Last updated: April 2026
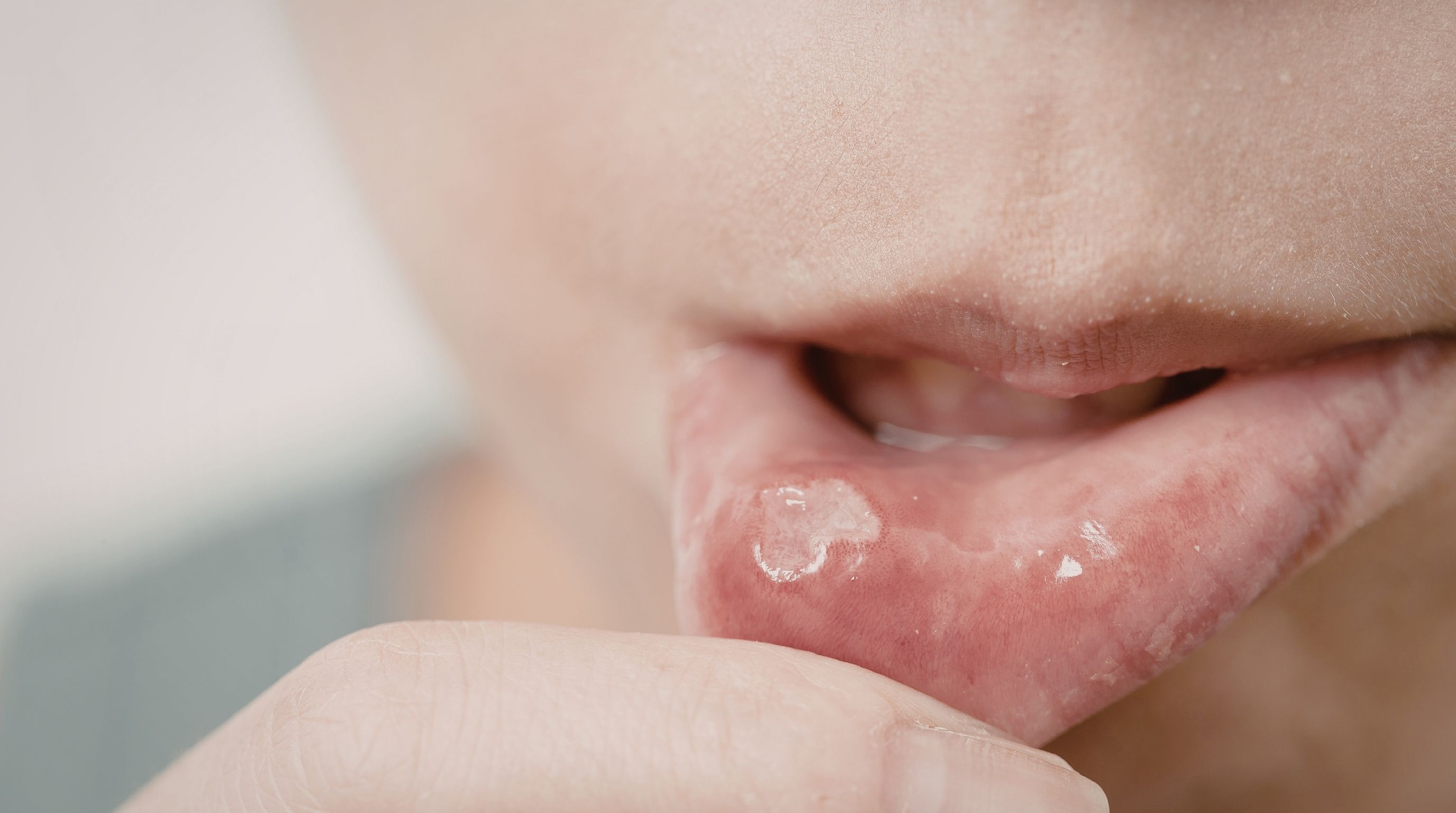
Yes, you can give someone genital herpes from a cold sore because HSV-1 spreads through direct oral-to-genital contact and infects mucosal tissue the moment it enters through microscopic breaks in the skin.
