Can You Get Tested for STDs While on PrEP? The Truth About Results and Timing
Last updated: April 2026
The most common signs of chlamydia include unusual discharge from the vagina or penis, a burning sensation when urinating, pelvic or lower abdominal pain in women, testicular discomfort in men, and bleeding after sex or between periods. Throat and rectal infections are almost always completely silent. And in the majority of all cases, roughly 80% in women and 50% in men, chlamydia produces no symptoms of any kind. The only way to know whether you have it is to test.
This article is the complete picture: what chlamydia actually feels like when symptoms do appear, what it looks like when they don't, how symptoms differ between men and women, where in the body infections can hide, and exactly when testing gives you a reliable answer. If you're trying to figure out whether what you're experiencing could be chlamydia, or whether the absence of symptoms means you're safe, this is the article that answers that.
The more important fact underpinning all of it: according to the CDC, chlamydia frequently produces no symptoms at all, which is exactly why over 1.5 million cases were still reported in 2024 even as testing has improved. Most infections aren't caught because someone felt sick. They're caught because someone tested.
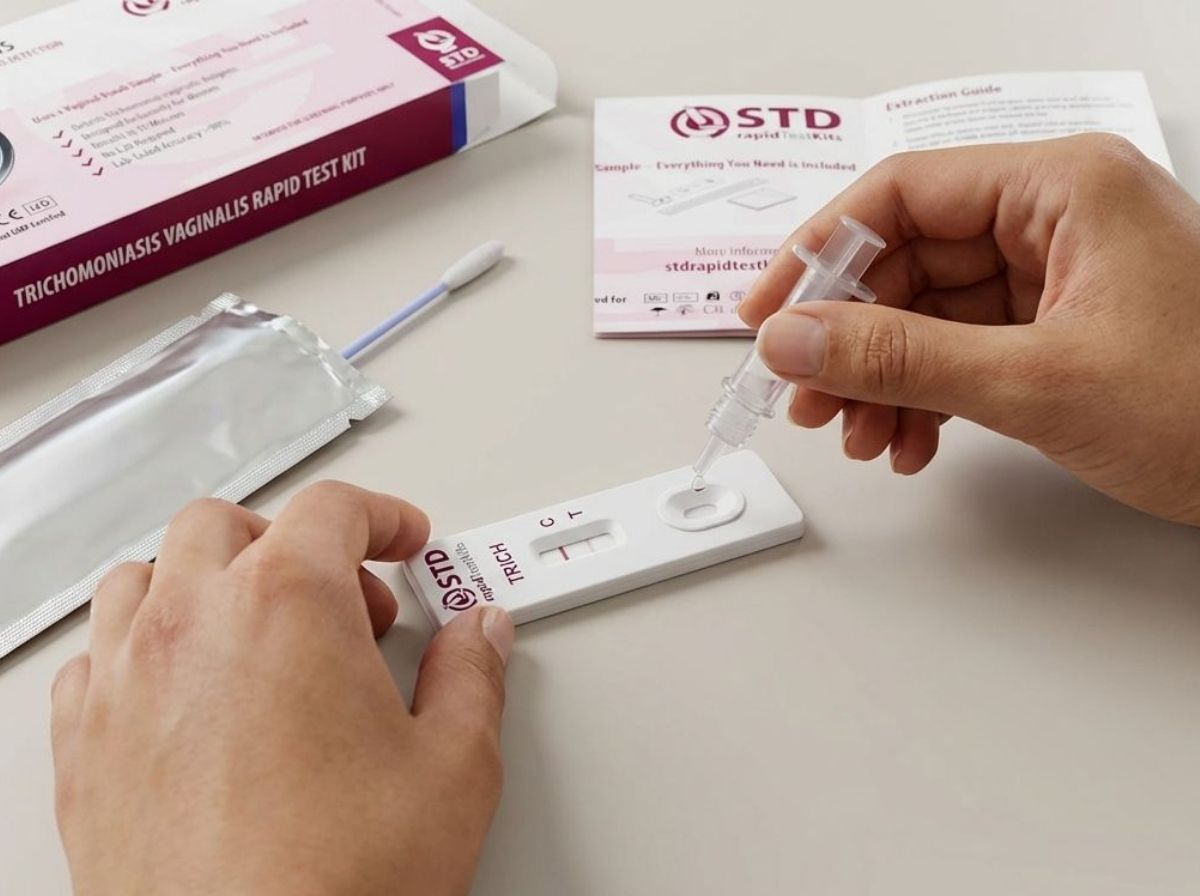
People are also reading: At-Home STD Testing: How It Works, How Accurate It Is, and What to Do With the Results
Does Chlamydia Always Have Symptoms? Why Most Infections Stay Silent
Imagine carrying an infection for months, feeling completely fine, and unknowingly passing it to multiple partners. That's not a worst-case scenario with chlamydia, it's the statistical norm. The biology is what makes this happen. Chlamydia trachomatis, the bacterium responsible, is an intracellular pathogen, meaning it lives and replicates inside your body's own cells. That's the reason it's so good at staying invisible: it doesn't trigger the kind of immediate inflammatory response that makes you feel sick. It just quietly replicates while you go about your life.
