Silent STDs in Men: Infections That Cause Damage Without Symptoms
Last updated: March 2026
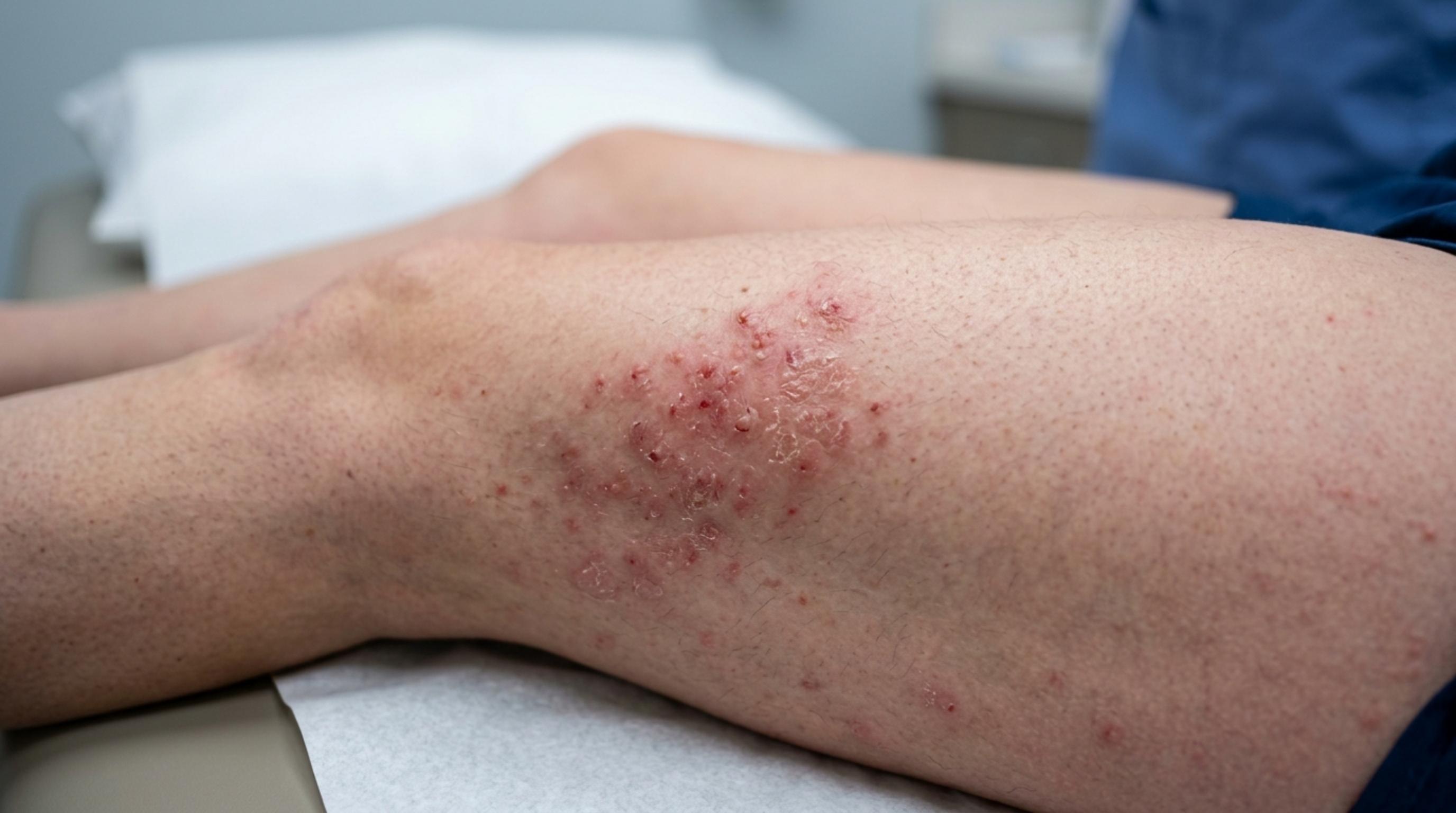
You're standing in decent lighting, squinting at something on your skin, trying to figure out if it's a pimple, a shaving irritation, or something that needs a doctor. This is one of the most common experiences people have after a new sexual encounter, and one of the least talked about. The internet does not help. Typing symptoms into a search engine at midnight almost always lands you somewhere between razor burn and a dramatic worst-case scenario, with very little useful information in between.
Here's the thing about STD-related skin changes: they don't always look dramatic. Some of the most serious infections, syphilis in particular, can produce rashes or sores that are so subtle or painless that people miss them entirely. Others, like herpes, can look almost identical to ingrown hairs, eczema, or folliculitis. The rash itself is rarely enough to make a diagnosis. What matters is the full picture: what it looks like, where it appeared, when it appeared relative to any sexual exposure, and whether it's accompanied by other symptoms.