Cold sores are often treated like a minor inconvenience, something you ignore until it disappears. But the virus behind them, HSV-1, does not stay limited to the lips. It moves through direct skin-to-skin contact, and oral sex is one of the most efficient ways it reaches a new location in the body. What looks like a harmless sore can become a lifelong genital infection for someone else.
Most people are never clearly told this. Cold sores are normalized early in life, while genital herpes is framed as something separate and more serious. In reality, they are caused by closely related viruses that behave almost identically once they enter the body. The only difference is where the virus enters, and how it spreads from there.
Understanding how that transmission actually works is what prevents accidental spread. With herpes, the biggest risk does not come from reckless behavior, it comes from not knowing how the virus actually moves between people.
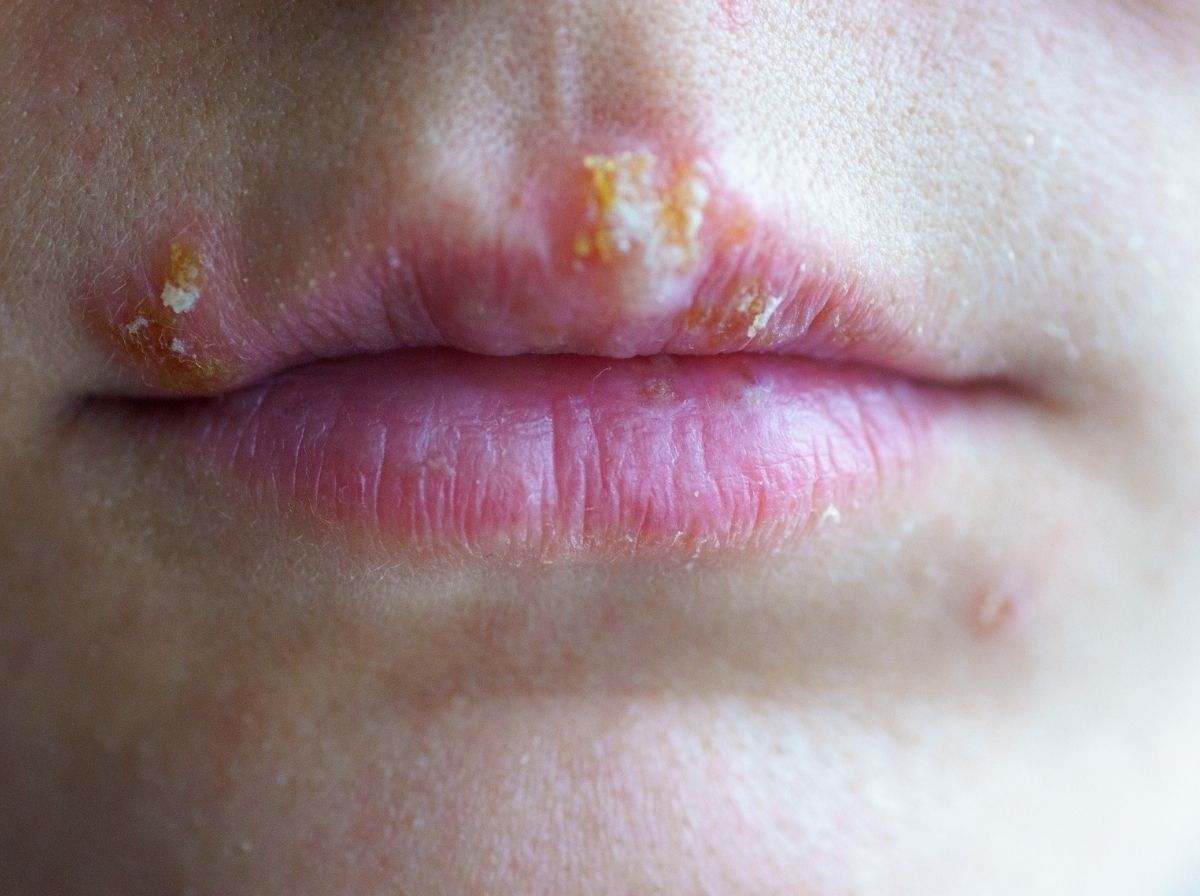
People are also reading: Understanding HIV Rash: Symptoms, Treatment, and Identification
Can a Cold Sore Cause Genital Herpes?
