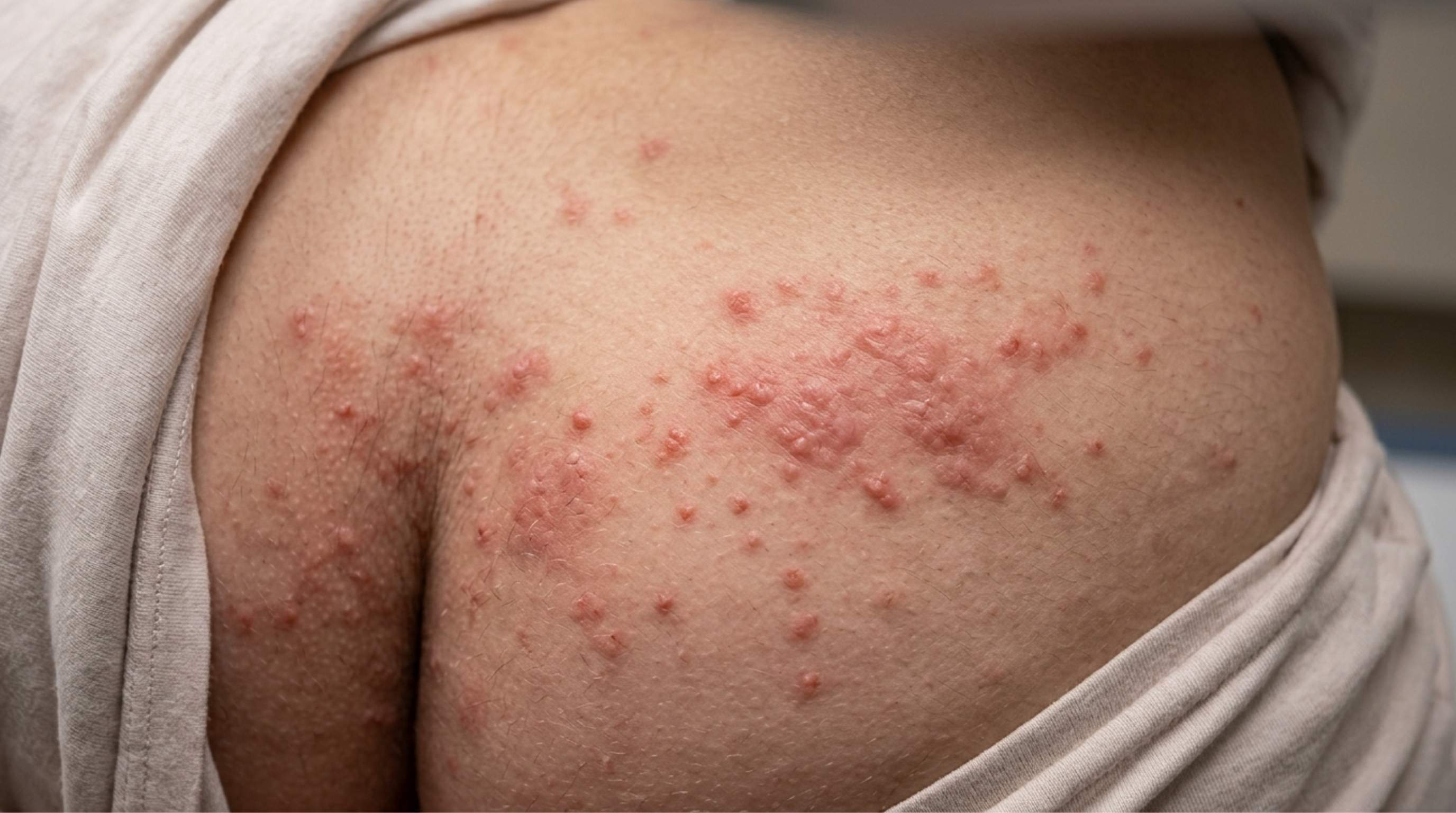
What Are Sexually Transmitted Diseases? How to Use STDs Rapid Test Kit?
