Last updated: April 2026
In February 2026, the Minnesota Department of Health issued a statewide health advisory declaring the largest known outbreak of a sexually transmitted fungal infection in US history. The culprit: a fungal strain called TMVII, Trichophyton mentagrophytes genotype VII, the only known sexually transmitted fungal infection in the world. More than 30 confirmed or suspected cases had clustered in the Twin Cities metropolitan area since July 2025, and the infection had already been quietly confirmed in New York City, San Francisco, and other major cities. The reason it spread so far before being caught is the same reason it is so hard to treat once identified: it looks exactly like something far more ordinary.
TMVII causes painful, coin-shaped ringworm rashes on the genitals, buttocks, inner thighs, face, and trunk. It spreads through direct skin-to-skin contact during sex, survives on shared towels and bedding, and will not respond to the antifungal cream you pick up at the pharmacy. Treating it incorrectly, especially with a corticosteroid cream, actively makes it worse. This is a new infection, and the information gap between what is actually happening and what most doctors are equipped to recognize is a real problem.

People are also reading: Can I Take a Home STD Test?
What Happened in Minnesota, And Why It Matters Nationally
On February 11, 2026, the Minnesota Department of Health issued a formal advisory after tracking more than 30 confirmed or suspected TMVII cases concentrated in the Twin Cities. Minnesota's first confirmed case appeared in July 2025, a Twin Cities resident who came in seeking care for a genital rash that refused to respond to standard treatment. By the time state officials issued their February alert, enough cases had accumulated that MDH was sending notices to hospitals, urgent care centers, emergency departments, dermatology clinics, and sexual health providers across the state asking them to watch for it.
Minnesota was not where TMVII started in the US. The first American case was identified in New York City in June 2024, in a man who had reported multiple male sexual partners while traveling in Europe. By October 2024, the CDC had formally documented those early New York cases in the Morbidity and Mortality Weekly Report. By January 2026, San Francisco had confirmed two cases in male patients with no recent international travel, meaning domestic transmission was already happening independently. According to a 2025 study published in Emerging Infectious Diseases, among 117 polled infectious disease clinicians, only a minority had experience diagnosing or treating TMVII, meaning for every cluster that gets identified, there are likely cases being logged as treatment-resistant jock itch and left uninvestigated.