According to provisional 2024 data from the CDC, there were still more than 2.2 million reported cases of chlamydia, gonorrhea, and syphilis in the United States, and overall STI case counts remain 13% higher than a decade ago. That figure only reflects reported cases of three infections. The real number of people walking around with an undiagnosed skin manifestation of an STD is substantially higher. Understanding what to look for, and when to stop guessing and just test, is genuinely useful information.
People are also reading: Can Condoms Prevent Trichomoniasis? What Safer Sex Really Looks Like
Which STDs Actually Cause Skin Rashes or Lesions
Not every STD produces visible skin changes, and not every skin change means an STD. But several common infections do have skin manifestations that bring people to their doctor or, more often, to a search engine. The ones most associated with rashes, sores, or lesions are syphilis, herpes (HSV-1 and HSV-2), HIV, gonorrhea (in its disseminated form), and scabies. Chlamydia and trichomoniasis are less commonly linked to visible rashes but can produce symptoms that get mistaken for skin conditions.
The table below gives a quick overview of which infections cause what kind of skin involvement, and whether those changes tend to be painful or not, which turns out to be one of the most useful diagnostic clues available before testing.
| Infection | Rash / Lesion Appearance | Body Location | When It Appears | Typically Painful? |
|---|---|---|---|---|
| Syphilis (primary) | Firm, round, painless ulcer (chancre) | Genitals, mouth, rectum, anus | 10–90 days after exposure (avg. 3 weeks) | Usually painless |
| Syphilis (secondary) | Rough, red-brown, non-itchy rash; may be subtle | Trunk, palms, soles of feet, face | 6 weeks to 3 months after primary sore | No |
| Herpes HSV-1 / HSV-2 | Clusters of fluid-filled blisters that ulcerate and crust | Genitals, anus, thighs, mouth | 2–12 days after exposure | Yes, often significantly |
| HIV (acute) | Flat, pink-red maculopapular rash; non-itchy | Trunk, face, arms | 2–4 weeks after exposure | Usually not |
| Gonorrhea (disseminated) | Small pustular or hemorrhagic spots | Arms, legs, near joints | Days to weeks after infection spreads | Sometimes |
| Scabies | Linear burrow tracks; intense widespread itch | Fingers, wrists, genitals, waistline | 2–6 weeks after first exposure; faster on re-exposure | Intensely itchy |
| Chlamydia / Trichomoniasis | Rarely causes visible rash; may cause genital irritation | Genital area | 5–10 days (chlamydia); 5–28 days (trich) | Variable |
The pain factor is significant. A lesion that is painless but won't go away, especially in the genital area, should never be dismissed as a pimple or friction rash. Syphilis sores are notoriously quiet. People can have one for three to six weeks and not notice it, particularly when it's inside the vaginal canal, rectum, or back of the throat. A painful cluster of blisters that appears with flu-like symptoms is a different picture, that's the pattern more consistent with herpes, particularly during a first outbreak.
It's also worth knowing that several STDs produce no skin symptoms at all. Chlamydia is one of the most common infections in the United States and often presents with zero visible signs, which is exactly why it spreads so efficiently. Someone can have chlamydia for months without any rash, bump, or discharge, and still transmit it to partners. This is why testing matters more than symptom-watching.
Syphilis: The Rash That Travels and Transforms
Syphilis has earned the nickname "the great imitator" for a reason. Its skin manifestations change completely depending on which stage of infection you're in, and in each stage, they can look like something else entirely. In the primary stage, the classic sign is a chancre, a single firm, round, painless ulcer at the site where the bacteria entered the body. It appears anywhere from 10 to 90 days after exposure, with three weeks being the typical average. Because it doesn't hurt, and because it heals on its own within three to six weeks, most people either don't notice it or assume it was nothing.
That disappearing act is part of what makes syphilis so dangerous. The sore going away does not mean the infection is gone. It means the disease has moved into its secondary stage, where things get more varied and harder to pin down. Secondary syphilis typically develops six weeks to three months after the initial sore appears, and it almost always produces a rash. This is the rash that shows up on the palms of the hands and the soles of the feet, an unusual location that is a strong clinical clue. It can also spread across the trunk, face, and the rest of the body. Critically, about 90% of secondary syphilis rashes do not itch, which sets them apart from most allergic, environmental, or viral rashes that people might otherwise confuse them with.
