Last updated: April 2026
Herpes simplex virus is one of the most prevalent human infections on the planet. According to the WHO, an estimated 3.8 billion people under 50, roughly 64% of the global population, carry HSV-1, the virus responsible for oral herpes and cold sores. Approximately 520 million people aged 15–49 carry HSV-2, the strain most commonly associated with genital herpes. In the United States, Johns Hopkins Medicine estimates that between 50% and 80% of adults carry oral herpes, and roughly 1 in 6 Americans aged 14–49 have genital herpes. The overwhelming majority of them, by some estimates up to 90%, have no idea. This is not a rare, shameful infection that happens to reckless people. It is a ubiquitous human virus that most of the sexually active population carries, managed or unmanaged, often without ever experiencing a recognizable symptom.
If you've just been diagnosed, are trying to figure out if what you're experiencing might be herpes, or have been living with it for years and still have unanswered questions, this guide is the honest, complete resource that most people never get from a five-minute clinical appointment.
In this guide: What herpes actually is · HSV-1 vs. HSV-2: what the difference means for you · Symptoms, outbreaks, and what to look for · Why most people don't know they have it · How herpes actually spreads · How to test, and when · After a positive result · Treatment options and what they do · Reducing transmission risk · Relationships, disclosure, and living with herpes · FAQs
People are also reading: STD Myths and Facts: Common Misconceptions About Sexually Transmitted Infections
What Herpes Actually Is, And What It Isn't
Herpes simplex virus is a DNA virus in the Herpesviridae family, the same family that includes chickenpox, mononucleosis, and cytomegalovirus, all of which most people carry without much drama about it. Like those relatives, HSV establishes what's called latency: after the initial infection, the virus retreats into nerve cells near the site of entry and stays there for life. It does not travel around the bloodstream, does not damage organs, and for most people causes either no symptoms at all or occasional mild outbreaks that resolve on their own.
What it is not: a disease that defines you, a moral verdict, or an automatic sign of recklessness. The CDC's National Health and Nutrition Examination Survey data found that HSV-1 prevalence among American adults aged 14–49 was nearly 48%, meaning about half the adult population carries the virus that causes cold sores, most having acquired it in childhood through a kiss from a relative or sharing a drink. The cultural weight attached to herpes has almost no relationship to its actual medical footprint for the majority of people who carry it. The gap between herpes as the internet imagines it and herpes as it actually exists in human biology is one of the largest in all of sexual health.
There is no cure for herpes, and that statement carries more weight than it should. The virus establishes permanent latency, which is true. What that means in practice depends enormously on the individual: some people have one outbreak and never another recognizable episode. Some manage outbreaks with antiviral medication that reduces both frequency and transmission risk significantly. Many carry the virus for their entire lives without a single identified symptom. "No cure" does not mean "constant suffering," or "ruined sex life," or "impossible relationships." It means the virus is present. What happens after that varies widely, and for most people, it varies much less dramatically than the stigma suggests.
HSV-1 vs. HSV-2: What the Difference Actually Means
The distinction between HSV-1 and HSV-2 is one of the most misunderstood aspects of herpes, partly because the traditional shorthand, HSV-1 is oral, HSV-2 is genital, is no longer biologically accurate as a general rule. Both viruses can infect both sites. Both can cause both oral and genital herpes. The distinction matters, but not in the way most people think.
HSV-1 has historically been transmitted orally, through kissing, shared utensils, or skin-to-skin contact around the mouth, and typically established latency in the trigeminal ganglia, the nerve cluster near the base of the skull that serves the face. This is the virus behind cold sores. However, a systematic review published in 2024 in the journal Cell Reports Medicine, covering 159 studies and over 190 seroprevalence measures in the United States, found that HSV-1 is increasingly being transmitted genitally, particularly in developed countries where improved childhood hygiene means fewer people are exposed to it orally before they become sexually active. That demographic shift means a person without prior oral HSV-1 exposure who receives oral sex from a partner with oral herpes can develop genital HSV-1. Genital HSV-1 tends to cause fewer recurrent outbreaks than genital HSV-2, often just one initial episode, but it is transmissible, and it matters for how you test and what you communicate to partners.
| Feature | HSV-1 | HSV-2 |
|---|---|---|
| Primary site of infection | Oral (historically); increasingly genital via oral sex | Genital |
| Main transmission route | Oral contact (kissing, sharing utensils); oral-genital sex | Genital-genital or oral-genital sexual contact |
| Latency location | Trigeminal ganglia (serves face and mouth) | Sacral ganglia (serves genitals and lower body) |
| Recurrence rate (genital infection) | Low, often 0–1 recurrences per year | Higher, average 4–6 recurrences per year initially |
| Global prevalence | ~3.8 billion people under 50 (64%), WHO 2025 | ~520 million people aged 15–49 (13%), WHO 2025 |
| Asymptomatic carriers | Majority, most people don't know they carry it | Up to 90% unaware, CDC / ASHA data |
| Detectable with at-home blood test? | Yes, HSV-1 rapid test kit (98.2% accuracy) | Yes, HSV-2 rapid test kit (98.2% accuracy) |
HSV-2 is primarily transmitted sexually and almost exclusively causes genital infection. It recurs more frequently than genital HSV-1, establishes latency in the sacral ganglia at the base of the spine, and is more likely to cause recognizable recurrent outbreaks. According to WHO data, HSV-2 infects women almost twice as often as men, because sexual transmission from male to female partners is more efficient anatomically. Women also tend to have more pronounced initial outbreaks. The crucial implication of the HSV-1/HSV-2 distinction for practical purposes: which type you have affects how often you're likely to have recurrent outbreaks, whether your partner needs specific information about oral versus genital exposure, and which antiviral approach is most relevant to your situation. It doesn't change the fundamental picture of what herpes is or how manageable it is.
