Last updated: April 2026
Most STD panels are designed to detect infections that have clear treatment pathways and high immediate health risks, which is why herpes often gets excluded despite being extremely common. Medical guidelines prioritize infections like chlamydia, gonorrhea, HIV, and syphilis because early detection directly changes treatment outcomes and transmission risk. Herpes, on the other hand, behaves differently in the body, and that difference is exactly why it gets skipped.
That gap creates a weird situation: you can leave a clinic thinking you’ve been “tested for everything,” when herpes was never part of the panel. And unless someone explains that clearly, most people don’t realize it until much later.
Herpes is not rare, not dangerous for most people, and not automatically included in testing. Those three facts together are what make this topic so confusing, and why it deserves a straight answer.
Herpes is not included in routine STD testing, as it is normally tested for with an antibody blood test, which can give false results for those without symptoms, and it is more important to avoid false positives than to identify all cases.
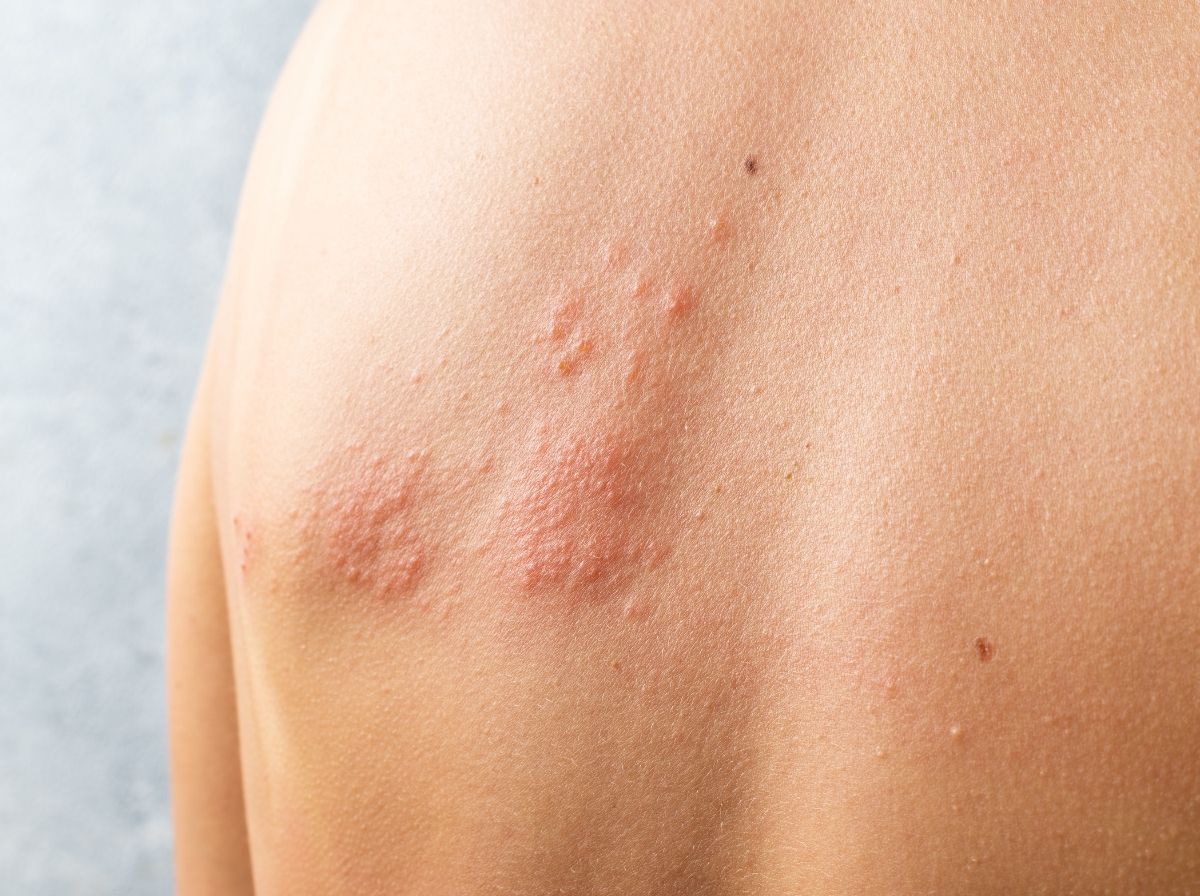
People are also reading: First Signs of Herpes, What You’ll Notice Early and What to Do Next
The Missing Test on Most “Full” STD Panels
When you ask for a full STD panel, the assumption is simple: everything gets checked. In reality, most panels are built around a specific group of infections that can be reliably detected early and treated immediately. That typically includes chlamydia and gonorrhea through NAAT testing, plus blood tests for HIV and syphilis.
