Last updated: April 2026
For most of the past two decades, syphilis carried a specific mental image, a disease concentrated in particular communities, easy to dismiss if you didn't fit a certain profile. That image is now wrong. New data and peer-reviewed research published in 2025 show that syphilis is actively shifting into populations who have historically had low infection rates, while slowly declining among the groups who have long carried the heaviest burden. If you've never once considered getting a syphilis test because it "wasn't something that affected you," this article is specifically for you.
Syphilis is now spreading into populations with no traditional risk factors, people who aren't on PrEP, who don't identify with high-risk behaviors, and who have never had a reason to think about this infection. According to a 2025 study published in the American Journal of Preventive Medicine analyzing data from nearly 57 million US adults, syphilis incidence is rising in exactly these low-burden groups, even as it declines among populations who've historically accounted for the majority of cases. The infection doesn't know who you think you are. It only knows whether it has a route.
People are also reading: No Sore, Still Syphilis? How Early Symptoms Get Missed
How Syphilis Became Someone Else's Problem, And Why That's No Longer True
The story of syphilis in America over the past 25 years is one of the more striking public health reversals on record. By the late 1990s, the CDC had launched an aggressive national elimination plan, and it was working. Cases hit historic lows in 2000 and 2001, and elimination, genuinely getting rid of syphilis as a public health concern in the US, seemed within reach. Then it all reversed. Cases climbed steadily through the 2000s and 2010s, concentrated primarily among men who have sex with men, and the broader public largely stopped paying attention because the numbers didn't seem relevant to them.
That selective attention created a blind spot that is now costing people. According to provisional CDC data released in September 2025, there were more than 209,000 total syphilis cases reported in 2023, the highest number since the 1950s. Cases have tripled since 2010. The rate per 100,000 people represents a 30-fold increase since 2000 and 2001, when elimination efforts had nearly succeeded. The disease didn't just come back. It came back at a scale that erased decades of progress.
What makes the current moment different from any previous point in that rise is who is now being infected. For years, syphilis data told a consistent story: cases were concentrated among men who have sex with men, people living with HIV, and communities with limited access to sexual health services. Prevention efforts, testing programs, and public awareness were calibrated to those groups accordingly. What the 2025 data reveals is that this calibration is now leaving an entirely different population exposed, one that has no reason to think the calibration applies to them, which is precisely why they aren't testing.
What the 2025 Research Actually Found
The shift being described here is not anecdotal. It is documented in peer-reviewed research published in 2025, using one of the largest real-world electronic health record databases in the United States. The study, published in the American Journal of Preventive Medicine, tracked monthly syphilis incidence across nearly 57 million US adults from January 2017 through October 2024. The finding is precise and alarming: while overall syphilis incidence peaked in July 2022 and has since declined, that decline is happening almost entirely among high-burden populations. Among low-burden groups, people without behaviors historically associated with STI acquisition, people not using PrEP, and people not living with HIV, incidence is still rising.
Think about what that means in practice. The prevention tools driving the decline in high-risk groups, expanded PrEP programs that require quarterly STI testing, doxycycline post-exposure prophylaxis, and increased awareness in communities with higher baseline risk, are working for the people they were designed for. They are not reaching the people who never thought they needed them. Someone who has never considered themselves at risk for syphilis is not asking their doctor for a syphilis test. Their doctor is probably not offering one either. The infection moves through that gap silently.
A separate finding from the CDC's provisional 2024 data reinforces this. Early non-primary, non-secondary syphilis, which functions as a marker for recent infections that were not caught and diagnosed during the infectious stages, increased among women by nearly 8% in 2024, even as primary and secondary syphilis declined overall. That 8% rise is a signal that transmission in heterosexual networks is continuing to accelerate even while the headline numbers look like progress. The infections are happening. They're just not being found until later, when they're harder to detect, and more damage has already been done.
