Spotting, Burning, or Silence? The Truth About HIV Symptoms
Last updated: April 2026
A rash that shows up a couple of weeks after a sexual encounter can send anyone into a spiral. Is it heat rash? An allergy? Something worse? When HIV is a possibility, that question becomes urgent, and the answer matters more than most people realize. This article breaks down exactly what an HIV rash looks like, when it appears, what causes it, how it differs from other rashes, and, critically, when and how to test. Whether you're trying to identify a current symptom or simply want to understand what early HIV infection actually looks like, here's what you need to know.
People are also reading: Condom Slipped Off During Sex: What to Do Next and Your Real STD Risk
What Does an HIV Rash Actually Look Like?
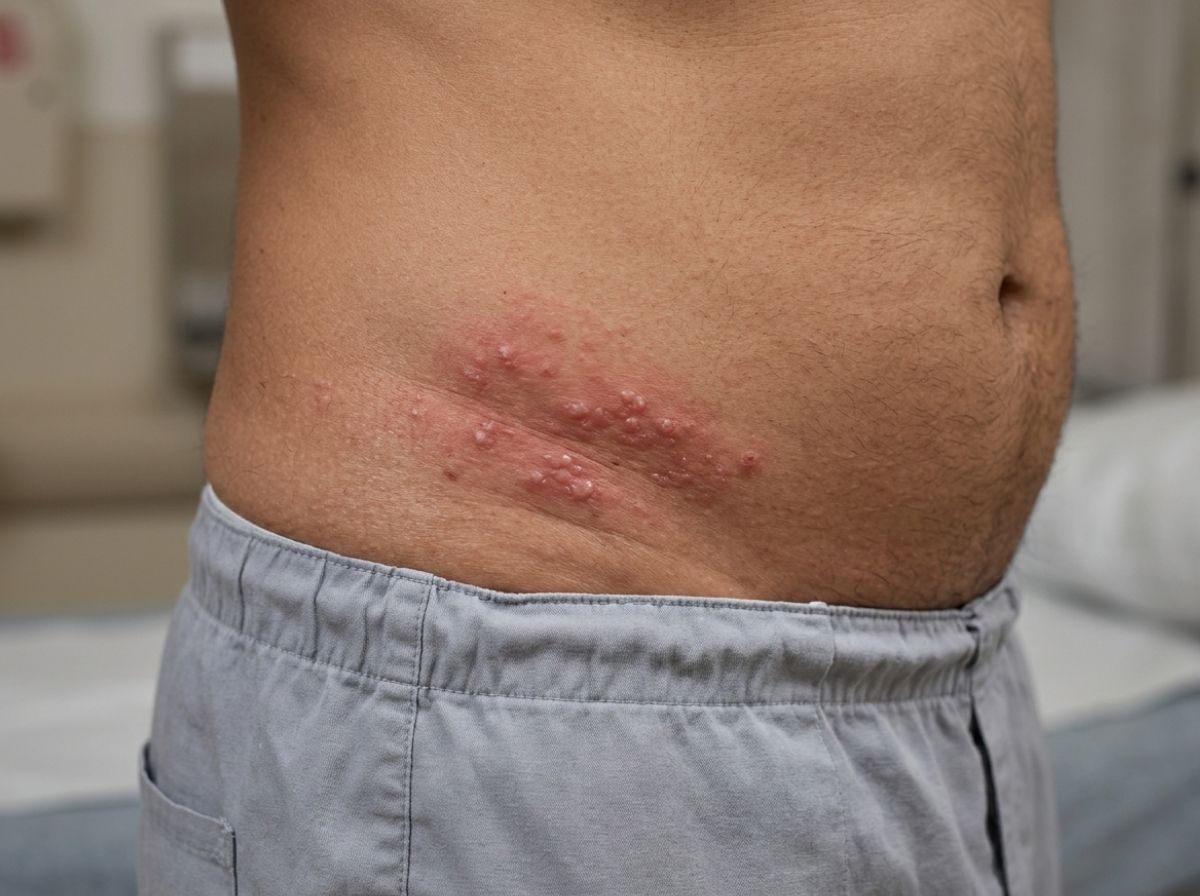
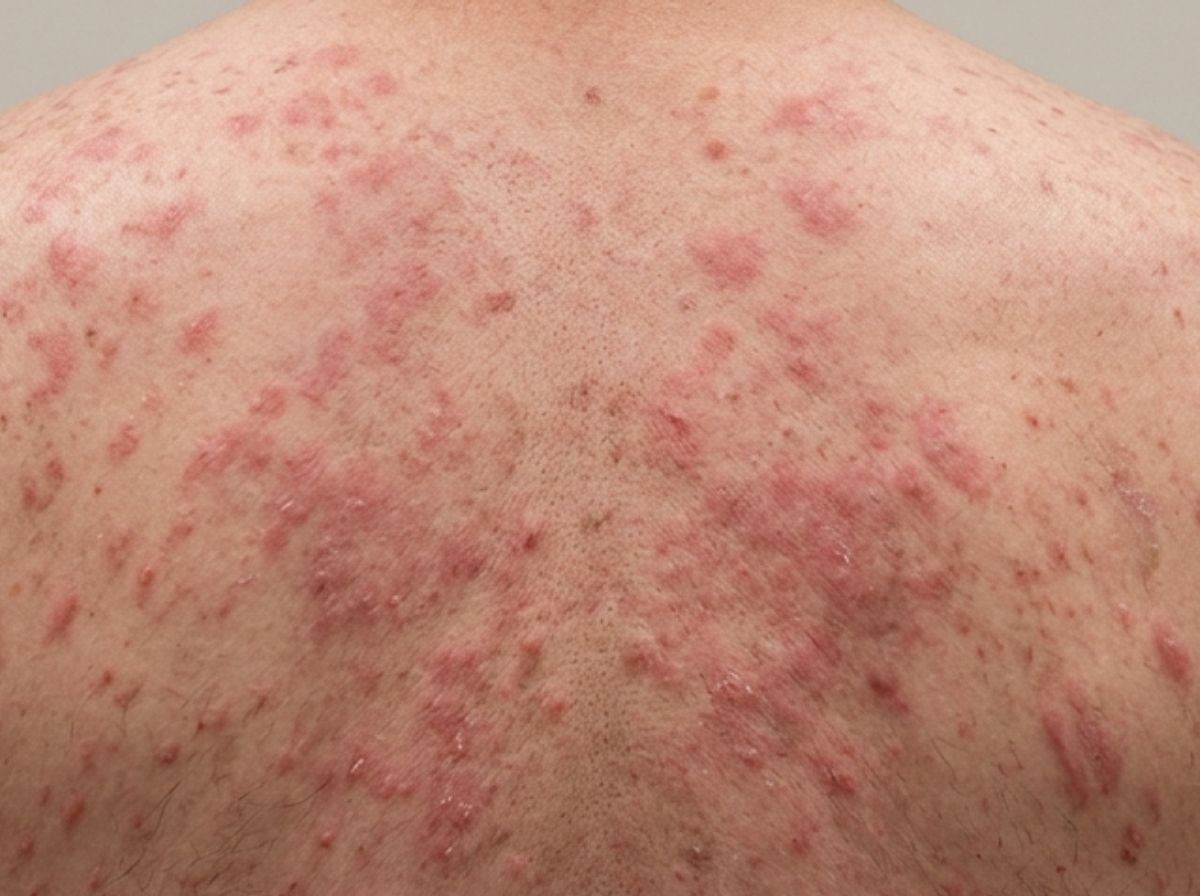
Picture waking up and noticing a scattering of pink or reddish patches across your chest or upper back, nothing dramatic, nothing that screams "emergency." That's actually what most acute HIV rashes look like. They're easy to miss, easy to write off, and that's precisely what makes them clinically significant. If you're aware of recent potential HIV exposure and a rash appears, dismissing it as heat rash or a soap allergy is a costly mistake.