Cold sores are caused by herpes simplex virus type 1 (HSV-1), and that same virus is fully capable of infecting the genital area if it reaches it through direct contact. There is no biological barrier that keeps HSV-1 “oral only.” The virus infects epithelial cells at the point of contact, then travels through local nerve endings where it establishes a lifelong presence in nearby nerve ganglia.
That’s why location is not determined by the virus type alone, but by where it enters the body. If HSV-1 enters through the lips, it becomes oral herpes. If it enters through the genital tissue during oral sex, it becomes genital herpes. The mechanism is identical; only the entry point changes.
This shift has already happened at a population level. According to World Health Organization data on HSV-1, oral herpes is extremely common globally, and a growing proportion of new genital herpes infections are now caused by HSV-1 rather than HSV-2. That change is driven largely by oral sex transmission, not traditional genital-to-genital spread.
The important part here is clarity: a cold sore is not just a cosmetic issue. It is an active viral state that can infect another person’s genitals if contact happens at the wrong moment.
And “wrong moment” does not mean only when a blister is visible.
How HSV-1 Moves from Mouth to Genitals During Oral Sex
The transmission itself is straightforward, but what makes it risky is how easily it happens without being obvious. HSV-1 spreads through direct skin-to-skin contact, specifically when infected oral tissue touches the thin, highly absorbent mucosal surfaces of the genitals.
Genital skin, especially areas like the vulva, cervix, or the urethral opening, contains microabrasions that occur naturally during sexual activity. These microscopic breaks are not injuries you can see or feel, but they are enough for the virus to enter. Once HSV-1 crosses that barrier, it begins replicating locally before establishing latency in the nervous system.
This process can begin within hours of exposure. The virus does not need prolonged contact, ejaculation, or repeated exposure. A single oral sex encounter during an active shedding period is sufficient to establish infection.
There is also a phase called the prodrome, the early stage before a cold sore becomes visible. During this phase, the virus is already replicating at the surface of the skin. Tingling, burning, or itching around the lip reflects nerve activation and viral movement toward the skin, which means transmission risk is already active at that point.
Even more important: transmission is not limited to visible outbreaks. HSV-1 can shed from oral tissue without any symptoms at all. This is why relying on “I don’t see a sore” is not a reliable way to assess risk.
Check Your STD Status in Minutes
Test at Home with RemediumGenital Herpes Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $45.99 $49.00
How Do People Accidentally Spread Genital Herpes Through Oral Sex?
Most people separate cold sores and genital herpes in their minds because that’s how they were introduced to them. Cold sores are framed as common and harmless, often picked up in childhood through non-sexual contact. Genital herpes, on the other hand, is framed as an STI associated with sexual transmission. That mental split creates a blind spot.
In reality, the virus does not follow those categories. HSV-1 does not “know” it started on the mouth. If it reaches the genitals, it behaves like genital herpes from that point forward. It can cause outbreaks, remain dormant, and reactivate later under the same biological rules.
Another reason this gets missed is timing. People often associate transmission only with visible sores, but viral shedding begins before a blister appears and can continue after it heals. According to research summarized in NCBI studies on HSV shedding patterns, HSV-1 is detectable on oral surfaces even when no lesions are present, which explains why many transmissions happen unintentionally.
