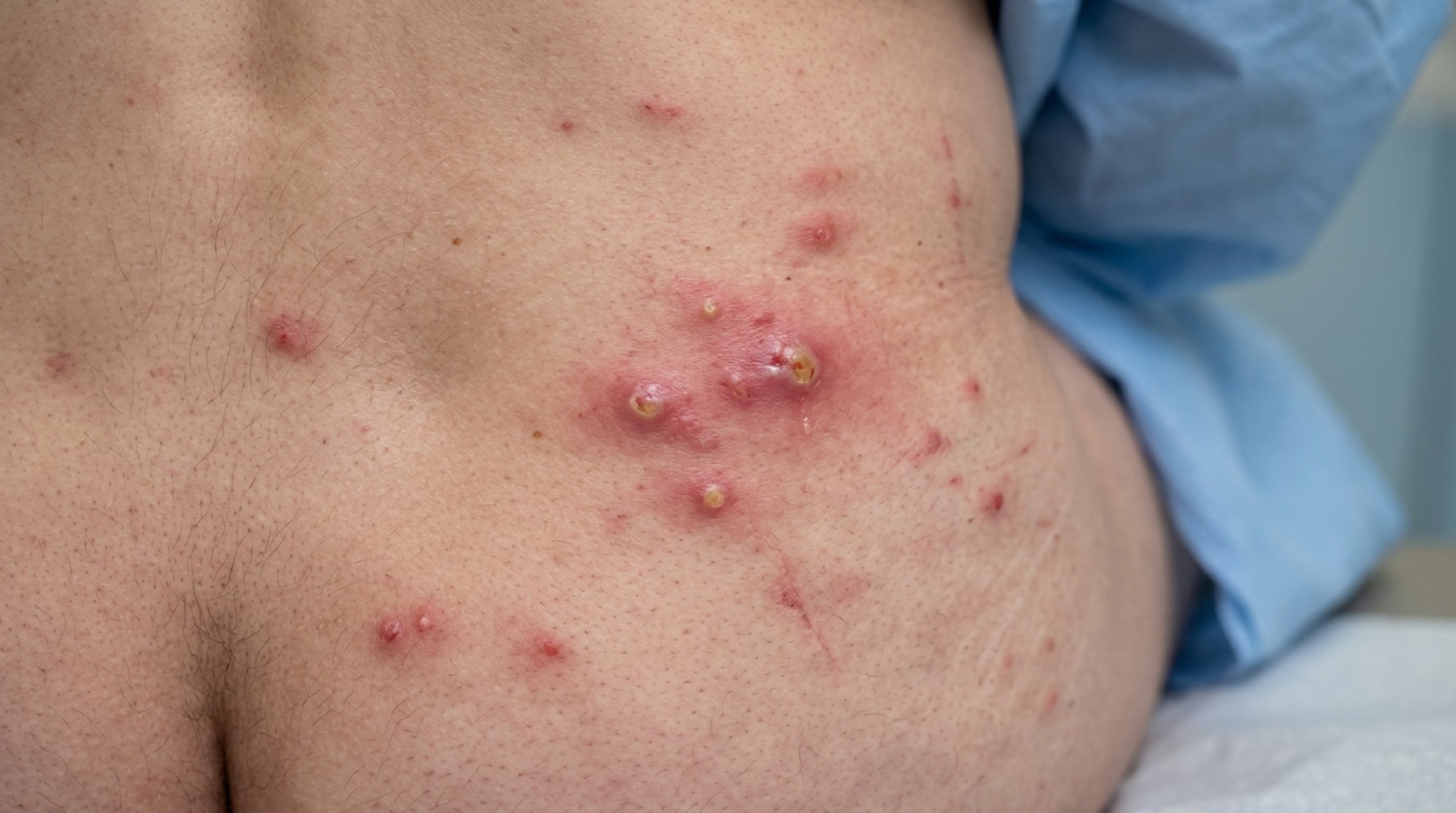
Herpes Symptoms in Women: What Shows Up First (And What Often Doesn’t)
Last updated: March 2026
A bump on your buttocks is one of those discoveries that tends to send people straight to Google at midnight, and straight into a spiral. The internet is not particularly helpful here. It will either tell you it's definitely herpes or offer you seventeen unrelated diagnoses that somehow include shingles and chickenpox. The truth is more useful: most bumps on the buttocks are not STDs. But some are, and knowing the difference matters, not just for peace of mind, but because two of the most common culprits respond very differently to waiting versus testing and treating.
