Last updated: April 2026
Seeing discharge without pain is one of those moments that sends people straight to Google, usually late at night, scrolling through worst-case scenarios. The tricky part is that discharge sits right in the overlap between completely normal body function and early-stage infection. That’s why guessing rarely works. What matters is understanding what’s happening biologically and when testing actually gives you a clear answer.
Discharge is your body’s way of moving fluids, cells, and bacteria out of the reproductive or urinary tract. That process doesn’t automatically involve inflammation or nerve irritation, which is why pain isn’t always part of the picture. In fact, some of the most common STDs are designed, biologically speaking, to stay quiet at first.
So instead of asking “does it hurt?”, the better question is: what type of discharge is this, and what timeline are we working with?
Discharge without pain can absolutely be caused by an STD, because many infections begin by altering mucous production without triggering inflammation or nerve signals. That means your body can be actively responding to bacteria or viruses while you feel completely normal.
People are also reading: STD Myths That Are Putting You at Risk (And What’s Actually True)
What Does Discharge Without Pain Actually Mean?
Discharge is not automatically a problem, it’s a biological function. The cells lining the genitals, urethra, and cervix constantly produce mucus as part of maintaining moisture, balancing bacteria, and clearing out debris. This process happens continuously, whether or not an infection is present.
The key detail is this: pain usually comes from inflammation, not from the presence of discharge itself. Inflammation happens when the immune system sends signals that irritate nearby tissue and activate nerve endings. If that immune response hasn’t kicked in yet, or is still mild, you can have visible discharge with zero discomfort.
This is why early-stage infections often go unnoticed. Bacteria like chlamydia infect the cells lining the genital tract and begin replicating inside them. During this phase, the body may increase mucus production as a response, but without enough immune activation to create pain or burning. The result is discharge that looks unusual but doesn’t feel like anything.
On the flip side, normal discharge also changes based on hormones, hydration, sexual activity, and natural bacterial shifts. That’s what makes this confusing: the same symptom can come from completely different mechanisms.
Can STDs Cause Discharge Without Any Pain?
Yes, and this is where a lot of people get misled. The absence of pain does not rule out an STD. In fact, several of the most common infections are known specifically for being silent in the early stages.
Chlamydia is a perfect example. It infects epithelial cells and replicates inside them, which allows it to spread without immediately triggering a strong immune response. Because of that, discharge can appear as one of the first visible signs, often before any burning, irritation, or pelvic discomfort develops.
Gonorrhea can behave similarly, especially in the first phase after exposure. The bacteria attach to mucosal surfaces and begin multiplying, leading to increased secretion. Pain typically shows up later, once inflammation intensifies and starts affecting surrounding tissue.
Even viral infections like herpes can present without pain at first, particularly if lesions are internal or very mild. In these cases, discharge may be related to the body’s immune response rather than visible sores.
What all of these have in common is timing. The infection starts at a cellular level, changes fluid production, and only later, if at all, triggers symptoms you can feel.
Normal vs STD Discharge: How to Tell the Difference
Trying to self-diagnose discharge based on appearance alone is one of the least reliable strategies. Still, there are patterns that can help you understand what’s more likely, not as a diagnosis, but as a signal of whether testing makes sense.
Normal discharge is driven by hormonal cycles and natural bacterial balance. It tends to be predictable, even if it varies slightly in consistency or volume. STD-related discharge, on the other hand, comes from infection-driven changes in the cells lining the reproductive or urinary tract.
The difference comes down to cause: hormone-regulated secretion versus infection-triggered secretion.
| Feature | Normal Discharge | Possible STD-Related Discharge |
|---|---|---|
| Color | Clear or white | Yellow, green, cloudy, or gray |
| Consistency | Changes with hormonal cycle | Persistent or unusually thick |
| Odor | Mild or none | Stronger or distinctly unusual |
| Timing | Follows hormonal patterns | Appears after sexual exposure |
| Pain | None | Often none in early-stage infections |
The Most Common STDs Linked to Discharge Without Pain
When discharge shows up without pain, the list of possible causes narrows down to infections that affect mucosal surfaces without immediately triggering inflammation. These infections change how cells produce and release fluids, that’s why discharge appears before discomfort.