Check Your STD Status in Minutes
Test at Home with RemediumGenital & Oral Herpes Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $75.00 $98.00
For all 2 tests
Symptoms, First Outbreaks, and How to Tell What You're Looking At
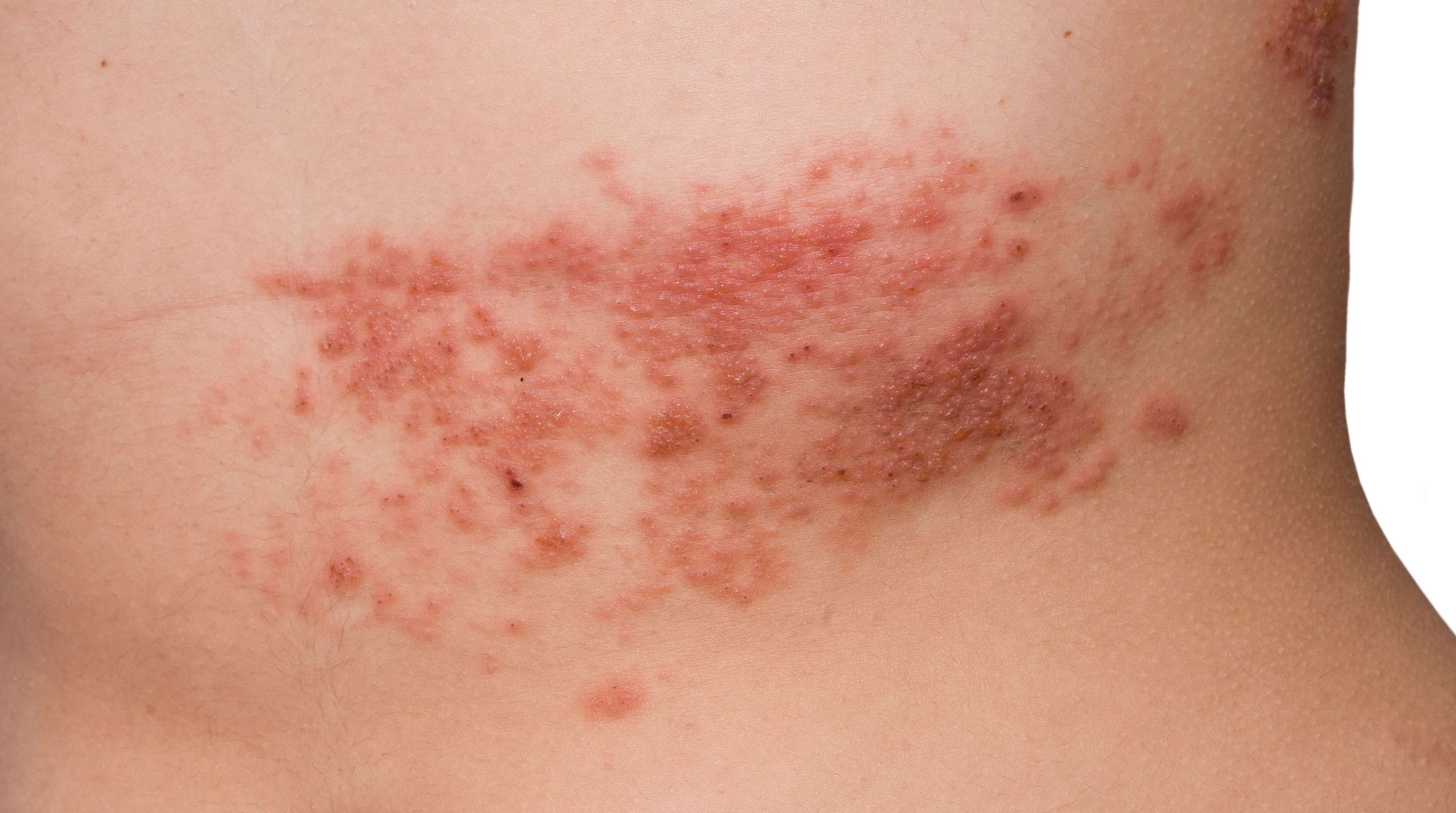
The reason so many people don't know they carry herpes is that the virus frequently produces either no symptoms at all or symptoms so mild they're attributed to something else entirely, a razor rash, a friction sore, an ingrown hair, a pimple, a small cut. The classic herpes depiction, dramatic blistering sores that are impossible to miss, represents the experience of a minority of infected people, primarily during a severe initial outbreak. Most people's experience is considerably more subtle.