The numbers tell the story clearly. Research published via the NIH's InformedHealth resource puts the asymptomatic rate at approximately 80% in women and 50% in men. That means even in the group where symptoms are more likely, men, half of all infections still produce nothing noticeable. For women, it's closer to four out of five infections that stay completely silent. If you're waiting to feel something before testing, the odds are not in your favor. For a deeper look at exactly how long an infection can go undetected, see How Long Can You Have Chlamydia Without Knowing?
This is why the CDC has recommended routine chlamydia screening for all sexually active people under 25, and for older individuals with new or multiple partners, not because symptoms should prompt testing, but because symptom-based testing catches only a fraction of infections. The CDC's provisional 2024 surveillance data shows chlamydia cases declined 8% compared to 2023, reflecting two consecutive years of improvement. But with over 1.5 million reported cases still recorded that year, and an unknown number of unreported silent infections, the burden remains significant. The decline in reported cases doesn't mean the risk has dropped; it means more people are testing before symptoms appear.
The takeaway is uncomfortable but important: if you're sexually active with new or multiple partners and you haven't tested recently, the absence of symptoms isn't reassurance. It's just silence. And chlamydia is very good at silence.
What Are the Symptoms of Chlamydia in Women?
| Symptom | What's Actually Happening | How Often It Appears |
|---|---|---|
| Unusual vaginal discharge | Cervical inflammation triggers increased mucus production | Common, but not universal |
| Burning or frequent urination | Urethral infection causes irritation during urination | Common, often mistaken for UTI |
| Pelvic or lower abdominal pain | Infection ascending toward the uterus or fallopian tubes | Less common; warrants urgent attention |
| Bleeding after sex or between periods | Cervical inflammation makes tissue more fragile | Moderate, easy to rationalize |
| Pain during sex | Inflammation at the cervix or deeper pelvic structures | Less common in early infection |
| No symptoms at all | Intracellular replication without triggering full immune response | Most common, approximately 80% of cases |
When symptoms do appear in women, they tend to be easy to dismiss or misattribute. The most common is an unusual vaginal discharge, cloudy, white, pale yellow, or slightly watery, that may look like a minor change from your normal pattern rather than a clear warning sign. You might notice it feels slightly thicker or has a faint, unfamiliar smell. Or the change might be subtle enough that you second-guess whether anything is actually different at all. That ambiguity is part of why chlamydia goes undetected for so long in so many people.
Burning or increased frequency when urinating is another common presentation. Because chlamydia infects the urethra as well as the cervix, urinary symptoms are well within its range, which means it's regularly confused with UTIs, especially in younger women. Someone treats what seems like a UTI, the urinary symptoms improve, and the underlying infection stays in place. Pain or bleeding during or after sex is another signal worth paying attention to. Chlamydia can cause cervical inflammation that makes the tissue more fragile and sensitive, which produces spotting or discomfort that feels like a rough encounter but isn't.
Lower abdominal pain or pelvic discomfort can indicate the infection has moved beyond the cervix and begun ascending into the reproductive tract. This matters because pelvic inflammatory disease, the complication that causes the most serious long-term damage, including fallopian tube scarring and infertility, often begins with symptoms that feel like a mild ache rather than an emergency. Irregular bleeding between periods, particularly after sex, should prompt testing rather than waiting to see if it resolves.