The reason the Minnesota cluster grew as large as it did before anyone connected the dots is the same reason TMVII has spread quietly through other US cities: the infection is new enough that most clinicians don't think to look for it, and the rash it produces is familiar enough that patients and providers assume something more mundane is going on. A round, red rash near the genitals is an easy misdiagnosis. The average person tries a topical cream, waits, tries more cream, and by the time they return to a provider open to alternative explanations, weeks have passed and the infection has spread further.
What TMVII Actually Is, And Why It's Not Regular Ringworm
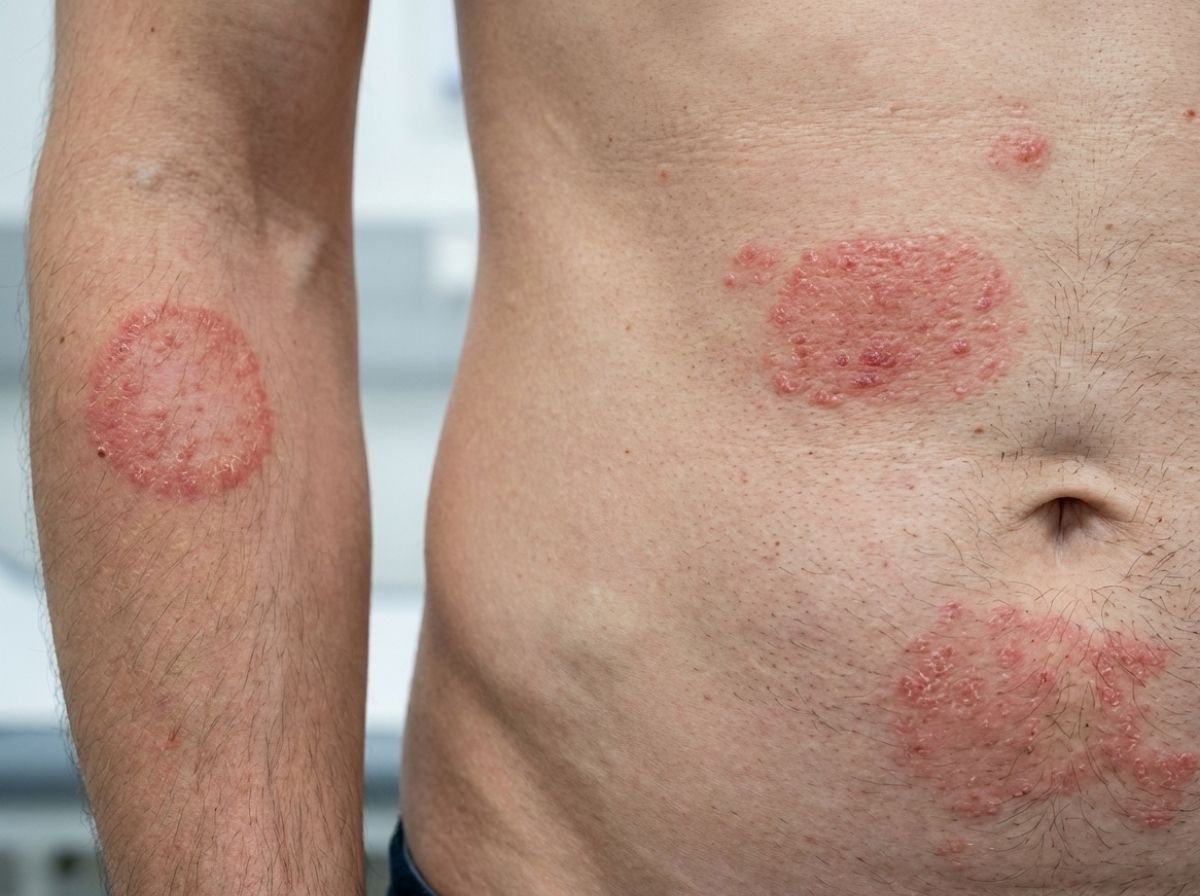
Ringworm, despite the name, has nothing to do with worms. It is a fungal skin infection caused by organisms called dermatophytes, and the "ring" refers to the circular shape the rash tends to take, with a slightly raised, darker edge around a lighter center. Jock itch, athlete's foot, and nail infections all belong to the same dermatophyte family. Standard ringworm, in almost all its forms, responds well to over-the-counter topical antifungal creams within two to four weeks. TMVII does not.
What sets TMVII apart comes down to a combination of factors that make it harder to clear and more likely to keep spreading. The infection is caused by a specific variant, genotype VII, of Trichophyton mentagrophytes, a species that has existed for a long time but whose genotype VII form appears to have only recently begun moving between humans through sexual contact. Genotype VII does not clear reliably with topical antifungals because the fungal spores penetrate more deeply into the skin. Without systemic oral treatment, the infection persists, spreads to new areas of the body, and can cause scarring and secondary bacterial infections if left alone long enough.
The transmission profile also makes it distinct. Standard ringworm picks up easily from gym mats, shared towels, and animal contact, you can get it without any skin-to-skin contact at all. TMVII does all of that, but its primary route is sexual contact. The close, sustained skin contact involved in sex creates exactly the right conditions for the fungus to transfer from an active rash to a new host. And because the rash can appear on the face, abdomen, and legs, not just the genitals, transmission risk is not limited to genital contact. Fungal spores also survive on shared objects, meaning household transmission through towels and bedding can continue even after partners stop having sex during a symptomatic period. According to the CDC's February 2026 clinician brief on emerging ringworm, TMVII is the only identified fungal organism that functions as a sexually transmitted infection.