When symptoms do occur, the pattern differs between a first outbreak and recurrences. A first episode (primary infection) is typically the most severe the virus will ever be, the immune system hasn't encountered this pathogen before, so it mounts a full inflammatory response. According to CDC STI clinical guidelines, symptoms of a primary genital herpes outbreak can include: tingling, itching, or burning at the site before sores appear; clusters of small fluid-filled blisters that break open to leave shallow, painful ulcers; pain or discomfort with urination if lesions are near the urethra; swollen lymph nodes in the groin; and, in some people, flu-like symptoms including fever, body aches, and fatigue during the initial immune response. A primary outbreak can last two to four weeks. It often happens weeks to months after the actual exposure, which is one of the reasons people frequently misattribute it to the wrong partner or the wrong time.
Recurrent outbreaks are almost always milder and shorter than the first. Many people experience prodromal symptoms, a tingling, burning, or itching sensation at the site, a day or two before any lesion appears. This prodromal phase is important to know about because the virus is already shedding and the person is already contagious before anything visible has developed. Research published in PMC tracking women with first-episode genital herpes found that recurrent outbreaks typically last three to seven days and become less frequent over time as the immune response matures. For HSV-1 genitally, a prospective cohort study published in JAMA found that genital shedding declined significantly from 12.1% of days at two months to 7.1% at eleven months, with recurrence often so infrequent that many people experience just one identifiable episode.
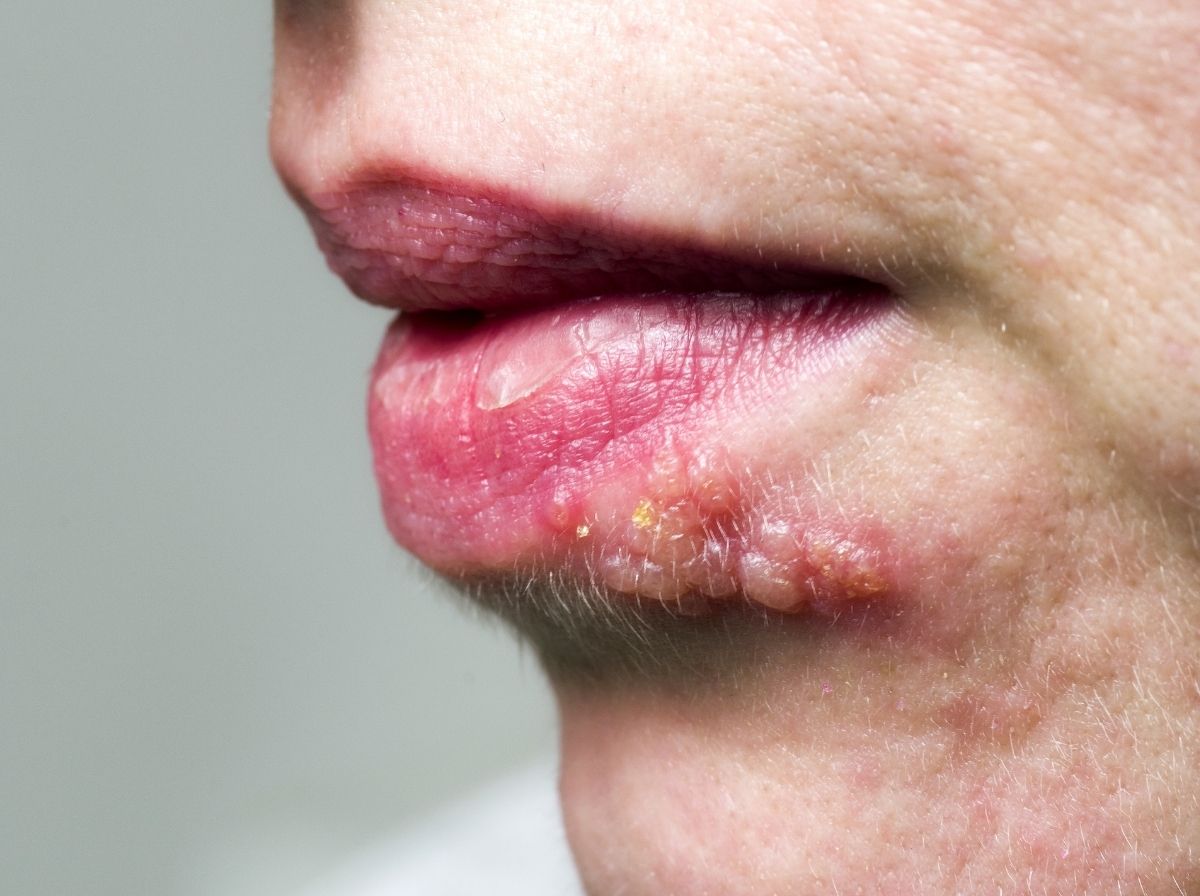
Where herpes appears depends on which nerve cluster the virus has established latency in. For oral HSV-1, lesions typically appear on or around the lips, sometimes on the chin, nose, or inside the mouth. For genital herpes from either HSV-1 or HSV-2, lesions can appear on the genitals (penis shaft, labia, vaginal opening), the inner thighs, buttocks, and anus. Lesions don't always appear at the original transmission site, they appear where the virus exits the nerve pathway, which can be anywhere in the territory that nerve cluster serves.