Then there’s the way oral sex is perceived. It’s often treated as lower risk compared to penetrative sex, which leads people to skip the kind of caution they might otherwise use. No condom, no conversation, no pause if something feels slightly off around the mouth. From a biological standpoint, though, oral-genital contact is a direct transmission pathway for HSV-1.
The result is a pattern that repeats constantly: someone has a cold sore history, doesn’t think of it as relevant, engages in oral sex, and only later realizes that genital symptoms have appeared in their partner. Not because they were careless, but because the risk was never explained clearly in the first place.
Asymptomatic Shedding: When Herpes Spreads Without a Sore
One of the biggest misconceptions about herpes is that transmission only happens when a sore is visible. In reality, HSV-1 can be active on the skin without producing any noticeable symptoms, a process known as asymptomatic shedding. This is not a rare exception, it is a built-in part of how the virus behaves.
After HSV-1 enters the body, it travels to nearby nerve ganglia where it remains dormant between reactivations. During these reactivations, the virus can move back to the surface of the skin. Sometimes that results in a visible cold sore. Other times, it reaches the surface, replicates briefly, and sheds without creating any lesion at all.
This is why someone can feel completely fine, see no sore, and still be contagious. Studies tracking oral HSV-1 activity show that viral DNA can be detected on the lips and surrounding tissue even when no outbreak is present. From a biological standpoint, the virus does not need to produce symptoms to be transmissible, it only needs to be present on the skin at the moment of contact.
In practical terms, this means oral sex carries risk even outside of obvious outbreaks. The absence of a sore does not equal zero risk. It simply means the virus is not producing visible inflammation at that moment.
This is also why timing matters more than intuition. You cannot reliably judge infectiousness based on how your mouth looks or feels. The only consistent factor you can control is when exposure happened and when testing becomes accurate afterward.

People are also reading: What Does Chlamydia Discharge Look Like? Complete Guide for Men and Women
STD Testing After Oral Herpes Exposure: What Actually Works
If you’ve had oral sex with someone who has a history of cold sores, or you’ve given oral sex while carrying HSV-1, testing is the only way to move from uncertainty to clarity. But timing is everything, because your body needs time to produce detectable markers of infection.
For herpes specifically, testing relies on blood tests that detect antibodies or swab tests taken directly from an active lesion. If no visible sore is present, a blood test becomes the primary method, but it only becomes reliable once your immune system has had time to respond.
Herpes follows a defined window period. Herpes HSV-1 and HSV-2: test from 6 weeks after exposure. This is the point at which antibody levels become detectable in most people. Testing before that window can produce a false negative, not because the infection isn’t there, but because the immune response has not reached measurable levels yet.
And herpes is not the only concern after oral-genital exposure. Oral sex can also transmit bacterial infections and other viruses, which is why comprehensive testing often includes multiple infections with different detection windows.
| Infection | When to Test |
|---|---|
| Chlamydia | Chlamydia: test from 14 days after exposure |
| Gonorrhea | Gonorrhea: test from 3 weeks after exposure |
| Syphilis | Syphilis: test from 6 weeks after exposure |
| HIV | HIV: test at 6 weeks for first indicator, retest at 12 weeks for certainty |
| Herpes (HSV-1 & HSV-2) | Herpes HSV-1 and HSV-2: test from 6 weeks after exposure |
| Hepatitis B | Hepatitis B: test from 6 weeks after exposure |
| Hepatitis C | Hepatitis C: test from 8–11 weeks after exposure |
For chlamydia and gonorrhea, nucleic acid amplification testing (NAAT) is used because it detects bacterial genetic material directly at the site of infection. These infections can establish quickly, which is why testing begins earlier, Chlamydia: test from 14 days after exposure and Gonorrhea: test from 3 weeks after exposure.