People are also reading: How Safe Is “Safe Sex”? The Truth About Condoms and STD Risk
What STDs Can Actually Cause Bumps on the Buttocks?
Not every STD causes visible skin changes, and of those that do, not all of them commonly affect the buttocks. But there are a few that genuinely can, and understanding how each one behaves will help you narrow down what you're actually dealing with.
Genital herpes caused by HSV-2 is the most likely STD explanation for bumps in the buttock area. The virus travels along nerve pathways, and the sacral nerve roots, which run through the lower back and buttocks, are a common site for outbreaks. This means blisters or sores don't have to appear directly on or near the genitals. They can show up on the lower buttocks, upper thigh, or even the tailbone area. According to the CDC, genital HSV-2 affects roughly one in six Americans aged 14 to 49, making it one of the most prevalent STIs in the country, and a significant proportion of those people don't know they have it.
Syphilis is the second serious contender. In primary syphilis, the initial sore, called a chancre, forms at whatever site the bacteria entered the body. For people who've had anal sex, this can mean a sore near or around the anus, and sometimes on the adjacent skin of the buttocks. These sores are typically painless and firm, which is part of why they're so often missed. In secondary syphilis, a rash can spread widely across the body, including the buttocks. The CDC has tracked a dramatic rise in syphilis cases in recent years, with over 200,000 reported cases annually in the US, a pattern that makes it increasingly relevant when evaluating any new skin change after sexual contact.
HPV (human papillomavirus) can cause genital warts that appear around the anus and on the perianal skin, which includes the surrounding buttock area. These warts are caused by low-risk HPV types (primarily 6 and 11) and have a distinctive appearance, usually flesh-colored, soft, and sometimes cauliflower-like in texture. They're generally painless. Unlike herpes or syphilis, genital warts from HPV don't come and go in outbreaks; they tend to stay put or multiply slowly over time unless treated.
Molluscum contagiosum, while technically not classified as a traditional STI in all contexts, can spread through skin-to-skin sexual contact and occasionally appears on or near the buttocks. The bumps are small, round, and have a characteristic dimpled or umbilicated center, almost like a tiny donut, which helps distinguish them from other conditions.
What Each STD Bump Looks Like: A Visual Identification Guide
One of the most frustrating things about online symptom checking is that most descriptions are vague, "blisters," "sores," "bumps", without telling you what actually distinguishes one from another. This section breaks it down as concretely as possible.
| Type of Bump | Most Likely Cause | Key Visual Features | Other Symptoms to Look For |
|---|---|---|---|
| Small fluid-filled blisters that burst and leave raw, shallow sores | Herpes (HSV-2) | Grouped blisters on a red base; sores may crust over; typically appear in clusters, not singly | Tingling or burning before blisters appear; muscle ache in thighs; itching; possible flu-like symptoms at first outbreak |
| Single firm, painless ulcer with raised edges | Syphilis (primary chancre) | Usually solitary; smooth clean base; raised indurated border; 1–2 cm; does not itch or hurt | Swollen lymph nodes in groin; often goes completely unnoticed |
| Widespread rough red or brown spots, flat or slightly raised | Syphilis (secondary rash) | Symmetric; can appear on buttocks, palms, soles; non-itchy; blotchy or papular texture | Fatigue, sore throat, headache, hair loss; flu-like symptoms |
| Soft, flesh-colored growths, flat or cauliflower-like clusters | HPV genital warts | Soft to touch; can be single or multiple; flesh/grey/whitish color; may have stalk-like base | Usually painless; occasionally itchy; may bleed if irritated |
| Small round bumps with dimpled center (like a tiny donut) | Molluscum contagiosum | Dome-shaped; flesh-colored or pearlescent; central pit or depression; typically 2–5mm | Mild itching; can appear in clusters; may spread by scratching |
| Red, inflamed bumps centered on hair follicles | Folliculitis (not an STD) | Each bump has a hair in the center; may have white or yellow pus tip; scattered across buttock skin | Mild tenderness; may be triggered by friction, shaving, sweat |
| Curved, ingrown bump with visible trapped hair | Ingrown hair (not an STD) | Reddish bump with curved hair visible under skin; often appears after shaving or waxing | Localized tenderness; may develop a small pus pocket; no systemic symptoms |
The most important distinction to understand is this: herpes sores are painful and come in clusters on a red, inflamed base. Syphilis chancres are typically single, painless, and firm, and are frequently missed for exactly that reason. HPV warts are soft, non-painful, and tend to grow over time rather than appear and disappear. Keeping these differences in mind cuts through a lot of the confusion that Google image searches create.