Check Your STD Status in Minutes
Test at Home with RemediumSyphilis Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $33.99 $49.00
Who Is "Low Risk", And Why That Label Is Doing Real Harm
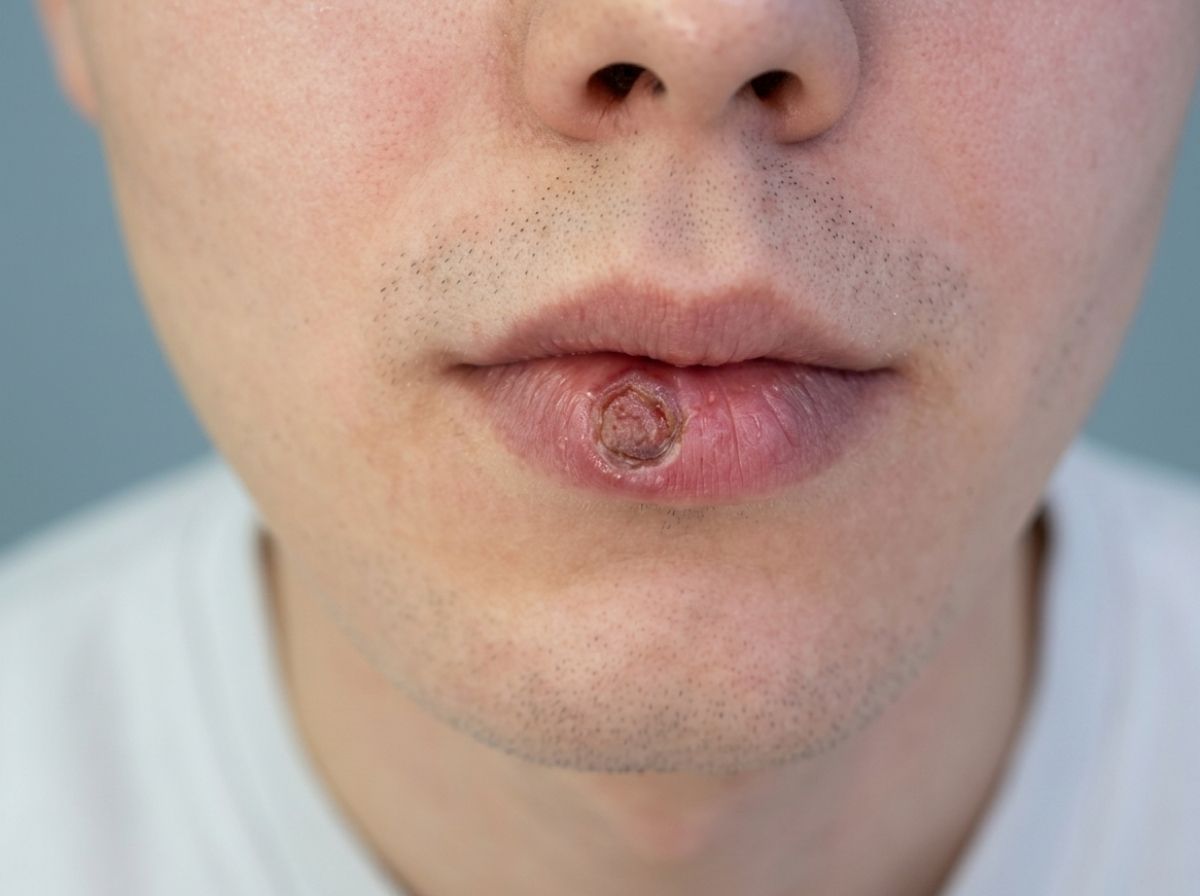
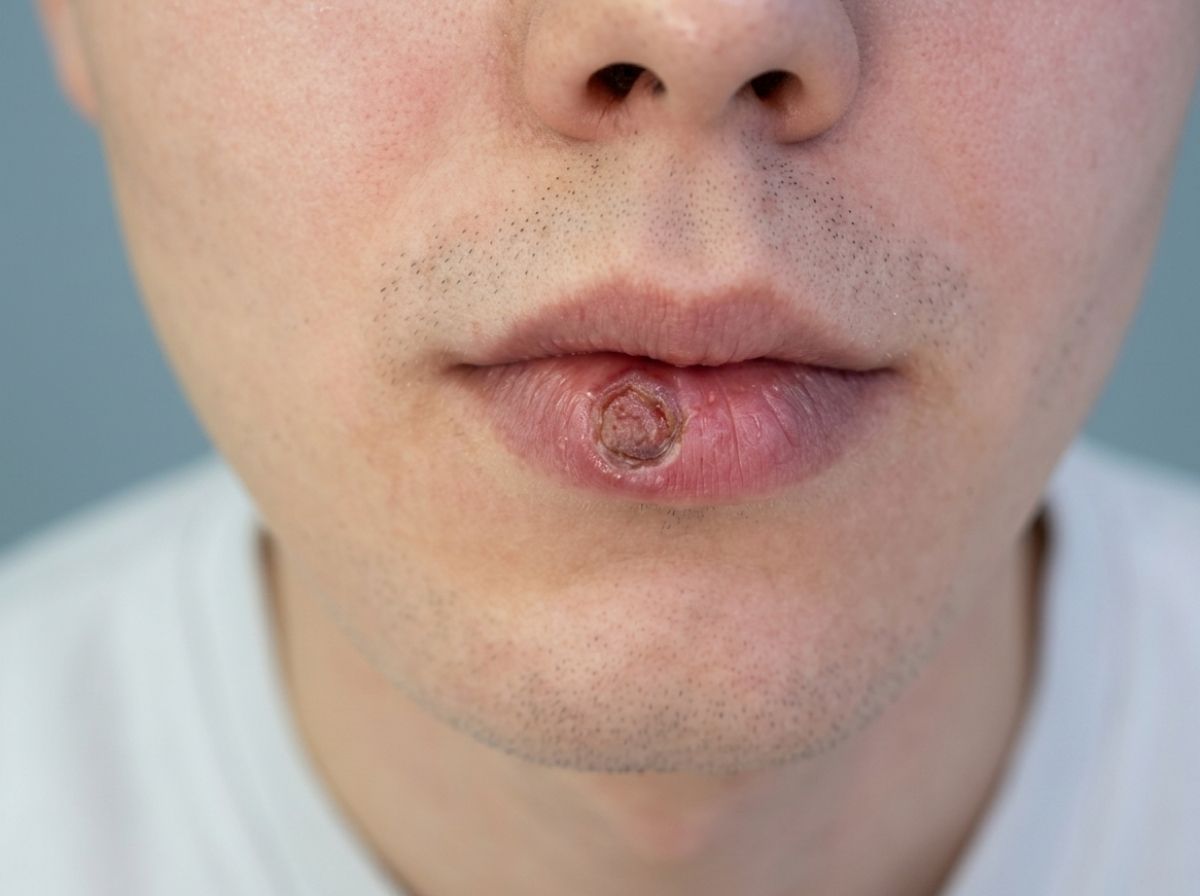
The concept of a "low-risk" population for syphilis has always been more about perception than biology. Treponema pallidum, the bacterium that causes syphilis, does not assess your identity, your relationship structure, your sexual orientation, or your self-image before deciding whether to infect you. It transmits through direct contact with a syphilis sore during sexual activity. Sores appear at the exact point where the bacteria entered the body, on the genitals, in the mouth, on the lips, or around the anus, and any sexual contact involving an active sore carries transmission risk, regardless of the type of sex.
The practical problem with "low risk" as a category is that it breeds a false sense of immunity that prevents testing. Someone who identifies as straight, is in a monogamous relationship, doesn't use drugs, and has never had an STI has every reason, by the old framework, to assume syphilis simply isn't something they need to think about. But that person's sexual history includes their partners' histories, and those histories include other partners, other risks, and other exposure windows they may know nothing about. A single undetected infection in one link of a sexual network can travel silently through multiple people before anyone gets a diagnosis.
The stigma attached to syphilis makes this worse. Because the disease has historically been associated with specific communities and behaviors, a diagnosis can feel like an accusation rather than a straightforward health event. That association discourages testing even when someone has reason to suspect an exposure, and it discourages honest disclosure between partners. The result is a disease that spreads most effectively through exactly the population that is least prepared to encounter it, people who never went looking for it because they never thought they had to.