| Condition | Appearance | Location | Responds to Topical Cream? | Key Difference |
|---|---|---|---|---|
| TMVII | Round, coin-shaped, raised edges, bumps or pimples on top | Genitals, buttocks, thighs, face, abdomen, legs | No, worsens with corticosteroids; oral treatment required | Spreads through sexual contact; history of new partner is a red flag |
| Jock itch | Red, ring-shaped, scaly, itchy edges | Inner thighs, groin, buttocks | Yes, clears with OTC antifungal in 2–4 weeks | Not sexually transmitted; responds normally to standard topicals |
| Eczema | Dry, cracked, inflamed patches; may weep or crust | Anywhere, arms, legs, neck are common | Improves with corticosteroids | Not infectious; no ring shape; a chronic condition |
| Psoriasis | Thick, silvery-scaled plaques on a red base | Elbows, knees, scalp, lower back | Improves with corticosteroids | Not infectious; scale is thicker and silvery; chronic condition |
What the Rash Looks Like, And Why It Keeps Getting Missed
You notice a round, red patch near your inner thigh a week or two after a sexual encounter. It is slightly raised at the edge, a little itchy, not dramatically painful yet. It looks like jock itch, or maybe a heat rash, or friction from clothing. You grab an antifungal cream at the pharmacy. A week later it is still there, maybe slightly larger. You use more cream. Nothing. By this point, weeks have gone by and the infection has likely spread to adjacent skin.
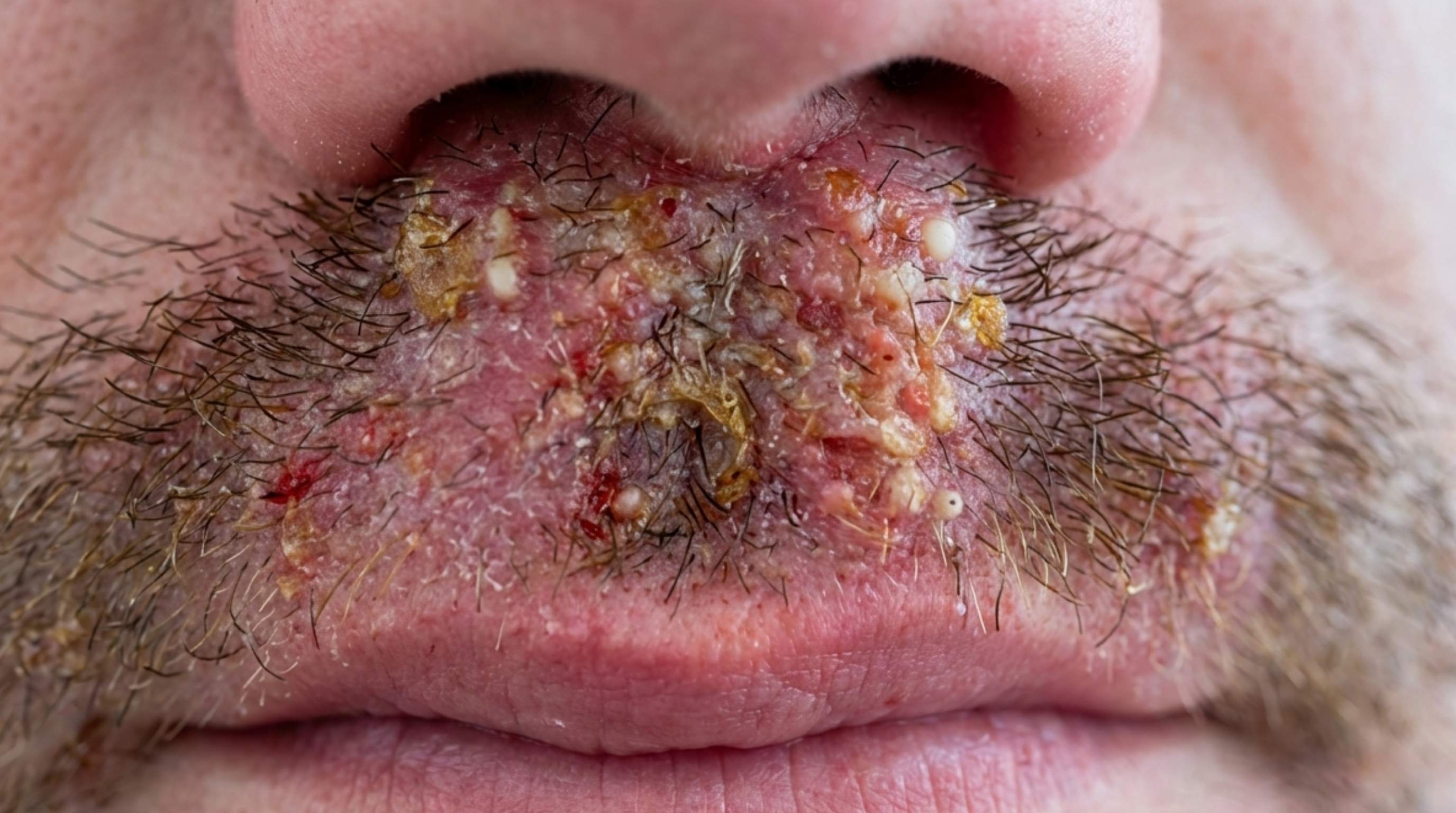
That sequence is why TMVII has traveled as far as it has. The rash it produces is clinically indistinguishable from several common conditions without laboratory testing. Features of a TMVII rash typically include round, coin-shaped lesions with red, irritated edges; raised bumps or pimple-like spots on the surface of the rash; and involvement anywhere on the body, genitals, buttocks, the area around the anus, inner thighs, abdomen, legs, arms, and face. In more advanced or untreated cases, the rash becomes painful, develops blisters, crusts over, and can leave permanent scarring. That a TMVII rash can appear on the face, including around the mouth, catches many people off guard. It is not where anyone expects an STI to show up, and it is often dismissed as a skin irritation with no connection to sexual history.