Last updated: April 2026
Could a rash be HIV? Yes, but only under specific conditions. An HIV rash typically appears 2 to 4 weeks after exposure as flat or slightly raised red spots (purple on darker skin) across the chest, back, and face, almost always alongside fever, fatigue, and swollen lymph nodes. It resolves within 5 to 8 days. A rash without those accompanying symptoms, or one that appears within a day or two of exposure, is very unlikely to be HIV. The only way to know for certain is to test at 6 weeks after exposure, when a reliable result is possible.
If you've noticed a rash after a sexual encounter you're not sure about, your brain has probably already gone to the worst-case scenario. That's normal. The internet makes it worse. Search "rash after sex," and you'll find enough results to convince yourself of fifteen different things before breakfast. Here's the more useful approach: learn what an HIV rash actually looks like, understand when it would realistically appear, and know exactly when a test will give you a reliable result. That's what this article is for.
A rash can be one of the first visible signs of HIV infection, but only under specific circumstances. CDC surveillance data from 2025 shows that over 39,000 people were diagnosed with HIV in the United States in 2023 alone, and a significant proportion had been living with the virus undetected for months or years before that diagnosis. The rash, when it does appear, is part of what's called acute HIV infection, the body's initial response to the virus. According to research, roughly 50% of people who contract HIV develop some symptoms during this window, per a large international prospective study cited by Johns Hopkins HIV Guide. The other half don't. That's why testing is the only thing that actually answers the question.
People are also reading: Can You Get an STD from a Virgin?
What Does an HIV Rash Actually Look Like?
You're standing in the bathroom, three weeks after a night you're not entirely sure about, and there's a rash on your chest or stomach that wasn't there before. The first instinct is to Google it. The second is to panic. Here's what the science actually says an HIV rash looks like, because knowing the specifics matters more than general fear.
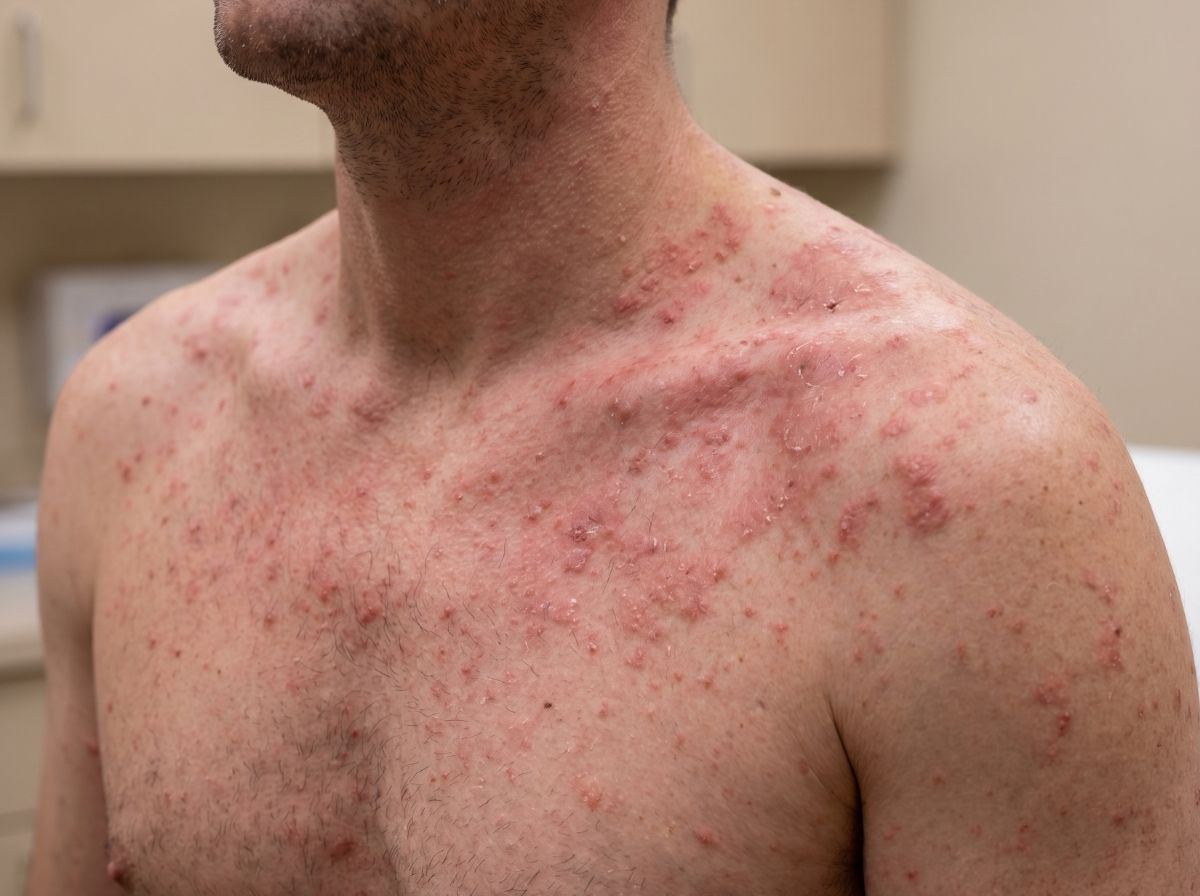