What Syphilis Actually Looks Like, And Why It Gets Missed
You're in the shower a few weeks after a sexual encounter, and you notice a sore, small, firm, painless. Not angry-looking, not oozing, not particularly alarming. Easy to write off as a razor bump, an ingrown hair, a friction irritation. You wait a few days. It disappears on its own. You move on. That is the most common first experience of primary syphilis, and the reason it gets missed so consistently is that it doesn't look or feel like most people's idea of an STI. The painlessness is the tell, and it's also the reason people don't act on it.
Syphilis progresses through four distinct stages, each with different characteristics and different levels of transmission risk. Primary syphilis presents as one or more painless sores called chancres, appearing at the exact site where the bacteria entered the body. Because they're painless and located where they're not visible, inside the vagina, on the cervix, in the mouth, or in the anorectal area, they go unnoticed entirely in a significant proportion of cases. The chancre appears between 10 and 90 days after exposure and resolves without treatment within 3 to 6 weeks. That resolution feels like recovery. It is not.
If untreated, syphilis moves into the secondary stage, typically 2 to 8 weeks after the initial sore appears. This stage is characterized by a rash, often described as rough, reddish-brown spots on the palms of the hands or soles of the feet, though it can appear anywhere on the body. The secondary stage can also produce flu-like symptoms, swollen lymph nodes, and sores in the mouth or genitals. It is the most infectious stage of the disease. At this point, Treponema pallidum has disseminated through the bloodstream and is present in the mucous membrane lesions and skin rashes themselves, meaning skin-to-skin or mucous membrane contact with those lesions during sex is a direct transmission route. After secondary syphilis, the infection enters a latent stage where no symptoms are present, but the bacteria remain in the body. Untreated latent syphilis can persist for years before progressing to tertiary syphilis, where the infection begins damaging the heart, brain, eyes, and nervous system in ways that can be permanent.
| Stage | Timing | Key Signs | Transmission Risk |
|---|---|---|---|
| Primary | 10–90 days after exposure | Painless sore (chancre) at site of infection; heals within 3–6 weeks without treatment | High, direct contact with sore |
| Secondary | 2–8 weeks after the primary sore appears | Rash on palms/soles, flu-like symptoms, mouth or genital sores | Highest, most infectious stage |
| Latent | After secondary; can last years | No symptoms, infection is silent but present | Lower but not zero |
| Tertiary | Years after untreated latent infection | Damage to heart, brain, eyes, nervous system; can cause blindness, paralysis, death | Not directly transmissible at this stage |
The practical takeaway from this progression is that syphilis is most detectable, through symptoms, at the stages when it's easiest to dismiss or overlook, and most dangerous at the stage when it produces no symptoms at all. Testing is the only way to catch it during the latent period, when treatment is still straightforward and effective. Waiting for symptoms that feel obviously like an STI means waiting past the window when catching it is simplest.
People are also reading: The Michigan Syphilis Cluster That Left 5 Women With Serious Eye Infections
Testing: The Only Way Out of the Guessing Game
The reason testing matters so much for the shift happening right now is not just personal, it's structural. The decline in syphilis among high-risk populations is partly attributable to more frequent, routine testing built into existing programs like PrEP. People on PrEP are tested for STIs every 3 months as a condition of their care. That regular cadence catches infections early, before they progress and before they spread further. The low-burden populations now seeing rising rates do not have that built-in testing cadence. They test when they have a symptom. With syphilis, the primary sore is painless and self-resolving, so that symptom-triggered approach means testing happens in the latent stage at the earliest, or not at all.
If you've had unprotected sexual contact, oral, vaginal, or anal, with a new partner in the past year and you haven't had a syphilis test, that is a gap worth closing. Testing for syphilis works by detecting antibodies your immune system produces in response to Treponema pallidum. The key timing point: test from 6 weeks after potential exposure. Testing before 6 weeks risks a false negative because your immune system hasn't yet produced detectable antibody levels, not because the infection isn't there, but because the test has nothing to measure yet. A negative result at 6 weeks is meaningful, but if you have ongoing concern about a specific exposure, a follow-up test at 12 weeks provides additional certainty.
