regularly, even if you haven't had any symptoms. The Silent Virus: Why HIV Symptoms Get Missed for Years goes into great detail about this.
7. Can skin contact spread an HIV rash?
No. The rash is a sign of the virus, not a separate infection. HIV can be spread through certain body fluids, such as blood, semen, rectal and vaginal fluids, and breast milk. Touching the rash on the skin does not spread HIV. The ways the disease spreads are the same whether or not there is a rash.
8. What should I do if I get a rash after I start taking HIV medicine?
Let your doctor know right away. Most rashes that people get when they start taking antiretroviral drugs are mild and easy to treat. If you notice that something is getting worse quickly, like blisters, trouble breathing, or dizziness, you need to see a doctor right away. Don't stop taking HIV medicine without talking to a doctor first, even if you get a rash.
9. How soon after being exposed can I be sure that I have HIV?
Six weeks is the minimum time that home rapid antibody tests are reliable. If you test before that, you might get a false negative, which means you might be infected but the test can't find it yet. A negative result at 6 weeks is very reassuring, and a negative result at 12 weeks is final. Some 4th-generation antigen/antibody tests done at a clinic can find infections a little earlier, but for tests done at home, 6 weeks is the time to plan around.
10. Is it possible that a rash after sex is not HIV?
Most likely, especially if the exposure was less risky or protected. Allergic reactions, friction or heat rash, pityriasis rosea, eczema flares, or seborrheic dermatitis are the most common causes, and none of these are related to HIV. The full breakdown is in "The 3 Rashes That Get Mistaken for HIV." Testing at the right time clears up the doubt that comparing symptoms can't.
Get Tested, Clarity Beats Guessing Every Time
If a rash has sent you searching, the next productive move isn't more Googling, it's planning your test for the 6-week mark and stopping the spiral now. At-home rapid testing has made this straightforward: no waiting room, no lab visit, no conversation you'd rather skip. A result in minutes, at home, on your timeline.
For HIV specifically, the HIV 1&2 At-Home Rapid Test Kit (99.7% accuracy) delivers a result from a finger-prick blood sample in minutes. If you want to cover the full picture from a single encounter, HIV, herpes, chlamydia, gonorrhea, syphilis, hepatitis B, and hepatitis C, the 7-in-1 Complete STD Home Test Kit (98.5% accuracy) handles all of it in one session. For the most comprehensive coverage including both herpes types, the Complete 8-in-1 (99% accuracy) is the strongest single option available. Visit STD Rapid Test Kits to order, and replace the uncertainty with an actual answer.
People are also reading: The 3 Rashes That Get Mistaken for HIV (And What They Really Are)
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. National Institutes of Health, HIV and Rash
2. CDC, HIV Diagnoses, Deaths, and Prevalence: 2025 Update
3. Medical News Today, HIV Rash: Causes, Symptoms, and Treatment
4. The Well by Northwell, HIV Rash: Understanding the Risk
5. WebMD, HIV Rash: Types, Related Symptoms, and Treatment
6. Ada Health, HIV: Can It Cause Skin Rashes?
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2025
This article is for informational purposes and does not replace medical advice.