The most important thing to understand about chlamydia symptoms in women is that even when they're present, they rarely feel dramatic. The infection that causes no symptoms and the infection that causes PID and long-term fertility damage are the same infection, the difference is time and whether it gets treated. A subtle discharge that's easy to ignore at week two becomes a risk for serious complications at week twelve if it goes untreated. That's not meant to create panic, but to explain why testing matters independently of how you feel.
What Are the Symptoms of Chlamydia in Men?
Men tend to be more likely to notice chlamydia symptoms than women, but "more likely" here is relative. Roughly half of male chlamydia infections are still completely asymptomatic. When symptoms do appear, the most recognizable is urethral discharge, fluid at the tip of the penis that's typically clear, cloudy, or slightly white or yellow. It's often subtle: a small amount that shows up in the morning or dries as a residue around the urethral opening. Because discharge isn't something men normally experience, even a small amount is clinically significant if it appears in the weeks following potential exposure.
A burning sensation during urination is another frequent symptom, caused by bacterial inflammation of the urethra. Testicular pain or swelling, typically one-sided, is a less common but more serious presentation. This can indicate the infection has spread from the urethra to the epididymis, the coiled tube running along the back of each testicle. Epididymitis is uncomfortable, and, if untreated, it carries a real risk of affecting fertility. If you notice testicular tenderness that wasn't there before, that's a prompt to test and see a provider, not a symptom to monitor at home for a week. Men who experience burning with no visible discharge at all may find it useful to read Burning, No Discharge, Still Chlamydia? The Signs Bi Men Can't Ignore, which covers that specific presentation in detail.
Men with rectal chlamydia, typically from receptive anal sex, may experience rectal discomfort, discharge from the rectum, or bleeding. Often there's nothing noticeable at all, which is why rectal site testing matters for MSM and any person who has receptive anal sex. Standard urine-based testing will miss a rectal infection entirely. The infection lives in the rectum, and only a swab of that site will detect it.
| Infection Site | Symptoms | What to Watch For |
|---|---|---|
| Urethra | Discharge (clear, cloudy, or white/yellow), burning urination | Often most noticeable in the morning |
| Epididymis | Testicular pain or swelling, usually one side | Warrants in-person evaluation, risk of fertility impact |
| Rectum | Rectal pain, discharge, bleeding, or no symptoms | Missed entirely by urine tests, requires swab |
| Throat | Mild sore throat or no symptoms | Almost always asymptomatic, missed without throat swab |
| No specific site (systemic) | No symptoms, but infection present and transmissible | Routine testing is the only way to catch this |
Can You Get Chlamydia in the Throat, Eyes, or Rectum?
Most people think of chlamydia as a genital infection. But the bacterium infects mucous membranes, and mucous membranes exist in more places than just the genitals. The throat, the rectum, and the eyes can all carry active chlamydia infections. In most of these locations, the infection produces no symptoms whatsoever, which makes them among the most consistently missed presentations in routine sexual health care.
Throat chlamydia typically develops after oral sex involving an infected partner. The overwhelming majority of throat infections are completely asymptomatic, if there are symptoms at all, they tend to be a mild sore throat indistinguishable from a minor cold or post-nasal drip. There's no rash, no obvious lesion, nothing that would push someone to make an appointment. Standard STI panels don't include throat swabs unless you specifically request them or your provider adds them. This gap means throat infections are regularly transmitted without anyone knowing they're there.
Rectal chlamydia follows the same pattern. Receptive anal sex is the primary route of infection, but rectal chlamydia can occasionally develop through the spread of genital infection in women without anal sex having occurred. Symptoms, when present, can include rectal discomfort, bleeding, or a mucus-like discharge, but again, silence is more common than symptoms. Urine testing misses rectal infections entirely. Only a rectal swab detects infection at that site.
Eye chlamydia, chlamydial conjunctivitis, is less common in adults but can occur when infected genital secretions come into contact with the eye, either directly or via contaminated hands. Symptoms include redness, irritation, discharge, and swelling of the eyelid. It looks very similar to other forms of conjunctivitis and is frequently misdiagnosed. In newborns, chlamydial conjunctivitis is a more significant concern, as the infection can be transmitted during childbirth from an untreated mother.