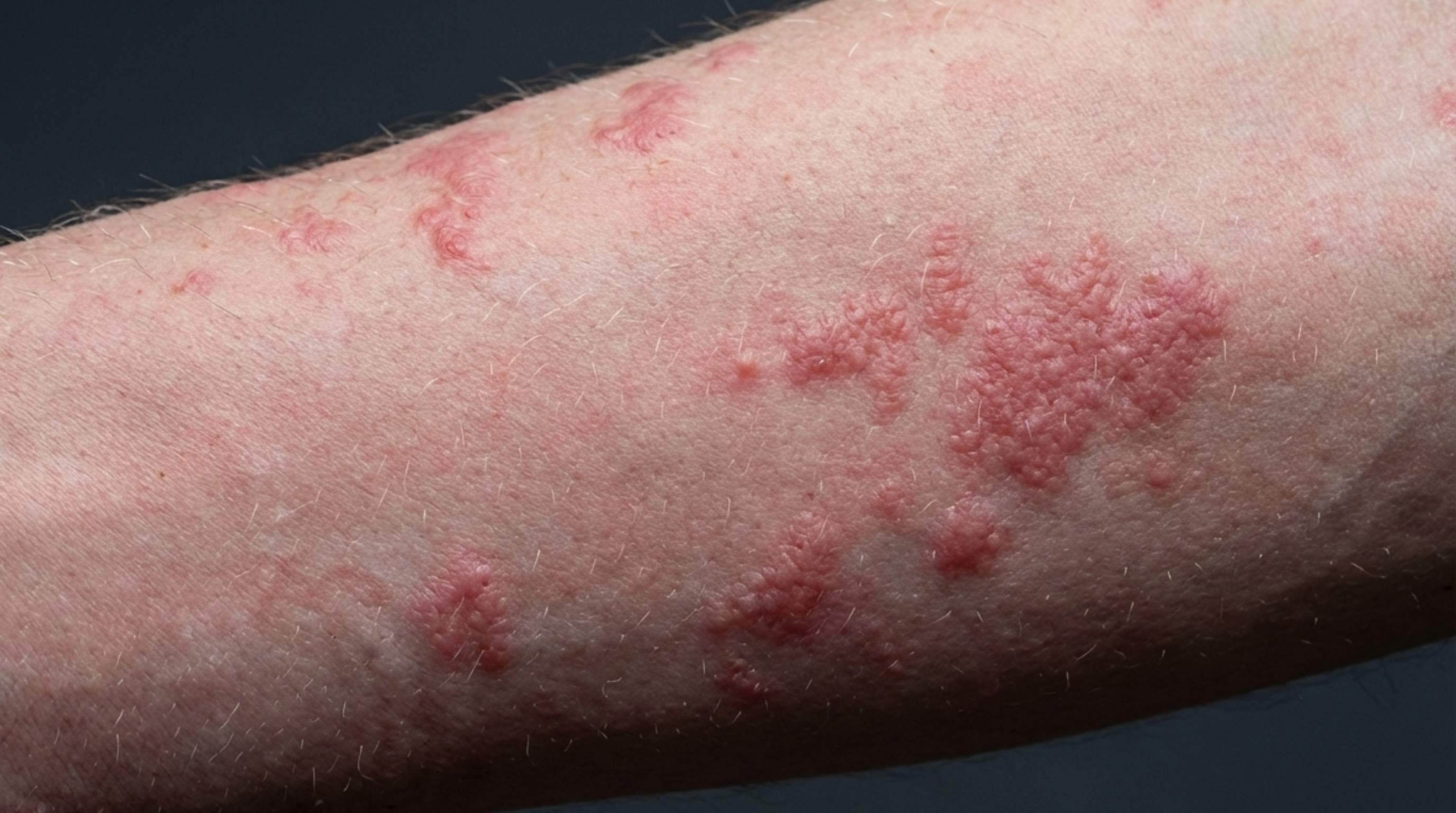
The rash itself is typically described as maculopapular, a combination of flat discolored patches (macules) and slightly raised bumps (papules). The color varies significantly depending on skin tone. On lighter skin, the rash tends to appear pink to red. On medium to darker skin tones, it often looks darker, brownish, reddish-purple, or even deep purple, which can make it harder to spot without good lighting. The bumps are usually symmetrical, meaning they appear in similar patterns on both sides of the body, and they rarely blister or become crusty in the early stage.
