Quick Answer: Yes, you can have both herpes and syphilis at the same time. Coinfection is medically documented, especially in people who are sexually active with multiple partners. While their symptoms sometimes overlap, herpes typically causes painful blisters while syphilis often starts with a painless sore. Testing is the only way to know for sure.
This Isn’t a “One or the Other” Kind of Situation
People love binaries. Good or bad. Clean or dirty. Safe or unsafe. But STDs don’t care about our need for clarity. They show up how they want, when they want, and, sometimes, with backup. According to a 2023 study in Sexually Transmitted Diseases, up to 18% of patients diagnosed with syphilis also tested positive for genital herpes. That number increases among populations with high partner turnover, inconsistent condom use, or pre-existing STDs like HIV.
The reason? Damage. STDs like herpes cause microscopic tears in the skin, which make it easier for other infections to sneak in. If you’ve already got herpes lesions and then have sex with someone carrying syphilis, especially during their highly contagious primary stage, your risk of catching both skyrockets. Add in the fact that early syphilis is often completely painless and herpes can present without any visible signs at all, and you’ve got the perfect storm of confusion and missed diagnoses.
What does this mean for you? It means stop looking for just one answer. It means your body might be telling you more than one story. And it means testing, real testing, is your only way out of the guessing game.
Herpes Sores, Syphilis Sores, and the Ones That Blur the Line
If you’ve ever tried to diagnose yourself using Google Images, you already know: STD visuals are a mess. What’s labeled “syphilis” on one site is called “herpes” on another. And what you’re looking at in the mirror might not look like any of them. But here’s what we know from clinicians and lived experience:
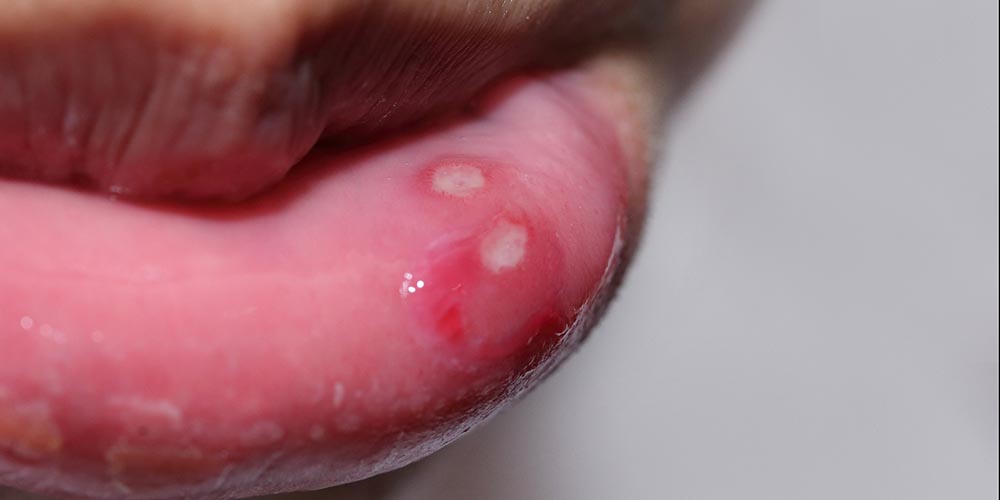
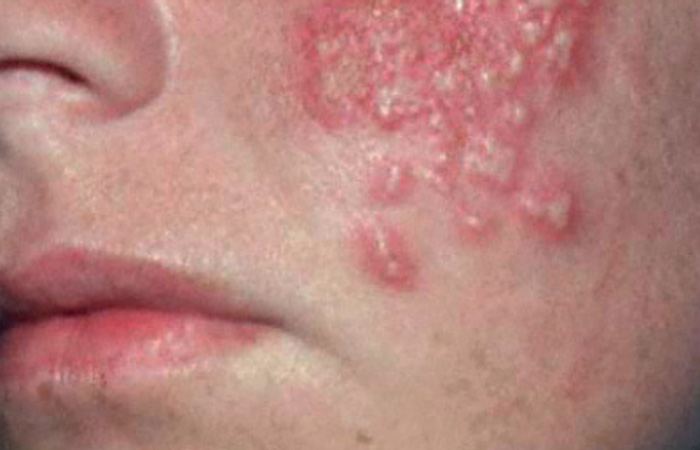
Herpes sores tend to show up in clusters, tiny, painful blisters that ooze and scab. They usually itch or burn, especially before they become visible. Most people say they feel a “tingling” before anything even surfaces. First outbreaks are brutal, flu-like symptoms, swollen lymph nodes, full-body ache. Recurrences are usually milder.