The rash associated with acute HIV infection is technically described as maculopapular, which sounds complicated but just means it appears as flat or slightly raised spots that can cover a moderate area of skin. On lighter skin tones, the spots are typically red or pink. On darker skin tones, they can appear purple, dark brown, or hyperpigmented. The spots tend to be small, somewhat uniform in size, and spread symmetrically, meaning they appear on both sides of the body in roughly the same pattern. The trunk, face, upper arms, and sometimes the palms or soles of the feet are the most common locations.
| Feature | What to Expect |
|---|---|
| Appearance | Flat or slightly raised spots (maculopapular); small, fairly uniform |
| Color (light skin) | Red or pinkish |
| Color (dark skin) | Purple, dark brown, or hyperpigmented |
| Common locations | Trunk (chest/back), face, upper arms; sometimes palms and soles |
| Pattern | Typically symmetrical, widespread, not isolated to one area |
| Itch level | Mild to none, not intensely itchy |
| Blistering or oozing | No |
| Appears with other symptoms? | Almost always, fever, fatigue, swollen glands, sore throat |
| Duration | 5–8 days on average before fading on its own |
| Timing after exposure | 2–4 weeks, typically alongside fever onset |
The rash is usually not intensely itchy, though mild irritation is possible. It doesn't blister, weep, or form open sores the way a herpes outbreak would. It tends to appear symmetrically across the chest, back, or face, not clustered on one side or concentrated in one spot. And critically, it almost never appears on its own. An HIV-related seroconversion rash is typically accompanied by other symptoms: fever, fatigue, swollen lymph nodes, sore throat, muscle aches, and the general feeling of being run down. If you have a rash and feel completely fine otherwise, that's actually a fairly meaningful data point.
How Does an HIV Rash Look on Different Skin Tones?
Most descriptions of an HIV rash, and most of the images that dominate search results, are based on how the rash presents on lighter skin. That's a significant gap, because the rash looks genuinely different on brown and dark skin tones, and those differences don't get nearly enough airtime. If you're working from the "red spots" description and your skin is darker, you might be looking for the wrong thing entirely.