Chlamydia is the most common cause in this category. It infects epithelial cells and replicates inside them, which allows it to spread quietly. The body responds by increasing mucus production, leading to discharge that may be clear, cloudy, or slightly yellow. Because the immune response builds gradually, pain is often absent in the early phase.
Gonorrhea also targets mucosal linings, particularly in the urethra, cervix, rectum, or throat. In its early stage, it increases fluid secretion as bacteria multiply on the surface of these tissues. Pain typically develops later, once inflammation intensifies and begins irritating nerve endings.
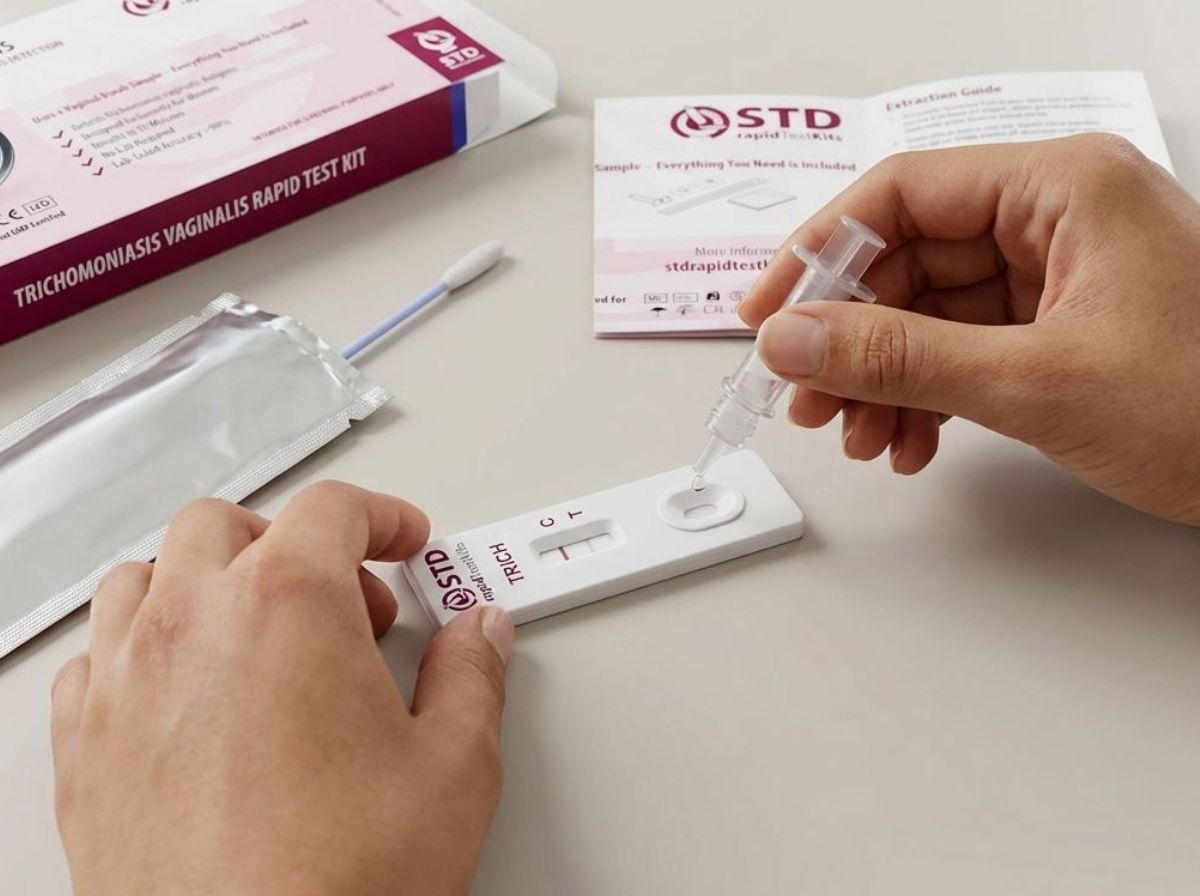
Trichomoniasis, caused by a protozoan parasite, can also produce discharge without immediate discomfort. The organism disrupts the natural balance of vaginal or genital flora, which changes the consistency and odor of discharge before irritation becomes noticeable.
What connects these infections is simple: they start by altering cells and secretions, not by triggering pain. That delay is exactly why timing your test correctly matters more than waiting for symptoms to escalate.