Secondary syphilis doesn't stop at the skin. The rash is usually accompanied by swollen lymph nodes, fatigue, sore throat, and sometimes fever or patchy hair loss. People frequently mistake the combination of a strange rash and flu-like symptoms for a viral illness. If you've had unprotected sex in the past three months and you notice a non-itchy rash appearing at the same time as what feels like a mild flu, that combination deserves a syphilis test, not a wait-and-see approach. The window for an accurate syphilis test is 6 weeks after exposure, and the test is a straightforward blood draw.
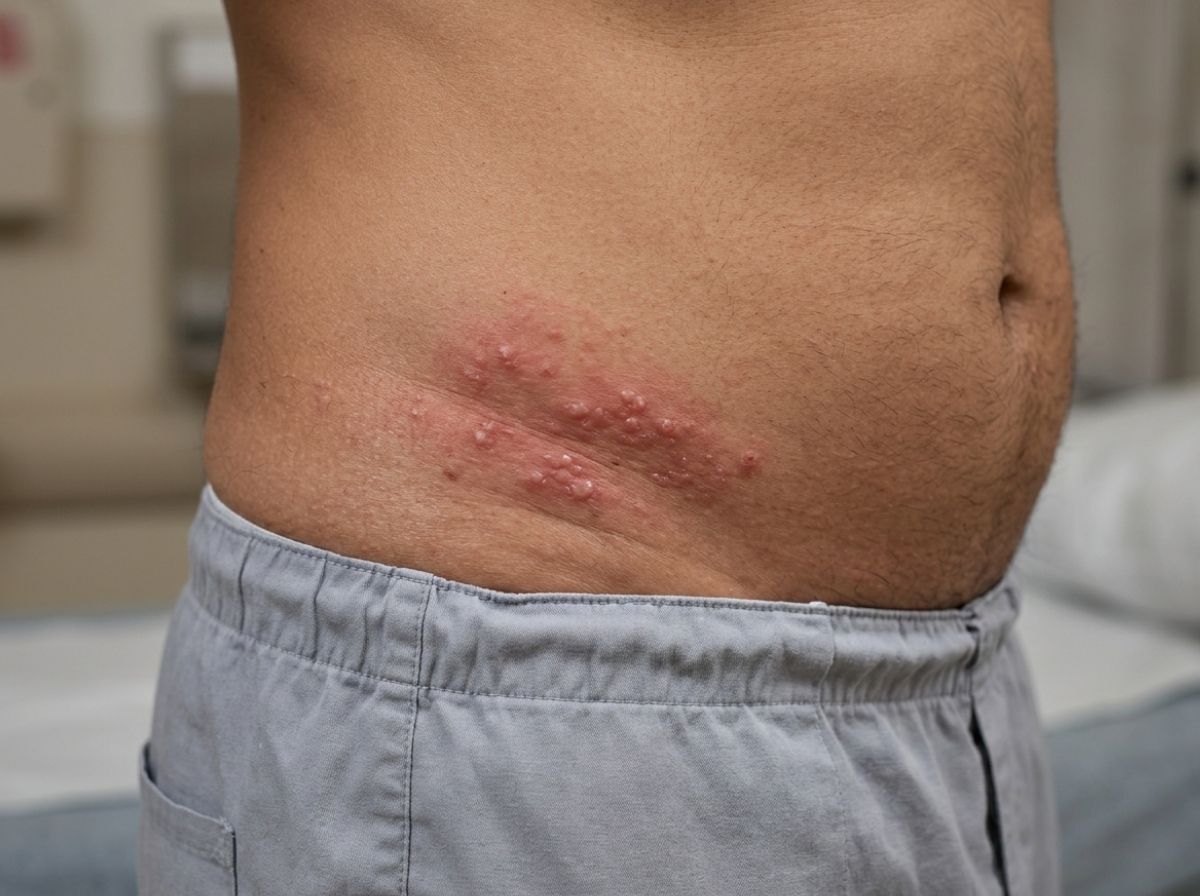
Herpes: What the Blisters Actually Look Like
The internet has convinced a lot of people that herpes is immediately obvious and dramatically painful. In reality, herpes exists on a spectrum. First outbreaks tend to be the most intense, producing clusters of fluid-filled blisters that break open into shallow, raw ulcers. These can be genuinely painful, burning during urination, discomfort when sitting, sensitivity even from clothing touching the area. The blisters typically appear within two to twelve days of exposure, often preceded by tingling, itching, or a sensation of heat in the affected area, sometimes called prodrome.
But many people's outbreaks are far milder than the textbook version. A small cluster of blisters that heals within a week, mild irritation that gets written off as friction or an ingrown hair, a single sore that seems to come and go, these are all within the range of how herpes can present. According to the CDC, the majority of people who have herpes either have no symptoms or symptoms mild enough that they go unrecognized for years. That's not a reassuring statistic for anyone hoping symptoms will tell the whole story.
