Can You Get Tested for STDs While on PrEP? The Truth About Results and Timing
Last updated: April 2026
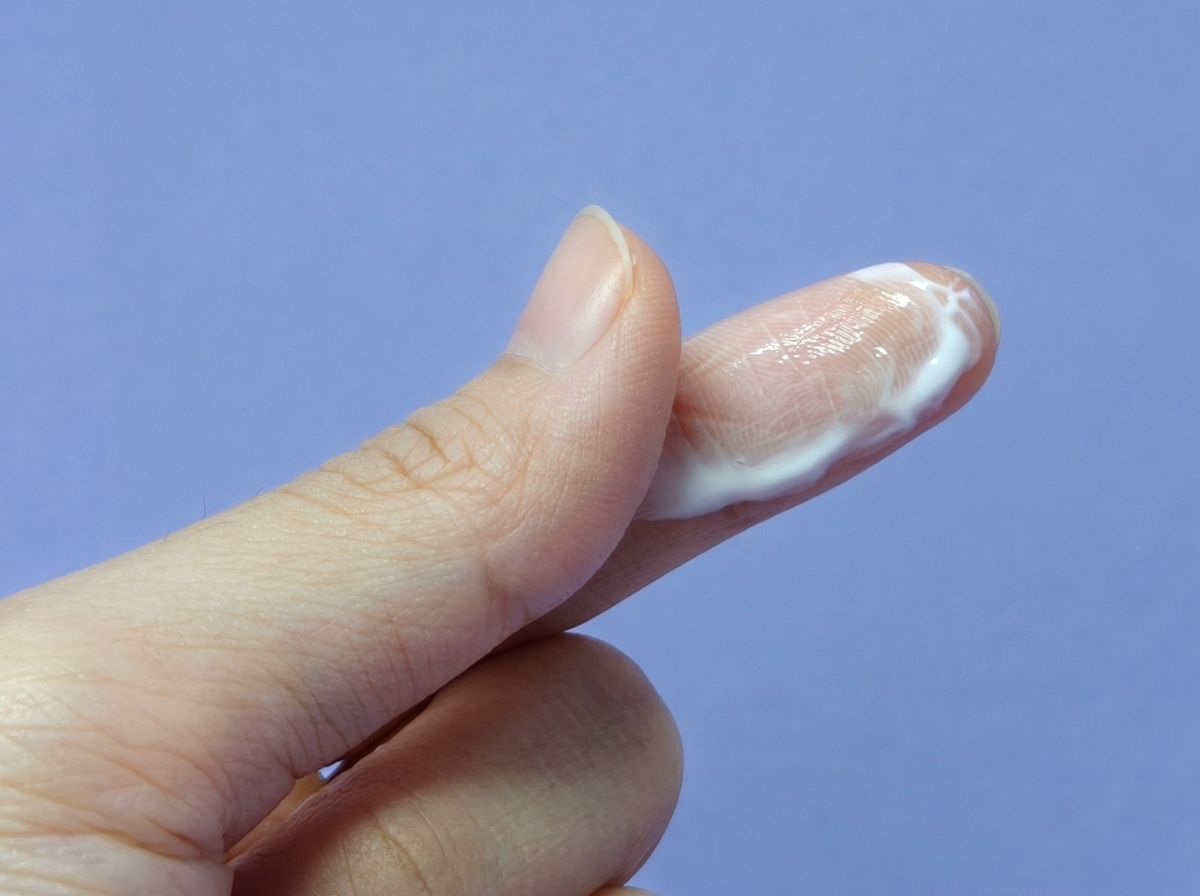
The short answer: Most vaginal discharge is completely normal. Clear, white, or off-white discharge that doesn't smell bad is your body doing its job. Yellow, green, or gray discharge, especially with an unusual odor, is more likely to signal an infection, including STDs like chlamydia, gonorrhea, or trichomoniasis. Brown discharge is almost always period-related. Any discharge accompanied by itching, burning, or a strong fishy or foul smell warrants a closer look, and often a test.
The longer answer requires understanding what discharge is in the first place. Your vagina continuously produces fluid, a mix of cells, bacteria, and secretions from the cervix, that flushes out debris and maintains the delicate bacterial ecosystem inside. This is healthy. The color, consistency, and volume of that fluid shifts throughout your cycle, and knowing those normal patterns is the single most useful tool for catching something that actually needs attention.