People are also reading: Scared to Get Tested for an STD? Here's How to Actually Pull Through
Is It Chlamydia or Something Else? How to Tell the Difference
Chlamydia doesn't have a look that's exclusive to it. The symptoms it produces, discharge, burning, pelvic discomfort, irritation, overlap significantly with several other conditions, and that's one of the main reasons visual or symptom-based self-diagnosis doesn't work. You can't tell chlamydia from a yeast infection, a UTI, gonorrhea, or bacterial vaginosis by how they feel or what they look like. This isn't a failure on your part. It's just biology: different conditions affect the same tissues in overlapping ways, and the body produces similar inflammatory responses to different triggers.
Gonorrhea is the closest clinical look-alike. Both infections target the same sites, produce similar discharge, and can cause identical urinary symptoms. Even clinicians can't distinguish them reliably without testing, which is why combination testing for both infections is a common recommendation when either is suspected. The Chlamydia & Gonorrhea 2-in-1 test exists precisely because co-infection rates run at approximately 30–40% according to CDC data, meaning if you have one, the probability of having the other simultaneously is substantial. Testing for only one while the other goes undetected is one of the most common reasons people think they've been re-infected when they actually weren't fully treated in the first place.
Bacterial vaginosis can produce cloudy or unusual discharge with an unfamiliar smell, easily mistaken for early chlamydia. Yeast infections produce thick, white, cottage cheese-like discharge with significant itching, generally more distinct, but not always. UTIs and urethral chlamydia both produce burning during urination; the distinction is that UTIs typically also cause increased urgency and frequency of urination and may produce fever, while chlamydial urethritis often doesn't. For a full side-by-side breakdown of how to distinguish chlamydia from a UTI specifically, see Burning, Peeing, or Nothing at All: UTI vs Chlamydia Symptoms in Women. Herpes produces clusters of sores or blisters, which chlamydia does not, though the soreness and irritation of herpes before visible lesions form can sometimes be confused with early genital discomfort from other STIs.
| Condition | Discharge | Urinary Symptoms | Other Distinguishing Features |
|---|---|---|---|
| Chlamydia | Cloudy, white, pale yellow, watery, or none | Burning, mild, or none | Often completely asymptomatic; may cause pelvic pain if advancing |
| Gonorrhea | Thicker, more noticeable, yellow-green | Burning, often more pronounced | Frequently co-occurs with chlamydia; clinically indistinguishable without testing |
| Bacterial Vaginosis | Gray-white, watery, fishy smell, especially after sex | Usually none | Not sexually transmitted; no partner treatment required |
| Yeast Infection | Thick, white, clumpy (cottage cheese texture) | Mild burning possible | Intense external itching; redness; not sexually transmitted |
| UTI | Usually none | Strong burning, increased urgency, frequency | May cause fever, cloudy urine; bacteria in bladder rather than urethra/cervix |
| Herpes (HSV) | Usually none (unless secondary) | Burning if urethra affected | Blisters, sores, or ulcers, visible lesions distinguish it from chlamydia |
The practical takeaway: if you're trying to figure out which of these conditions you might have, you're already at the point where testing is the faster and more accurate route than symptom-matching. A test gives you a definitive answer. Symptom comparison gives you a narrowed list of possibilities and a lot of continued uncertainty.
How Soon Do Chlamydia Symptoms Appear After Exposure?
Most people want to know: how long until I'd feel something if I had it? The honest answer is seven to twenty-one days, if symptoms appear at all. That's the general incubation window, the period between exposure and when the bacterial load has replicated enough to trigger a visible inflammatory response. Some people notice changes earlier, around the one-week mark. Others don't see anything until the third week. And a significant portion of people never develop symptoms that would prompt them to investigate, even as the infection continues to replicate.