Syphilis, on the other hand, often starts with a single, round, painless sore called a chancre. It doesn’t hurt. It doesn’t itch. That’s why people miss it. It might look more like a shallow crater than a blister, and it disappears in a few weeks even without treatment. That’s when people think it’s “gone.” But it’s not. It’s just moved on to the bloodstream, potentially causing rashes, hair loss, even organ damage if untreated.
Now imagine having both at once. Maybe one sore stings and another doesn’t. Maybe you’ve got a cluster on your labia but also a single spot on your shaft. Maybe you’re dealing with both pain and silence at the same time. It’s overwhelming, but it’s not uncommon.
“I thought I was being punished,” Ty says, weeks after receiving both diagnoses. “I felt so stupid. Like, who gets two STDs at once? But my doctor didn’t blink. She said it happens all the time.”
Because it does.
People are also looking for: STDs and Self-Esteem: Why Diagnosis Feels Like Rejection
People Don’t Talk About It, But Coinfection Happens a Lot
There’s shame around just having one STD. Having two? That hits a deeper nerve. But here’s the truth: coinfection isn’t a moral failure. It’s a math problem. The more partners you have, the more chances for exposure. But even one night with one person who didn’t know they were contagious is enough. That doesn’t make you reckless. It makes you human.
A CDC report from 2024 found that coinfections with herpes, syphilis, and chlamydia are significantly rising, especially among people under 30. It's not because people are “riskier.” It’s because more people are using dating apps, exploring fluid sexual identities, and often skipping testing after casual hookups out of fear, shame, or inconvenience.
But here's the other reason coinfections go undetected: testing gaps. Most clinics don’t automatically test for herpes unless you have an active sore. Syphilis, on the other hand, can be detected through blood even without symptoms. That means some people might treat one and not know they’re carrying the other.
“We need to stop treating STD testing like a punishment,” says a sexual health nurse practitioner in a Planned Parenthood interview. “Testing is care. It’s maintenance. Like getting your oil changed or teeth cleaned.”
So if you’ve got a sore, even just one, and you’re spiraling between diagnoses? Get the full panel. Not just one box ticked. Not just one infection ruled out. The truth is: the sore doesn’t care what name you give it. It just wants attention.
The Emotional Whiplash of a Double Diagnosis
There’s something uniquely cruel about being told you have not one, but two STDs. Ty described it as “getting hit while already on the floor.” After years of clean tests, careful hookups, and near-religious condom use, he still ended up with both herpes and syphilis. One painful, the other silent. Both misunderstood.
“I felt disgusting. Like who gets two at once? I remember looking in the mirror and thinking, ‘You’ve ruined yourself.’”
This reaction is heartbreakingly common, and dangerously internalized. Because we don’t talk about coinfection publicly, it feels like a freak occurrence. But in reality, most clinicians aren’t surprised by it. They’ve seen it again and again: a painless syphilitic chancre hidden under the foreskin and a cracked herpes blister nearby. A vaginal herpes outbreak triggered by the immune stress of an undiagnosed syphilis infection. Two diseases, one tired immune system, zero judgment.
It’s not just about biology. It’s about shame, stigma, and silence. The kind that keeps people from testing until the symptoms are too obvious to ignore. The kind that whispers, “If you were more careful, this wouldn’t have happened.”
But here’s the medical truth: coinfections are biologically more likely once you have one STD. Herpes lesions create open doors for syphilis to enter. And syphilis-induced inflammation may increase herpes viral shedding. It’s not moral. It’s medical. And that’s exactly why testing is both care and prevention.
Testing Isn’t Just a Form, It’s a Filter for Truth
One of the biggest myths about STDs is that they’re obvious. That if you had herpes, you’d know. That syphilis would scream its presence with rashes or sores or “dirty” vibes. But most infections, especially in early stages, are quiet. Especially when they overlap.
A common scenario looks like this: you get tested after noticing a sore. The herpes swab comes back positive. You breathe a half-sigh of relief, at least you know what it is. But what you don’t know is that you also picked up syphilis from a different partner weeks earlier. The sore wasn’t from herpes or syphilis, it was from both.
That’s why comprehensive testing matters. You need a swab for herpes and a blood draw for syphilis. If a provider doesn’t offer the full range, ask for it. Or consider a discreet option like an at-home combo test kit that checks for multiple infections at once.
This combo STD test kit screens for multiple common infections from the privacy of home, no judgment required. If you’re not sure what sore you’re dealing with, or even if you’ve already been diagnosed with one STD, it’s worth checking for the rest. Clarity is power. Especially when you’re scared.
You don’t need to wait for symptoms to test. You don’t need to have slept with “a lot of people.” And you definitely don’t need to feel shame. What you do need is data. And action. And support.
Check Your STD Status in Minutes
Test at Home with RemediumGenital Herpes Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $45.99 $49.00
“I Got Diagnosed. Then I Got Angry.”