HSV-1 and HSV-2 behave similarly once established. HSV-1 classically causes oral herpes, cold sores around the mouth, but can be transmitted to the genitals through oral sex. HSV-2 primarily causes genital herpes but can affect the mouth through the same route. Both types produce blisters that scab over and heal without scarring, a key difference from syphilis sores, which can leave marks. Herpes outbreaks also tend to recur, sometimes triggered by stress, illness, or changes in the immune system. The virus stays dormant in nerve tissue and can reactivate, though recurrent outbreaks are typically shorter and less severe than the first.
One of the most common questions people have is whether what they're seeing is herpes or something else entirely, ingrown hair, a pimple, folliculitis, or an allergic reaction. The distinguishing features of herpes are: the blisters appear in a cluster rather than a single isolated spot; they progress through stages from blistering to ulceration to crusting; they occur in areas consistent with skin-to-skin sexual contact; and they are typically preceded by that tingling or burning sensation. Ingrown hairs, by contrast, tend to be singular, close to the skin surface, surrounded by mild redness, and don't blister or ulcerate. If there's any doubt, the fastest way to settle the question is an at-home rapid test, not a Google Image comparison.
Check Your STD Status in Minutes
Test at Home with RemediumGenital Herpes Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $45.99 $49.00
How to Tell an STD Rash Apart from Common Look-Alikes
This is where most of the genuine confusion happens. The genital and groin area is skin like anywhere else, it reacts to friction, sweat, allergens, shaving, and heat. A lot of people convincing themselves they have an STD are dealing with something far less dramatic. And a smaller but meaningful group of people dismissing something as "just a rash" are missing a diagnosis they need. The difference between these two groups usually comes down to context and a few key clinical features.
Heat rash appears in skin folds where sweat accumulates and disappears within hours or a day when the area is cooled and dried. It never blisters and never crusts. Folliculitis, inflammation of hair follicles from shaving, waxing, or friction, produces small red bumps clustered around individual hairs, not in the spreading or clustered pattern typical of herpes. Yeast infections produce intense itching, a thick white discharge, and irritation of the vulvar area without sores or blisters. Allergic contact dermatitis from soaps, detergents, latex, or fabric produces a widespread, intensely itchy red rash that typically improves quickly once the irritant is removed. None of these involve the progression from bump to blister to ulcer that characterizes herpes, and none produce the firm, ulcerated sore of syphilis.
Before comparing conditions side by side, it helps to run through the three questions that matter most when a rash shows up in or around the genital area. Timing, location, and accompanying symptoms together paint a much clearer picture than appearance alone.
| Question to Ask | Points Toward STD | Points Away from STD |
|---|---|---|
| Timing: When did it appear? | Appeared days to weeks after unprotected sex or a new partner | Appeared after a new product, fabric, exercise, or shaving, with no recent sexual exposure |
| Location: Where exactly is it? | Genitals, anus, inner thighs, mouth, palms, or soles of feet | Areas with no sexual contact, back of knees, elbows, scalp (unless HIV-related) |
| Appearance: What does it look like? | Blister that ulcerates; firm painless sore; non-itchy red-brown spots on palms/soles | Bump near a hair follicle; rash that fades within hours; thick white discharge without sores |
| Pain profile: Does it hurt or itch? | Painful blisters with tingling beforehand (herpes); painless but firm and persistent (syphilis) | Itchy with no blistering and resolves quickly, more consistent with irritation or allergy |
| Accompanying symptoms, Anything else going on? | Fever, swollen lymph nodes, sore throat, fatigue, or unusual discharge alongside the rash | Symptoms tied clearly to a known cause, seasonal allergy, new medication, or heat |
| Duration: How long has it been there? | Persists beyond a week, doesn't respond to topical creams, or keeps coming back | Disappeared within 24–48 hours on its own with no recurrence |
Two or more answers in the "Points Toward STD" column, especially timing after sexual exposure combined with a persistent or blistering lesion, is enough reason to test. You don't need a full match. The checklist isn't a diagnosis; it's a decision tool. If you're sitting on the fence after running through it, that fence is exactly where a rapid at-home test becomes useful.