People are also reading: Do You Need a Follow-Up STD Test After Treatment? What Each Infection Actually Requires
What Normal Vaginal Discharge Looks Like
Before getting into what's abnormal, it's worth being clear about the baseline. Normal discharge is clear to white or slightly off-white. It tends to be odorless or very mildly scented. Its texture changes throughout the menstrual cycle, watery and stretchy around ovulation (that characteristic egg-white consistency), thicker and creamier in the days before a period, and sometimes barely noticeable in between. Volume also fluctuates naturally: higher around ovulation, during sexual arousal, and in the days before menstruation.
If your discharge fits that description, nothing is wrong. Your vagina is working exactly as intended. The issue is that "clear to white" covers a broad range, and that range overlaps with some early infection presentations, which is precisely where the confusion starts.
One thing worth knowing: discharge volume tends to increase throughout the reproductive years and can be noticeably heavier during pregnancy or when using certain hormonal contraceptives. That's normal. The thing to pay attention to isn't so much the volume as the combination of color, smell, and any accompanying symptoms like itching or burning.
White Discharge: Normal Until It Isn't
White discharge is the most common and, most of the time, the least concerning. Thick, creamy white discharge that appears before your period and has no accompanying odor or irritation is simply part of the luteal phase of your cycle, hormonal, healthy, and nothing to worry about.
The white discharge that deserves attention looks different. Thick, clumpy, cottage-cheese-like white discharge, particularly when it comes with intense itching, burning, or vulvar swelling, is the classic presentation of a yeast infection (vaginal candidiasis). Yeast infections aren't sexually transmitted; they result from an overgrowth of Candida, a fungus that normally lives in the vagina in small amounts. Antibiotics, hormonal changes, high blood sugar, and a compromised immune system are all common triggers. The discharge itself is characteristically odorless, which distinguishes it from the fishy-smelling discharge of bacterial vaginosis.
Another white presentation to know: thin, watery white discharge with a noticeable fishy odor, especially if the smell intensifies after sex, is a hallmark of bacterial vaginosis (BV). BV isn't an STD in the traditional sense, but it is associated with changes in sexual partners and the disruption of the vaginal microbiome. According to a 2025 updated review in StatPearls, bacterial vaginosis is one of the most common vaginal infections in women aged 15–44, and the discharge is typically thin and gray-white rather than thick.
White discharge is not typically a sign of chlamydia or gonorrhea on its own, though both can occasionally produce a whitish or off-white discharge. If white discharge comes with pelvic pain, bleeding between periods, or burning during urination after sexual contact, testing for STDs is a reasonable next step regardless of the color.
Yellow Discharge: The Color That Needs Context
Yellow discharge is where a lot of women panic unnecessarily, and sometimes miss something important. The key is context. Pale yellow discharge with no smell and no other symptoms, particularly at certain points in your cycle, can fall within the normal range. Discharge that's clearly yellow, has a noticeable odor, or comes with any other symptom is a different story.
The two most common STD-related causes of yellow discharge are chlamydia and gonorrhea. Both are bacterial infections that frequently cause a yellowish or greenish-yellow discharge from the vagina or cervix. The critical thing about both is that they're usually asymptomatic, most people with chlamydia or gonorrhea have no symptoms at all. When symptoms do appear, the American College of Obstetricians and Gynecologists notes that yellow discharge from the vagina or urethra is among the most reported, along with bleeding between periods and pain during urination.
Trichomoniasis, a parasitic STD that's actually more prevalent in the US than gonorrhea and chlamydia combined, also commonly produces yellow discharge, often described as frothy or bubbly with a particularly unpleasant fishy odor. According to the CDC, about 70% of people with trichomoniasis have no symptoms at all, which makes the infection notoriously easy to carry and transmit without knowing. When symptoms do appear, they typically include yellow-green frothy discharge, vaginal odor, itching, and discomfort during urination or sex.