Herpes testing works differently. Instead of detecting the virus directly in most cases, standard screening uses IgG antibody blood tests that measure your immune response. That response takes time to develop, and once it exists, it stays in your system indefinitely. So a positive result tells you that your body has encountered HSV-1 or HSV-2 at some point, not when it happened or where the infection is located.
This is why herpes becomes a blind spot. You can test negative for every infection on a standard panel and still carry HSV without knowing it. The absence of herpes in routine testing isn’t an oversight, it’s a deliberate decision based on how the biology of the virus interacts with current testing methods.
Why the Medical System Leaves Herpes Out
The decision to exclude herpes from routine screening comes down to how antibody testing behaves in real-world populations. IgG tests detect immune memory, not active infection. That creates two major issues: timing and interpretation.
After exposure, herpes antibodies typically become detectable from 6 weeks after exposure, but in some cases, they are only reliably detected closer to 12 weeks. During that window period, a test can return a false negative even if the virus is present in the body. On the other end, low-positive results can occur in people who have never had symptoms, especially with HSV-2, creating uncertainty about whether the result reflects a true infection.
Because of that, organizations like the CDC herpes guidelines and the USPSTF recommendation on HSV screening advise against routine testing in asymptomatic individuals. The concern is not that herpes is unimportant, but that unclear results can create confusion without changing medical management.
That said, the system is optimized for population-level outcomes, not individual clarity. And those are not always the same thing.
This Is Why So Many People Don’t Know They Have Herpes
Roughly 80% of people who carry herpes don’t know they have it, and the reason is not mysterious. It comes directly from how testing is handled. When a virus is not included in routine screening, and most infections don’t produce noticeable symptoms, the majority of cases will remain undiagnosed by default.
Herpes often stays under the radar because the virus can remain inactive in nerve cells for long periods, or cause symptoms so mild they are mistaken for something else like skin irritation, razor burn, or a small ingrown hair. Without targeted testing, there is no biological trigger that forces detection. The body does not “announce” HSV in a consistent or obvious way.
Now combine that with the fact that standard STD panels exclude herpes unless specifically requested. The result is predictable: people test regularly, receive negative results, and assume that includes HSV. It doesn’t. That gap between perceived testing and actual testing is exactly why such a large percentage of infections remain undiagnosed.
This is also why timing matters so much when you do choose to test. Because herpes relies on antibody detection, testing from 6 weeks after exposure provides the first reliable signal, and testing again at 12 weeks increases accuracy by confirming whether the immune response has fully developed.
Check Your STD Status in Minutes
Test at Home with RemediumGenital Herpes Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $45.99 $49.00
The Cost of Not Knowing Your Status
When herpes is excluded from testing, the immediate result is simple: people assume they are negative when they have never actually been tested. That misunderstanding changes how they approach new relationships, disclosure, and risk.
Herpes transmission often occurs during periods without visible symptoms because the virus can shed from the skin even when there are no lesions. Biologically, that happens because HSV resides in nerve cells and can reactivate intermittently, releasing viral particles without triggering noticeable inflammation. That means someone can pass the virus without realizing it.
The first time many people discover their status is either during a symptomatic outbreak or after a partner tests positive. At that point, the issue is not just medical, it becomes emotional and relational. The shock doesn’t come from the virus itself, but from the gap between what someone believed about their status and what is actually true.
When Herpes Testing Actually Makes Sense
Even though routine screening is not recommended for everyone, there are specific situations where herpes testing becomes medically useful and logically consistent with how the virus behaves.
If you have had sexual contact with a new or untested partner, testing should be timed based on how the immune system responds. For herpes, that means testing from 6 weeks after exposure provides the first meaningful antibody signal, while testing again at 12 weeks improves accuracy by allowing the immune response to fully develop.
Testing also makes sense when a partner has a confirmed HSV diagnosis, because it establishes whether transmission has already occurred. In this context, a type-specific IgG blood test helps clarify exposure history rather than diagnose a current outbreak.
For people who want a complete understanding of their sexual health status, at-home testing can provide that clarity without relying on whether a provider includes it. Options like the Herpes HSV-1 & HSV-2 rapid home test kit allow you to check your status directly, using the same antibody detection approach but on your own timeline.