For viral infections like HIV, syphilis, herpes, and hepatitis, blood tests are used because they detect immune response markers rather than the pathogen itself. This is why the window period is longer. Syphilis: test from 6 weeks after exposure and Hepatitis B: test from 6 weeks after exposure reflect the time required for antibody production, while Hepatitis C: test from 8–11 weeks after exposure accounts for its slower detectability.
HIV follows a two-step confirmation process. HIV: test at 6 weeks for first indicator, retest at 12 weeks for certainty. The first test detects early immune response, while the second confirms that no late seroconversion occurred.
If you want clarity without waiting for clinic appointments, using a comprehensive at-home option like the Complete 7-in-1 STD Home Test Kit allows you to check multiple infections within their correct biological windows, using the same timing principles described above.
The key takeaway is simple but often missed: testing too early does not give you peace of mind, it gives you incomplete information. Accurate results depend on matching the test to the biology of the infection.
Check Your STD Status in Minutes
Test at Home with RemediumOral Herpes Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $33.99 $49.00
What Do Herpes Text Results Mean?
A negative herpes test result only means that no detectable antibodies were found at the time of testing. If the test was taken before the 6-week window, it does not rule out infection, it means the immune system may not have produced enough antibodies yet. This is what creates a false negative.
A positive result, on the other hand, confirms that HSV-1 or HSV-2 is present in the body. It does not tell you when the infection occurred or where it entered, but it does confirm that the virus is established and capable of reactivation.
This is where retesting becomes important. If an initial test is taken early, repeating it after the full window period ensures that delayed antibody production is captured. The reason is biological, not procedural, the immune system builds detectable markers over time, not instantly.
For someone exposed through oral sex, this means the timeline matters more than the moment of concern. Testing at the correct interval is what turns uncertainty into a clear answer. Without that timing, results can easily be misinterpreted.
How Do You Prevent Spreading Genital Herpes During Oral Sex?
Understanding how HSV-1 spreads does not mean avoiding intimacy altogether. It means making decisions based on how the virus actually behaves, not on assumptions. The most effective way to reduce risk is to avoid oral sex during active outbreaks and during the prodrome phase, when tingling or burning signals that the virus is moving to the surface of the skin.
Barrier protection adds another layer. Condoms and dental dams reduce direct skin-to-skin contact, which is how HSV-1 transmits. They do not eliminate risk entirely, because herpes can affect areas outside the covered region, but they significantly lower the chance of transmission during oral-genital contact.
There is also a timing component that most people overlook. The longer the gap since the last outbreak, the lower the likelihood of active viral shedding on any given day. While shedding can still occur unpredictably, spacing sexual contact away from recent outbreaks reduces the probability that the virus is present at the surface.
For people who experience frequent cold sores, long-term management strategies can further reduce transmission risk by limiting how often the virus reactivates. The key is understanding that prevention is not about guessing, it is about aligning behavior with how HSV-1 actually operates in the body.
And if there has already been a potential exposure, testing at the correct time point is the most reliable way to replace uncertainty with a clear answer.
The best ways to stop HSV-1 from spreading are to stop it from getting to another person's genital tissue at the right times.
| Prevention Step | What It Changes Biologically |
|---|---|
| Avoid oral sex during an active cold sore | This prevents contact during the phase when HSV-1 is concentrated at the skin surface and most easily transmitted. |
| Avoid oral sex during the prodrome stage | Tingling, burning, or itching can mean the virus is already moving through nerve pathways back to the skin, so transmission risk begins before a blister fully appears. |
| Use condoms or dental dams during oral sex | Barrier protection reduces direct skin-to-mucosa contact, which lowers the chance that HSV-1 reaches genital tissue through microscopic breaks in the skin. |
| Wait until the outbreak has fully resolved before resuming contact | This reduces the chance of exposure while viral shedding remains active around healing tissue. |
| Test after a known exposure at the correct window | Herpes HSV-1 and HSV-2: test from 6 weeks after exposure, because antibody-based blood tests need time for the immune response to become detectable. |
None of these steps stop HSV-1 from coming back, but they do lower the chances that oral shedding will lead to genital transmission.