A positive syphilis test result does not mean a health crisis; it means a curable infection that has been caught. Syphilis is one of the most treatable STIs that exists, provided it's found before it reaches the tertiary stage. A positive result is the beginning of a straightforward medical conversation, not a verdict. What matters is that the conversation happens. The Syphilis At-Home Rapid Test Kit from STD Rapid Test Kits gives you a 99.4% accurate result in about 20 minutes, using a simple finger-prick blood sample, with no clinic visit, no waiting room, and no audience. Testing at home removes every logistical reason not to know.
For anyone who wants broader coverage, syphilis co-occurs with chlamydia and gonorrhea at documented rates in surveillance data, and the CDC recommends testing for all three together when any one is suspected. The Chlamydia, Gonorrhea & Syphilis 3-in-1 At-Home Rapid Test Kit screens for all three of the most common bacterial STIs in a single session. Chlamydia can be tested from 14 days after exposure, gonorrhea from 3 weeks after exposure, and syphilis from 6 weeks, so timing your test at the 6-week mark covers all three accurately in one go. If you want the most complete picture available, the 7-in-1 Complete At-Home STD Test Kit adds HIV, HSV-2, Hepatitis B, and Hepatitis C to that panel. One test session. Comprehensive results. Take control of your sexual health today.
The Congenital Syphilis Crisis, And What It Reveals About the Testing Gap
The most devastating consequence of the shift in syphilis transmission is playing out in newborns. Congenital syphilis, an infection transmitted from a pregnant person to their baby during pregnancy or childbirth, has risen for 12 consecutive years in the United States. Provisional CDC data from September 2025 reported nearly 4,000 cases in 2024, representing a 700% increase since 2015, when just 495 cases were on record. These are babies born with a bacterial infection that causes bone damage, neurological problems, blindness, deafness, and death. Every one of those cases is preventable with a timely test and appropriate treatment.
The reason congenital syphilis keeps rising even as adult cases begin to plateau is the testing gap among heterosexual women, precisely the low-burden population that the current shift is now affecting most acutely. A pregnant person who doesn't know they have syphilis can't be treated for it. A person who doesn't think syphilis is something they need to test for doesn't get tested during prenatal care as thoroughly as they should. The CDC data showing that early non-primary, non-secondary syphilis rose nearly 8% among women in 2024 is not just a statistic; it is a direct predictor of how many more babies will be born with congenital syphilis in the coming year.
New York State's Department of Health issued an urgent public advisory in August 2025 after six infants died from congenital syphilis in counties outside New York City in 2024, with a third death reported in 2025 before the year was half over. Mississippi has seen a 1,000% increase in congenital syphilis over six years. South Dakota leads the nation in congenital syphilis rates. These are not statistics from communities that historically appeared in syphilis surveillance data. They are the direct result of an infection spreading into populations who weren't looking for it, and a testing system that wasn't looking for it either.
Check Your STD Status in Minutes
Test at Home with RemediumSyphilis Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $33.99 $49.00
Why the Old Risk Profile No Longer Protects You
The factors driving syphilis into low-burden populations are not mysterious. Dating apps and digital platforms have created new sexual networks that operate faster and with fewer points of contact than previous generations of sexual behavior. Someone can have a sexual encounter with a person whose full sexual history is unknown, in a context that doesn't trigger any of the traditional mental flags for STI risk, and walk away with an infection that will take 6 weeks or more to appear on a test and potentially years to produce symptoms. The network dynamics of how infections spread don't require high-frequency sexual activity or multiple concurrent partners. They require opportunity and a gap in testing.
Declining condom use is another documented driver. Research published in 2025 reviewing global syphilis trends identified declining condom use as a consistent factor in resurgence across the United States, the United Kingdom, Canada, and other high-income countries. Condoms reduce syphilis transmission risk but do not eliminate it entirely, sores can be present in areas not covered by a condom, but their reduced use in low-risk-identified populations removes even that partial protection. The combination of expanded sexual networks, reduced condom use, and near-zero baseline testing in populations who don't perceive themselves as at risk creates precisely the conditions the current data is documenting.