Check Your STD Status in Minutes
Test at Home with Remedium3-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $69.00 $147.00
For all 3 tests
When to Test: Timing Matters More Than Symptoms
This is the part most people get wrong. Testing too early can give you a negative result even if an infection is already in your body. That’s because STD tests detect either the genetic material of bacteria (NAAT tests) or antibodies produced by your immune system (blood tests). Both require time after exposure to reach detectable levels.
If discharge appears after sexual contact, the correct move is not immediate testing; it’s testing at the right biological window. That’s what determines whether your result is accurate.
At-home STD testing uses two main methods: NAAT (nucleic acid amplification tests) for infections like chlamydia and gonorrhea, and blood tests for infections like HIV, syphilis, herpes, and hepatitis. Each test has a specific window period based on how the infection develops in the body.
| STD | When to Test | Detection Method | Biological Reason |
|---|---|---|---|
| Chlamydia | 14 days after exposure | NAAT (urine or swab) | Bacteria replicate inside epithelial cells before DNA becomes detectable |
| Gonorrhea | 3 weeks after exposure | NAAT (urine or swab) | Bacterial load must reach detectable levels in mucosal tissue |
| Syphilis | 6 weeks after exposure | Blood test | Antibodies require time to develop in bloodstream |
| HIV | 6 weeks (first test), 12 weeks (confirmation) | Blood test | Immune response markers increase progressively after infection |
| Herpes (HSV-1 & HSV-2) | 6 weeks after exposure | Blood test | Antibody production becomes detectable after immune activation |
| Hepatitis B | 6 weeks after exposure | Blood test | Viral antigens and antibodies appear after incubation period |
| Hepatitis C | 8–11 weeks after exposure | Blood test | Antibodies and viral RNA reach detectable levels over time |
A negative result means that no infection was detected at the time of testing, but if the test was taken before the window period, the pathogen may still be present but below detectable levels. That’s what creates a false negative.
A positive result means the infection has been confirmed through either genetic detection (NAAT) or antibody presence in blood. At that point, the next step is clinical follow-up for treatment or management, not more guessing.
If you test before the correct window, retesting is necessary because your body may not have produced enough detectable markers yet. This is not a precaution; it’s based on how infections replicate and how the immune system responds over time.
For complete clarity, using a full-panel kit that covers all major infections removes the need to guess which test to take:
Complete STD Home Test Kit Package
Testing is the fastest way to stop the uncertainty, and when it’s done at the right time, it gives you a definitive answer.
What Happens If You Ignore Discharge?
Ignoring discharge without pain doesn’t stop an infection, it just allows it more time to develop. The underlying issue is that many STDs continue replicating at a cellular level even when symptoms remain mild or absent.
Chlamydia and gonorrhea, for example, can ascend the reproductive tract over time. In people with a cervix, this can lead to pelvic inflammatory disease when bacteria reach the uterus and fallopian tubes. In people with a penis, untreated infection can affect the epididymis, which plays a role in sperm transport.
This progression is not about how intense symptoms feel, it’s about how long the bacteria have been present and multiplying. That’s why relying on pain as a signal can delay detection.
Even in cases where discharge is not caused by an STD, ignoring persistent changes means missing the opportunity to identify what your body is responding to. Either way, clarity comes from testing, not waiting.
What to Do Next If You Notice Discharge Without Pain
If you’re seeing discharge without pain, the next step is not guessing, it’s aligning your timeline with the correct testing window. Discharge tells you that something in your body’s normal fluid balance has changed. What matters is identifying whether that change is driven by hormones, natural bacterial shifts, or an infection that started after a specific exposure.
The most important question to answer is: when was your last sexual contact with a new or untested partner? That date determines everything. If the exposure happened recently, testing immediately may not detect an infection yet. If enough time has passed to match the testing windows, you can get a definitive result.
This is where most people lose time, they either test too early and get a false negative, or they wait for symptoms like pain that may never show up. Neither approach gives clarity. Testing at the correct biological window does.
If your exposure falls within the correct timeframe, using a full-panel at-home test removes the need to guess which infection to check for. One kit, one sample process, complete clarity:
Peace of mind is not about waiting, it’s about getting a clear answer based on how your body actually works.