The rash most commonly affects the torso, chest, back, and abdomen, along with the face, neck, and arms. Less frequently it appears on the palms of the hands or soles of the feet, though this pattern is more characteristic of secondary syphilis (worth knowing, since the two are sometimes confused). The rash isn't typically dramatic or isolated to one spot; it usually covers a broader area in a diffuse pattern. Mild itching can occur, but many people describe their acute HIV rash as barely itchy at all, which ironically makes it easier to overlook.
| Skin Tone | Typical Rash Color | Appearance | Most Common Locations |
|---|---|---|---|
| Fair / Light | Pink to red | Flat or slightly raised patches, sometimes with small bumps | Chest, back, face, arms |
| Medium / Olive | Red to reddish-brown | Diffuse, may have rough or elevated texture | Torso, neck, limbs |
| Dark / Deep | Dark purple to dark brown | Can be subtle, symmetric patches | Chest, back, face, limbs |
How long does the rash last? In the acute stage, it generally resolves on its own within one to two weeks, sometimes as quickly as a few days. That disappearance does not mean the virus is gone. It means the initial immune response phase is ending. The virus is still present, still replicating, and still transmissible. This is an important distinction: the rash clearing up is not a green light, it's a reason to go get tested.
The Three Types of HIV-Related Rashes
Not every rash connected to HIV looks the same, and not every HIV rash means the same thing. There are three distinct categories of rashes that can occur in people with HIV, and understanding which type is which changes how urgent the response should be. Conflating them, or assuming that all HIV rashes are early-stage and minor, can lead to missed warning signs.
The first is the acute HIV rash, the one most people are referring to when they search "HIV rash." This appears during the primary infection phase, typically two to four weeks after exposure, as the immune system mounts its first response to the virus. According to the NIH's HIVinfo, this type of rash is a direct result of the immune system fighting the virus, and it tends to resolve without treatment. The problem isn't its severity, it's the false reassurance that comes when it disappears on its own.
The second type involves rashes caused by opportunistic infections. Without effective treatment, HIV progressively damages the immune system, allowing pathogens the body would normally suppress to cause serious problems. Conditions like herpes zoster (shingles), molluscum contagiosum, fungal infections, and Kaposi's sarcoma can all produce skin changes in people living with HIV. These rashes are not early-stage warning signs, they're indicators that the immune system is already substantially compromised. The appearance varies widely depending on the specific infection involved, but they tend to be more persistent, more painful, and less likely to resolve on their own compared to the acute HIV rash.
The third kind is caused by drugs. Antiretroviral therapy works and can change your life, but some HIV medicines can make your skin allergic. These rashes can show up in the first few weeks of treatment. They usually look like pink or red spots, and sometimes they have raised bumps on them. Most rashes caused by medications are not serious and go away on their own in a few weeks. But in very rare cases, a medication rash can be a sign of a serious hypersensitivity reaction, such as Stevens-Johnson Syndrome (SJS), which can be life-threatening. Anyone with HIV who gets a rash along with a fever, blisters, or trouble breathing should see a doctor right away. This is not a wait-and-see situation.