| Condition | Appearance | Key Difference from Herpes |
|---|---|---|
| Herpes (HSV) | Clusters of small fluid-filled blisters that ulcerate; often in the same location recurrently | Recurs in the same area; preceded by tingling or itching; heals without scarring |
| Ingrown hair | Single raised bump, often with a visible hair underneath; may have a whitehead | Usually solitary; trapped hair often visible; not preceded by tingling; appears after shaving |
| Razor rash / folliculitis | Multiple small red bumps or pustules following a shaving area | Appears immediately after shaving; follows hair follicle pattern; no preceding tingling |
| Acne / cyst | Single pimple or cyst; deeper and less painful at the surface | No blistering phase; not preceded by prodromal tingling; doesn't ulcerate the same way |
| Contact dermatitis | Diffuse redness or rash with no distinct blistering pattern | No cluster formation; usually caused by a product or allergen; no prodrome |
| Syphilis sore (chancre) | Single, painless, firm ulcer, typically without the blister phase | Usually painless (unlike herpes); typically solitary; requires separate testing to distinguish |
The honest answer to "is this herpes?" based on appearance alone is: you cannot tell reliably. Herpes lesions look like several other conditions, and several other conditions look like herpes. Visual diagnosis from a Google image search is not how herpes is identified, not by patients, and frequently not even by clinicians without a laboratory test. If you have a sore or cluster of sores in the genital area or around the mouth that you can't explain, testing is the only way to get a definitive answer. Guessing from appearance in either direction, convincing yourself it's nothing, or assuming the worst, leaves you without the information you actually need.
Why Most People Don't Know They Have It, And Why That Matters
The data on this is stark and consistently underappreciated: the American Sexual Health Association, citing CDC figures, reports that as many as 90% of people with genital HSV-2 infection are unaware they carry it. For HSV-1, unawareness is even higher. This isn't about denial or avoiding testing. It's about biology. The virus frequently produces symptoms so mild, a brief tingling, an itch, a small sore that's gone in two days, that people attribute them to friction, a minor skin irritation, or nothing at all. And for a significant proportion of carriers, the virus produces no recognizable symptoms, ever.
What this means epidemiologically is that herpes transmission happens overwhelmingly between people who don't know they're infected. The person who gave it to you almost certainly didn't know they had it. The shame narrative around herpes, that it's a consequence of recklessness or dishonesty, collapses when you understand that the infection is so commonly asymptomatic that the majority of carriers have never had a reason to be tested for it. Herpes is not on standard STI panels in most clinical settings, which means most people have never been specifically tested, and a negative result on a general STI panel tells you nothing about herpes status.
Asymptomatic viral shedding, where the virus is active and transmissible on the skin surface without any visible sore present, is the primary mechanism by which most herpes transmission occurs. A CDC MMWR analysis of national HSV-2 seroprevalence data confirmed that viral shedding and transmission to sex partners can occur in the absence of symptoms or a noticeable lesion, with 81.1% of HSV-2 infections found to be asymptomatic or unrecognized. A PMC-published cohort study tracking women with first-episode genital herpes over a median of 63 weeks found that asymptomatic shedding occurred in 10–23% of participants depending on the strain and prior infection history, and that asymptomatic cervical shedding was three times more frequent in the first three months after primary infection than in later periods. A mathematical transmission model published in PMC confirmed that asymptomatic shedding accounts for the majority of HSV-2 transmissions, even though viral load during visible lesions is higher. This is why condoms reduce transmission risk but don't eliminate it, herpes is present on skin surfaces that a condom doesn't cover, and why antiviral suppressive therapy, which reduces shedding as well as outbreak frequency, is an important tool for couples where one partner is positive and one isn't.

People are also reading: Scared to Get Tested for an STD? Here's How to Actually Pull Through
How Herpes Actually Spreads, The Real Picture
Herpes is a skin-to-skin contact virus. It spreads when the virus present on one person's skin or mucous membranes makes contact with a small break, crack, or mucous membrane on another person's skin. It does not spread through blood, urine, or casual non-intimate contact. You cannot get it from a toilet seat, a swimming pool, or a door handle. The transmission routes that matter are oral contact (kissing, sharing utensils during an active oral outbreak) for HSV-1, and genital-genital or oral-genital sexual contact for both strains.
The oral-to-genital transmission pathway deserves specific attention because it accounts for a growing proportion of genital herpes cases, particularly HSV-1. When someone with oral herpes (cold sores) performs oral sex on a partner who has not previously been exposed to HSV-1 orally, that partner can develop genital HSV-1. This happens because the virus is present in oral secretions and on skin surfaces around the mouth, including during asymptomatic shedding periods when no sore is visible. The increasing prevalence of this transmission route is directly related to the demographic shift described earlier: more young adults are reaching sexual debut without prior oral HSV-1 exposure, making them susceptible to genital transmission from a partner with oral herpes who doesn't realize they're contagious.