Why Discharge Can Appear Without Other Symptoms
One of the most misunderstood aspects of STDs is that symptoms don’t appear all at once. Biologically, infections develop in stages. The first stage often involves colonization, where bacteria or viruses attach to cells and begin replicating. During this phase, the body may increase mucus production as a response, which shows up as discharge.
At this point, the immune response is still localized and relatively mild. That means inflammation hasn’t reached the level needed to trigger nerve irritation, which is what creates pain, burning, or discomfort. So the infection is active, but your body hasn’t escalated its response yet.
This is especially common with chlamydia, where the bacteria live inside cells and avoid immediate detection. According to the CDC, a large percentage of infections remain asymptomatic in early stages, which is why routine testing is emphasized as a primary detection method rather than symptom-based diagnosis.
The takeaway is simple: discharge is often an early signal, not a late one. Waiting for additional symptoms means waiting for the infection to progress.
When Discharge Is NOT an STD
Not all discharge is linked to sexually transmitted infections. In many cases, the cause is completely unrelated to sexual exposure and instead tied to normal biological processes or temporary imbalances.
Hormonal fluctuations are one of the most common reasons. Estrogen levels directly influence mucus production, which means discharge naturally changes throughout the menstrual cycle. Around ovulation, for example, discharge becomes clearer and more elastic as the body prepares for potential fertilization.
In people with a penis, pre-ejaculatory fluid (pre-cum) can appear without any sexual activity leading to ejaculation. This fluid is produced by glands that lubricate the urethra and can be released in response to arousal, again, without pain or discomfort.
Bacterial imbalance is another factor. When the natural microbiome shifts, the body may produce more discharge as it tries to restore balance. This is not always related to an STD, but it can look similar, which is why testing becomes the deciding factor when timing aligns with exposure.
The key distinction is cause: if discharge appears independently of sexual exposure, it is more likely linked to internal regulation. If it appears after exposure, testing becomes essential to rule out infection.
People are also reading: I Think I Saw a Chancre, What Should I Do?
FAQs
1. Can you have an STD with discharge but no pain?
Yes. Infections like chlamydia and gonorrhea often begin by increasing mucus production without triggering inflammation, which means discharge can appear before any pain develops.
2. How soon after exposure can discharge appear?
Discharge can appear within several days after exposure because bacterial replication begins quickly, but testing accuracy depends on reaching the correct detection window.
3. Is clear discharge a sign of an STD?
Clear discharge is often normal, but if it appears after sexual exposure and differs from your usual pattern, testing is the only way to confirm whether infection is present.
4. Should I wait for pain before getting tested?
No. Pain is caused by inflammation, which may develop later or not at all. Testing should be based on exposure timing, not symptom intensity.
5. What STD causes discharge without burning?
Chlamydia is the most common, followed by early-stage gonorrhea and trichomoniasis, all of which can produce discharge before irritation begins.
6. Can discharge go away on its own if it’s an STD?
Visible discharge may decrease temporarily, but the infection remains active at a cellular level until treated.
7. Is odor a reliable sign of an STD?
Odor changes can occur with infections, but they are not specific enough to identify a particular STD without testing.
8. Can you test too early for an STD?
Yes. Testing before the window period can result in a false negative because the infection has not reached detectable levels.
9. What is the most accurate way to test?
NAAT tests for bacterial STDs and blood tests for viral infections provide high accuracy when used at the correct time after exposure.
10. What should I do right now if I have discharge?
Identify your last potential exposure, match it to the correct testing window, and use a full-panel test to get a definitive answer.
Take Control of Your Sexual Health
If you’re dealing with discharge and uncertainty, the fastest way to move forward is testing. Not guessing, not waiting, not overanalyzing symptoms, just a clear answer based on how your body actually works.
Get the 7-in-1 Complete At-Home STD Test Kit
Explore all STD testing options
Your results, your privacy, your clarity, all from home.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC, 2024 National STI Surveillance Data Release
2. NCBI StatPearls, Urethritis: Clinical Review
3. CDC STI Treatment Guidelines, Urethritis and Cervicitis
4. MSD Manual, Chlamydia: Symptoms and Diagnosis
5. MedlinePlus, Chlamydial Infections in Males
6. World Health Organization, Chlamydia Fact Sheet
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.