Check Your STD Status in Minutes
Test at Home with RemediumHIV Rapid Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $33.99 $49.00
HIV Rash vs. Other Rashes: How to Tell the Difference
Here's the honest truth: you cannot definitively identify an HIV rash just by looking at it. No one can, not from a photo, not from a description, and not from a symptom checker. The acute HIV rash looks almost identical to rashes caused by other viral infections, allergic reactions, heat, medication side effects, and common skin conditions like eczema or pityriasis rosea. The internet is full of people trying to self-diagnose from images, and it almost never works. What the rash looks like is one data point. When it appeared, and in what context, matters far more.
That said, there are a few patterns that raise the likelihood of HIV involvement. The key contextual clues are timing and symptom clustering. An acute HIV rash rarely appears in isolation, it almost always comes alongside other symptoms of what's called acute retroviral syndrome: fever, fatigue, swollen lymph nodes, sore throat, muscle aches, and sometimes mouth ulcers. This collection of symptoms together, appearing two to four weeks after a potential HIV exposure, is the real signal. A rash alone, with no other symptoms and no known exposure, is far less likely to be HIV-related.
The most commonly confused conditions include heat rash (miliaria), which appears in hot and humid conditions and tends to be itchier with more uniform tiny bumps. Drug reactions can look almost identical to an HIV rash, which is why medication history matters. Syphilis can produce a rash, classically on the palms and soles, that's worth knowing about since syphilis and HIV share transmission routes and are sometimes acquired together. Pityriasis rosea produces a distinctive "herald patch" followed by a widespread secondary rash. Eczema and psoriasis tend to be more chronic and are usually accompanied by a personal or family history. The honest bottom line: if you're worried about HIV exposure and you have a rash, get tested. That's the only way to actually know.
| Condition | Typical Appearance | Timing / Context | Key Distinguishing Feature |
|---|---|---|---|
| Acute HIV Rash | Flat or raised red/purple patches; symmetric | 2–4 weeks after possible exposure | Appears alongside flu-like symptoms; resolves in 1–2 weeks |
| Heat Rash | Tiny, uniform itchy bumps | During or after heat exposure | No fever or lymph node involvement; resolves with cooling |
| Drug Reaction | Variable; often widespread | Within days to weeks of starting a new medication | Direct link to medication start date |
| Syphilis Rash | Rough, reddish-brown spots | Weeks after a sore appears | Often on palms and soles; doesn't itch |
| Pityriasis Rosea | Oval patches with a herald patch first | Spontaneous onset, no known exposure | "Christmas tree" pattern on back; usually not systemic |
| Eczema | Dry, scaly, intensely itchy | Chronic or recurring | Usually has personal/family history; appears in skin creases |
When and How to Test for HIV After a Rash
If you've noticed a rash two to four weeks after potential HIV exposure, whether through unprotected sex, a shared needle, or any other route of transmission, this is the moment to act. Not in a few more weeks once you see if it clears up. Now. The reason timing matters this much is that the window period for HIV testing is real, and testing too early produces unreliable results regardless of whether an infection is present.
For HIV specifically, the testing window is 6 weeks after exposure for a first meaningful result. This is because most HIV tests detect antibodies, proteins the immune system produces in response to the virus, and it takes the body some time to generate detectable levels of those antibodies. Testing at day seven or even day fourteen is unlikely to give you reliable results. Testing at 6 weeks after exposure provides a strong initial indicator, and retesting at 12 weeks confirms certainty. These are the numbers to work with, not vague guidance like "wait a little while" or "test soon."
At-home rapid HIV tests are one of the fastest, most private ways to get an answer. The HIV 1&2 At-Home Rapid Test Kit from STD Rapid Test Kits delivers results in minutes with 99.7% accuracy, no lab visit, no clinic, no waiting room. The process is straightforward: a simple finger-prick blood sample, a waiting period of a few minutes, and a clear result. If the result comes back positive, that's not the end of the story, it's the beginning of a treatment plan. If it comes back negative but you tested before the 6-week mark, retest. If it comes back negative at 12 weeks, you can be highly confident in that result.