Yellow discharge after unprotected sex, especially with a new partner, is a genuine reason to test. It doesn't confirm an STD, but it's a reliable enough signal that waiting to see if it resolves on its own isn't the right call. Chlamydia and gonorrhea in particular are both easily treatable when caught early, and both can cause serious complications like pelvic inflammatory disease (PID) if left untreated.
| Appearance | Likely Cause | Other Symptoms to Look For |
|---|---|---|
| Pale yellow, no odor, no symptoms | Possibly normal (cycle-related) | None, monitor only |
| Yellow, slight odor, thin texture | Bacterial vaginosis | Fishy smell, mild itching |
| Yellow or greenish, cloudy | Chlamydia or gonorrhea | Often no symptoms; may have pelvic pain, burning urination |
| Yellow-green, frothy, strong odor | Trichomoniasis | Itching, soreness, pain during sex or urination |
Green Discharge: Take This One Seriously
Green vaginal discharge is not normal. It's one of the clearest visual signals that something is off, and it typically points to a bacterial infection or STD. The two most common culprits are trichomoniasis and gonorrhea, both of which can produce a distinctly green or yellow-green discharge, often frothy and foul-smelling in the case of trich, and thicker and cloudier in the case of gonorrhea.
You're lying in bed after noticing something that looks decidedly green when you wipe, and you're trying to convince yourself it's just the lighting. It's usually not the lighting. Green discharge is the body's fairly unambiguous way of signaling that there's a significant bacterial or parasitic presence that needs addressing.
Gonorrhea is particularly worth flagging here because it's increasingly resistant to antibiotics. The World Health Organization has flagged gonorrhea as a serious antimicrobial resistance concern globally, with some strains now resistant to multiple antibiotic classes. This makes early detection and treatment more important than ever, catching it while standard treatments are still effective is the goal. Waiting until symptoms are severe narrows the treatment options.
Green discharge can also occur with BV in some cases, though the classic BV presentation is gray-white rather than green. If the discharge is green and comes with pelvic pain, fever, or bleeding between periods, pelvic inflammatory disease (PID), a serious complication of untreated STDs, is a possibility that requires immediate medical attention.
The bottom line on green discharge: test, don't wait. There is no plausible normal explanation for green vaginal discharge. It needs to be investigated.
People are also reading: That Rash That Won't Quit After Sex Might Not Be Jock Itch
Gray Vaginal Discharge: What It Means and When to Worry
Gray discharge is almost always bacterial vaginosis. BV is caused by an overgrowth of anaerobic bacteria in the vagina, specifically a disruption in the normal dominance of Lactobacillus species, and produces a thin, grayish or gray-white discharge with a distinctive fishy odor that tends to be strongest after sex or during menstruation. The pH of the vagina rises above its healthy acidic range, which is what gives that characteristic smell.
BV is not technically an STD; it can occur in women who've never had sex, but it is strongly associated with changes in sexual partners, unprotected sex, douching, and other disruptions to the vaginal environment. What makes it particularly worth taking seriously is that BV significantly increases the risk of acquiring an STD if you're exposed to one: the disrupted vaginal microbiome provides less protection against incoming pathogens. It also increases susceptibility to HIV.
The other thing about BV: it's extremely common, often asymptomatic, and highly recurrent. Many women treat a BV episode with antibiotics, feel fine for a few weeks, and then find themselves back in the same situation. If you're dealing with recurring gray discharge and fishy odor, that cycle is worth discussing with a healthcare provider rather than just repeating antibiotic treatment indefinitely.
One important distinction: gray discharge is not a sign of chlamydia, gonorrhea, or trichomoniasis specifically. But because BV and STDs frequently coexist, and because BV can mask or mimic early STD presentations, testing for both when you have gray discharge after a new sexual encounter makes clinical sense.
Brown Discharge: What It Actually Means at Every Stage of Life
Brown discharge triggers more alarm than it almost ever deserves, and that's largely because the internet tends to jump straight to worst-case explanations. In the vast majority of cases, brown discharge is simply old blood. Blood that takes longer to exit the body oxidizes as it travels, turning darker shades of red, rust, and eventually brown. That process is completely normal and happens to most women at some point in their cycle.
Brown discharge at the very beginning or end of your period is one of the most common experiences in reproductive health. As your uterine lining starts or finishes shedding, the flow slows down and the blood has more time to oxidize before it exits, producing that characteristic dark brown or rusty color. This is not a sign of anything wrong. It's just your period tapering off or warming up. Light brown spotting in the middle of your cycle can also occur around ovulation in some women, when a small amount of blood is released alongside the egg. Again, entirely normal if it's brief and doesn't recur in a concerning pattern.
