Last updated: April 2026
Not every bump on your face is acne, but not every bump is an STD either. If you are staring at your skin and mentally zooming in like it owes you an explanation, this guide will help you sort out what is more likely, what facial STD symptoms can actually look like, and when testing makes sense.
A facial breakout can trigger a very specific kind of panic. You notice a red bump near your mouth, along your cheek, or on your chin, and your brain skips right past ordinary explanations and lands on herpes, syphilis, or some mystery infection you wish you had never Googled. That reaction is common because facial skin is visible, emotionally loaded, and easy to overread.
Here is the direct answer: most facial bumps are acne, irritation, or another non-STD skin issue. A true STD-related facial rash is less common and usually comes with a different pattern, different timing, or different sensations than standard acne. The fastest way to stop guessing is to compare the details carefully and test when the exposure history and symptom pattern actually line up.

People are also reading: HPV in the Throat, Genitals, or Nowhere: What You Need to Know
Why Facial Bumps Cause So Much STD Anxiety
You are in the bathroom mirror, leaning closer than you probably should, trying to decide whether the bump you found is just a clogged pore or something that started after a sexual encounter. That moment is exactly why this topic matters. Facial symptoms create instant anxiety because they are visible, hard to ignore, and easy to connect to oral sex, kissing, or skin-to-skin contact.
What makes this confusing is that the face is a crowded neighborhood in skin terms. Oil glands are active there, pores clog easily, shaving or waxing can irritate the surface, cosmetic products can trigger inflammation, and viruses like herpes can also affect the area around the mouth. So when a bump shows up, the question is not just “what does it look like?” but also “how did it start, how fast did it change, and what does it feel like?” Those details matter a lot more than one blurry glance.
The internet does not help. Search results and image galleries love dramatic examples, and dramatic examples are rarely the average case. A single pimple gets interpreted as herpes. A patch of dry irritation gets interpreted as syphilis. A healing cold sore gets interpreted as cystic acne. Real talk: half the fear here comes from the fact that several skin problems can look similar in a static photo, but they behave differently over time. Skin tells its story through pattern and timing, not just appearance.
Acne usually begins inside a clogged pore. An STD-related facial lesion, when it happens, is more likely to involve a specific exposure route and a different biological process. Herpes, for example, infects skin and nerve endings, which is why people can feel tingling, burning, or tenderness before visible blisters appear. Acne does not work that way. Acne is driven by oil, dead skin, inflammation, and bacterial overgrowth inside the follicle. That difference in mechanism creates a difference in texture, pain pattern, and progression.