What this means practically is that you can't use the absence of symptoms at day three, or day seven, or even day fourteen to reassure yourself you're clear. The incubation window and the testing window are related but different things. Symptoms, when they appear, reflect your immune system beginning to respond to the infection. The testing window reflects when there's enough bacterial genetic material in your sample for a NAAT to reliably detect it, which is 14 days after exposure. These two windows can diverge: someone might start noticing mild symptoms at day ten but still get an unreliable test result at that point, because the concentration of bacterial DNA in their sample hasn't reached the threshold for confident detection. If you've already tested before that window and got a negative, Tested Too Early for Chlamydia? Here's the Timing That Actually Works explains exactly what that result means and when to retest.
| Days After Exposure | Symptom Status | Testing Reliability |
|---|---|---|
| 1–6 days | Almost certainly none, too early for immune response | Not reliable, high false-negative risk |
| 7–13 days | Possible early symptoms in some people | Possible detection, but not fully reliable |
| 14+ days | Symptoms may be present or absent, doesn't change test accuracy | Most accurate window, recommended test point |
| Ongoing (weeks to months) | Many people remain fully asymptomatic throughout | Testing remains accurate, delayed testing still beats no testing |
Testing at 14 days gives you the most accurate result. Testing at day three or five because anxiety has spiked is understandable, but the result doesn't actually tell you what you need to know. A negative result before the 14-day window isn't clearance; it's an inconclusive test at an inconclusive time. If that's where you are, the correct move is to retest in two weeks.
Check Your STD Status in Minutes
Test at Home with RemediumChlamydia Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $33.99 $49.00
How to Test for Chlamydia at Home, and When to Do It
If you've been reading this and mentally running through a recent exposure, this is the section that moves you from uncertainty to an actual answer. Testing for chlamydia doesn't require a clinic visit, a doctor's appointment, or any of the logistics that make people delay. An at-home rapid test gives you a real result from your own bathroom, and the technology behind it is the same NAAT method that clinics use; it detects the bacteria's DNA directly, which is why it's accurate rather than suggestive.
The Chlamydia At-Home Rapid Test Kit (99.7% accuracy) works for both men and women, requires a simple urine sample, and delivers results in minutes. The 14-day rule applies regardless of whether you have symptoms: test at 14 days after exposure for a result you can actually rely on. Testing earlier is the most common reason people get false negatives and spend additional weeks in unnecessary anxiety, convinced they're clear when the test was just too early to say.
Because co-infection with gonorrhea is common, the CDC puts concurrent infection rates at around 30–40%, testing for both at the same time is the smarter move when either is a concern. The Chlamydia & Gonorrhea 2-in-1 At-Home Rapid Test Kit (98% accuracy) covers both infections in one test. If you've had a recent exposure and you're not sure what you might have been exposed to, the Chlamydia, Gonorrhea & Syphilis 3-in-1 (99.5% accuracy) adds syphilis to the panel, a bacterium that's been rising steadily in the US and shares some transmission routes with chlamydia.
A positive result means you have the infection and need treatment, which is straightforward, effective, and doesn't require panic. A negative result at 14 days or later means the infection is not present. Peace of mind is one test away, and testing is the only thing that actually stops the guessing game. If you want to understand exactly what each line on your rapid test result means, Chlamydia Rapid Test Instructions: What Each Line Really Means walks through it clearly.
What Happens If Chlamydia Goes Untreated?
The reason this matters beyond the discomfort of symptoms is what untreated chlamydia does over time. The infection doesn't simply plateau and stay contained. Left without treatment, it can ascend through the reproductive tract in women, causing pelvic inflammatory disease. PID is the condition that causes scarring of the fallopian tubes, and it's that scarring that creates lasting fertility complications, including difficulty conceiving and elevated risk of ectopic pregnancy. The damage from PID can occur even when chlamydia was never noticeable in the first place, because PID itself can be silent in its early stages.
In men, untreated chlamydia can progress to epididymitis, inflammation of the coiled tube attached to each testicle, which causes testicular pain and swelling and carries a risk, in serious cases, of affecting sperm function and fertility. Prostatitis is another possible complication, causing discomfort and urinary symptoms. Reactive arthritis, joint inflammation triggered by the body's immune response to the infection, is a less common but real consequence, typically developing in the weeks after the primary infection.
Beyond reproductive health, untreated chlamydia can increase susceptibility to HIV. The inflammation caused by chlamydia creates a more favorable environment for HIV transmission, both in terms of receiving and transmitting the virus. This isn't hypothetical; the CDC explicitly notes this connection. It's one of the reasons that STI control is considered part of the HIV prevention strategy.