One thing worth knowing: the acute phase of HIV, the period when the rash typically appears, is also when the virus is at its highest concentration in the blood. This is the phase of highest transmissibility. If you suspect you're in this window, being careful about sexual contact and informing recent partners is important, not just for your health but theirs.
People are also reading: Can a Baby Be Born With Syphilis? What Congenital Syphilis Means
Other Symptoms That Appear Alongside the HIV Rash
The rash rarely travels alone. During the acute phase of HIV infection, the body launches what's called an acute retroviral syndrome, essentially a whole-body immune response to the sudden presence of a fast-replicating virus. Most people experience this as something that feels like a bad flu, and many dismiss it exactly that way. It is, in the early days, almost indistinguishable from influenza or mononucleosis. The difference becomes meaningful in retrospect, especially when testing reveals what was actually happening.
Alongside the rash, common symptoms of acute HIV infection include fever, often described as persistent and notable rather than mild, swollen and tender lymph nodes in the neck, armpits, or groin, extreme fatigue, sore throat, muscle aches, night sweats, and sometimes mouth ulcers. According to HIV.gov, around two-thirds of people experience some form of flu-like symptoms within two to four weeks of infection. The rash fits within that broader picture. Its significance increases substantially when it appears together with these other symptoms rather than in isolation.
What happens after the acute phase is another reason early testing matters so much. Once the initial immune response settles, HIV infection typically enters a chronic phase where the virus continues to replicate, but far more quietly. Many people experience no noticeable symptoms for years. This asymptomatic period doesn't mean the virus is harmless; it means the damage is happening out of sight. Without treatment, the immune system gradually loses the cells (CD4 T-lymphocytes) it needs to fight off other infections. By the time significant symptoms return, the disease has progressed considerably. Catching it early, even at the rash stage, changes the entire treatment trajectory.
What the Rash Tells You About HIV Progression
The context of a rash in someone's HIV journey says a lot about where they are in that journey. An acute HIV rash appearing two to four weeks after exposure is a very different situation from a persistent skin condition developing in someone who has been living with untreated HIV for years. Both matter, but they require different responses and carry different implications.
In the early acute phase, the rash is a sign that the immune system is responding, that the body is aware something is wrong and is mobilizing against it. At this point, viral load (the amount of virus circulating in the blood) is extremely high, which is part of why the immune response is so pronounced. The CDC's latest surveillance data indicates that in 2023, over 39,000 people in the United States received a new HIV diagnosis, and roughly 21% were already at stage 3 (AIDS) at the time of diagnosis, suggesting they had been living with undetected infection for a long time. The rash stage is precisely when early detection has the greatest impact.
In someone who has been living with HIV without adequate treatment, rashes take on a different meaning. Skin conditions in advanced HIV are often caused by opportunistic infections, pathogens that the immune system can no longer suppress effectively. These might include herpes zoster (shingles), which reactivates when CD4 counts drop, or fungal infections that produce persistent skin changes, or in the most advanced cases, Kaposi's sarcoma, a type of cancer associated with AIDS that produces dark red, brown, or purple lesions. These are not early-warning symptoms. They're signals that the immune system is severely compromised and that treatment, if not already underway, is urgently needed.
Managing and Treating HIV-Related Skin Rashes
Managing an HIV rash depends almost entirely on identifying its cause. If the rash is part of the acute phase and you haven't yet started treatment, the rash itself will likely resolve within one to two weeks without any specific intervention. That doesn't mean there's nothing to do, it means that the most important action isn't a cream or antihistamine, it's getting tested and evaluated by a healthcare provider as quickly as possible so that treatment can be started if needed.