When Do These Bumps Appear After Exposure?
Timing is one of the most useful clues when trying to figure out what you're dealing with. If you've had unprotected sex recently and a bump has appeared, the timeline between exposure and symptoms can tell you a lot.
With herpes, the first outbreak typically appears within 2 to 12 days of exposure, though some people don't notice symptoms until weeks or months later, or ever. The first outbreak tends to be the most severe. After that, the virus settles into the sacral nerve roots and can reactivate periodically, meaning subsequent outbreaks can appear on the buttocks with little warning. A tingling, itching, or aching feeling in the thighs, lower back, or buttocks often precedes an outbreak by a day or two, which is the nervous system's way of announcing what's coming.
With syphilis, the initial chancre typically appears 10 to 90 days after exposure, with most people noticing it around three weeks after contact. It heals on its own within three to six weeks, but the bacteria remain in the body. If untreated, secondary syphilis follows anywhere from a few weeks to three months after the chancre disappears, bringing a widespread rash that can cover the buttocks, palms, and soles. The fact that the chancre is painless and self-resolving is exactly why syphilis is called "the great imitator", it can seem like it went away when it absolutely has not.
With HPV-related warts, the timing is notoriously unpredictable. Warts can appear anywhere from a few weeks to several months, sometimes even years, after initial exposure. The virus can remain dormant in the skin long after the sexual contact that transmitted it, which is why tracing exactly when or from whom you contracted it is often impossible.
| STD | Typical Onset of Skin Symptoms | Pattern Over Time |
|---|---|---|
| Herpes HSV-2 | 2–12 days for first outbreak (can be longer) | Recurring outbreaks; later episodes often milder; tingling prodrome common |
| Syphilis (primary chancre) | 10–90 days; median ~21 days | Single ulcer heals on its own in 3–6 weeks; secondary rash follows weeks to months later if untreated |
| HPV genital warts | Weeks to several months; sometimes years | Persistent; warts may grow or multiply without treatment; do not come and go like herpes |
| Molluscum contagiosum | 2–7 weeks after exposure | Gradually increases in number; individual bumps may self-resolve over months |
Not Every Bump Is an STD, Knowing the Difference
Here's a fact that most people who've landed on this article probably need to hear: statistically, the bump on your buttocks is more likely to be folliculitis, a razor bump, an ingrown hair, or simple acne than any STD. The buttocks are a high-friction area covered much of the day, prone to sweat, and frequently subjected to shaving or waxing, all of which are ideal conditions for non-STD skin irritation.
Folliculitis is inflammation of the hair follicle, and it's extremely common on the buttocks. Each bump appears around a follicle and may develop a small white or yellow pus tip. Unlike herpes, folliculitis bumps are scattered rather than clustered in one area, and each bump sits centered on a hair. They're triggered by friction from tight clothing, sweating, or irritation from new soaps or lotions. They typically resolve on their own without any treatment, and they have nothing to do with sexual contact.