The straightforward part is that chlamydia is bacterial, and bacterial infections respond to antibiotics. Treatment is effective. The window where treatment prevents complications is wide, but it's not unlimited. The longer an infection goes untreated, the greater the cumulative risk of progression. Testing catches it before the timeline becomes medically significant. That's the entire argument for regular testing in one sentence.
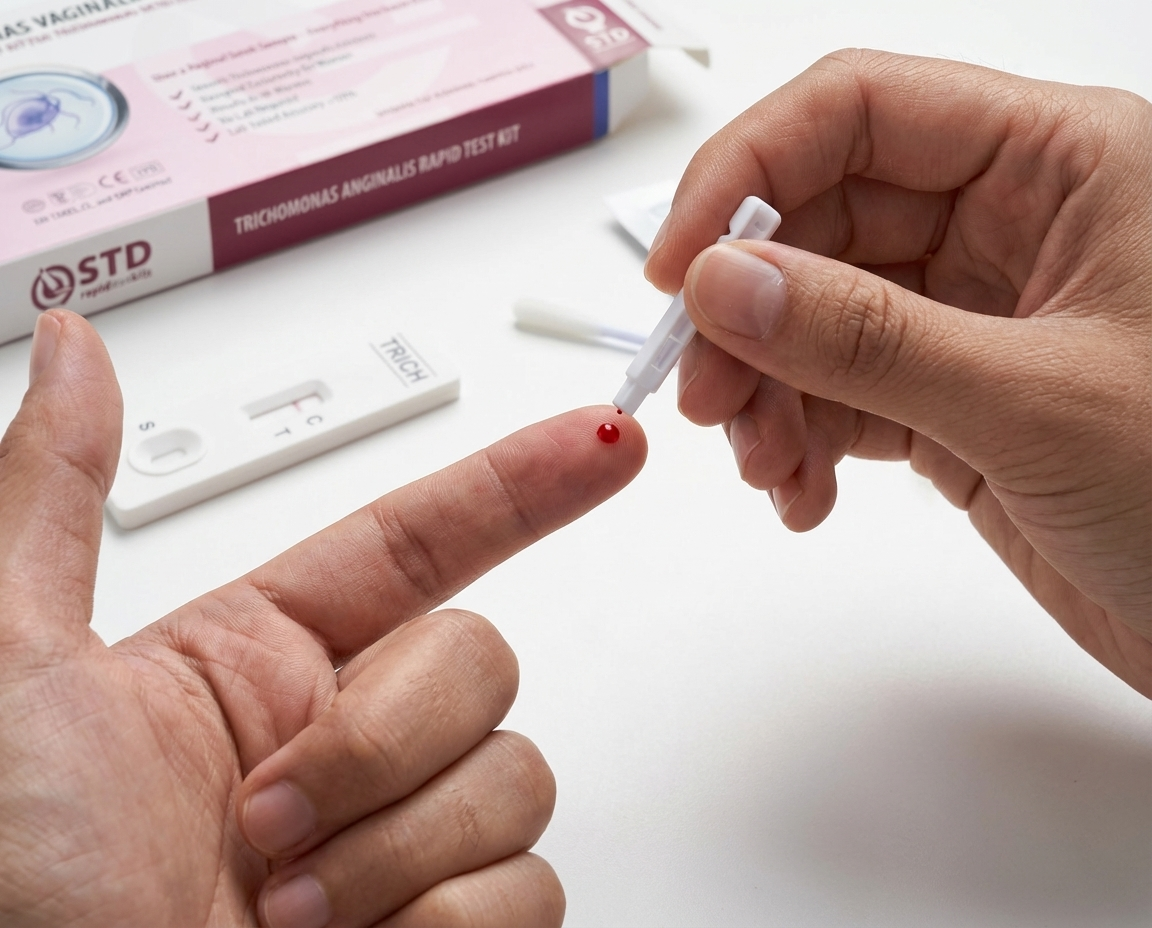
People are also reading: STD Myths and Facts: Common Misconceptions About Sexually Transmitted Infections
What Are the Symptoms of Chlamydia During Pregnancy?