Ty didn’t just feel shame, he felt betrayed. Not by his body, but by the system that never told him this was possible. “I’ve been through health class. I’ve been through gay sex ed webinars. Nobody ever said you could have both. Nobody said herpes might hurt but syphilis might not. It felt like a setup.”
He’s not wrong. Our public health messaging often oversimplifies STDs to make them easier to teach. Herpes is painful. Syphilis is rare. HIV is lifelong. Chlamydia is curable. But the reality is messier, and sometimes, infections come in pairs. Especially in communities that are under-tested, under-treated, or over-stigmatized.
According to the World Health Organization, over 1 million STIs are acquired every day worldwide. Many go undetected, especially in early stages or when multiple infections mask each other’s symptoms. A 2024 surveillance review showed that coinfections are highest among sexually active adults under 35, especially those navigating queer, poly, or fluid sexual networks without regular testing access.
So no, Ty wasn’t alone. And neither are you.
“But We Used Protection”, Yeah, About That
Condoms are amazing. They reduce the risk of transmission for a lot of STDs. But not all. Herpes and syphilis are both spread through skin-to-skin contact. That means if a sore is on an area that isn’t covered, a pubic mound, inner thigh, shaft base, scrotum, labia, you can still catch it. Oral sex? Same deal. Dental dams and condoms help, but they aren’t perfect shields.
That doesn’t mean protection isn’t worth it. It absolutely is. But we need to stop treating it like a binary. You wore a condom, but you still got an STD? That’s not failure. That’s reality. That’s human. And that’s why testing, again and again, not just once a year, is what keeps you truly safe.
The idea that you must’ve done something “wrong” to catch more than one STD is rooted in outdated, moralistic thinking. The truth is: viruses don’t discriminate. They don’t care if you’re queer or straight, in a monogamous relationship or sleeping with three people. If there's skin contact, there's risk. And if there's silence around symptoms? There's a gap.
So let’s stop whispering. Let’s stop assuming one sore means one answer. Let’s stop punishing ourselves for being human, curious, and sexually active. Coinfection isn’t the end of the world. It’s the start of a conversation you deserve to have, with your partner, your doctor, and yourself.
Okay, But What Do I Do Now?
First, take a breath. Seriously. The panic you're feeling right now? It's valid, but it's also beatable. Coinfection doesn’t make you dirty, broken, or unlovable. It makes you part of a very real, very fixable public health issue. And the next step isn’t punishment, it’s power.
Let’s be clear: both herpes and syphilis are treatable. Syphilis, especially in its early stages, is curable with a single shot of penicillin or a short antibiotic course. Herpes isn’t curable, but it is very manageable with daily antivirals. Many people never have a second outbreak. Others go years between flare-ups. You are not doomed to live in pain, shame, or silence.
What’s important is that you don’t delay. The longer syphilis goes untreated, the more it hides, moving from your genitals into your bloodstream, brain, and organs. Herpes might lay low too, but it doesn’t vanish. You want to catch both early, not just for yourself, but for anyone you sleep with going forward.
And let’s talk about partners. You might feel tempted to hide the diagnosis, especially if you’re newly seeing someone or rekindling a flame. But silence feeds shame. And most people, once you explain what’s going on, are far more understanding than you expect. Especially if you’re already taking steps to test, treat, and protect.
“My partner thanked me,” Ty says, “for telling them. We both got tested together. They didn’t run. They actually respected me more.”
Honesty isn’t always easy. But it builds safety. And no matter your status, your body deserves safety, not just from infection, but from fear.

People are also reading: Top 8 At-Home STD Tests in 2025 (And Which Ones Actually Work)
How to Protect Yourself Without Giving Up Pleasure
Here’s where we flip the script. Because prevention doesn’t have to mean fear. And protection doesn’t mean celibacy or turning every hookup into a medical interview. It means being prepared, proactive, and honest about what you know, and what you don’t.
If you’re sexually active, especially if you have multiple partners or engage in unprotected oral or genital sex, you should be testing regularly. That means a full STD panel every 3–6 months depending on your lifestyle. Not just when symptoms show up. Not just when you start dating someone new. Regular testing is like brushing your teeth. It’s hygiene, not punishment.
And if symptoms do appear? Don’t freeze. Don’t guess. At-home STD test kits exist for exactly this moment. They’re confidential, accurate, and can test for multiple infections, herpes, syphilis, HIV, chlamydia, and more, all in one go. You deserve information that helps, not haunts.
If you’re in a relationship, talk about testing before ditching condoms. If you're exploring with new people, normalize asking when they last tested. If you're dealing with an outbreak, take care of yourself, and let partners know before engaging sexually. It doesn’t make you dangerous. It makes you decent.