That is also why panic-testing the day after exposure usually creates more confusion, not less. Biology does not care that you are worried on a Tuesday night. Infections need time to replicate to detectable levels, and acne does not follow STD testing windows at all. So before jumping to conclusions, it helps to understand what acne actually does on facial skin and why it is still the most common explanation for new bumps around the face.
What Acne Actually Looks Like on the Face
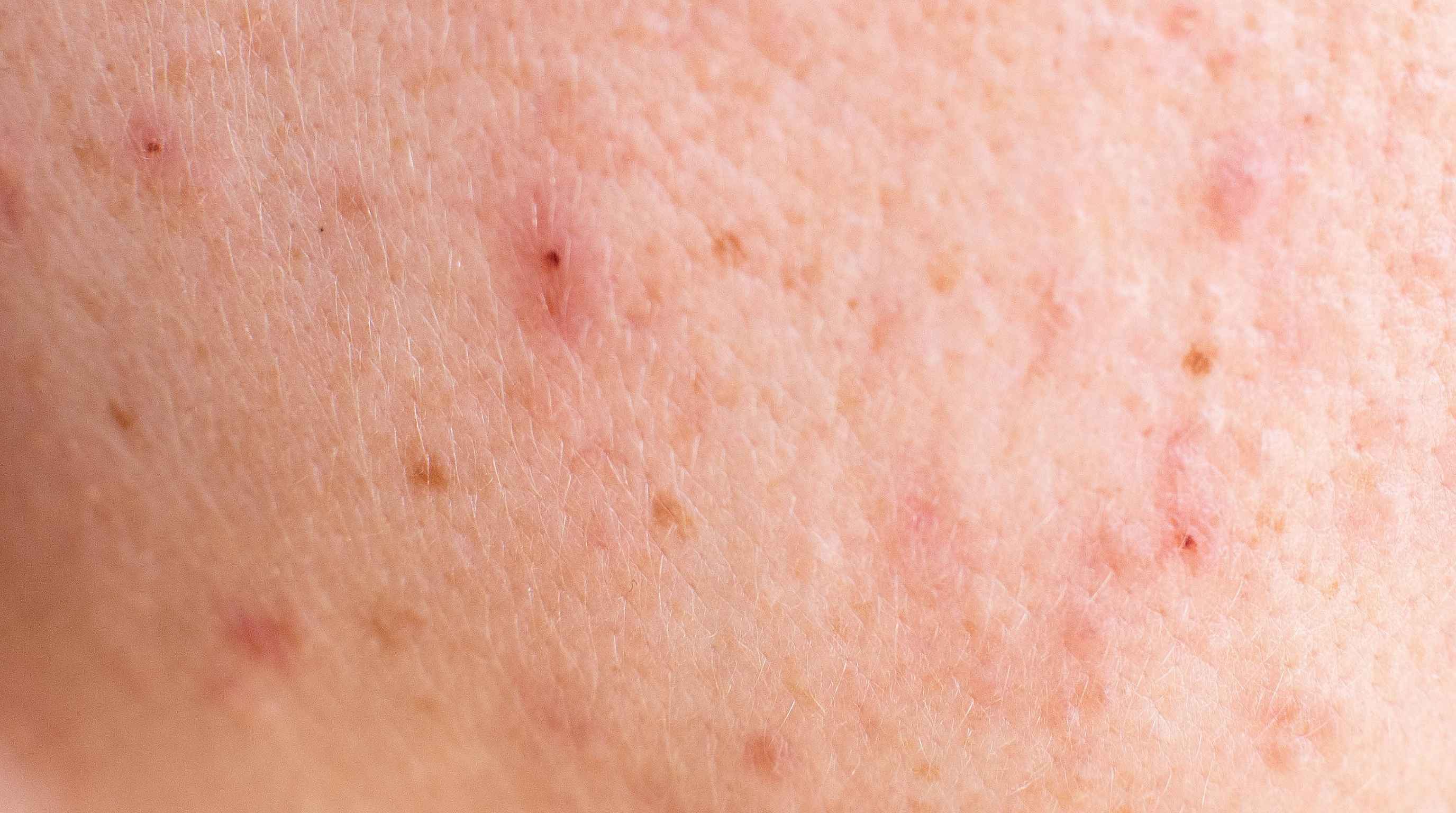
Acne forms when a hair follicle and its oil gland get blocked by sebum and dead skin cells. Once that plug forms, the pore can stay closed and become a whitehead, remain open and darken into a blackhead, or become inflamed and turn into a red, swollen bump. If bacteria inside the clogged follicle multiply and the immune system responds, the area can become more tender, more raised, and more obvious. That is why acne often looks angry without being dangerous.
On the face, acne tends to follow oil-rich zones. The forehead, nose, chin, jawline, and cheeks are classic locations because sebaceous glands are more active there. If you get repeated bumps in those same general areas, especially in clusters, that pattern leans much more toward acne than an STD rash. Acne also tends to come with company. One bump might show up first, but it is common to see nearby clogged pores, blackheads, tiny flesh-colored bumps, or older healing spots in the same region.
The texture of acne is another clue. A pimple usually feels like a defined bump under or on the skin. It can be sore when pressed, but it does not usually begin with tingling or burning before you see anything. It also does not usually turn into grouped clear-fluid blisters. If a bump comes to a white or yellow head over a day or two, that points more toward inflammation inside a follicle than a viral lesion on the skin surface.
Timing matters here too. Acne can build gradually over several days because the pore has to clog, swell, and inflame. Hormonal shifts, stress, sweating, makeup, beard products, sunscreen, friction from masks, and shaving all make that process more likely. You may not notice the earliest stage, then suddenly spot the breakout once it becomes raised and red. That can make acne feel “sudden,” even when the biology has been building quietly for longer than you realized.
Facial acne also tends to repeat familiar patterns. Someone who breaks out around the chin after stress, around the mouth after occlusive lip products, or along the beard line after shaving is dealing with a skin behavior pattern, not a random one-off mystery. That history matters. If your skin has done versions of this before, the odds shift further toward acne, irritation, or folliculitis rather than an STD.