Razor burn and ingrown hairs produce a very similar picture: red, bumpy irritation that appears after shaving or waxing. The telltale sign is a curved hair visible just under the skin surface. These bumps tend to appear in lines or patterns that follow shaving direction, not randomly scattered the way folliculitis presents, and certainly not in the tight cluster formation characteristic of herpes. They're uncomfortable, occasionally pustular, and entirely benign.
Acne on the buttocks is also more common than most people realize. Unlike facial acne, buttock acne tends to appear as deeper, firm bumps that can be somewhat painful when pressed. They lack the fluid-filled, clustered appearance of herpes blisters, and they're not associated with any burning or tingling prodrome. Body acne flares with heat, friction, and sweat, the same conditions that make the buttocks particularly prone.
The practical test is this: if the bump appeared shortly after shaving, you've recently worn tight synthetic fabric, or you've been sweating heavily, think non-STD first. If the bump appeared with no obvious mechanical trigger, within weeks of sexual contact, and especially if there's any burning, tingling, or grouped blister formation, think testing.
Check Your STD Status in Minutes
Test at Home with RemediumGenital Herpes Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $45.99 $49.00
If You Have Bumps and You're Unsure: Which Test to Take
Testing is the only way to know for certain. Visual identification can get you a good working hypothesis, but it can't give you a definitive answer, and the consequences of misidentifying syphilis as a random sore or mistaking herpes for folliculitis are significant enough that guessing isn't worth it.
If the bumps look like fluid-filled blisters, especially if they're clustered, burning, or came with a tingling prodrome, the priority test is the Genital Herpes HSV-2 At-Home Rapid Test Kit. This test detects HSV-2 antibodies from a finger-prick blood sample and delivers results in minutes. The important timing note: test no sooner than 6 weeks after the exposure you're concerned about. Testing too early can produce a false negative because the immune system hasn't had enough time to generate the antibodies the test detects. If you test negative before 6 weeks, retest at the 6-week mark for a reliable result.
If the bump looks like a single painless ulcer, firm, clean-edged, not clustered, and especially if it appeared around 3 weeks after sexual contact, syphilis should be on your radar. The Syphilis At-Home Rapid Test Kit (99.4% accuracy) is the right place to start. For syphilis, test at least 6 weeks after exposure for a reliable result. The chancre's tendency to be painless and self-resolve is why so many people miss the primary stage entirely, testing is especially important here because syphilis is straightforwardly curable when caught early.
If you're genuinely unsure which infection you're dealing with, or if you've recently had unprotected sex and want a fuller picture, a combination kit covers more ground. The Chlamydia, Gonorrhea & Syphilis 3-in-1 kit and the broader 6-in-1 combination kit are good options if you want to rule out multiple infections at once rather than testing sequentially.
A note on window periods, because this matters: testing too soon after exposure is one of the most common reasons for false negatives. The body needs time to produce the antibodies that at-home rapid tests detect. If your exposure was recent, meaning less than 6 weeks ago, a negative result today does not rule out infection. Mark the 6-week point on your calendar and test then for a result you can rely on.
Genital Herpes: The Basics
Genital herpes is caused by the herpes simplex virus, which exists as two types: HSV-1 and HSV-2. HSV-2 is the primary driver of genital herpes, and it's far more common than most people realize. According to the CDC, approximately one in six Americans between the ages of 14 and 49 has genital HSV-2 infection. Critically, a large majority of those people are unaware they have it, estimates suggest up to 87% of people with HSV-2 have never received a formal diagnosis. That means transmission often happens with no visible symptoms and no awareness on the transmitting partner's part.
The virus establishes itself permanently in the sacral ganglia, nerve clusters at the base of the spine, which is why outbreaks occur in the genital, anal, and buttock areas. This is also why herpes sores on the buttocks don't indicate anything different about how the infection was transmitted; it's simply the virus following its nerve pathway. A new outbreak can be triggered by stress, illness, immune suppression, menstruation, or even localized friction or sun exposure. Not everyone has recurrent outbreaks, some people have one episode and then very few or none afterward, while others experience them several times a year.