For symptom relief in the meantime, keeping the skin cool and well-moisturized helps reduce irritation. Avoiding direct sun exposure and hot showers can prevent the rash from worsening. Over-the-counter hydrocortisone cream can reduce mild inflammation, and antihistamines may help if there's significant itching. These are comfort measures, they address the symptom, not the underlying condition. Never stop or alter any HIV medication without consulting a doctor, even if you suspect the medication is causing a rash.
For medication-induced rashes, the approach depends on severity. Mild rashes that appear shortly after starting a new antiretroviral medication often resolve on their own within weeks. If the rash persists, worsens, or is accompanied by systemic symptoms like fever or blistering, a medication change may be necessary. This needs to be managed by a doctor, there are now multiple highly effective antiretroviral regimens available, and finding one that works well for each individual without causing severe side effects is absolutely achievable. The key message here is straightforward: effective treatment exists, options exist, and a rash caused by one medication is not a reason to abandon treatment altogether.
Check Your STD Status in Minutes
Test at Home with Remedium8-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $149.00 $392.00
For all 8 tests
FAQs
1. What does an HIV rash look like exactly?
The acute HIV rash is typically a maculopapular rash, a mix of flat discolored patches and slightly raised bumps that appears across the torso, chest, back, and sometimes the face and arms. On lighter skin tones it tends to look pink to red; on medium to darker skin tones it often appears reddish-brown, dark purple, or deep brown, which can make it subtler and easier to miss. The rash is usually symmetrical, covering both sides of the body in a similar pattern, and it doesn't blister or crust in the early stage. Mild itching can occur, but many people describe it as barely itchy at all, which is part of why it gets dismissed.
2. When does an HIV rash appear after exposure?
The acute HIV rash typically appears two to four weeks after exposure, during what's called the primary infection phase. This is when the immune system is mounting its first major response to the virus, producing cytokines and inflammatory signals that drive the skin changes. It doesn't appear immediately after exposure; the body needs time to recognize and begin fighting the virus. If a rash shows up within a day or two of a potential exposure, that timeline is too fast for it to be the acute HIV rash.
3. How long does an HIV rash last?
The acute HIV rash usually resolves on its own within one to two weeks, sometimes faster. This can create a false sense of relief, the rash clears, other symptoms fade, and it's tempting to assume nothing was wrong. But the disappearance of the rash means the acute phase is ending, not that the virus is gone. HIV continues to replicate during the chronic phase that follows, often with no symptoms at all for years. The rash going away is a reason to test, not a reason to stop worrying.
4. Can you get an HIV rash without any other symptoms?
It's possible, but the rash appearing entirely in isolation is less typical. During the acute phase, the HIV rash almost always occurs alongside other symptoms of acute retroviral syndrome, fever, fatigue, swollen lymph nodes, sore throat, and muscle aches. This cluster of symptoms together, appearing two to four weeks after potential exposure, is the real clinical signal. A rash on its own with no other symptoms and no known exposure is far less likely to be HIV-related, though only a test can rule it out definitively.
5. Does the HIV rash itch?
It can, but mild or absent itching is actually more characteristic of the acute HIV rash than intense itching, which sets it apart from conditions like eczema or heat rash that are typically intensely itchy. Medication-induced rashes associated with antiretroviral therapy can itch more noticeably. The takeaway is that if your rash is barely itchy but accompanied by fever, swollen lymph nodes, and fatigue after a potential exposure, that combination is more significant than the itching level alone. Don't rule out HIV because the rash "isn't itchy enough."
6. Can I tell if I have HIV just by looking at the rash?
No, and this is one of the most important things to understand about the HIV rash. The acute rash looks virtually identical to rashes caused by other viral infections, allergic reactions, drug side effects, and common skin conditions. Even an experienced clinician cannot diagnose HIV from a rash alone. What matters is the full picture: whether there was a potential exposure in the past two to four weeks, whether the rash is accompanied by fever and flu-like symptoms, and whether a test taken at the correct window confirms or rules out infection. The rash is a reason to test, not a diagnosis.