One more thing people miss: acne does not need sexual contact to explain itself. It needs pores, oil, inflammation, and the right trigger. So if you notice a bump and your only reason for suspecting an STD is “I had sex recently,” that alone is not enough to make the bump suspicious. The face breaks out for boring reasons all the time. The job here is not to dismiss STD risk completely. It is to stop letting timing alone outrank the actual symptom pattern.
| Feature | What It Usually Suggests |
|---|---|
| Whitehead, blackhead, or red inflamed bump | Blocked pore with inflammation, which fits acne more than an STD lesion |
| Several bumps in the same oily area | Pattern consistent with acne-prone skin rather than a single exposure-related lesion |
| Jawline, chin, cheeks, forehead, or beard area | Classic acne distribution because these areas have active oil glands |
| Bump becomes pustular over 1 to 3 days | Typical follicle inflammation pattern seen with acne |
| No tingling before the bump appeared | Leans away from herpes, which more often has a nerve-related warning sensation |
That said, acne can absolutely be mistaken for something infectious when it shows up near the lips or when it becomes raw from picking, shaving, or friction. Around the mouth, things get trickier because cold sores, irritation, angular cheilitis, ingrown hairs, and perioral dermatitis can all enter the conversation. This is where people start searching things like “pimple vs herpes face” or “cold sore vs acne around mouth” at 2 AM and making themselves miserable.
The main point for now is simple: acne usually looks and behaves like a pore problem. It sits in acne-prone zones, often appears in multiples, and follows an inflammation pattern rather than a blistering pattern. If your bump fits that description, acne is the more likely explanation. In Part 2, we will get into what STD-related facial symptoms can actually look like, especially herpes, and how the side-by-side differences become much clearer once you know what to watch for.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
What an STD Rash on the Face Can Actually Look Like
Now let’s talk about the part that triggers most of the anxiety: what if it is an STD? The reality is that very few STDs regularly show up on the face, and when they do, they usually follow specific biological patterns. The main one people worry about is herpes (HSV-1 or HSV-2), because it can be transmitted through oral contact and can affect the lips, surrounding skin, or nearby facial areas.
Herpes behaves very differently from acne because it is a virus that lives in nerve cells. Before anything visible appears, the virus can reactivate along a nerve pathway, which is why people often feel a tingling, itching, or burning sensation in a very specific spot. That sensation typically shows up first, followed by small fluid-filled blisters that cluster together. Acne does not cluster into clear blisters like that, and it does not start with nerve-related tingling.
Those herpes blisters usually evolve quickly. Within 24 to 72 hours, they can break open, release fluid, and then crust over into a scab before healing. This progression is one of the biggest clues. Acne tends to swell, form a head, and slowly resolve. Herpes moves through stages: sensation, blister, rupture, crust, healing. If what you are seeing follows that pattern, it leans strongly away from acne.
Another difference is location behavior. Herpes around the face most often appears on or around the lips, sometimes called cold sores. It can extend slightly beyond the lip border but usually stays localized to one area during an outbreak. Acne, on the other hand, tends to appear across broader zones like the cheeks, chin, or forehead, often with multiple unrelated bumps at once.
There are other STDs that people worry about, but they are far less likely to show up as facial “pimples.” Syphilis can cause a rash, but it typically appears on the palms of the hands and soles of the feet during its secondary stage, not as isolated facial bumps. HPV can cause warts, but facial involvement is uncommon and looks more like raised, rough growths rather than inflamed pimples or blisters. The key takeaway is that herpes is the primary STD that realistically overlaps with acne in appearance on the face.