Pregnancy doesn't change the basic biology of chlamydia; the infection behaves the same way, with the same tendency toward silence and the same clinical presentations when symptoms appear. What changes is the stakes. Untreated chlamydia during pregnancy carries real risks for both the pregnant person and the baby, which is why routine chlamydia screening is a standard part of prenatal care in the US for all pregnant women under 25 and those at increased risk at any age.
The symptoms of chlamydia during pregnancy are identical to those outside of it: unusual vaginal discharge, burning or discomfort when urinating, pelvic pain, or bleeding after sex. The catch, the same catch that applies throughout, is that the majority of infections are completely asymptomatic. A pregnant person can carry active chlamydia from the first trimester through delivery without ever feeling anything that would suggest infection. This is precisely why symptom-based detection during pregnancy is unreliable, and why the screening recommendation exists independently of how someone feels.
The most significant risk is transmission during delivery. A baby born vaginally to a parent with active chlamydia is exposed to the bacteria at the cervix during birth. This can result in two well-documented complications: chlamydial conjunctivitis, a serious eye infection in the newborn, typically appearing within the first two weeks of life, and neonatal chlamydial pneumonia, which develops several weeks after birth and can cause persistent coughing and breathing difficulties. Both are entirely preventable when the infection is identified and treated before delivery, which is the direct argument for prenatal screening.
Beyond transmission risk, chlamydia during pregnancy has been associated in some studies with preterm labor, premature rupture of membranes, and low birth weight, though the strength of this evidence varies and the mechanism isn't fully established. What is established is that untreated chlamydia increases the risk of postpartum complications, including endometritis, an infection of the uterine lining that can develop in the weeks following delivery.
If you're pregnant and haven't been screened, your prenatal provider is the right starting point. First-trimester screening is standard. If you're concerned about a recent exposure between prenatal visits, an at-home test can give you an answer at the 14-day mark so you're not waiting weeks for an appointment. A positive result during pregnancy is treated the same way as any other time, effectively and safely, with antibiotics appropriate for use in pregnancy. The infection is manageable. Missing it is what creates risk.
FAQs
1. What are the first signs of chlamydia?
In the cases where symptoms appear, which is less than half of all infections in men and fewer than one in five in women, the earliest signs tend to show up seven to twenty-one days after exposure. For women, this is most often a subtle change in vaginal discharge: slightly cloudier, a different color, or mildly unfamiliar. For men, it may be a small amount of discharge at the tip of the penis, especially noticeable in the morning, or a mild burning sensation when urinating. Both can be easy to dismiss as minor irritation. The most common first sign of chlamydia, though, is nothing, no symptom, no discomfort, no signal at all.
2. Can you have chlamydia with no symptoms?
Yes, and this is the rule rather than the exception. Approximately 80% of women and 50% of men with chlamydia experience no noticeable symptoms throughout the infection. That means the majority of people carrying active chlamydia feel completely fine. The infection replicates inside cells, which allows it to avoid triggering the full immune response that would produce obvious symptoms. No symptoms doesn't mean no infection, it means the infection is doing what it usually does. Testing is the only reliable way to know.
3. How long does it take for chlamydia symptoms to appear?
When symptoms develop, they typically appear within seven to twenty-one days after exposure. That's the general incubation window, the time it takes for the bacteria to replicate enough to trigger a response from the immune system. Some people notice changes as early as one week; others don't develop any symptoms until the third week or later. A significant portion of people never develop symptoms at all, regardless of how long the infection has been present. Importantly, the testing window is separate from the symptom window: 14 days after exposure is when a NAAT gives you a reliable result, regardless of whether symptoms have appeared.
4. What does chlamydia feel like in women?
When it produces symptoms in women, chlamydia most often feels like something subtle rather than dramatic, a mild burning when urinating, a change in discharge that's easy to attribute to other causes, or a dull ache in the lower abdomen. Bleeding after sex or between periods can also occur. None of these feel like an obvious emergency, which is part of why the infection goes unnoticed for so long in so many people. In many women, chlamydia doesn't feel like anything at all, which is why symptoms alone are an unreliable screening tool.