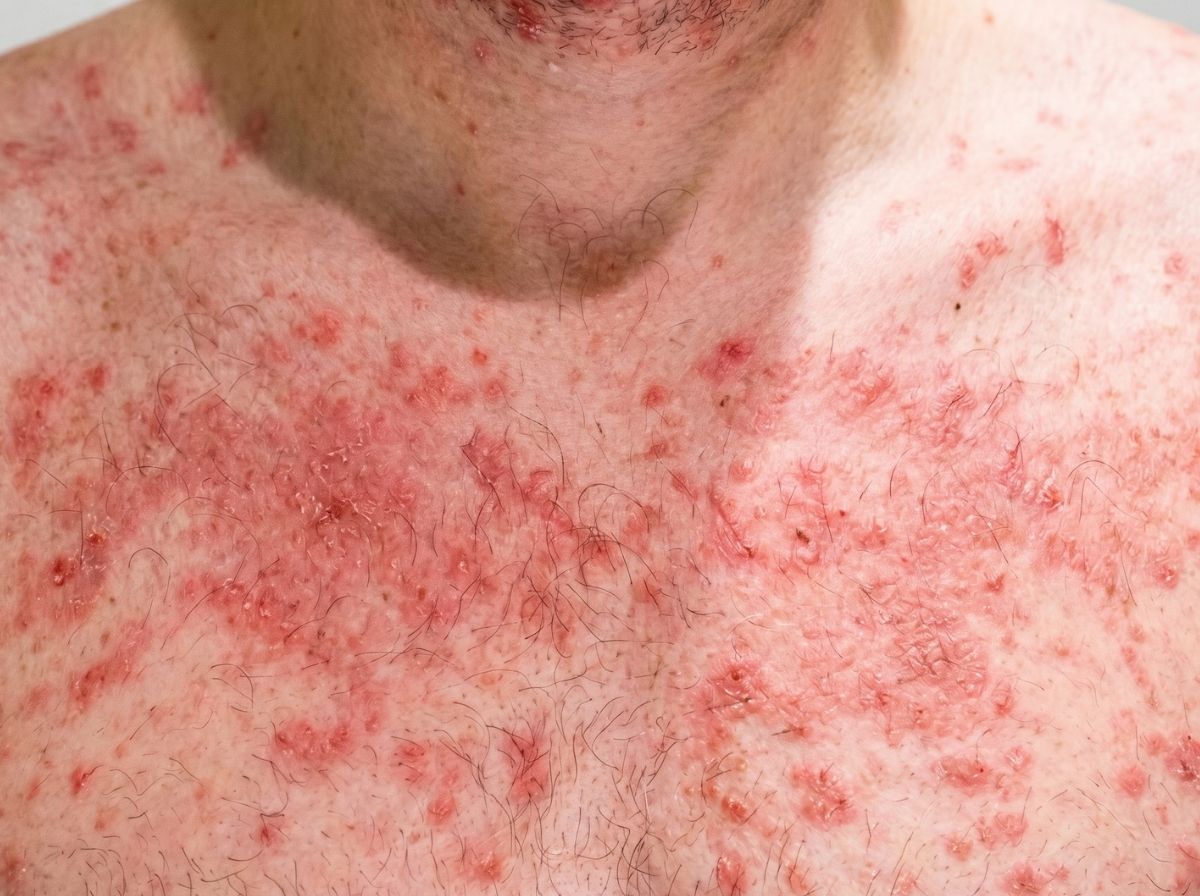
On lighter skin, the seroconversion rash presents as pink or red spots, relatively easy to notice against a pale background. On medium to darker skin tones, the same rash typically appears as purple, deep brown, or hyperpigmented patches that can be harder to distinguish from the surrounding skin in certain lighting. The texture and pattern remain the same, flat or slightly raised, symmetrical, spread across the trunk and face, but the color difference is significant enough to cause real confusion. Someone with dark skin who's been told to look for "red spots" may dismiss the rash entirely, which matters because timing is everything when it comes to HIV exposure and testing.
This isn't a minor editorial point. According to CDC surveillance data, Black and Hispanic individuals are disproportionately affected by HIV in the United States, and gaps in health information, including symptom descriptions that don't reflect diverse skin tones, contribute directly to delayed testing and delayed diagnosis. Knowing what the rash actually looks like on your skin is part of being informed enough to act when it matters.
When Does an HIV Rash Appear, and How Long Does It Last?
Timing is one of the most important things to understand when you're trying to figure out whether a rash could be related to HIV. The rash doesn't show up the next day. It doesn't appear the same week. Biology has its own schedule, and it's actually quite predictable.
After HIV enters the body, there's a phase called acute retroviral syndrome, the period when the immune system first recognizes the virus and mounts a response. This typically begins 2 to 4 weeks after exposure. The rash, when it appears, usually develops a few days after the fever sets in. Clinical case data published in the Canadian Medical Association Journal describes the rash as typically appearing around 3 days after fever onset and persisting for 5 to 8 days before resolving on its own. The whole acute illness, rash included, usually runs its course in 1 to 2 weeks, though in some people it can linger longer.