Early pregnancy is another very common cause of brown discharge. Implantation bleeding, which occurs when a fertilized egg attaches to the uterine lining, typically 6–12 days after conception, often appears as light pink or brown spotting rather than red. It's usually brief, lighter than a period, and not accompanied by significant cramping. Many women mistake it for the start of an early period. If you've had recent unprotected sex and notice light brown spotting around the time your period would be due, a pregnancy test is a reasonable first step.
| When It Appears | Most Likely Cause | Action |
|---|---|---|
| Start or end of period | Old blood from uterine shedding, normal | No action needed |
| Mid-cycle, brief and light | Ovulation spotting, normal | Monitor; no action if it resolves quickly |
| Around expected period date, after unprotected sex | Possible implantation bleeding | Take a pregnancy test |
| Between periods, recurring or persistent | Hormonal imbalance, cervical irritation, STD-related spotting | See a provider; consider STD test if sexually active |
| After sex, repeatedly | Cervical inflammation, possible STD (chlamydia, gonorrhea) | Test for STDs; see provider |
| Postmenopausal women, any amount | Requires evaluation, atrophy, polyps, or rarely cancer | See a provider promptly |
The brown discharge situations that genuinely warrant a closer look are fewer but important to know. Persistent brown discharge between periods, meaning it's happening regularly outside of your normal cycle pattern and isn't explained by ovulation or a new contraceptive, deserves a gynecological evaluation. The same applies if brown discharge is accompanied by pelvic pain, an unusual odor, or fever. A foul-smelling brown discharge in particular can indicate an infection rather than simple old blood, and that combination should be assessed promptly.
Brown discharge after sex, especially if it happens more than once, is worth taking seriously. Repeated post-sex bleeding or spotting, which can appear brown if it's light, is often caused by cervical inflammation or irritation. Two of the most common STD-related causes of that inflammation are chlamydia and gonorrhea, both of which can make the cervix more fragile and prone to bleeding on contact. Neither infection typically produces brown discharge as its primary symptom, but both can cause the kind of cervical irritation that results in spotting after intercourse.
For postmenopausal women, the calculus changes entirely. Any vaginal bleeding or brown discharge after menopause, even a tiny amount, should be evaluated by a healthcare provider without delay. Postmenopausal bleeding is not automatically cancer, and in most cases it isn't. Vaginal atrophy, polyps, and hormonal changes account for the majority of cases. But it is the symptom most associated with endometrial cancer when it does occur, and early detection matters significantly for outcomes. This is one context where "wait and see" is genuinely the wrong approach.