Two things drive most misdiagnoses. First, TMVII at onset looks almost identical to eczema and psoriasis, both of which are treated with corticosteroid creams. Applying a corticosteroid to a TMVII infection actively worsens it, because the steroid suppresses the local immune response that would otherwise help contain the fungus. The rash may appear to calm down briefly while the infection spreads under the skin. Second, standard topical antifungals that handle jock itch reliably do not work on TMVII. A patient who tries an over-the-counter treatment, sees no improvement, and decides the rash must be something non-fungal is now pointing themselves in exactly the wrong direction. According to infectious disease experts interviewed by Healio in March 2026, the most reliable early signal that a rash might be TMVII rather than a lookalike is simply the absence of treatment response, a rash that does not clear after two weeks of topical antifungal treatment, or that gets worse after corticosteroid application, warrants evaluation at a sexual health or dermatology clinic, full stop.
People are also reading: Do You Need STD Testing After Sex With a Condom? What Your Risk Actually Looks Like
How TMVII Spreads and Who Is Currently Most at Risk
The primary transmission route is direct skin-to-skin contact with an active rash during sexual activity. Because TMVII lesions can appear anywhere on the body, the risk extends well beyond genital-to-genital contact. Any skin that presses against an active rash during sex is a potential entry point for fungal spores, which is why rashes on the face, abdomen, and thighs all carry transmission risk during close physical contact.
Beyond direct sexual contact, TMVII spores survive on surfaces and fabric. Shared towels, bed linens, clothing, sex toys, and razors have all been identified as potential transmission routes in the epidemiological data from both the Minnesota outbreak and earlier European case series. The Minnesota Department of Health advises washing all clothing and linens on high heat to kill spores and disinfecting shared items with diluted bleach or benzalkonium chloride. This matters even during treatment; if shared items are not properly cleaned, reinfection can continue after sexual contact has stopped.
The current US outbreak has occurred predominantly among men who have sex with men, which reflects the population where TMVII first entered the country and where active surveillance has been most concentrated. The Minnesota Department of Health specifically identifies MSM, people who use anonymous dating apps, and people with a history of prior STIs as the groups currently at the highest risk. Infectious disease specialists at Duke Global Health Institute have been direct about this: anyone can contract TMVII regardless of gender, sexual orientation, or relationship structure. The risk is tied entirely to skin contact with an active rash. The current concentration in MSM networks reflects where the infection entered the US and how sexual networks are structured, not any biological susceptibility. As awareness grows and surveillance expands, cases in other populations will become more visible.
Testing for TMVII, And the Co-Infections That Often Come With It
TMVII itself is not something you can test for at home. Diagnosing it requires an in-person clinical assessment; a healthcare provider at a sexual health clinic or dermatology practice needs to scrape a skin sample from the active rash, examine it under a microscope for fungal elements, and attempt a fungal culture. DNA sequencing to confirm the TMVII genotype can take additional weeks to return, which is why both the Minnesota Department of Health and the CDC recommend that clinicians begin treatment based on the clinical picture and exposure history rather than waiting on full laboratory confirmation. If you have a rash that matches the profile and it has not responded to standard topical treatment, that is enough clinical justification to begin evaluation and empiric treatment.