One of the most practically important facts about herpes is that transmission can occur even when no sores are visible, through a process called asymptomatic viral shedding. This means someone who has never had a recognizable outbreak can still pass the virus to a partner. It's one of the reasons herpes prevalence stays high despite people actively trying to avoid transmission, the virus doesn't always announce itself before it spreads.
Syphilis and the Buttocks: Why It Gets Missed
Syphilis deserves its own section in this discussion because it's genuinely underestimated as a cause of buttock skin changes, and because missing it has more serious long-term consequences than missing most other STDs at this stage. The CDC has documented a sustained and significant rise in syphilis rates over the past decade, making it more clinically relevant today than it was twenty years ago.
The primary chancre of syphilis forms wherever the Treponema pallidum bacterium enters the body. For someone who has had anal sex with an infected partner, that entry point can be around the anus or on the perianal skin, and the surrounding buttock region can also be affected. The chancre is typically a single, firm, round ulcer with clean edges and no discharge. What makes it particularly deceptive is that it's painless. Most people notice a sore because it hurts. A painless sore in an area that's already difficult to see is easy to dismiss as a minor skin irritation, sit on, and forget about, especially since it resolves on its own within a few weeks.
The resolution of the chancre does not mean the infection has resolved. Without treatment, syphilis progresses to the secondary stage, during which bacteria have spread through the bloodstream. The secondary rash that follows, which can appear on the buttocks, trunk, palms, and soles, is accompanied by systemic symptoms including fatigue, swollen lymph nodes, and low-grade fever. After the secondary stage, syphilis enters a latent phase with no visible symptoms, potentially for years, before potentially progressing to tertiary syphilis with serious organ involvement. Treatment at any early stage is straightforward and effective. The problem is that the window to catch it easily keeps sliding shut.
People are also reading: Polyamory and STDs: Does Having Multiple Partners Increase Your Risk?
How Herpes Outbreaks Behave Over Time
Understanding the pattern of herpes outbreaks helps make sense of why bumps on the buttocks might appear, disappear, and reappear, and why the absence of active sores doesn't mean the infection isn't there. After the initial infection, HSV-2 travels to the sacral nerve ganglia and establishes a lifelong latency. It can remain dormant indefinitely, or it can reactivate in response to various triggers.
The first outbreak is usually the most severe. Blisters appear, typically in a cluster, on a red inflamed base. They're often painful or burning, and may be accompanied by flu-like symptoms, swollen glands in the groin, fatigue, muscle aches in the thighs and lower back. After the blisters rupture, they leave shallow, raw sores that eventually crust and heal over one to four weeks. Recurrent outbreaks tend to be shorter and milder than the first, though this varies considerably from person to person.
A key feature that distinguishes herpes from many other skin conditions is the prodrome, the warning signs that often precede an outbreak by one to two days. These typically manifest as tingling, itching, or a burning sensation in the affected nerve area before any sores are visible. On the buttocks, this might feel like an unexplained ache in the tailbone or upper thigh. If you know what to look for, the prodrome is often more useful than the sore itself as a diagnostic clue, because the sore can be ambiguous, but a consistent pattern of tingling followed by a small cluster of sores in the same location is a fairly specific signal.
Common factors that can trigger a herpes recurrence include emotional or physical stress, fever or systemic illness, immunosuppression, hormonal changes (including menstruation), and sometimes mechanical friction in the area. Managing these triggers can reduce outbreak frequency for some people, though it varies substantially.
Transmission: How These Infections Actually Spread
A common misconception about STDs that cause skin symptoms is that transmission only happens when visible sores are present. For herpes and syphilis specifically, this is wrong, and understanding why helps explain how people contract these infections from partners who had no idea they were infectious.
HSV-2 spreads through direct skin-to-skin contact, and transmission can occur during asymptomatic viral shedding, periods when the virus is active at the skin surface without producing visible blisters or sores. Research cited by the American Sexual Health Association indicates that people with genital herpes can shed virus asymptomatically anywhere from 5% to 20% of the time, meaning transmission risk exists even between visible outbreaks. Penetrative sex is not required for transmission, skin-to-skin contact in the genital or buttock area is sufficient.