One final thing worth saying: brown discharge is not a characteristic presentation of chlamydia, gonorrhea, or trichomoniasis. If you're seeing brown discharge and wondering whether you have an STD, the color itself isn't the indicator to focus on. Focus instead on whether the discharge has an unusual odor, whether it's appearing after sex, whether it's accompanied by pelvic discomfort, and whether you've had any recent unprotected sexual contact. Those factors, not the color alone, are what determine whether STD testing makes sense.
At-Home STD Testing: When to Test and What to Test For
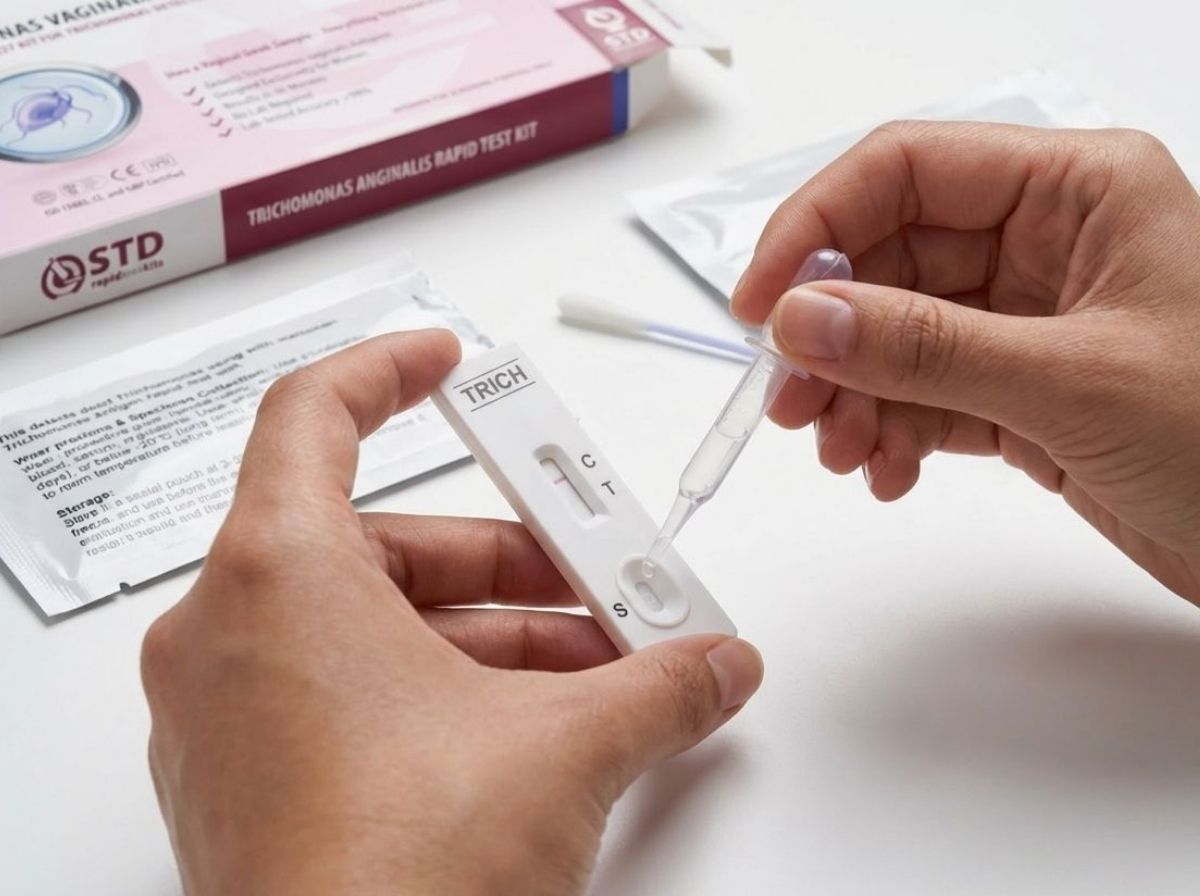
If you've noticed a change in discharge, particularly yellow, green, or gray discharge with an odor, and you've had recent sexual contact with a new or untested partner, testing is the single most useful thing you can do. Not because the discharge definitely means you have an STD, but because the only way to tell the difference between BV, a yeast infection, trichomoniasis, chlamydia, and gonorrhea with any certainty is to test. Symptoms and colors overlap too much to diagnose reliably from appearance alone.
At-home rapid STD test kits make this straightforward. No clinic visit, no waiting room, no explaining your situation to a receptionist. You collect a sample at home, and results are available in minutes. For discharge-related concerns, the most relevant infections to test for are chlamydia, gonorrhea, trichomoniasis, and, if there's been genital contact, herpes. Use these exact testing windows for accurate results:
Chlamydia: test from 14 days after exposure. Gonorrhea: test from 3 weeks after exposure. Trichomoniasis: test from 5–28 days after exposure (symptoms can appear within that window). Syphilis: test from 6 weeks after exposure. HIV: test at 6 weeks for a first indicator result, then retest at 12 weeks for certainty. Herpes HSV-1 and HSV-2: test from 6 weeks after exposure. Hepatitis B: test from 6 weeks after exposure. Hepatitis C: test from 8–11 weeks after exposure.
| Color | Most Likely Cause | STD Possible? | Action |
|---|---|---|---|
| Clear / white, no odor | Normal discharge | No | No action needed |
| Thick white, cottage cheese texture | Yeast infection | No | OTC antifungal; see provider if recurring |
| Thin white / gray, fishy odor | Bacterial vaginosis | Unlikely (but increases STD risk) | See provider; consider STD test if new partner |
| Yellow, cloudy or odorous | Chlamydia, gonorrhea, or BV | Yes, likely | Test for chlamydia and gonorrhea |
| Yellow-green, frothy, foul odor | Trichomoniasis | Yes, very likely | Test for trichomoniasis; also test for other STDs |
| Green, thick or frothy | Gonorrhea or trichomoniasis | Yes, test immediately | Test for gonorrhea and trichomoniasis |
| Brown, around period | Old blood / normal cycle variation | Rarely | Monitor; see provider if persistent or mid-cycle |
For women dealing with abnormal discharge after a new sexual encounter, the Female STD Test Kits range is designed specifically with female-pattern infections in mind. The Trichomoniasis At-Home Rapid Test Kit (98.38% accuracy) is the most targeted option if the discharge presentation matches trich. For broader coverage, including chlamydia, gonorrhea, syphilis, HIV, and more, the Women's 10-in-1 Complete STD Home Test Kit covers all ten of the most common infections in a single session. Testing is the fastest way to stop the guessing game and get to an answer.