One of the most misleading situations is when a cold sore is in its early stage or healing stage. Early on, it might look like a small red bump before blisters fully form. Later, when it crusts, it can resemble a dry, irritated pimple. This is where people mislabel herpes as acne or vice versa. The timeline is what separates them. If it changed rapidly over a couple of days and involved blistering or crusting, that is not typical acne behavior.
| Feature | Acne | Herpes (STD-related) |
|---|---|---|
| Cause | Clogged pores, oil, bacteria | Viral infection affecting nerves and skin |
| Early sensation | No warning sensation | Tingling, burning, or itching before visible lesions |
| Appearance | Single bumps, whiteheads, or inflamed pimples | Clusters of small fluid-filled blisters |
| Progression | Gradual swelling → possible pus → healing | Blister → rupture → crust → healing within days |
| Distribution | Multiple areas (cheeks, chin, forehead) | Localized to one area, often lips or nearby skin |
| Pain type | Tender when pressed | Burning or stinging even without pressure |
Recurrence is another important factor. Hormones or skin care can make acne come and go, but herpes tends to come back in the same spot because the virus lives in the nerve next to it. If someone sees that the same spot keeps getting worse with the same symptoms, that pattern is more likely to be herpes than acne.
At this point, you might be thinking: what if I had oral sex recently and now there is a bump on my face? That connection is what drives most of the confusion. Timing matters here, but not in the way people expect. Symptoms from herpes do not reliably appear the next day. There is usually an incubation period before visible signs develop, which we will break down clearly in the next section.
Acne vs STD Rash, Why Timing and Behavior Matter More Than Appearance
This is where people either calm down or spiral further, depending on how they interpret timing. You have a sexual encounter, and then within a day or two, you notice something on your face. The instinct is to connect the two immediately. But biologically, most infections do not show up that fast in a visible way.
Herpes has an incubation period that typically ranges from 2 to 12 days after exposure before symptoms appear. That means a bump showing up the very next day is far more likely to be unrelated acne or irritation rather than a new herpes infection. This timing gap is one of the most important reality checks because it breaks the automatic “I had sex → I have a bump → it must be an STD” chain of thinking.
Acne, on the other hand, does not follow exposure timelines. It follows skin conditions. A pore can clog due to sweat, oil buildup, friction, or products, and the visible bump may appear shortly after. That is why acne often feels random or badly timed. It shows up when the skin environment allows it, not when your sexual activity timeline says it should.
Behavior over time is another strong differentiator. If a bump stays relatively stable, maybe gets a whitehead, and then slowly fades over several days, that is classic acne behavior. If it rapidly evolves, forms blisters, breaks open, and crusts, that pattern is not acne. Watching what happens over 48 to 72 hours often gives more clarity than trying to diagnose it in the first 10 minutes of noticing it.
There is also the question of spread. Acne can appear in multiple new spots over time because multiple pores can clog independently. Herpes tends to stay localized during an outbreak. It may look like several small lesions, but they are usually grouped in one area rather than scattered across different parts of the face.
This is why guessing based on a single snapshot is unreliable. Skin conditions are dynamic. The timeline, sensation, and evolution of the bump tell you more than its initial appearance. And when those signals are still unclear, that is where testing comes in, not as a panic reaction, but as a way to get a definitive answer based on biology rather than assumptions.
People are also reading: Casual Sex, Real Risk: Why STDs Slip Through in FWB Setups
When to Test (And Which Test Actually Gives You a Clear Answer)
This is the part most people skip or rush, and it is exactly where clarity comes from. If you are stuck between “this is probably acne” and “what if it is an STD,” testing is what ends the guessing. But the timing of your test matters a lot more than most people realize. Testing too early can give you a false negative, which feels reassuring but is not actually reliable.
Different infections require different types of tests because they behave differently in the body. Bacterial infections like chlamydia and gonorrhea are detected using NAAT (nucleic acid amplification tests), which look for the genetic material of the bacteria. Viral infections like HIV, herpes, and hepatitis are typically detected through blood tests that measure antibodies or viral markers produced by your immune system.
If your concern is a facial bump, herpes is usually the main STD in question. That means a blood test is often the appropriate route unless there is an active blister that can be swabbed. But most people are not testing a perfect fresh blister. They are testing uncertainty. That is where timing becomes everything.
Here are the exact testing windows you need to follow:
- Chlamydia: test from 14 days after exposure
- Gonorrhea: test from 3 weeks after exposure
- Syphilis: test from 6 weeks after exposure
- HIV: test at 6 weeks for first indicator, retest at 12 weeks for certainty
- Herpes HSV-1 and HSV-2: test from 6 weeks after exposure
- Hepatitis B: test from 6 weeks after exposure
- Hepatitis C: test from 8–11 weeks after exposure
These timelines exist because your body needs time to either build enough of the infection (for NAAT tests) or produce detectable antibodies (for blood tests). If you test before these windows, the infection can still be present but invisible to the test. That is what creates false reassurance.