What at-home rapid testing covers, critically, is everything that tends to travel alongside TMVII. The people most at risk right now are sexually active individuals with recent new partners, and that exact exposure history is the same situation that warrants a full STI screening. TMVII won't appear on a standard STI panel, but HIV, syphilis, gonorrhea, chlamydia, herpes, and hepatitis do, and co-infection rates among people diagnosed with one STI are consistently higher than in the general population. Catching a co-infection early changes outcomes meaningfully.
Timing your tests correctly matters. Test for HIV at 6 weeks after potential exposure for a first indicator result; a negative at 6 weeks carries real weight, but retest at 12 weeks for full certainty, a confirmed negative at 12 weeks means you did not contract HIV from that exposure. Test for syphilis from 6 weeks after exposure; the antibody response needs time, and testing earlier carries a genuine false-negative risk. Test for chlamydia from 14 days after exposure, and gonorrhea from 3 weeks after exposure. For herpes HSV-1 and HSV-2, test from 6 weeks after exposure. For hepatitis B, test from 6 weeks after exposure. For hepatitis C, test from 8 to 11 weeks after exposure, testing before 8 weeks carries real false-negative risk, and a negative after 11 weeks is considered conclusive.
| Infection | Test From | Negative Result Means | Positive Result Means |
|---|---|---|---|
| HIV | 6 weeks (first indicator); retest at 12 weeks for certainty | Negative at 12 weeks = did not contract HIV from that exposure | Virus is present; connect with a healthcare provider immediately |
| Syphilis | 6 weeks after exposure | No syphilis detected; retest at 12 weeks if ongoing concern | Infection present; curable with prompt treatment |
| Chlamydia | 14 days after exposure | No chlamydia detected; retest if new exposure occurs | Bacterial infection present; treatable |
| Gonorrhea | 3 weeks after exposure | No gonorrhea detected from that exposure | Infection present; requires prompt treatment |
| Herpes HSV-1 & HSV-2 | 6 weeks after exposure | No herpes antibodies detected from that exposure | Antibodies detected; indicates current or past infection |
| Hepatitis B | 6 weeks after exposure | No infection detected; reliable given shorter incubation period | Active infection; requires medical follow-up |
| Hepatitis C | 8–11 weeks after exposure | Conclusive after 11 weeks | Infection present; now curable in most cases |
Check Your STD Status in Minutes
Test at Home with Remedium8-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $149.00 $392.00
For all 8 tests
What To Do If You Think You Have TMVII
If a rash near your genitals, buttocks, inner thighs, or face appeared within days to a few weeks of a new sexual partner and has not cleared after two weeks of standard topical antifungal cream, go to a sexual health clinic or dermatology provider. Do not apply corticosteroid cream, hydrocortisone or any other steroid product, as this will worsen TMVII by suppressing the local immune response that is partially limiting the spread, and the rash may look temporarily calmer while the infection advances underneath.
While you have an active rash, avoid sexual contact and close skin-to-skin contact with others. Wash all clothing, towels, and bed linens on high heat. Do not share towels, razors, or sex toys. Notify recent sexual partners so they can be evaluated. TMVII can spread from an active rash even before it becomes painful enough to drive someone to seek care, and partners may be infected without knowing it yet. The Minnesota Department of Health advises that fungal spores can be killed with common disinfectants, including diluted bleach (a quarter cup per gallon of water) or benzalkonium chloride on hard surfaces.
Treatment requires oral antifungal medication prescribed by a healthcare provider. The specific agent and course length depend on the severity of the infection and how it responds, but treatment courses typically run from six weeks to three months. Completing the full course matters, stopping treatment when the rash appears to clear risks relapse because fungal spores can remain viable in the skin even after visible symptoms resolve. There is no at-home test for TMVII itself. Evaluation and confirmation require in-person clinical assessment, skin scraping, fungal culture, and in some cases, DNA sequencing at a laboratory. What you can do at home is test for the co-infections that consistently appear alongside TMVII in the same risk contexts, and do it at the right window so the results actually mean something.