Transmission from genital HSV-2 follows similar principles. The virus is present on genital skin surfaces, not just on visible sores, and can be transmitted during asymptomatic shedding. Transmission is more efficient from male to female partners than the reverse, due to anatomical differences in mucous membrane surface area. The risk of transmission per sexual encounter is not 100% and is affected by several factors: whether sores are present (higher risk), whether antiviral suppressive therapy is being used (significantly lower risk), and whether condoms are used consistently (moderate risk reduction). None of these factors, individually or combined, reduces transmission risk to zero, but the combination of suppressive therapy and consistent condom use represents a substantial reduction in risk for discordant couples (where one partner is positive and one is not).
What herpes is not transmitted by: sharing towels or bedding (the virus survives only briefly outside the body on surfaces), kissing on the cheek or forehead (general skin-to-skin contact without mucous membrane or lesion contact does not transmit herpes), or any form of casual social contact. The transmission picture is narrower and more specific than the stigma implies.
How to Test for Herpes, and the Critical Question of When
Here is the thing that surprises most people about herpes testing: it is not included in standard STI panels. If you've been tested for STIs at a clinic and were told everything was clear, that result almost certainly says nothing about your herpes status unless you specifically requested herpes testing. This is a policy decision by most clinical guidelines, the rationale being that most people with herpes are asymptomatic and testing without symptoms can generate false positives or anxiety without clear clinical benefit. The practical consequence is that most people have never been specifically tested for herpes, and most people who have it don't know.
At-home rapid testing changes that picture. Both HSV-1 and HSV-2 can be tested for at home using a blood-based rapid test that detects the IgG antibodies your immune system produces in response to infection. The test works via finger-prick blood sample, delivers results in ten to twenty minutes, and achieves 98.2% accuracy for both strains. The combined HSV-1 and HSV-2 combo test covers both strains in a single session. For people who want to know their herpes status specifically, as part of a comprehensive sexual health check, before beginning a new relationship, or after a potential exposure, at-home testing provides that answer without requiring a specific clinical request or a difficult conversation in a medical setting.
The critical variable for accurate herpes testing is timing. IgG antibodies, the type detected by blood-based herpes tests, take time to develop after initial infection. The testing window for herpes is 6 weeks after exposure for both HSV-1 and HSV-2. Testing before the 6-week mark can produce a false negative, not because the test is flawed, but because the immune response hasn't had enough time to generate detectable antibody levels. If you test negative before 6 weeks, the result is provisional; retest after the window closes. Testing at or after 6 weeks gives you a reliable, actionable result. In some cases where initial exposure timing is uncertain or where a negative result doesn't align with symptoms, a 12–16 week retest provides additional certainty. For testing during an active outbreak specifically, where a swab of the lesion rather than a blood sample can detect the virus directly, sensitivity is highest when sores are present and actively shedding.
| Test Type | What It Detects | When to Test | Accuracy | Best For |
|---|---|---|---|---|
| Blood-based IgG antibody test (rapid) | HSV-1 and/or HSV-2 antibodies from past infection | 6 weeks after exposure (minimum) | 98.2% | Establishing baseline status; knowing if past exposure resulted in infection |
| Clinical viral culture / PCR swab | Active virus from a lesion directly | During an active outbreak with sores present | Highest when sores are fresh | Confirming an active outbreak; distinguishing HSV from other conditions |
| Clinical Western Blot (confirmatory) | HSV-specific antibodies, most specific test available | Used to confirm low-positive or ambiguous IgG results | Gold standard | Resolving uncertain or low-value IgG results |
One nuance worth understanding: IgG blood tests can occasionally produce low-positive results in the 1.1–3.5 index value range that carry higher false-positive rates than clearly positive results. If you receive a low-positive IgG result, either from a rapid test or a clinical test, and have no history of recognizable symptoms, a confirmatory Western Blot test is the most specific follow-up available. This doesn't mean every positive IgG result is uncertain; clearly positive results at higher index values are reliable. It means that for ambiguous results, confirmation is worth pursuing before making clinical decisions.
Check Your STD Status in Minutes
Test at Home with RemediumGenital Herpes Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $45.99 $49.00
After a Positive Result: What Herpes Actually Means for Your Health
A positive herpes test result is medical information. It is not a verdict, not a catastrophe, and not the end of a normal sex life or relationship. The gap between how most people imagine a herpes diagnosis before they receive one and what it actually means in practice is one of the widest in all of sexual health, and closing that gap is one of the most useful things this guide can do.
Medically, a positive HSV result means the virus has established latency in your nervous system and will remain there. What happens next depends heavily on which strain you have, how your immune system responds to it, whether you choose suppressive antiviral therapy, and a significant degree of individual variability that the research is honest about. Some people have one initial outbreak, manage it with antiviral medication, and have no further recognizable episodes. Some have periodic recurrences that decrease in frequency and severity over time. Some experience more frequent outbreaks and benefit significantly from daily suppressive therapy, which both reduces outbreak frequency and, importantly, reduces the likelihood of transmitting the virus to a partner. There is no single herpes experience, and what you read about the worst-case scenarios online represents the most severe end of a very wide spectrum.