Yes, you can still have amazing, joyful, safe sex after a herpes or syphilis diagnosis. You just might use a little lube, take a daily antiviral, and communicate a bit more than you used to. Welcome to grown-up sexual health, it’s better than the fear.
The Stories That Don’t Get Told
We hear a lot about single STDs. About the burning pee. The dreaded text from an ex. The cold panic of a missed period or strange rash. But coinfections? They don’t get headlines. They don’t show up in Instagram infographics or TikTok sex-ed accounts. They feel too complicated, too shamey, too... much.
But they matter. Because herpes and syphilis don’t live in silos. They share space, inside bodies and across communities. And understanding them, together, isn’t about scaring people into celibacy. It’s about equipping people to move through the world with clarity, confidence, and care.
Coinfection isn’t a red flag. It’s not a warning sign that you’ve done something wrong. It’s a signal, one that says it’s time to stop assuming, and start knowing. Time to stop blaming, and start protecting. Time to treat sexual health like the life-affirming act it is, not the shame-filled crisis it’s been made out to be.
You deserve pleasure. You deserve partners who care. You deserve doctors who don’t flinch, and tools that help you test without judgment. You deserve answers, not assumptions.
And if you’ve got both? That’s not the end of your story. It’s just a plot twist. One you can absolutely handle.
FAQs
1. Can I really have both herpes and syphilis?
Yes, annoyingly, you can. It’s not rare, it’s not dramatic, and it doesn’t mean anything about your worth. Coinfection is medically common, especially if you’ve got one infection already. Herpes can create tiny skin breaks that make it easier for syphilis to sneak in.
2. How do I tell which sore is which?
Truth bomb? You probably can’t. Herpes sores usually hurt and come in clusters. Syphilis sores are often solo, round, and weirdly painless. But both can get creative. Best move? Don’t play dermatology detective, get both a swab and a blood test.
3. What if I already know I have herpes, is syphilis still something to worry about?
Definitely. One doesn’t cancel the other out. In fact, herpes can increase your risk of catching syphilis. If it’s been a while since your last full panel, or your symptoms feel “off”, get checked for syphilis too.
4. Can I get this from oral sex?
Yup. Both herpes and syphilis can be passed through mouth-to-genital or mouth-to-mouth contact. If someone has a cold sore or oral syphilis (which exists and isn’t talked about nearly enough), and you go down on them, boom, risk.
5. Do I need to tell my partner if I’m diagnosed?
It's not just respectful, it’s empowering. You don’t have to spill every detail of your sexual history, but giving your partner a heads up helps them make decisions for their own health. Most people? They won’t freak. Especially if you come to them with clarity and a plan.
6. But we used a condom, how did this happen?
Condoms lower risk, but they don’t make you invincible. Herpes and syphilis can both live outside the covered zone. A sore on the thigh, scrotum, or outer labia can still transmit infection during “protected” sex.
7. What happens if I ignore a syphilis infection?
At first? Maybe nothing. The sore disappears. You might even think it healed. But inside? It’s leveling up. Untreated syphilis can eventually damage your brain, heart, and nervous system. It’s one of those infections you don’t want to ghost you.
8. Is herpes forever?
Technically yes, but it’s not what you think. Herpes can go dormant for months or years, and many people never have another outbreak. Daily medication can reduce symptoms and transmission risk. And no, your sex life isn’t over. Pinky swear.
9. How do I even start testing for both?
You don’t need to jump through hoops. A combo at-home test kit lets you test for multiple STDs in one go, herpes, syphilis, HIV, chlamydia, and more. No clinic lines. No awkward questions. Just clarity.
10. What if I’m scared to know?
Then you’re like 90% of people Googling this at 2AM. It’s okay to be scared. But knowing is kinder than spiraling. Whatever shows up, there’s a plan for it. And nothing, nothing, you find means you’re alone or unworthy.
You Deserve Answers, Not Assumptions
This isn’t just about one sore, or even two. It’s about rewriting how we think about our bodies, our risks, and our right to clarity. Coinfections like herpes and syphilis aren’t rare, shameful, or hopeless, they’re treatable realities that more people experience than you’d ever guess.
Don’t sit in the spiral. Don’t assume. Get answers.
This at-home combo test kit checks for the most common STDs discreetly and quickly. It’s time to stop guessing, and start knowing.
Sources
1. World Health Organization – STI Fact Sheet
2. Planned Parenthood – STDs & Testing
3. CDC – Herpes Treatment Guidelines
4. Mayo Clinic – Syphilis Overview
5. Reddit – STD Confession Threads
6. PMC – Coinfection Patterns in Japan
7. Incidence of Co-Infections of HIV, Herpes Simplex Virus Type 2 and Syphilis