This is important for a few reasons. If you noticed a rash 2 days after potential exposure, that timeline doesn't fit an acute HIV infection. If you've had a rash for 6 weeks and it's still there, that also doesn't fit the typical acute presentation. Neither of these things means you don't need to test, it just means the rash itself isn't tracking with the biology of an HIV seroconversion rash. The timeline matters as much as the appearance.
One other thing worth knowing: the rash resolving on its own doesn't mean everything is fine. The acute phase of HIV ends regardless of whether someone gets treatment. After symptoms subside, the virus continues to replicate, silently, for years in some cases. This is why people go undiagnosed for so long. The rash fades, they feel better, and they assume it was just a bug. That assumption is exactly what drives delayed diagnosis.
Check Your STD Status in Minutes
Test at Home with RemediumHIV Rapid Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $33.99 $49.00
HIV Rash vs. Other Rashes, The Comparison That Actually Helps
The internet will tell you that an HIV rash is "not itchy" and therefore if your rash itches, it isn't HIV. That's an oversimplification, and it's the kind of one-feature logic that sends people down the wrong path. The more reliable way to tell if a rash could be HIV is to look at the whole picture together: when it appeared relative to any exposure, what else is happening in your body, how the rash is behaving over time, and what the actual transmission risk was. No single feature is diagnostic on its own. What follows is how each common rash type tends to behave differently, and what that difference actually means for ruling things in or out.
Heat rash vs. HIV rash: Heat rash (also called prickly heat or miliaria) clusters in areas where sweat gets trapped, under the arms, behind the knees, in the crease of the groin, and across the back of the neck. It improves when you cool down and tends to clear up within a few hours to a day. It's caused by blocked sweat glands, not an immune response to a virus. If your rash is concentrated in skin folds, worsens in heat, and you've been sweating heavily, the explanation is almost certainly environmental rather than infectious.
Hives vs. HIV rash: Hives (urticaria) are raised, irregular welts, often intensely itchy, that typically appear and resolve quickly. Individual welts usually flatten within 24 hours and may shift location across the body. That behavior, appearing in one spot and disappearing, then reappearing elsewhere, is not how an HIV seroconversion rash works. An HIV rash doesn't travel. It appears in a fairly consistent distribution and stays there until it fades. If your rash is moving around or responding to antihistamines, it's pointing toward an allergic reaction rather than an acute HIV infection.
Eczema and atopic dermatitis vs. HIV rash: Eczema tends to be chronic, recurring, and concentrated in predictable locations for that person, inner elbows, behind the knees, hands, and sometimes the face. It's tied to known triggers: cold weather, certain soaps, synthetic fabrics, and stress. A first-time eczema flare is possible, but even then it doesn't come with fever, swollen lymph nodes, and sore throat. If you're seeing a dry, scaly, intensely itchy rash in typical eczema zones, the seroconversion picture doesn't fit.
Shingles vs. HIV rash: Shingles (herpes zoster) is distinctive enough that it's genuinely one of the easier comparisons. It presents as a painful, blistered band that follows the path of a single nerve, almost always on one side of the body only, often the torso or face. There's usually burning or hypersensitivity before the rash even appears. An HIV seroconversion rash is bilateral, non-blistered, and doesn't follow a nerve path. If what you're seeing is one-sided and painful before the rash appeared, that's shingles territory.
Genital herpes vs. HIV rash: A herpes outbreak presents as painful, fluid-filled blisters concentrated around the genitals, buttocks, or thighs, not spread across the chest and face. Herpes blisters crust over and heal over 1 to 2 weeks, and outbreaks tend to recur in the same location. The texture, location, and behavior are all fundamentally different from a seroconversion rash.
Drug reaction rash vs. HIV rash: This is the trickiest comparison, because a drug-induced maculopapular rash can look nearly identical to an HIV seroconversion rash, widespread, red, symmetrical. The key question here is simple: Did you start a new medication in the past 1 to 3 weeks? If yes, the rash may be the medication. Drug rashes typically appear days to weeks after starting a new drug and resolve when the drug is stopped or switched. This is one of the reasons clinicians always ask about medication history when evaluating a rash.