For your physical health beyond the outbreaks themselves: herpes does not damage organs, does not affect fertility, and does not increase cancer risk on its own. The medically significant interaction is the bidirectional relationship between herpes and HIV. The CDC's STI Treatment Guidelines note that HSV-2 infection increases the risk of acquiring and transmitting HIV by at least twofold, because genital herpes lesions create entry and exit points that HIV can exploit, and because the local immune activation triggered by HSV-2 makes genital tissue more susceptible to HIV acquisition. The WHO similarly confirms this bidirectional risk in its HSV fact sheet. For people in populations where HIV exposure is a realistic risk, knowing your herpes status is therefore directly relevant to your HIV risk, which is one of the strongest public health arguments for routine herpes testing alongside standard STI panels. Herpes in pregnancy is also a specific clinical consideration, particularly primary HSV infection acquired late in pregnancy, which carries transmission risk to the newborn during delivery. This is a conversation your obstetrician needs to be part of, early identification and management significantly reduces neonatal risk.
What a positive result does not mean: that you are dirty, reckless, or dishonest. The biology of asymptomatic transmission makes the moral narrative around herpes almost entirely disconnected from the epidemiological reality. The person who transmitted it to you almost certainly didn't know they had it. If you transmitted it to someone without knowing you carried it, you had no information to act on. The appropriate response to a diagnosis is not shame, it's accurate information, a conversation with a healthcare provider about management options, and a thoughtful approach to how you communicate your status to future partners.
Treatment Options, What They Do, and What They Don't
There is no cure for herpes, but there is effective treatment, and the distinction between those two things matters more than most people realize when they first hear the diagnosis. Treatment doesn't eliminate the virus. What it does is give you meaningful control over what the virus does: how often outbreaks occur, how severe they are when they do, how long they last, and how likely you are to transmit the virus to a partner. For many people, that level of control is the practical difference between herpes being a constant presence in their life and it being something they rarely think about.
Antiviral treatment for herpes works in two distinct modes, serving different goals. Episodic therapy is taken at the first sign of an outbreak, during the prodromal tingling or immediately when sores begin to appear. CDC STI treatment guidelines confirm that episodic antiviral therapy shortens the duration and severity of individual outbreaks when started early, with the greatest benefit when treatment begins during the prodromal phase before lesions develop. For someone who has infrequent outbreaks and mainly wants to reduce their duration and discomfort, episodic therapy taken on-demand is the most practical approach.
Suppressive therapy is taken daily, continuously, regardless of whether an outbreak is occurring. Its purpose is different from episodic therapy: rather than treating an outbreak after it starts, suppressive therapy reduces the frequency of outbreaks, reduces the amount of viral shedding between outbreaks, and, importantly, reduces the risk of transmitting herpes to an uninfected partner. A landmark clinical trial published in PMC found that daily suppressive antiviral treatment reduced the risk of symptomatic genital herpes transmission to a susceptible partner by approximately 75%, and reduced overall HSV-2 acquisition by approximately 50% in serodiscordant couples. For people who have frequent outbreaks, for people in serodiscordant relationships who want to reduce transmission risk, or for people whose quality of life is significantly affected by the psychological burden of the infection regardless of outbreak frequency, daily suppressive therapy is clinically appropriate and widely used.
Neither approach is permanent. People can move between episodic and suppressive therapy depending on their circumstances, starting suppressive therapy when entering a new relationship, or stopping it if their situation changes. The decision is a conversation with a healthcare provider, not a one-time irreversible commitment. What both approaches share is that they work best when started with accurate information: knowing your HSV type (HSV-1 versus HSV-2) matters clinically because genital HSV-1 recurs less frequently and may not warrant ongoing suppressive therapy in the same way that frequent-recurrence HSV-2 often does. Testing isn't just the beginning of understanding your status, it informs which management approach actually makes sense for your situation.
People are also reading: At-Home STD Testing: How It Works, How Accurate It Is, and What to Do With the Results
Reducing Transmission Risk, What the Research Actually Shows
Prevention of herpes transmission is one of the most misunderstood areas of sexual health, partly because the answer is genuinely more complicated than it is for infections transmitted through body fluids. Herpes is a skin-to-skin contact virus that sheds asymptomatically, which means some of the standard risk-reduction tools that work well for chlamydia or gonorrhea are less effective for herpes, and some people who do everything right still occasionally transmit the virus. Understanding what the evidence actually shows about each prevention tool, rather than overstating or understating any of them, is what allows people to make genuinely informed decisions.
Condoms reduce herpes transmission risk, but by a more modest margin than most people assume and in a way that differs by sex. A large pooled analysis of prospective studies published in PMC, covering 5,384 participants and over two million follow-up days, found that consistent condom use was associated with approximately a 30% reduction in HSV-2 acquisition overall. The reason condoms are less effective against herpes than against fluid-transmitted infections is biological: herpes is present on skin surfaces that a condom doesn't cover, the perineum, the upper thighs, the buttocks, and transmission can occur from those uncovered areas. Condoms still matter and should be used consistently in serodiscordant relationships; a 30% reduction in risk is clinically meaningful. But they are not a complete solution in the way they are for chlamydia or gonorrhea.