There is also the matter of what happens when testing infrastructure erodes. In recent years, states have lost STI prevention funding, health departments have faced staffing cuts, and the public health systems designed to catch and interrupt syphilis transmission have operated under increasing strain. The 2025 research on congenital syphilis noted an ongoing shortage of the primary treatment used for pregnant individuals and infants, creating additional complications for cases that are caught. Prevention infrastructure matters at a population level even for individuals who consider themselves low risk, when the system designed to catch infections early is under-resourced, infections travel further before they're found.
What Routine Testing Actually Looks Like, And Why It's Easier Than You Think
The gap between knowing you should probably test and actually testing is almost always logistical and emotional rather than informational. People know, abstractly, that sexual health testing is a responsible habit. What stops them is the friction, making an appointment, sitting in a waiting room, having a conversation with a provider that feels uncomfortable, waiting days for results, and doing all of that on a calendar that already feels full. At-home rapid testing eliminates most of that friction.
A practical routine for someone who is sexually active with new or multiple partners looks like this: test for syphilis and other bacterial STIs at the 6-week mark after any new sexual contact with an untested partner. The Syphilis At-Home Rapid Test Kit takes about 20 minutes from finger prick to result, ships discreetly, and doesn't require anyone to know you've tested except you. The result is either a clean negative, which tells you something useful and specific, or a positive, which tells you something even more useful and gets you into treatment that resolves the infection completely.
For anyone who is pregnant or planning to become pregnant, a syphilis test is not optional; it is essential, regardless of perceived risk level. The congenital syphilis data make clear that the old assumption that "someone like me doesn't need to worry about syphilis" is exactly how nearly 4,000 babies a year are being born with a preventable infection. Prenatal testing recommendations from the CDC call for syphilis screening at the first prenatal visit, again in the third trimester, and again at delivery for those in high-prevalence areas. Testing at home before or during early pregnancy gives you information and time to act on it before complications develop.
| Infection | Test From | Negative Result Means | Positive Result Means |
|---|---|---|---|
| Syphilis | 6 weeks after exposure | No syphilis detected from that exposure, retest at 12 weeks if ongoing concern | Infection is present, curable with prompt treatment |
| Chlamydia | 14 days after exposure | No chlamydia detected; retest if new exposure occurs | Bacterial infection present, treatable with antibiotics |
| Gonorrhea | 3 weeks after exposure | No gonorrhea detected from that exposure | Infection present, requires prompt treatment |
| HIV | 6 weeks (first indicator); retest at 12 weeks for certainty | Negative at 12 weeks = did not contract HIV from that exposure | Virus is present, connect with a healthcare provider immediately |
| Herpes HSV-1 & HSV-2 | 6 weeks after exposure | No herpes antibodies detected from that exposure, note that HSV-1 is extremely common and a negative result does not rule out pre-existing oral herpes | Antibodies detected, indicates current or past infection; connect with a healthcare provider to discuss management |
| Hepatitis B | 6 weeks after exposure | No infection detected; reliable given shorter incubation period | Active infection, requires medical follow-up |
| Hepatitis C | 8–11 weeks after exposure | Conclusive after 11 weeks | Infection present, now curable in most cases |
FAQs
1. I'm not in a high-risk group; do I really need to worry about syphilis?
Yes, and the 2025 research is specific about this. A study of nearly 57 million US adults found that syphilis incidence is rising in populations without traditional risk factors while declining in high-burden groups. The old risk profile no longer accurately predicts who is getting infected.
2. How is syphilis transmitted?
Syphilis spreads through direct contact with a syphilis sore during sexual activity, oral, vaginal, or anal sex. Sores can appear on the genitals, in the mouth, on the lips, around the anus, or on the fingers. Transmission requires contact with an active sore; it does not spread through casual contact, shared surfaces, or air.