Secondary syphilis rash vs. HIV rash: Secondary syphilis is worth knowing about because it's an STI with its own distinctive rash, and it can appear alongside HIV transmission risk. The secondary syphilis rash is widespread and often copper-toned rather than red. Its signature feature, one that doesn't appear in the HIV seroconversion rash, is involvement of the palms of the hands and soles of the feet. If you're seeing spots on your palms and soles, syphilis is a stronger candidate than HIV alone. Testing for both simultaneously is the smart move.
| Rash Type | Appearance | Typical Location | Accompanying Symptoms | Key Differentiator |
|---|---|---|---|---|
| HIV seroconversion rash | Flat/raised red or purple spots | Trunk, face, arms | Fever, fatigue, swollen glands, sore throat | Appears 2–4 weeks post-exposure; resolves in 5–8 days |
| Heat rash | Small red bumps or blisters | Skin folds, sweaty areas | None (or mild discomfort) | Triggered by heat/sweat; improves with cooling |
| Hives (urticaria) | Raised, irregular welts | Variable, can move around | Itching (often intense) | Individual spots resolve within 24 hours; linked to allergen |
| Eczema/dermatitis | Dry, scaly, inflamed patches | Elbows, knees, hands | Chronic itching | Recurrent, tied to known triggers |
| Herpes (HSV-2) | Fluid-filled blisters, painful | Genitals, buttocks, thighs | Tingling, burning, pain | Blisters that crust and heal; recurring outbreaks |
| Shingles | Painful blistered band | One side of torso or face | Pain, burning before rash appears | Always one-sided; follows nerve path |
| Drug reaction | Widespread red maculopapular rash | Trunk, spreading outward | Variable | Began after starting a new medication |
| Syphilis secondary rash | Copper-colored spots, often on palms/soles | Entire body including palms and soles | Flu-like, hair loss, mucous patches | Distinctive palm/sole involvement; copper tone |
The Exposure Is the Deciding Factor, Not Just the Rash
Here's the piece of the puzzle that gets left out of most rash articles: the rash is not the deciding factor. The exposure is. This is one of the most important things a sexual health clinician would tell you, and it's the single clearest way to cut through the anxiety spiral.
If there was a real exposure, unprotected penetrative sex, a condom that broke, or another genuine transmission risk, and a rash appeared 2 to 4 weeks later alongside flu-like symptoms, that combination absolutely warrants an HIV test. Not because you have HIV, but because the biology fits, and a test is the only thing that actually answers the question. On the other hand, if you used protection correctly, or the contact was low-risk, or the rash appeared 2 days later and you feel completely fine, the rash alone is not a logical trigger for HIV concern. Most rashes that people attribute to HIV anxiety have a far simpler explanation.
This isn't about dismissing concern. It's about being honest that anxiety doesn't make a rash more likely to be HIV; it just makes it feel more likely. The actual risk factors for HIV transmission are well understood: unprotected anal or vaginal sex, shared needles, or specific exposure to blood or other infectious fluids. If none of those apply, a rash on your chest is almost certainly not HIV. If they do apply, testing is the only way to know for sure, and testing is straightforward, fast, and something you can do from home.

People are also reading: Your Partner Looks Healthy, Why That Means Nothing for STDs
How Do I Know If My Rash Is From HIV? Take the Test at the Right Time
HIV antibody tests, the kind used in most rapid at-home test kits, work by detecting the antibodies your immune system produces in response to the virus. Here's the biology of why timing matters: when HIV enters the body, it takes time for the immune system to produce enough antibodies to reach a detectable level in the blood. This period, between exposure and detectable antibody levels, is called the window period. Test inside this window, and you may get a negative result even if HIV is present, because the antibodies simply haven't built up enough yet. That's not a flaw in the test. It's biology.
For antibody-based rapid tests, the window period closes at approximately 6 weeks after exposure. Testing at 6 weeks gives you a reliable first indicator. For complete certainty after a genuinely high-risk exposure, unprotected anal sex, a broken condom with a partner of unknown status, shared needles, and retesting at 12 weeks provides the definitive result. The reason the 12-week retest matters is that a small percentage of people take longer to develop detectable antibody levels, and a confirmed negative at 12 weeks is conclusive. Testing before 6 weeks, especially in the first 2 to 3 weeks when the seroconversion rash would be appearing, is almost certain to return a negative result regardless of actual status, which can give a dangerous false sense of reassurance at exactly the wrong moment.