Why TMVII Keeps Getting Missed, The Diagnostic Gap Explained
The diagnostic gap around TMVII is not a failure of individual clinicians; it is a structural problem with how new infections enter the healthcare system. TMVII was first formally identified as a human pathogen circulating through sexual networks in Europe in the early 2020s, with the first US case documented in 2024. That means most practicing clinicians in the US trained and built their diagnostic instincts in a world where sexually transmitted fungal infections did not exist as a category. When a patient presents with a genital rash, a clinician's first mental list of possibilities, herpes, syphilis, molluscum, contact dermatitis, jock itch, does not include a fungal infection acquired through sex, because until very recently, that wasn't a real thing.
Standard fungal cultures used in most clinical laboratories can detect that a Trichophyton species is present, but cannot identify TMVII specifically. Confirming the genotype requires advanced molecular testing, DNA sequencing, which is only available at select reference laboratories and can take weeks to return results. This creates a situation where even a clinician who suspects TMVII cannot get fast confirmation and must make treatment decisions based on clinical presentation and exposure history while waiting on laboratory results. The CDC's February 2026 advisory addressed this directly, recommending that providers begin empiric treatment for TMVII based on symptoms and sexual history without waiting for genotype confirmation when the clinical picture is consistent.
The surveillance gap compounds the diagnostic one. TMVII is not a nationally reportable infection in most US states, meaning there is no mandatory case-counting system tracking how broadly it has spread. The Minnesota cluster was identified because alert clinicians recognized an unusual pattern and proactively contacted the state health department, not because an automated surveillance system flagged it. In cities where that kind of clinical alertness is absent, TMVII cases are almost certainly being recorded as treatment-resistant jock itch or unspecified dermatitis and never investigated further. As NYU dermatologist Dr. Avrom Caplan, one of the clinicians who published the early US case series, noted in a March 2026 interview with Healio: more outbreaks are expected as awareness increases, given how the infection spreads through sexual networks.
Why This Matters Right Now, And What It Means for Sexual Health More Broadly
TMVII's emergence in the US is not an isolated event, it is part of a broader pattern that public health officials have been tracking for years. Infectious diseases circulate globally through interconnected sexual networks, and dating apps have made it structurally easier for skin-contact pathogens to travel further and faster than historical STI patterns would have predicted. TMVII circulated in Europe for years before reaching the US, and the same pattern, European circulation among MSM, spread through international sexual contact, eventual domestic transmission, has been documented for other infections.
The lesson here is not panic. TMVII is treatable. It has not been associated with serious systemic illness in immunocompetent people, and the oral antifungal medications used to treat it appear effective based on the case data collected so far. The lesson is that a rash that does not respond to standard treatment is not something to keep self-managing with pharmacy products. Two weeks of topical antifungal cream with no improvement is the signal to seek clinical evaluation, not to try a different cream. And any new sexual contact is a reasonable prompt to run a comprehensive at-home STI screen, not because TMVII will show up on it, but because catching HIV, syphilis, gonorrhea, chlamydia, herpes, or hepatitis early makes all the difference for outcomes, partner notification, and peace of mind.
The same care and attention that makes someone a responsible sexual health participant, getting tested, knowing their status, communicating with partners, is exactly the behavior that limits TMVII's ability to spread undetected. The infections that have at-home rapid tests are a good place to start.

People are also reading: How Ozempic Can Aid People with HIV and Hepatitis
FAQs
1. What is TMVII?
TMVII stands for Trichophyton mentagrophytes genotype VII, the only known sexually transmitted fungal infection in the world. It causes painful, coin-shaped ringworm rashes that can appear on the genitals, buttocks, face, inner thighs, and trunk, and it requires oral antifungal treatment to clear. It does not respond to the topical antifungal creams you can buy without a prescription.
2. Why is TMVII in the news right now?
In February 2026, the Minnesota Department of Health declared the largest known US outbreak of TMVII, with more than 30 confirmed or suspected cases in the Twin Cities metro area. It was the latest cluster in a series that started with New York City cases in 2024, and it prompted the CDC and state health departments across the country to issue clinical advisories asking providers to watch for it.
3. How does TMVII spread?
Primarily through direct skin-to-skin contact with an active rash during sexual activity. Because the rash can appear anywhere on the body, including the face, abdomen, and legs, transmission is not limited to genital contact. The fungal spores also survive on shared towels, bed linens, clothing, razors, and sex toys, which means household transmission is possible without ongoing sexual contact if those items aren't properly cleaned.