| Condition | Itchy? | Blisters / Sores? | Heals Without Treatment? | Key Distinguishing Feature |
|---|---|---|---|---|
| Herpes (HSV) | Sometimes | Yes, clusters | Temporarily, but recurs | Painful blisters that ulcerate and crust |
| Syphilis chancre | No | Firm ulcer | Yes (sore), but infection progresses | Painless, well-defined, solitary sore |
| Ingrown hair | Mildly | No, small bump | Yes, quickly | Visible hair beneath bump, near shaved area |
| Folliculitis | Mildly | Small pus-filled bumps | Yes | Clustered around individual hair follicles |
| Heat rash | Mildly | No | Yes, within hours | Disappears with cooling; no progression |
| Yeast infection | Intensely | No | Not without antifungal treatment | Thick discharge, no sores |
| Allergic reaction | Intensely | No | Yes, once irritant removed | Widespread, improves after removing product |
| Scabies | Intensely (especially at night) | Linear burrow tracks | No, requires treatment | Distinctive burrows between fingers, wrists |
The honest reality is that visual identification alone, even by an experienced clinician, is not definitive. Syphilis has been called a great imitator for over a century because its rashes and sores can genuinely look like other conditions. Herpes sores during mild or atypical outbreaks can be subtle enough to miss. If you've had a recent sexual exposure and something on your skin won't resolve within a few days, or if you notice a painless sore that seems to be lingering for weeks, the correct move is not to keep Googling, it's to test.
At-Home Testing: When to Test and What to Use
One of the most common mistakes people make after a potential STD exposure is testing too soon. Biology doesn't run on your timeline. Even if an infection is present, most tests need a window period, time for the body to produce detectable levels of the pathogen or the antibodies that signal infection. Testing before that window closes can produce a false negative that offers false reassurance. Knowing the correct window for each infection is not optional information.
If you're worried about a skin rash in the context of a recent sexual encounter, here are the exact testing windows to work with: for herpes (HSV-1 and HSV-2), test 6 weeks after exposure for the most reliable result. For syphilis, the same window applies, 6 weeks after exposure. For HIV, a first-indicator result is available at 6 weeks, but retesting at 12 weeks gives full certainty. If you're covering your bases and want to rule out chlamydia or gonorrhea alongside any skin concerns, chlamydia can be tested from 14 days after exposure and gonorrhea from 3 weeks after exposure.
For rash concerns specifically, the test you should take depends on what you're seeing. The table below maps rash type directly to the most relevant kit, along with the correct window period to wait before testing.
| If Your Rash Looks Like This | Most Likely Infection | Test to Take | Wait Until |
|---|---|---|---|
| Painful fluid-filled blisters that ulcerate and crust; tingling beforehand | Herpes HSV-2 (genital) or HSV-1 | Genital Herpes HSV-2 Rapid Test (98.2%) or Herpes HSV-1+2 2-in-1 (98.2%) | 6 weeks after exposure |
| Single firm, painless sore that won't heal; or non-itchy red-brown rash on palms and soles | Syphilis | Syphilis At-Home Rapid Test (99.4%) | 6 weeks after exposure |
| Flat, non-itchy pink-red rash on trunk or face alongside fever, fatigue, swollen glands | Acute HIV | HIV 1&2 At-Home Rapid Test (99.7%) | 6 weeks (retest at 12 weeks for certainty) |
| Intense nighttime itch; burrow tracks between fingers, wrists, or genitals | Scabies | Requires clinical diagnosis, see a healthcare provider; also consider a broader STD panel to rule out co-infection | As soon as possible |
| Genital irritation, discharge, or burning with no clear visible rash | Chlamydia or Gonorrhea | Chlamydia & Gonorrhea 2-in-1 (98%) | 14 days (chlamydia) / 3 weeks (gonorrhea) |
| Unsure, or multiple symptoms present after unprotected sex | Multiple possible | 7-in-1 Complete STD Test Kit (98.5%) | 6 weeks after exposure covers all infections above |
A positive result means you have actionable information. A negative result, taken at the correct window, means genuine peace of mind, not just a guess. Testing is the fastest way to stop the guessing game.
Scabies, Gonorrhea Rash, and the STDs That Affect Skin Differently
Not all STD-related skin changes follow the sore-or-rash pattern that most people picture. Scabies is caused by a microscopic mite, Sarcoptes scabiei, that burrows under the skin and lays eggs, triggering an immune response that produces one of the most intensely itchy rashes in medicine. The itch is characteristically worse at night, a feature so distinctive it's almost a diagnostic sign on its own. The skin changes in scabies look like thin, wavy lines or burrow tracks, most commonly found between the fingers, on the wrists, around the waistline, and on the genitals. This is not a typical STD in the sense that it can spread through any close or prolonged skin contact, sharing towels, bedding, or clothing can transmit it. But sexual contact is a very efficient transmission route, which is why it appears consistently in STD discussions.
Gonorrhea is primarily known for its urethral, cervical, rectal, and throat presentations, but in a small percentage of cases, particularly when the infection enters the bloodstream, it can produce skin involvement. Disseminated gonococcal infection (DGI) creates small reddish or purplish spots on the skin of the arms and legs, often associated with joint pain and fever. This is not a common presentation, but it's worth knowing that a widespread spotty rash appearing alongside joint pain and a recent sexual exposure is something that warrants immediate medical attention, not home treatment.