One practical clarification worth knowing: the seroconversion rash typically appears during the window period itself, before a reliable antibody test is even possible. This is one reason the rash feels so alarming and simultaneously so unhelpful as a diagnostic tool. You're in the period where the biology is most visible, and the test is least reliable. The rash may be real, the anxiety is real, but the answer has to wait for the window to close.
The HIV 1&2 At-Home Rapid Test Kit (99.7% accuracy) is designed for exactly this situation, private, fast, and giving you a result in minutes without needing a clinic visit or a lab. If you're at or past the 6-week mark after a potential exposure and want clarity, that's your next step. Testing is not a confession. It's the most responsible thing you can do, both for yourself and for anyone you're close to.
If you've had a high-risk exposure very recently, within the past 72 hours, post-exposure prophylaxis (PEP) is also an option worth discussing with a healthcare provider urgently. PEP is a short course of medication that can significantly reduce the risk of HIV taking hold if started quickly enough. That's a separate conversation from testing, but a critical one if the timing applies.
Other Skin Conditions Associated with HIV: What Comes Later
The seroconversion rash is the one most people are worried about during the panic of a potential exposure. But it's worth knowing that HIV and skin problems have a longer relationship than just those first few weeks. For people who are living with HIV, particularly those who aren't yet on treatment or whose immune system has been significantly affected, other skin conditions become more common over time. Understanding this helps separate an acute worry from a longer-term health picture.
When the immune system is suppressed, the body struggles to hold off opportunistic infections, organisms that would normally be kept in check without issue. Some of these show up on the skin. Eosinophilic folliculitis presents as an itchy, persistent rash of red bumps around hair follicles, most commonly seen in people with more advanced HIV. Molluscum contagiosum, a viral skin infection that causes small, dome-shaped bumps, tends to be more widespread and harder to clear in people with a weakened immune system. Seborrheic dermatitis, which causes flaky, oily patches around the scalp and face, is also more common and more severe in people with HIV.
Kaposi's sarcoma, a type of cancer associated with a herpesvirus, can cause distinctive dark red, purple, or brown patches or nodules on the skin and is strongly associated with late-stage HIV and AIDS. It's worth mentioning not to alarm anyone, but because it looks very different from a seroconversion rash, the spots are larger, often nodular, and don't resolve on their own. If you're seeing something in that category, it's not a "wait and see" situation.
The key takeaway here is that most of the more serious skin manifestations of HIV appear in people whose infection has been unmanaged for a long time. Early diagnosis and effective antiretroviral treatment dramatically reduce the likelihood of ever reaching that stage. This is one more reason why knowing your status, especially after any real exposure risk, is genuinely important health management, not just peace of mind.
People are also reading: STD Testing Window Periods And When to Test for Each
What a Rash Can and Cannot Tell You
Imagine lying awake at 2 AM, phone in hand, comparing photos of rashes online to a spot on your arm that you've convinced yourself is suspicious. It's one of the most common experiences people have when processing anxiety about a possible HIV exposure, and it's also one of the least productive. Here's the hard truth: visual diagnosis of HIV from a rash, whether in a mirror, in photos, or through a Google image search, is not reliable. Not for you, not for anyone.
The reason isn't that people aren't smart enough. It's that the rash itself is genuinely non-specific. Many different rashes look similar. The HIV seroconversion rash is not so distinctive that you can identify it from appearance alone. What changes the calculation is the full context: when it appeared, what else is happening in the body, what the actual exposure risk was, and what a test says. Remove any one of those pieces and the rash alone tells you very little.
What the rash can do is motivate you to test. And that's actually valuable. If you've noticed something on your skin, combine it with recent exposure risk, and you're concerned, that concern is data. Use it. Don't use it to spiral; use it to take the step that ends the uncertainty. A rash that triggers a test that comes back negative is a rash that gave you peace of mind. A rash that triggers weeks of Googling gives you nothing except anxiety.
FAQs
1. How soon after HIV exposure does a rash appear?
The seroconversion rash typically appears 2 to 4 weeks after exposure, usually a few days after fever sets in. A rash that shows up within a day or two of potential exposure isn't following the biological timeline for acute HIV infection.