7. When should I get tested for HIV if I have a rash?
If you have a rash and a possible HIV exposure, start thinking about testing now, but understand that the timing of the test determines whether the result is meaningful. HIV tests detect antibodies your immune system produces in response to the virus, and those antibodies take time to reach detectable levels. Testing before 6 weeks after exposure risks a false negative even if infection is present. Test at 6 weeks for a first meaningful result, and retest at 12 weeks for full certainty. If you're in the acute window right now, that's also the period of highest viral load and transmissibility, being cautious about sexual contact in the meantime matters.
8. Can an HIV rash appear years after initial exposure?
Yes, but late-stage rashes are a completely different phenomenon from the acute HIV rash. If HIV goes untreated for years, the immune system gradually loses its ability to suppress other pathogens. Rashes that appear later in HIV infection are usually caused by opportunistic infections, herpes zoster, fungal infections, molluscum contagiosum, or in advanced cases, by Kaposi's sarcoma, which produces dark red or purple lesions associated with AIDS. These are not early warning signs; they're indicators of significant immune compromise. Any new or persistent rash in someone living with HIV should be evaluated by their healthcare provider promptly.
9. Is the HIV rash itself contagious?
The rash itself is not contagious, it's a skin reaction driven by the immune system's response to the virus, not a surface infection that can spread through touch. However, the person experiencing the rash is in the acute phase of HIV infection, which is the period of highest viral load and highest transmissibility. The virus spreads through blood, semen, vaginal fluids, rectal fluids, and breast milk, not through the rash, but the timing of the rash coincides with when HIV is most efficiently transmitted through sexual contact.
10. If my rash is caused by HIV medication, should I stop taking it?
No, stopping antiretroviral medication without medical guidance is dangerous and should not be done. Most medication-related rashes that appear shortly after starting a new HIV treatment are mild and resolve on their own within a few weeks. They don't require stopping the medication. However, there are exceptions: if the rash is accompanied by fever, blistering, mouth sores, or difficulty breathing, these could signal a serious hypersensitivity reaction like Stevens-Johnson Syndrome, which is a medical emergency. In that situation, seek immediate medical attention. For anything short of that, contact your prescribing provider before making any changes to your treatment plan.

People are also reading: Did Houston Really Have 42,000 STD Cases This Spring Break?
Know Your Status, Testing Is the Next Step
A rash that appears weeks after a potential HIV exposure isn't something to watch and wait on. It's a signal worth taking seriously, and the fastest way to take it seriously is to get tested at the right time. HIV is highly manageable when caught early, modern treatment allows people living with HIV to maintain full, healthy lives and even achieve an undetectable viral load, which means they cannot transmit the virus to sexual partners. That outcome starts with knowing your status.
The HIV 1&2 At-Home Rapid Test Kit (99.7% accuracy) gives you results in minutes from home, no clinic, no waiting room, complete privacy. If you're in a situation where HIV exposure is a possibility alongside other STIs, the 7-in-1 Complete At-Home STD Test Kit covers HIV, genital herpes (HSV-2), chlamydia, gonorrhea, syphilis, hepatitis B, and hepatitis C in a single kit, because rashes and overlapping exposures are common enough that comprehensive testing makes more sense than testing one thing at a time. For the most complete picture, the Complete 8-in-1 Kit adds oral herpes (HSV-1) to the panel.
Testing is not a confession. It's not an overreaction. It's the only way to turn uncertainty into clarity, and clarity into action. Visit STD Rapid Test Kits to find the right test for your situation.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
3. CDC, HIV Diagnoses, Deaths, and Prevalence: 2025 Update
4. NIH HIVinfo, The Stages of HIV Infection
5. WebMD, HIV Rash: Types, Related Symptoms, and Treatment
6. Healthline, HIV Rash: Pictures, Treatment, and More
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.