Check Your STD Status in Minutes
Test at Home with Remedium10-in-1 STD Test Kit

 For Women
For Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $189.00 $490.00
For all 10 tests
The STDs Most Likely to Change Your Discharge
Not every STD affects discharge. HIV, herpes, and syphilis don't typically cause discharge changes as a primary symptom. The ones that do, and the ones most worth knowing about in this context, are chlamydia, gonorrhea, and trichomoniasis. Here's what distinguishes each one.
Chlamydia is the most commonly reported STD in the United States. Most women with chlamydia have no symptoms at all, which is exactly what makes it dangerous, it can quietly cause fallopian tube damage and infertility before anyone knows it's there. When discharge does occur, it's typically yellow or off-white, sometimes with a mild odor, and may be accompanied by bleeding between periods or after sex. The CDC recommends annual chlamydia screening for all sexually active women under 25, and for older women with new or multiple partners, partly because the infection is so often silent.
Gonorrhea overlaps significantly with chlamydia in its presentation. Yellow or greenish discharge, possible bleeding between periods, burning urination, and in many cases, no symptoms at all. Gonorrhea's particular risk is its growing antimicrobial resistance, which makes prompt detection and treatment more important than it used to be. Left untreated, it can progress to PID, potentially causing permanent damage to the reproductive system. The two infections frequently coexist, which is why testing for both simultaneously is standard practice.
Trichomoniasis is the most common non-viral STD in the United States, and it's dramatically underscreened. Research published in NCBI shows that trichomoniasis infection rates in the US are higher than gonorrhea and chlamydia combined. Unlike chlamydia and gonorrhea, which peak in women under 25, trichomoniasis is as common in women over 40 as in younger women. The discharge presentation is the most distinctive of the three: yellow-green, frothy or bubbly, with a strong fishy or foul odor. Around 70% of infections are asymptomatic, meaning most people who have it don't know.
What to Do If Your Discharge Changes
The practical framework is simple. If your discharge changes, in color, smell, texture, or volume, and doesn't return to normal within a few days, pay attention to it. If it's accompanied by any of the following, don't wait:
Itching or burning in the vaginal area. Pain during sex or urination. Pelvic pain or pressure. Bleeding between periods or after sex. A noticeably fishy, foul, or unfamiliar odor. Any discharge that is yellow, green, or gray in color after recent sexual contact.
None of these on their own guarantees an STD, yeast infections and BV are far more common than most STDs and can produce overlapping symptoms. But the only way to know with certainty what you're dealing with is to test. Color and smell don't distinguish between BV and gonorrhea reliably enough to skip testing when there's been potential STD exposure.
A note worth making: many women treat what they assume is a yeast infection with an over-the-counter antifungal and feel better, only to have symptoms return weeks later. If that cycle sounds familiar, it may be because the original issue was BV or a low-grade STD, not yeast, and the antifungal didn't address it. Testing is always more accurate than self-diagnosis from symptoms alone.
People are also reading: Treated for an STD? Here's Everything You Need to Do Before Having Sex Again
FAQs
1. Does yellow discharge always mean you have an STD?
No, but it can be. Pale yellow discharge that doesn't smell or hurt can be normal, especially at certain times of the cycle. If your discharge is clearly yellow, smells strange, or comes with other symptoms like itching, burning, or pain in the pelvic area, it is more likely to mean you have an infection. If you have yellow discharge after having unprotected sex with a new partner, you should get tested for chlamydia, gonorrhea, and trichomoniasis even if you don't have any other symptoms.
2. What does the discharge from trichomoniasis look like?
Trichomoniasis usually causes a yellow-green, frothy or bubbly discharge that smells very bad like fish. It's one of the most visually unique ways to show discharge. That being said, about 70% of people with trichomoniasis don't have any symptoms at all. This is why not having this specific discharge doesn't mean you don't have it after being exposed.