Suppressive antiviral therapy has a stronger evidence base for reducing transmission than condoms do. The landmark valaciclovir transmission trial referenced in the previous section found that daily suppressive therapy in the HSV-positive partner reduced the risk of symptomatic herpes transmission to an uninfected partner by 75%, and reduced overall HSV acquisition by approximately 50%. CDC guidance on HSV-2 management explicitly recommends daily antiviral therapy as a strategy to reduce both clinical and subclinical reactivation and to reduce transmission risk to uninfected partners. Suppressive therapy and consistent condom use used together represent the most effective combination strategy currently available for serodiscordant couples, not a guarantee of zero transmission, but a meaningful and evidence-backed reduction in risk.
| Strategy | Estimated Risk Reduction | Evidence Source | Key Limitation |
|---|---|---|---|
| Consistent condom use | ~30% reduction in HSV-2 acquisition overall; higher for female partners | PMC pooled analysis of 5,384 participants (Martin et al.) | Doesn't cover all shedding sites; less effective than for fluid-transmitted STIs |
| Daily suppressive antiviral therapy | ~75% reduction in symptomatic transmission; ~50% reduction in overall acquisition | PMC landmark valaciclovir transmission trial | Reduces but doesn't eliminate asymptomatic shedding |
| Avoiding contact during outbreaks and prodrome | Removes the highest-risk period; clinically significant | CDC STI Treatment Guidelines 2021 | Asymptomatic shedding continues between outbreaks |
| Suppressive therapy + condoms combined | Greatest cumulative risk reduction of any available strategy | CDC guidance; clinical consensus | No strategy reduces transmission risk to zero |
Avoiding sexual contact during outbreaks and the prodromal phase is the third component, and in many ways the most intuitive. Viral load is highest during active outbreaks, which means transmission risk is also highest at that time. Recognizing and responding to prodromal symptoms, tingling, itching, or burning that precedes a visible sore, as a signal to avoid sexual contact is a practical risk-reduction step that carries real clinical weight. The honest answer about prevention is that none of these measures, individually or together, eliminates transmission risk entirely. Herpes is biologically unusual in that asymptomatic shedding makes complete prevention difficult even with perfect adherence. What the combination of suppressive therapy, consistent condom use, and outbreak awareness achieves is a substantial reduction in risk that allows most serodiscordant couples to maintain an active sexual relationship with informed, manageable risk, rather than facing an impossible binary of total abstinence or unmitigated exposure.
Relationships, Disclosure, and What Living With Herpes Actually Looks Like
The relationship question is usually the one that feels most urgent after a diagnosis, and it gets the least honest treatment in most online resources. So here is the honest version. People with herpes have normal relationships. They have satisfying sex lives. They get married. They raise families. They date successfully. The fear that a herpes diagnosis ends your romantic life is almost entirely a product of stigma, not biology, and the stigma, while real and genuinely painful, is not the same as the medical picture.
Disclosure, telling a new partner about your herpes status before sexual contact, is both an ethical obligation and, practically, less catastrophic than most people anticipate before they've done it. The fear of disclosure is usually worse than the experience. Partners who respond with rejection after disclosure are often operating on the same misinformation about herpes that you likely had before your diagnosis. Partners who are informed, who understand the actual transmission risk and what reduces it, and who care about the person in front of them typically respond differently. There is no single script for this conversation, and the timing (early in a relationship versus closer to sexual activity) depends on personal values and relationship context. What doesn't change: disclosure before sexual contact is the standard, and it is more manageable than the anticipatory anxiety about it suggests.
For couples where one partner is HSV-positive and one is not (serodiscordant couples), the data on transmission risk and reduction strategies is actionable. CDC clinical guidance indicates that daily suppressive antiviral therapy, consistent condom use, and avoiding sexual contact during outbreaks and prodromal symptoms each independently reduce transmission risk, and the combination of all three reduces it substantially. This is not a guarantee of zero transmission risk, but it is a meaningful risk reduction that allows couples to navigate the situation with information rather than fear. Many serodiscordant couples find that the conversation around herpes management becomes integrated into their relationship without defining it, one more practical health consideration among many.
The emotional impact of a herpes diagnosis is real and should not be minimized. Shame, fear of rejection, anger, grief about a changed sense of self, these are normal responses that many people experience. They also, for most people, diminish significantly over time as the diagnosis becomes integrated into a fuller understanding of what herpes actually is, how manageable it is, and how little it defines the life being lived. Support communities exist online and offline for people navigating this, and a therapist familiar with sexual health issues can be genuinely useful for processing the diagnosis in its early stages. The diagnosis is a piece of medical information. What you do with it, how you manage the virus, how you communicate with partners, how you think about yourself, is where your agency actually lives.

People are also reading: Can You Get an STD in a Relationship? The Complete Guide for Couples
FAQs
1. Can you have herpes and not know it?
Yes, and this is the norm, not the exception. The American Sexual Health Association cites CDC data indicating that up to 90% of people with genital HSV-2 are unaware they carry it. HSV-1 unawareness is even higher. The virus frequently produces no recognizable symptoms, or symptoms so mild they're attributed to something else. Herpes is also not included in standard STI panels in most clinical settings, meaning most people have never been specifically tested for it regardless of how many times they've been tested for other infections.
2. What's the difference between a cold sore and herpes?
There is no difference, cold sores are herpes. A cold sore is caused by HSV-1, the most common strain of herpes simplex virus, which affects roughly half to two-thirds of all adults. The cultural split between "cold sores" (socially acceptable) and "herpes" (stigmatized) has no basis in virology. They are the same virus, managed differently partly because of where they appear and partly because of how long society decided one version was acceptable and the other wasn't.