5. What does chlamydia feel like in men?
In men with symptoms, the most common experience is a burning sensation during urination and a small amount of discharge from the tip of the penis, clear, slightly cloudy, or faintly white or yellow. Testicular discomfort or mild swelling can also occur if the infection has spread to the epididymis. But in roughly half of male chlamydia cases, there's nothing noticeable at all. The discharge, when present, is often subtle enough that it gets dismissed as a minor irritation or dried residue, especially if it only appears in the morning.
6. Does chlamydia go away on its own?
No. Chlamydia is a bacterial infection, and bacterial infections don't resolve without antibiotic treatment. The immune system can suppress the symptoms, which is part of why infections appear silent, but it cannot clear Chlamydia trachomatis on its own. An untreated infection can persist for months or years, continuing to cause internal damage and remaining transmissible to partners throughout that time. The symptoms fading, or never appearing in the first place, is not evidence that the infection is gone. Treatment is required, and it's effective, but it has to happen for the infection to clear.
7. Can you get chlamydia without having sex?
In rare cases, yes, but sexual contact is by far the dominant transmission route. Chlamydia spreads through direct mucosal contact with infected secretions, which means vaginal, anal, and oral sex are the primary ways it passes between people. It cannot be transmitted through casual contact, sharing towels, toilet seats, swimming pools, or everyday physical contact will not spread it. The one non-sexual transmission route that matters clinically is from a pregnant person to their baby during childbirth, which is why prenatal screening exists. In adults, a positive chlamydia test almost always reflects a sexual exposure, even if that exposure was oral sex or occurred weeks or months ago.
8. Is chlamydia in the throat the same as genital chlamydia?
It's the same bacterium, Chlamydia trachomatis, infecting a different mucosal site. Throat chlamydia typically develops after oral sex involving an infected partner. In almost all cases, there are no symptoms, or at most a mild sore throat that's indistinguishable from a common cold. Standard STI panels don't include throat swabs unless specifically requested, which means throat infections are commonly missed. If you've had oral sex with a new or untested partner and you're concerned about chlamydia exposure, ask specifically about throat swab testing or look for a panel that includes it.
9. Can chlamydia come back after treatment?
Yes, but it's not a relapse; chlamydia doesn't recur the way a viral infection can. Reinfection happens. If a partner wasn't tested and treated at the same time as you, the infection can be passed back and forth. It can also be acquired from a different partner. Follow-up testing after treatment is recommended to confirm the infection has cleared, and if you test positive again after completing a full treatment course, the most likely explanation is reinfection rather than treatment failure. The practical answer is that treated chlamydia is gone, but tested-and-treated-together is the only version of treatment that actually breaks the cycle.
10. When should I test for chlamydia after exposure?
The right time is 14 days after the exposure you're concerned about. That's when a NAAT, the gold-standard test for chlamydia, reliably detects bacterial DNA at the concentrations needed for an accurate result. Testing before 14 days can produce a false negative even when infection is present, not because the test is flawed but because the bacterial load hasn't reached the detection threshold yet. If you've tested early and got a negative, that result isn't meaningful. Retest at two weeks and treat that result as your actual answer.
Test for Chlamydia From Home, No Appointments, No Waiting
Chlamydia is common, quiet, and almost always treatable when caught. The problem isn't the infection itself; it's the time between exposure and testing, when the infection sits undetected and the risk of complications quietly accumulates. That gap closes with a test. If you've read this far because you're thinking about a recent exposure, that's the signal to act on.
The Chlamydia At-Home Rapid Test Kit (99.7% accuracy) gives you a clear result in minutes from home, no clinic, no appointment, no delay. For broader coverage, the Chlamydia & Gonorrhea 2-in-1 At-Home Rapid Test Kit (98% accuracy) tests for both infections at once, which makes sense given their high co-infection rate. If you want a more comprehensive panel, the Chlamydia, Gonorrhea & Syphilis 3-in-1 (99.5% accuracy) covers three of the most common bacterial STIs in a single test.
Test at 14 days after exposure for your most reliable result. Take control of your sexual health today, and visit STD Rapid Test Kits to find the right kit for your situation.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
2. StatPearls, Chlamydia (NCBI Bookshelf)
3. InformedHealth, Overview: Chlamydia (NIH/IQWiG)
6. HIV.gov, CDC Releases 2024 National STI Data
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.