When Is HSV-1 Most Likely to Spread?
HSV-1 is most likely to spread when the virus is actively replicating at the surface of the skin, which happens during specific phases of its lifecycle. The highest transmission risk occurs during an active cold sore, when viral particles are concentrated in the blister and surrounding tissue.
The next highest-risk phase is the prodrome stage. This is the period just before a sore appears, when tingling, burning, or itching signals that the virus is traveling from nerve cells back to the skin. At this point, viral shedding has already begun, even though no visible lesion is present.
Outside of these phases, HSV-1 can still spread through asymptomatic shedding. This occurs when the virus briefly reactivates and reaches the skin without causing noticeable symptoms. The amount of virus present is typically lower than during an outbreak, but transmission is still biologically possible if direct contact occurs.
This pattern is what makes HSV-1 difficult to predict. The virus does not follow a visible schedule, and transmission risk is tied to microscopic activity rather than what can be seen. That’s why timing, not appearance, is the most reliable way to think about risk.

People are also reading: Is Discharge Without Pain a Sign of an STD?
FAQs
1. Can you get genital herpes from a cold sore?
Yes. HSV-1 from a cold sore can infect genital tissue during oral sex if it reaches mucosal surfaces or microscopic breaks in the skin.
2. Is HSV-1 the same as genital herpes?
HSV-1 is a virus type. When it infects the genitals, it becomes genital herpes, even though it is more commonly associated with oral infections.
3. Can herpes spread without a visible sore?
Yes. Asymptomatic shedding allows HSV-1 to be present on the skin without visible symptoms, making transmission possible even when no sore is seen.
4. How soon after exposure should I test for herpes?
Herpes HSV-1 and HSV-2: test from 6 weeks after exposure to allow antibodies to reach detectable levels.
5. Can one encounter cause genital herpes?
Yes. A single oral sex encounter during a shedding period is sufficient for HSV-1 transmission and lifelong infection.
6. What does a negative herpes test mean?
A negative result means no detectable antibodies at the time of testing. If taken before 6 weeks, it may not rule out infection.
7. What does a positive herpes test mean?
A positive result confirms that HSV-1 or HSV-2 is present in the body and can reactivate over time.
8. Can HSV-1 spread genitally after oral infection?
Yes. Once HSV-1 infects the genitals, it can be transmitted through genital contact under the right conditions.
9. Do condoms fully prevent herpes transmission?
No. They reduce risk significantly but do not eliminate it, because herpes can spread from uncovered skin.
10. What is the most reliable way to know if I was infected?
Testing at the correct biological window, combined with understanding exposure timing, provides the most accurate answer.
Check Your STD Status in Minutes
Test at Home with RemediumGenital & Oral Herpes Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $75.00 $98.00
For all 2 tests
Take Control of Your Sexual Health
Cold sores are common, but the virus behind them carries real transmission risk when oral sex is involved. That risk is not about fear, it is about understanding how HSV-1 behaves and making informed decisions based on that reality.
If there has been any potential exposure, the fastest way to stop second-guessing is to test at the right time. A targeted option like the HSV-1 At-Home Rapid Test Kit or a broader screen like the Complete STD Home Test Kit allows you to check your status privately and accurately.
For full access to all available options, visit the STD Rapid Test Kits homepage and choose the test that matches your situation. Clarity is not something you wait for, it is something you take action on.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. World Health Organization, Herpes Simplex Virus (HSV-1 and HSV-2)
2. CDC, Genital Herpes Fact Sheet
3. NCBI, Herpes Simplex Virus Shedding and Transmission
4. NCBI, Herpes Simplex Virus Overview
5. CDC, STI Treatment Guidelines: Herpes
6. WHO, Global Health Sector Strategies on STIs
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: STD Rapid Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.