HIV can also produce skin changes during the acute phase of infection, typically two to four weeks after exposure. The HIV rash associated with acute infection is a flat, red-pink, maculopapular rash that appears on the trunk and sometimes the face and limbs. It doesn't itch much and occurs alongside fever, swollen lymph nodes, sore throat, and fatigue, symptoms that collectively resemble a severe flu. This combination is sometimes called acute retroviral syndrome, and it's the body's initial response to the virus entering the system. The rash typically resolves within a few weeks on its own, but the infection obviously does not.
People are also reading: Herpes Itching Explained: Which Stage It Happens and Why
New Developments: Emerging Skin Infections Spread Through Sexual Contact
The landscape of sexually transmitted skin conditions isn't static. In early 2026, public health officials in Minnesota issued a health advisory after identifying what they described as the country's largest known outbreak of TMVII, a fungal strain formally known as Trichophyton mentagrophytes genotype VII. According to CIDRAP, the infection causes round, coin-shaped rashes, red, irritated, and sometimes pustular, appearing on the genitals, buttocks, thighs, and trunk. It spreads through skin-to-skin contact, including during sex, and can also be transmitted via shared towels, clothing, and bedding.
What makes TMVII particularly relevant to any discussion of STD rashes is how easily it can be mistaken for other conditions. The CDC has noted that TMVII rashes are frequently misidentified as eczema, psoriasis, or other common skin conditions, leading to delayed or incorrect treatment. Minnesota's first confirmed case appeared in July 2025, when a patient sought care for a genital rash. The outbreak has since grown to more than 30 confirmed or suspected cases in the Twin Cities area, with scattered cases identified in larger U.S. cities. The infection is treatable, but treatment can last up to three months, and delayed diagnosis allows the rash to become more painful and persistent.
The practical takeaway is straightforward: a persistent skin rash in the genital area, particularly one that doesn't respond to topical treatments and that appeared after sexual contact, deserves evaluation beyond what you can find on a symptom-checker. Conditions previously considered outside the STD category are increasingly being identified as sexually transmissible. When in doubt, see a healthcare provider and consider STD testing as part of the workup, not an afterthought.
Rashes That Are NOT STDs, And How to Recognize Them
Most people who notice something unusual on their skin after sex do not have an STD. That's not false reassurance, it's just statistically true. The genital area is skin, and skin reacts to friction, sweat, heat, shaving, new products, and a dozen other things that have nothing to do with infection. One of the most useful things this article can do is help you recognize when what you're seeing is almost certainly not an STD, so you can stop spiraling and deal with the actual cause.
Folliculitis is probably the most common thing people mistake for herpes. It's an inflammation of the hair follicles caused by shaving, waxing, tight clothing, or friction during sex. It looks like small red bumps or pustules clustered around individual hairs in the pubic area or inner thighs. The key differences from herpes: the bumps sit directly at the base of a visible hair, they don't progress into blisters or ulcers, they don't appear in clusters spreading beyond the shaved area, and they typically resolve within a few days without any treatment. If you shaved recently and the bumps appeared within a day or two right along the shave line, folliculitis is the much more likely explanation.
Heat rash appears in skin folds where sweat gets trapped, the groin, inner thighs, and under the waistband are prime locations. It presents as small red bumps or a flushed, prickly area that appears quickly and resolves just as fast once the area is cooled and dried. The defining feature is its timeline: heat rash is essentially gone within hours. Nothing STD-related clears up in hours. If it appeared on a hot day after exercise or tight clothing and was gone by the time you showered, it wasn't herpes.
Contact dermatitis, an allergic or irritant reaction, is extremely common in the genital area precisely because the skin there is sensitive. Scented soaps, bubble baths, latex condoms, spermicides, fabric softeners, and synthetic underwear are all frequent culprits. The rash is typically widespread rather than localized to a specific point, intensely itchy, and improves noticeably within 24 to 48 hours of removing the offending product. There are no blisters, no ulcers, and no progression, just redness and irritation that fades when the irritant is gone. Switching to unscented, pH-neutral products and cotton underwear often resolves it completely.
Ingrown hairs deserve their own mention because they generate a disproportionate amount of STD anxiety. An ingrown hair produces a single raised bump, sometimes with a visible hair trapped beneath the surface, sometimes with a small white head, that is mildly tender when pressed. It doesn't spread, doesn't ulcerate, and doesn't come with flu-like symptoms. It appears near areas that have been shaved or waxed and typically resolves on its own within a week. Compare that to a syphilis chancre, which is firm, well-defined, and appears weeks after exposure at the exact site of sexual contact, or to herpes, which starts with tingling and progresses to a cluster of blisters. These are not the same thing, even when anxiety makes them feel like it.