If you are in that in-between stage, symptoms unclear, timing uncertain, a comprehensive option is to use a combo STD test kit. This allows you to check multiple infections at once from home, giving you a clearer overall picture rather than chasing one possibility at a time.
Now let’s break down what your result actually means, because that is where a lot of confusion continues even after testing.
If your result is negative: This means no infection was detected at the time of testing. If you tested within the correct window period, that is strong reassurance. If you tested too early, however, the result may not be reliable yet, and retesting at the correct time is necessary to confirm.
If your result is positive: This means the infection is present and confirmed. At that point, the next step is straightforward: follow up with a healthcare provider for confirmation and management. The important shift here is that you are no longer guessing. You are working with a defined answer.
When should you retest? If your initial test was done before the full window period, or if you continue to notice symptoms that do not match acne patterns, retesting after the appropriate timeframe is necessary. This is not overreacting. It is aligning with how infection biology works.
Testing is not about assuming the worst. It is about removing uncertainty. If your bump behaves like acne, you may not need to test immediately. But if the timing, sensation, or progression does not fit acne clearly, testing is the fastest way to stop second-guessing your own skin.
Timing Reality Check: Why Your Brain Connects Things That Are Not Actually Connected
One of the most common patterns goes like this: you have a sexual encounter, and within a day or two, you notice something on your face. Your brain links those two events instantly. It feels logical. But biologically, that connection often does not hold up.
Most STDs, like herpes, have a time when they can be spread. That means that symptoms don't show up right away after exposure. That wait is usually between 2 and 12 days for herpes. If you wake up the next morning with a bump, it is almost certainly not because of that recent encounter. It's more likely that it was something that was already happening, like acne or irritation.
This mismatch between emotional timing and biological timing is what fuels a lot of unnecessary anxiety. Your brain wants a clear cause-and-effect story. Your body does not operate on that schedule. Skin conditions, especially acne, can surface quickly once inflammation reaches a visible level, even if the process started earlier.
There is also something called attention bias. Once you are worried, you start scanning your face more closely than usual. You notice bumps that might have been there already or that you would normally ignore. That does not mean you are imagining things. It means you are paying closer attention, and everything feels more significant.
The key here is to separate coincidence from causation. Just because two things happen close together does not mean one caused the other. When you apply the correct timelines and symptom patterns, the picture becomes much clearer and a lot less alarming.
Check Your STD Status in Minutes
Test at Home with Remedium6-in-1 STD Rapid Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $119.00 $294.00
For all 6 tests
What to Do Next If You’re Still Not Sure
If you are standing in front of the mirror still unsure, here is the grounded approach. First, look at the behavior of the bump over 48 to 72 hours. Does it act like acne, slowly forming and possibly developing a head? Or does it change rapidly, blister, or crust in a way that does not fit a clogged pore?
Second, think about sensation. Acne is usually tender when pressed. Herpes is more likely to feel like burning, tingling, or stinging even before anything visible appears. That difference comes from the underlying biology, surface inflammation versus nerve involvement.
Third, consider your history. If your skin has done this before in similar areas, acne becomes the more likely explanation. If something feels completely new, behaves differently, and aligns with a realistic exposure window, then testing becomes the smart next step.
And here is the honest truth most people do not hear enough: guessing rarely leads to peace of mind. You either convince yourself it is nothing and keep checking, or convince yourself it is serious and spiral. Testing cuts through that loop. It gives you a clear answer based on evidence, not interpretation.
If you are on the fence, a discreet at-home option like a rapid STD test kit can give you clarity without needing to navigate appointments or awkward conversations. It is not about assuming something is wrong. It is about getting a definitive answer so you can move on, either way.
Final Reality Check: Most Facial Bumps Are Not STDs
By this point, you have probably realized something important: the overlap between acne and STD-related facial symptoms exists, but it is not equal. Acne is extremely common. Facial STD symptoms are relatively uncommon and usually follow very specific patterns when they do occur.
That does not mean you should ignore something that feels off. It means you should evaluate it based on how it behaves, not just how it looks in a single moment. Skin tells a story over time. Acne builds, inflames, and resolves. Herpes signals, blisters, and heals in a different rhythm. Those patterns are your best guide.