3. Is it possible to have chlamydia or gonorrhea without any discharge?
Yes, all the time. Most women with chlamydia and gonorrhea don't have any noticeable symptoms. Discharge that does happen is usually yellow or cloudy, but many infections don't show up in any way that you can see. This is why it's important to get tested regularly; you can't just look at your symptoms to know your status.
4. What is the difference between STD discharge and BV discharge?
The discharge from BV is usually thin, gray-white, and smells like fish. The smell gets stronger after sex. Discharge from an STD like gonorrhea, chlamydia, or trichomoniasis is usually yellow, green, or frothy, not gray-white. The smell of STD-related discharge is often bad, but it is not the same as BV's fishy smell. That said, the overlap is big enough that testing is more reliable than just looking at the discharge to figure out what's wrong.
5. If I notice strange discharge, how soon should I test after sex?
It depends on the type of infection you're testing for. Wait 14 days for chlamydia. Wait three weeks for gonorrhea. Symptoms of trichomoniasis can show up anywhere from 5 to 28 days after infection, so testing during that time is fine. Testing too soon can give a false negative, even if there is an infection, because the body needs time to make enough of the pathogen or antibodies for the test to find them.
6. Is it always bad to have green discharge?
Yes, green discharge from the vagina is not normal and should always be looked into. Most of the time, it means you have a bacterial or parasitic infection, like gonorrhea or trichomoniasis. There is no normal reason for green discharge to happen. Don't wait to see if it goes away on its own; go to a provider or test at home right away.
7. Can a yeast infection make your discharge yellow or green?
No. The discharge from a yeast infection is thick, white, and smells bad. People often say it looks like cottage cheese. A yeast infection does not show up as yellow or green discharge. If you have yellow or green discharge and think it's a yeast infection, you're probably dealing with something else, and an over-the-counter antifungal won't help.
8. What does the smell of normal discharge smell like?
Normal vaginal discharge has a mild, slightly tangy or acidic smell. This is the natural smell of a healthy vaginal environment that is full of Lactobacillus bacteria. It shouldn't smell bad, fishy, or strong. One of the most reliable signs that something has changed in the vaginal microbiome is a noticeable change in smell, like a new fishy or very unpleasant smell.
9. I have gray discharge, but it doesn't smell. Could it still be BV?
Yes. The fishy smell is the most common sign of BV, but not everyone with it notices a strong smell. Some women only notice a change in discharge without a strong smell. Getting checked out is important if you have gray or grayish-white thin discharge on its own, especially after having sex for the first time or taking antibiotics. A vaginal pH test or swab from a doctor or clinic can quickly show that you have BV.
10. Is it possible for me to have more than one infection at the same time that is causing discharge?
Yes, and more often than most people think. BV and trichomoniasis often happen at the same time. Chlamydia and gonorrhea are frequently co-occurring. BV makes it easier to get STDs, so it's possible to have more than one infection at the same time. This is why it's better to do a full test instead of just testing for one infection when the discharge is clearly abnormal.
Test at Home, Know Exactly What You're Dealing With
Abnormal discharge is your body flagging something that deserves a clear answer, not a guessing game between OTC treatments. At-home rapid test kits give you that answer in minutes, without a clinic visit or a referral.
For women specifically concerned about discharge changes after a new partner, the Trichomoniasis At-Home Rapid Test Kit (98.38% accuracy) and the Chlamydia and Gonorrhea 2-in-1 At-Home Test Kit (98% accuracy) cover the three STDs most likely to cause discharge changes. For the most comprehensive picture, covering all ten of the most common STDs including HPV and trichomoniasis, the Women's 10-in-1 Complete STD Home Test Kit is the gold standard. Browse the full Female STD Test Kits range to find the right option for your situation, or visit STD Rapid Test Kits for everything available. Your results, your privacy, your peace of mind.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. Centers for Disease Control and Prevention, About Trichomoniasis
2. Centers for Disease Control and Prevention, STI Treatment Guidelines: Vaginal Discharge
3. American College of Obstetricians and Gynecologists, Chlamydia, Gonorrhea, and Syphilis
4. StatPearls / NCBI, Bacterial Vaginosis (Updated 2025)
5. StatPearls / NCBI, Trichomoniasis
6. World Health Organization, Gonorrhoea Fact Sheet
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.