Jock itch (tinea cruris) is a fungal infection, the same family as athlete's foot, that thrives in warm, moist skin folds. It produces a red, scaly, ring-shaped rash in the groin and inner thighs that is itchy but doesn't blister or ulcerate. It's not sexually transmitted and responds well to over-the-counter antifungal treatment. If the rash is in the crease of the groin, has a slightly raised scaly border, and has been building gradually over days, jock itch is far more likely than any STD.
| Condition | What It Looks Like | Key "Not an STD" Clues | Typical Resolution |
|---|---|---|---|
| Folliculitis | Small red bumps at hair follicles | Appeared after shaving; sits at hair base; no blistering | Days, on its own |
| Heat rash | Red, prickly bumps in skin folds | Appeared in heat; gone within hours of cooling | Hours |
| Contact dermatitis | Widespread redness and itch | Linked to new product; no sores; improves after removal | 24–48 hours |
| Ingrown hair | Single raised bump, sometimes with trapped hair | Near shaved area; visible hair; doesn't ulcerate or spread | Under a week |
| Jock itch | Red, scaly, ring-shaped rash in groin folds | Gradual onset; scaly border; no blisters; responds to antifungal | Days to weeks with treatment |
| Yeast infection | Redness, swelling, thick white discharge | No sores or blisters; intense itch; discharge present | Days with antifungal treatment |
The honest bottom line: if your rash appeared quickly, is tied to an obvious cause like shaving or a new product, doesn't involve blistering or a firm persistent sore, and is already improving, you probably don't need an STD test for that specific rash. If it's lingering, progressing, or appeared in the context of a recent sexual exposure with no other obvious cause, testing is the right call. The goal isn't to test for everything all the time, it's to know when testing actually makes sense.
When to Test, When to See a Doctor, and What Comes Next
There's a spectrum of urgency here, and knowing where your situation falls is genuinely useful. A rash that appeared after using a new laundry detergent, improved after stopping use, and doesn't involve sores or blisters is probably not an STD. A single firm, painless sore that appeared in the genital area two to four weeks after unprotected sex and hasn't gone away after three weeks, that gets a syphilis test, full stop. Flu-like symptoms alongside a new rash or skin changes within a few weeks of a sexual exposure, that's worth a comprehensive STD panel, not a guess.
At-home rapid testing covers a wide range of the most common infections efficiently and privately. But there are situations where in-person evaluation adds something a rapid test can't provide: visual examination of an active lesion, swab testing of a blister or sore for herpes identification during an active outbreak, or assessment for conditions like TMVII or DGI that require clinical judgment. If you have a sore or lesion that is actively present, a swab taken during that active phase is significantly more accurate for herpes detection than a blood-based antibody test. Both matter, but timing changes which test gives the most information.
Getting a positive result is not the end of a conversation, it's the beginning of one with a healthcare provider. The vast majority of bacterial STDs (chlamydia, gonorrhea, syphilis) are curable with treatment. Viral infections like herpes and HIV are manageable with appropriate care. Knowing your status is always better than not knowing it. Testing is not a sign that something has gone wrong, it's what responsible sexual health looks like in practice.
Check Your STD Status in Minutes
Test at Home with Remedium8-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $149.00 $392.00
For all 8 tests
FAQs
1. Can chlamydia cause a skin rash?
Chlamydia rarely causes a visible skin rash directly. In most cases, it produces no external skin changes at all, which is a big part of why it spreads so widely undetected. Occasionally, chlamydia affecting the throat or rectum can cause localized irritation, but the classic presentation is discharge and burning rather than a rash. If you have a rash alongside chlamydia symptoms, another STD may also be present, since co-infections are common.
2. What does a syphilis rash look like on the hands and feet?
The secondary syphilis rash on the palms and soles tends to appear as rough, reddish-brown spots that are slightly raised and don't itch. The fact that it affects the palms and soles is one of the most distinctive features, very few other rashes consistently show up in those locations. It can be subtle enough to look like dry skin at first glance, which is part of why it gets missed.
3. How do I know if a genital sore is herpes or something else?
The key features that point toward herpes are: a cluster of small blisters that progressed from tingling to visible blisters to ulcers; the sores being painful or sensitive; and their location being consistent with a sexual contact site. A single painless sore that doesn't blister is more suggestive of syphilis. An ingrown hair sits close to the surface, near a hair follicle, and doesn't ulcerate. Testing during an active outbreak using a swab is the only reliable way to confirm herpes.