Syphilis spreads through direct contact with a syphilis sore or rash during sexual activity. During primary syphilis, the chancre is highly infectious, it contains large numbers of Treponema pallidum bacteria in its serous fluid. The risk of acquiring syphilis from a single sexual encounter with an infectious partner is estimated at approximately 30–50%. During secondary syphilis, the rash (including any that appears on the buttocks) is also infectious. After the rash resolves, transmission through sexual contact becomes less likely, though a person can still carry and transmit the infection.
HPV spreads through skin-to-skin contact in the anogenital area. Condoms reduce but do not eliminate transmission risk because they don't cover all potentially infectious skin. A partner can transmit HPV with no visible warts, the virus can be present in skin without producing visible growths. Once warts do appear, they indicate active HPV presence and are directly infectious through contact.
What Undiagnosed or Untreated Infections Can Lead To
Most people who find a bump and decide to wait and see are acting on the reasonable instinct that most things resolve on their own. For folliculitis or a razor bump, that instinct is correct. For HSV-2 or syphilis, the calculus is different, not because these infections are necessarily dangerous in the near term, but because they have long-term implications that waiting doesn't address.
Undiagnosed HSV-2 means continued transmission to partners who may not know they're being exposed. It also means missing the opportunity to understand your own outbreak patterns, recognize prodromal symptoms, and take steps to reduce transmission. There are also secondary health considerations, HSV-2 infection has been shown to increase susceptibility to other sexually transmitted infections, including HIV, because the skin disruption caused by sores creates an easier entry point for other pathogens. For pregnant people, undiagnosed HSV-2 carries the additional risk of neonatal herpes, a serious condition that requires specific precautions during delivery.
Untreated syphilis progresses through stages that become increasingly difficult to manage. The latent stage may last for years with no symptoms, during which the infection continues to cause systemic damage. Tertiary syphilis, which affects the heart, brain, and other organs, is rare today because most cases are caught earlier, but it remains a risk in people who go undiagnosed for extended periods. Congenital syphilis, transmitted from mother to fetus during pregnancy, has seen a troubling resurgence in the US in recent years. The straightforward part is that early syphilis responds very well to treatment, catching it early is almost always much simpler than catching it late.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
FAQs
1. Can herpes really appear on the buttocks and not on the genitals?
Yes, and it's more common than most people expect. HSV-2 lives in the sacral nerve ganglia at the base of the spine, which means outbreaks can occur anywhere those nerve pathways run, including the lower buttocks, upper thighs, and tailbone area. The location of an outbreak doesn't indicate anything different about how the infection was acquired.
2. How do I tell the difference between a herpes sore and a pimple on my buttocks?
Herpes sores tend to appear in small clusters on a red, inflamed base, often with burning or tingling beforehand. They're usually fluid-filled at first, then rupture and crust over. A pimple or folliculitis bump is typically a single bump centered on a hair follicle, may have a white tip, and doesn't follow any prodromal symptoms. If you're genuinely unsure, testing is the most reliable approach, visual diagnosis, even by a clinician, isn't definitive for herpes.
3. Is a painless sore on my buttocks always syphilis?
Not always, but a painless, firm, clean-edged ulcer that appeared around three weeks after sexual contact is a textbook description of a syphilis chancre and should be tested for. Other painless lesions exist, molluscum contagiosum bumps, for example, are painless, but the combination of timing, firmness, and single-lesion presentation warrants taking syphilis seriously. Test at least 6 weeks after the relevant exposure for an accurate result.
4. I had bumps that went away on their own. Does that mean it wasn't an STD?
Not necessarily. Syphilis chancres resolve on their own within a few weeks, but the infection continues progressing internally. Herpes sores also heal between outbreaks. A bump disappearing is not reassurance that it wasn't infectious; it's sometimes the opposite. If you had an unexplained skin change after sexual contact, testing is still worthwhile even after the symptom resolves.