If your bump fits acne patterns, it is likely just that. If it does not, or if your anxiety is not settling, testing gives you clarity. Either way, you are not stuck guessing. You have a way forward.
And that is really the goal here. Not to panic, not to dismiss, but to understand what your skin is actually telling you and respond with clarity instead of fear.
FAQs
1. Can acne really look like an STD on the face?
Honestly, yes, and that’s why so many people end up here. A red, irritated pimple near your mouth can look way more dramatic than it actually is. The key difference isn’t just how it looks in one moment, but how it behaves. Acne hangs out, swells, maybe forms a head. STD-related bumps, especially herpes, tend to change fast, blistering, breaking, crusting. It’s the timeline that tells the truth.
2. How do I actually tell a cold sore from a pimple without guessing?
Think about what you felt before you saw anything. Cold sores usually announce themselves with tingling or burning, like your skin is warning you. Pimples don’t do that. They just show up uninvited. Then watch what happens next. If it turns into tiny fluid-filled blisters, that’s not acne. If it builds into a single inflamed bump, it probably is.
3. What if it’s just one bump, can herpes start like that?
It can start small, which is where people get thrown off. But it rarely stays that way. Within a couple of days, herpes usually turns into a cluster or goes through that blister → crust cycle. If your bump just sits there, maybe gets a whitehead, and slowly calms down, that’s acne behavior.
4. I got a bump right after sex… should I be worried?
This is one of the biggest anxiety traps. The timing feels suspicious, but biologically it usually doesn’t line up. Most STDs, including herpes, don’t show visible symptoms the next day. If something pops up that quickly, it’s almost always unrelated, like acne, irritation, or friction. Your brain is connecting dots that your body didn’t actually connect.
5. Do STD-related bumps hurt more than acne?
It’s not really about “more” pain, it’s about the type of sensation. Acne hurts when you press on it. Herpes can feel active even when you’re not touching it, burning, tingling, or stinging. That difference comes from where the issue is happening: surface inflammation vs nerve involvement.
6. Can oral sex cause bumps on my face?
It can, but not in the random way people imagine. Herpes can be transmitted through oral contact, but it follows a very specific pattern and timeline. A breakout that looks and behaves like typical acne, especially in areas where you normally break out, is far more likely to be just that.
7. Why does everything online make this look worse than it is?
Because the internet loves extremes. You’re seeing the most obvious, textbook, worst-looking examples. Real-life cases are usually way less dramatic and way more ambiguous. That’s why comparing yourself to images online often creates more confusion than clarity.
8. Is it a bad idea to pop it just to see what happens?
Very bad idea. Not because it’s dangerous in a dramatic way, but because it ruins your ability to read what’s going on. You turn one bump into a red, irritated mess, and now everything looks suspicious. Plus, it can slow healing and increase the chance of scarring.
9. At what point should I stop watching it and just get tested?
If you’ve spent more than a couple of days analyzing it, checking it, Googling it, and you still don’t feel sure, that’s your answer. Testing isn’t about panic. It’s about ending the loop. Especially if the timing and symptoms don’t clearly match acne.
10. What if it turns out to be nothing and I tested for no reason?
Then you bought yourself peace of mind, and that’s not nothing. Most people who test in this situation end up confirming it’s not an STD. But the difference is, they know. And that shift, from guessing to knowing, is what actually lets you relax.
Take Control of the Guessing Game
If you have made it this far, you already understand the key difference: acne follows a pore-based pattern, while STD-related symptoms follow a completely different biological timeline and behavior. But when your brain keeps second-guessing what you are seeing, clarity matters more than reassurance.
A comprehensive option like a STD combo test kit allows you to check multiple infections at once from home, giving you a clear answer without waiting or wondering. If your concern is more specific, you can also explore targeted options through individual STD tests designed for accuracy and privacy.
If you are ready to stop guessing and get real clarity, you can explore all available options here: STD Rapid Test Kits. Your results, your timeline, your peace of mind.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it “came back.” In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC, Genital Herpes Fact Sheet
4. NCBI, Acne Vulgaris Overview
5. CDC, STD Testing Guidelines
6. MedlinePlus — Herpes Simplex
7. Planned Parenthood — Herpes
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.