4. Can jock itch cream fix TMVII?
No. Standard over-the-counter antifungal creams that handle jock itch reliably do not work on TMVII. The infection requires oral antifungal medication prescribed by a healthcare provider, typically for anywhere from six weeks to three months. If a rash in or near the genital area hasn't improved after two weeks of topical treatment, that's your signal to see a clinician, not to try a different cream.
5. Can the wrong treatment make TMVII worse?
Yes, and this is one of the most important points about TMVII. Corticosteroid creams, like hydrocortisone, commonly used for eczema and skin inflammation, suppress the local immune response that helps contain the fungus. Applying a corticosteroid to a TMVII rash can make it look temporarily calmer while allowing the infection to spread more aggressively underneath. Do not use steroid creams on a genital or perianal rash until TMVII has been ruled out.
6. Who is most at risk of TMVII right now?
The Minnesota Department of Health currently lists men who have sex with men, people who use anonymous dating apps, and people with a history of previous STIs as the highest-risk groups in the current outbreak. Infectious disease experts from Duke Global Health Institute have been clear that anyone can contract TMVII through skin contact with an active rash, the current concentration in MSM networks reflects where the infection entered the US and how those networks are structured, not any biological predisposition.
7. Is there an at-home test for TMVII?
No, TMVII requires in-person clinical evaluation: a skin scraping, microscopy, fungal culture, and in many cases DNA sequencing at a reference lab to confirm the genotype. There is no rapid at-home test for TMVII. However, at-home rapid tests do exist for the STIs that commonly co-occur in the same exposure contexts as TMVII, including HIV, syphilis, chlamydia, gonorrhea, herpes, hepatitis B, and hepatitis C, and getting those tests at the right timing window is genuinely useful.
8. Can TMVII spread through bedding or towels?
Yes. Fungal spores from an active TMVII infection survive on fabric and surfaces. Shared towels, bed linens, clothing, and sex toys are all documented transmission routes. During an active infection, keep personal items that contact the affected skin separate from household items, wash fabric on high heat, and disinfect hard surfaces and shared objects with diluted bleach or benzalkonium chloride.
9. What happens if TMVII goes untreated?
Untreated TMVII spreads to new areas of the body and becomes progressively harder to address. Persistent rashes can leave permanent scars. Open or blistered lesions create entry points for bacteria, which can lead to secondary bacterial infections requiring additional treatment. Early treatment with oral antifungals leads to significantly better outcomes than treatment that starts after the infection has had weeks or months to expand.
10. What STI tests should I get if I was in the same risk situation as TMVII exposure?
Test for HIV at 6 weeks for a first indicator result and again at 12 weeks for certainty. Test for syphilis and herpes (HSV-1 and HSV-2) from 6 weeks after exposure. Test for chlamydia from 14 days after exposure and gonorrhea from 3 weeks after exposure. For hepatitis B, test from 6 weeks after exposure. For hepatitis C, test from 8 to 11 weeks, testing before 8 weeks carries real false-negative risk, and a negative after 11 weeks is conclusive. You cannot test for TMVII at home; clinical evaluation is required for that.
Get Clear Answers About What You Might Have Been Exposed To
TMVII can't be caught with an at-home test, that part requires a clinician. But everything that tends to travel alongside it can be tested at home, accurately, in about 20 minutes. If you've had a new sexual partner recently and you're in any of the risk groups the Minnesota Department of Health has flagged, comprehensive STI testing isn't an overreaction. It's just good information to have.
The 7-in-1 Complete At-Home Rapid Test Kit covers HIV, syphilis, HSV-2, chlamydia, gonorrhea, hepatitis B, and hepatitis C in a single session, test at 6 weeks post-exposure, and every infection with a 6-week window is covered accurately at once. For the most comprehensive panel available, the Women's 10-in-1 Complete At-Home Rapid Test Kit adds HPV 16&18 and trichomoniasis. If you'd rather start with a single targeted test, the HIV 1&2 At-Home Rapid Test Kit delivers a 99.7% accurate result in 20 minutes. Your results, your privacy, your power.
Browse the full range of rapid at-home test kits at STD Rapid Test Kits. Take control of your sexual health today.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
3. CDC Clinician Brief: Emerging Ringworm, February 2026
5. Duke Global Health Institute: A New STI Is Spreading in the US, What You Should Know, March 2026
6. CDC: Emerging Types of Ringworm, February 2026
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.