3. What does a syphilis sore actually look like?
The primary stage sore, called a chancre, is typically small, firm, and painless, easy to mistake for a razor bump, ingrown hair, or minor irritation. It appears at the site of infection between 10 and 90 days after exposure and heals on its own within 3 to 6 weeks, even without treatment. That healing does not mean the infection is gone.
4. Can you have syphilis with no symptoms at all?
Yes. After the primary and secondary stages, syphilis enters a latent phase with no symptoms, during which the bacteria remain in the body and can continue causing internal damage. Latent syphilis can persist for years without any external signs. Testing is the only way to detect it during this stage.
5. When should I test for syphilis after a potential exposure?
Test from 6 weeks after potential exposure. Testing before 6 weeks risks a false negative because your immune system hasn't yet produced detectable antibody levels. A negative at 6 weeks is reliable; if you have ongoing concern about a specific exposure, a follow-up test at 12 weeks provides additional certainty.
6. Is syphilis curable?
Yes, completely, when caught before it reaches the tertiary stage. Effective treatment is available and works across primary, secondary, and latent stages. A positive result is not a health crisis; it is a curable infection that has been found. The earlier it is caught, the simpler the treatment and the less damage occurs.
7. What happens if syphilis goes untreated?
Untreated syphilis progresses from the painless primary stage through an infectious secondary stage with rash and flu-like symptoms, then into a silent latent phase. Tertiary syphilis, which can develop years after initial infection, damages the heart, brain, eyes, and nervous system, and can cause blindness, deafness, paralysis, and death. These outcomes are entirely preventable with timely testing and treatment.
8. Can syphilis affect a pregnancy?
Yes, and seriously. Syphilis can be transmitted from a pregnant person to their baby during pregnancy or childbirth, which is congenital syphilis. It causes bone damage, neurological problems, blindness, deafness, stillbirth, and infant death. Congenital syphilis has risen for 12 consecutive years in the US, with nearly 4,000 cases in 2024. Testing during pregnancy is essential regardless of perceived risk.
9. Can you get syphilis from oral sex?
Yes. Syphilis sores can appear in the mouth and on the lips, and transmission through oral sex is documented. Any sexual contact involving an active sore, regardless of the type of sex, carries transmission risk. This is one of the reasons syphilis spreads more broadly than people expect.
10. How often should I test for syphilis if I'm sexually active?
At minimum, test once a year if you are sexually active with new or multiple partners. If you have had unprotected sexual contact with someone whose STI status is unknown, test from 6 weeks after that exposure. People who are pregnant should test at their first prenatal visit, again in the third trimester, and at delivery if they are in a high-prevalence area.
The Test Is Simpler Than the Diagnosis You're Avoiding
The data is clear, and it points in one direction: syphilis is no longer a disease that belongs to someone else's risk profile. It is spreading into populations that have spent years, reasonably, based on outdated information, assuming they didn't need to think about it. That assumption is now the primary driver of undetected infections, rising congenital syphilis cases, and a transmission chain that continues precisely because the people in it aren't testing. The solution is not complicated. It is a test.
If you have been sexually active with a new partner in the past year and haven't tested, the Syphilis At-Home Rapid Test Kit gives you a 99.4% accurate answer at the 6-week mark, privately, in about 20 minutes. For broader coverage in a single session, the Chlamydia, Gonorrhea & Syphilis 3-in-1 At-Home Rapid Test Kit screens for the three most common curable bacterial STIs at once, time your test at 6 weeks post-exposure and all three are covered accurately. For women who want the most comprehensive panel available, the Women's 10-in-1 At-Home STD Test Kit covers syphilis alongside nine other infections, including HPV and Trichomoniasis. Your results, your privacy, your power.
You can browse the full range of at-home rapid test kits at STD Rapid Test Kits.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC, Latest National Data on Syphilis in Newborns and STIs, September 2025
4. Healthbeat, Are STDs Truly Declining, or Is the Data Just Lacking? (2025)
5. NCBI, Advances in Syphilis Diagnostics to Address the 21st-Century Epidemic (2025)
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.