2. Can you have HIV without getting a rash?
Yes, around half of the people who contract HIV don't develop any noticeable symptoms during the acute phase, including no rash. The absence of a rash absolutely does not mean you don't have HIV. Testing is the only reliable answer.
3. How long does an HIV rash last?
The seroconversion rash typically resolves within 5 to 8 days. The broader acute illness, including fever and fatigue, usually lasts 1 to 2 weeks. If a rash has been present for several weeks unchanged, it's less likely to be tracking with acute HIV infection.
4. Is an HIV rash itchy?
The seroconversion rash is typically mild in terms of itching; it may have some irritation, but it's not intensely itchy the way an allergic reaction or eczema would be. That said, itchiness alone can't rule HIV in or out. The full picture matters more than any one feature.
5. Can a rash appear on the palms of the hands with HIV?
Yes, the seroconversion rash can extend to the palms and soles in some people; this is one feature it shares with the secondary syphilis rash. If you're seeing a rash on your palms alongside other systemic symptoms, that's worth taking seriously and testing for both HIV and syphilis.
6. What's the difference between an HIV rash and a syphilis rash?
Both can appear widespread, but the secondary syphilis rash has a particularly distinctive feature: it almost always involves the palms of the hands and soles of the feet, and the spots tend to be copper-toned rather than red. Syphilis also progresses through distinct stages with specific timing. If there's any real exposure risk, testing for both is the sensible move.
7. Can stress cause a rash that looks like an HIV rash?
Yes. Stress-induced hives, anxiety-related skin flushing, and stress eczema can all look concerning. Stress rashes tend to be patchy, itchy, and resolve faster, and they don't come with fever, swollen glands, or the systemic symptoms of acute retroviral syndrome. If the only thing happening is a rash and anxiety, that's a very different picture from HIV seroconversion.
8. When is the earliest I can take an HIV test after exposure?
The testing window for antibody-based rapid tests opens at 6 weeks after exposure. Testing before that point risks a false negative result because antibody levels may not yet be detectable. For full certainty, retesting at 12 weeks gives a definitive answer after a high-risk exposure.
9. What if my test comes back negative at 6 weeks?
A negative result at 6 weeks is a strong indicator, but if the exposure was genuinely high-risk, confirming with a second test at 12 weeks gives complete certainty. A negative at 12 weeks is conclusive.
10. Can an HIV rash be the only symptom of early HIV infection?
Rarely. The seroconversion rash almost always appears alongside other symptoms, particularly fever, fatigue, and swollen lymph nodes. An isolated rash with no other symptoms is less consistent with acute HIV infection, though it doesn't entirely rule it out. If you've had a real exposure risk, test regardless of what symptoms are or aren't present.
Get Tested and Get Your Answer
A rash is a reason to pay attention. It's not a diagnosis. The only thing that actually tells you your HIV status is a test, and the good news is that testing has never been easier, faster, or more private than it is right now. You don't need a clinic appointment or a doctor's visit. You need the right test, taken at the right time.
If you're at or past the 6-week window after a potential exposure, the HIV 1&2 At-Home Rapid Test Kit (99.7% accuracy) gives you results in minutes, at home, with complete privacy. For broader peace of mind, particularly if you're not certain which exposures to account for, the 7-in-1 Complete At-Home STD Test Kit covers HIV alongside gonorrhea, chlamydia, syphilis, herpes HSV-2, hepatitis B, and hepatitis C in one kit. And for women who want the most comprehensive panel available, the Women's 10-in-1 Kit adds HPV and trichomoniasis to the full panel.
Testing is the fastest way to stop the guessing game. Whatever the result is, knowing puts you in control. Visit STD Rapid Test Kits and take that next step today.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC, HIV Diagnoses, Deaths, and Prevalence: 2025 Update
3. CMAJ / PMC, Acute HIV Infection in a 39-Year-Old Man (Case Report)
4. New York State AIDS Institute, Diagnosis and Management of Acute HIV Infection
5. Healthline, HIV Rash: Pictures, Treatment, and More
6. Aidsmap, What Are the Symptoms of Early HIV Infection?
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.