5. How long after unprotected sex should I wait before testing for herpes?
For an accurate result, wait at least 6 weeks after the exposure you're concerned about. At-home rapid tests detect HSV-2 antibodies, and the body needs time to produce a detectable antibody response after initial infection. Testing too early can produce a false negative even if infection has occurred.
6. Can I get syphilis on my buttocks without having anal sex?
Syphilis spreads through direct contact with a syphilis sore during any sexual activity, vaginal, anal, or oral. If the sore is on a partner's genitals and your buttocks are in contact with that area during sex, transmission is theoretically possible. The chancre forms wherever the bacteria entered your body, and perianal skin is in contact with partners during a range of sexual activities.
7. I have bumps on my buttocks but I've never had genital sores. Could I still have herpes?
Yes. Some people's herpes outbreaks occur exclusively on the buttocks or thighs without ever producing sores on the genitals themselves. Additionally, many people with HSV-2 never experience recognized outbreaks at all. The absence of classic genital sores does not rule out HSV-2 infection. A blood antibody test is the only way to know for certain.
8. What does a syphilis rash on the buttocks look like compared to herpes?
Secondary syphilis produces a widespread, non-itchy, reddish-brown rash that can appear on the buttocks along with the palms, soles, and torso. It's typically flat or slightly raised and doesn't blister. Herpes produces clustered, fluid-filled blisters that break open and crust over, usually localized to one area rather than spreading across the body. The fact that a syphilis rash doesn't itch is often the detail that clinicians find most useful, itching tends to point away from syphilis.
9. Are genital warts and herpes the same thing?
No. They're caused by entirely different viruses, herpes by HSV-2 (or HSV-1), and genital warts by specific strains of human papillomavirus (HPV). Herpes produces fluid-filled blisters that heal and recur. Warts from HPV are soft, flesh-colored growths that don't come and go in outbreak cycles, they tend to persist or multiply without treatment. Different viruses, different appearance, different behavior, different tests, different management.
10. Can I have both herpes and syphilis at the same time?
Yes, and co-infection is not particularly rare. Having active HSV-2 sores actually increases susceptibility to syphilis and vice versa, because open skin disruptions make it easier for other pathogens to enter. If you're uncertain about a buttock bump after sexual exposure, testing for both infections rather than assuming it can only be one makes practical sense, especially given how different their treatment protocols are.
Get Clarity on What You're Dealing With
Sitting with uncertainty about a bump on your buttocks, wondering whether it's herpes, syphilis, or something completely unrelated, is one of the more avoidable sources of anxiety in sexual health. These two infections are the most clinically significant explanations for buttock bumps after sexual contact, and both are straightforwardly testable at home without a clinic visit, a conversation with a receptionist, or a wait for an appointment.
For bumps that look like blisters, clustered, burning, potentially accompanied by tingling, the Genital Herpes HSV-2 At-Home Rapid Test Kit (98.2% accuracy) gives results from a simple finger-prick sample in minutes. For a single painless ulcer or unexplained skin changes after sexual contact, especially if it resolved on its own, the Syphilis At-Home Rapid Test Kit (99.4% accuracy) is the direct answer. Both ship discreetly and test at home with no lab required.
If you'd rather test for multiple infections at once and settle the question more broadly, the 6-in-1 Complete STD Test Kit covers HSV-2, Chlamydia, Syphilis, HIV, Hepatitis B, and Hepatitis C in a single order. Testing isn't a big deal, it's what informed, health-conscious people do. Visit STD Rapid Test Kits to explore the full range of at-home options.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. Centers for Disease Control and Prevention, Genital Herpes Fact Sheet
2. StatPearls / NCBI, Syphilis (Treponema Pallidum): Stages, Clinical Presentation, Diagnosis
3. American Sexual Health Association, Fast Facts About HSV
4. CDC STD Treatment Guidelines, Anogenital Warts (HPV)
5. Cleveland Clinic, Syphilis: Stages, Symptoms, Causes, and Treatment
6. PMC / NCBI, Secondary Syphilitic Lesions: Clinical Features and Differentiation
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: March 2026
This article is for informational purposes and does not replace medical advice.