4. Can an STD rash go away on its own?
Some STD-related skin changes do resolve without treatment, syphilis sores disappear on their own, and the secondary rash fades. But the underlying infection does not go away. A rash clearing up is not a sign the STD is gone; it can mean the infection has progressed to a later, less visible stage. Always treat disappearing symptoms as reason to test, not reason to stop worrying.
5. How long does a herpes outbreak last?
A first herpes outbreak typically lasts two to four weeks from the appearance of initial symptoms to full healing. Recurrent outbreaks are usually shorter, often resolving within seven to ten days. Prodrome symptoms, the tingling or burning before blisters appear, can begin one to two days before visible lesions emerge. The blisters themselves usually burst within three to five days and then crust over before healing.
6. Can you get an STD rash without having sex?
Scabies can be transmitted through non-sexual close contact, sharing towels, clothing, or bedding with someone who has the infection. Herpes can theoretically be transmitted through non-sexual skin-to-skin contact if there's an active outbreak or viral shedding, though sexual contact is by far the most common route. Most other STD-related skin changes require sexual activity for transmission.
7. What is the HIV rash and when does it appear?
The rash associated with acute HIV infection typically appears two to four weeks after exposure. It's a flat, pink-to-red, non-itchy rash that develops on the trunk and sometimes the face and arms. It occurs during acute retroviral syndrome, alongside fever, swollen lymph nodes, sore throat, and fatigue. The rash fades on its own within a few weeks, but the infection persists. HIV can be tested from 6 weeks after exposure for a first-indicator result, with retesting at 12 weeks for full certainty.
8. Is a rash on my inner thigh always an STD?
No, the inner thigh is a common location for friction rash, folliculitis, heat rash, and fungal infections like jock itch, none of which are sexually transmitted. That said, herpes and syphilis can both produce lesions in the inner thigh area, particularly if that area was involved in sexual contact. Context matters: if the rash appeared after unprotected sex, involves blistering or a firm sore, and hasn't resolved within a few days, testing is the appropriate next step.
9. How soon after unprotected sex should I test for an STD if I have a rash?
The window periods determine how soon a test will be accurate: chlamydia from 14 days, gonorrhea from 3 weeks, syphilis and herpes from 6 weeks, and HIV from 6 weeks (with confirmation at 12 weeks). If you have an active sore or blister, a swab during the active outbreak can give faster, more accurate herpes-specific results. Don't test earlier than the window period and interpret a negative as reassurance, retest at the correct window if you tested too early.
10. Can scabies be mistaken for an STD?
Yes, and in the other direction too. Scabies in the genital area can be mistaken for an STD rash, and STD-related rashes can sometimes be dismissed as scabies or a general skin condition. The distinctive features of scabies are the burrow tracks (thin, wavy lines under the skin surface), the extreme nighttime itching, and the locations where it tends to cluster, between the fingers, on the wrists, and around the genitals. If you or a partner have an intensely itchy genital rash with no blistering, scabies should be part of the diagnostic conversation alongside STDs.
Test with Confidence, At-Home Kits That Give You Real Answers
If something on your skin has you questioning your status, the most useful thing you can do right now is test. Not in a week. Not after one more Google search. The sooner you know, the sooner you can either stop worrying or start dealing with the situation on your terms. STD Rapid Test Kits offers discreet, accurate at-home options that deliver results in minutes without a lab visit, a doctor's appointment, or anyone else knowing you tested.
For skin-specific concerns, the Syphilis At-Home Rapid Test Kit (99.4% accuracy) and the Genital Herpes HSV-2 At-Home Rapid Test Kit (98.2% accuracy) are the most directly relevant starting points. If your exposure was recent and unprotected, a broader panel makes more sense, the Complete 8-in-1 STD At-Home Rapid Test Kit (99% accuracy) covers herpes HSV-2, chlamydia, gonorrhea, syphilis, HIV, hepatitis B, and hepatitis C in a single kit at the right window periods. Women looking for the most comprehensive coverage available can also consider the Women's 10-in-1 Complete At-Home Test Kit, which adds trichomoniasis and HPV 16 & 18 to the full panel.
Your sexual health decisions belong to you. Testing is what makes those decisions informed ones. Visit STD Rapid Test Kits to find the right kit for your situation and get results the same day.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC, Sexually Transmitted Infections Surveillance, 2024 (Provisional)
4. CIDRAP, Minnesota Health Officials Warn of Sexually Transmitted Fungal Infection Outbreak
6. ACOG, Chlamydia, Gonorrhea, and Syphilis: Patient FAQ
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: March 2026
This article is for informational purposes and does not replace medical advice.