3. Can HSV-1 (oral herpes) cause genital herpes?
Yes, and this is increasingly common. When someone with oral herpes performs oral sex on a partner who hasn't previously been exposed to HSV-1, that partner can develop genital HSV-1. A 2024 systematic review in Cell Reports Medicine confirmed that the proportion of genital herpes cases caused by HSV-1 is rising in developed countries, largely because improved childhood hygiene means fewer people have prior oral HSV-1 immunity before becoming sexually active.
4. Can you get herpes without having sex?
For HSV-1, yes, it is commonly transmitted through non-sexual contact, primarily kissing and sharing utensils or lip products during an active oral outbreak. Many people acquire it in childhood or adolescence this way. For HSV-2, sexual contact is the primary transmission route, though non-sexual skin-to-skin contact in the genital area is theoretically possible. You cannot get either strain from toilet seats, towels, swimming pools, or any form of casual non-intimate contact.
5. When should I test for herpes after an exposure?
The testing window for blood-based IgG antibody tests is 6 weeks after exposure for both HSV-1 and HSV-2. Testing before 6 weeks risks a false negative, not because the test is inaccurate, but because IgG antibodies take time to reach detectable levels. If you test negative before the window closes, retest after it does. If you have visible sores, a viral culture or PCR swab test during the active outbreak is more sensitive for confirming a current infection than a blood test.
6. Is a positive herpes test always accurate?
At index values clearly above the positive threshold, blood-based IgG herpes tests are highly reliable. The accuracy nuance arises at low-positive index values (1.1–3.5), where false-positive rates are higher. If you receive a low-positive result with no history of recognizable symptoms, a confirmatory Western Blot test, the gold standard for herpes serology, is worth requesting before drawing conclusions. Clearly positive results at high index values are reliable and don't typically require confirmation.
7. Can herpes be spread without visible sores?
Yes, this is one of the most important things to understand about herpes transmission. Asymptomatic viral shedding, where the virus is active on the skin surface without any visible lesion, occurs between 5% and 20% of the time in infected individuals according to public health data. This is the primary mechanism by which most herpes transmission occurs, between people who have no active sores and no reason to suspect they're contagious.
8. What triggers herpes outbreaks?
Common outbreak triggers include physical stress on the body (illness, fever, surgery), emotional stress, hormonal changes (particularly around menstruation for people with HSV-2 or genital HSV-1), sun exposure for oral herpes (UV light can trigger cold sore outbreaks), friction or trauma to the affected area, and immune suppression from illness or medication. Not everyone experiences the same triggers, and some people find their outbreaks occur without any identifiable precipitating factor.
9. Can herpes affect pregnancy?
Yes, though the risk profile is specific. Primary HSV infection (first-time infection) acquired late in the third trimester carries the highest transmission risk to the newborn during delivery, potentially 30–50%, because the mother hasn't yet developed protective antibodies. Recurrent herpes in a pregnant person who has carried the virus for some time carries much lower transmission risk, and standard obstetric management includes suppressive antiviral therapy in the final weeks of pregnancy to reduce outbreak risk during delivery. If you have herpes and are pregnant or planning to become pregnant, this is a conversation to have explicitly with your OB, early identification and management significantly reduces neonatal risk.
10. Does a herpes diagnosis mean my relationship is over or my sex life is ruined?
No. People with herpes have relationships, get married, have active sex lives, and raise families. The fear that a diagnosis ends normal romantic life is one of the most persistent and most inaccurate aspects of herpes stigma. Disclosure to partners, combined with practical risk-reduction approaches (suppressive therapy, consistent condom use, avoiding contact during outbreaks), allows most people to navigate relationships with their herpes status as one consideration among many rather than a defining barrier. The anticipatory fear of disclosure is typically worse than the actual experience of it.
Testing Is How You Get Real Information About Your Status
Herpes is common, manageable, and in the majority of cases invisible, which is exactly why most people carrying it don't know, and exactly why testing matters. A negative result after the window period tells you something real. A positive result gives you information you can actually do something with: talk to a healthcare provider about management, make informed decisions about disclosure, and reduce transmission risk for partners. Neither outcome is improved by not knowing.
If you want to test specifically for herpes, the HSV-1 and HSV-2 combined rapid test covers both strains at 98.2% accuracy, with results in twenty minutes at home. For comprehensive STI coverage that includes herpes alongside seven other major infections, the Complete 8-in-1 kit gives you the full picture in one session. Women who want the most complete panel available, including HPV and trichomoniasis, will find everything in the Women's 10-in-1 kit. The full range is at STD Rapid Test Kits. Test from 6 weeks after exposure. Know where you stand.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. World Health Organization, Herpes Simplex Virus Fact Sheet (2025)
2. CDC / NCHS Data Brief No. 304, Prevalence of HSV-1 and HSV-2 in the United States, 2015–2016
5. PMC, A Pooled Analysis of the Effect of Condoms in Preventing HSV-2 Acquisition (Martin et al.)
6. PMC, Reducing the Transmission of Genital Herpes: Antiviral Suppressive Therapy Efficacy Trial
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.