| Infection | Why timing and test type matter in routine screening |
|---|---|
| Chlamydia | NAAT can detect the infection directly, which is why chlamydia: test from 14 days after exposure fits more easily into routine screening. |
| Gonorrhea | NAAT also detects gonorrhea directly, and gonorrhea: test from 3 weeks after exposure gives clinics a clearer early screening pathway. |
| Syphilis | Blood testing is standard, and syphilis: test from 6 weeks after exposure gives a defined point for follow-up screening. |
| HIV | Blood testing is widely standardized, and HIV: test at 6 weeks for first indicator, retest at 12 weeks for certainty is already built into screening logic. |
| Herpes HSV-1 and HSV-2 | Herpes relies on IgG antibody detection rather than routine direct screening, which is why herpes HSV-1 and HSV-2: test from 6 weeks after exposure requires more careful interpretation. |
| Hepatitis B | Blood testing is standard, and hepatitis B: test from 6 weeks after exposure fits established screening workflows. |
| Hepatitis C | Blood testing is also standard here, with hepatitis C: test from 8–11 weeks after exposure used to guide accurate follow-up. |
At-Home Herpes Testing: How the Rapid Test Actually Works
At-home herpes tests work on the same fundamental principle as any other test, which is based on the presence of IgG antibodies developed by your immune system in response to the presence of HSV-1 or HSV-2. These are not the viruses; they are simply proof that your immune system has seen the viruses and reacted accordingly.
The test is quite simple. A small sample of blood is drawn, usually by pricking your finger, which is then placed on a test cassette. This test cassette contains chemicals that specifically bind to IgG antibodies for both HSV-1 and HSV-2. If the antibodies are present, they will bind to the test strip, which will create a line.
The timing for herpes testing is the same at home as it is in any other medical facility. Herpes testing can be done at any time after 6 weeks from the time of infection, when IgG antibodies first appear in the bloodstream. Before this time, the test will come back negative because the immune system has had no time to produce any antibodies.
This is why herpes testing must be repeated. While the initial test after 6 weeks is the first indication of infection, repeating the test after 12 weeks is necessary because without it, the possibility remains that the initial infection was too early to have been detected.
What at-home tests offer is control. Instead of relying on whether herpes is included in a clinic panel, you can test on your own timeline, with the same antibody-based detection method used in standard laboratories. Options like the HSV-1 & HSV-2 rapid home test kit allow you to check your status discreetly and get results within minutes, without sacrificing accuracy when used within the correct testing window.

People are also reading: Thick Eye Discharge: How to Tell Pink Eye from Gonorrhea
The Real Problem Isn’t Herpes; It’s How the System Handles It
By now, the pattern is clear. Herpes is common, often asymptomatic, and biologically different from other STDs in how it is detected. But the real issue is not the virus itself, it is how the medical system chooses to handle it.
Routine screening is designed for clarity at scale. That means prioritizing infections where early detection leads to immediate treatment decisions and where test results are easy to interpret. Herpes does not fit neatly into that model. It relies on antibody detection, has a defined but delayed window period, and produces results that require context rather than a simple yes-or-no clinical action.
So instead of adapting the system to include that nuance, the system often excludes herpes entirely unless there is a visible reason to test. The result is a gap between what patients think is being tested and what is actually being tested. That gap is where confusion, miscommunication, and delayed diagnosis happen.
This is also where most misconceptions about herpes testing begin. People assume that a negative STD panel includes everything. It doesn’t. They assume doctors automatically test for what matters most. They don’t always. And they assume that if herpes were important enough, it would be included by default. That assumption is exactly what keeps so many people uninformed about their actual status.
Check Your STD Status in Minutes
Test at Home with RemediumGenital & Oral Herpes Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $75.00 $98.00
For all 2 tests
Common Misconceptions About Herpes Testing, And Why They Persist
One of the most persistent myths is the idea that herpes would have shown up on a standard STD test. It wouldn’t. Unless a herpes-specific antibody test was ordered, HSV-1 and HSV-2 are simply not part of routine screening panels.
Another common belief is that doctors automatically include every relevant test. In reality, providers follow guidelines designed to balance accuracy, cost, and clinical impact across large populations. That means patient preference and individual clarity do not always drive what gets included in a panel.
There is also the assumption that herpes testing is unnecessary because the infection is manageable. While it is true that herpes is not dangerous for most people, that has nothing to do with whether knowing your status matters. From a biological standpoint, HSV can still be transmitted without symptoms due to asymptomatic viral shedding, which makes awareness of status directly relevant to partner risk.
Finally, there is the belief that a positive result would automatically disrupt your relationships or sex life. In practice, most of the disruption comes from the shock of not knowing earlier. When people understand their status, transmission patterns, and options, herpes becomes something they manage, not something that defines them.
Common Misconceptions About Herpes Testing, And Why They Persist
Most confusion around herpes testing doesn’t come from the virus itself; it comes from assumptions about how STD testing works. When something is not routinely included in screening, people fill in the gaps with what they think should happen instead of what actually happens.
These misconceptions tend to stick because they feel logical. But once you look at how testing is actually structured, they start to fall apart quickly.
| Common belief | What is actually happening biologically and clinically |
|---|---|
| If I tested negative on a full STD panel, I don’t have herpes | Standard panels typically exclude HSV-1 and HSV-2 unless specifically requested. A negative result only reflects the infections that were actually tested, not herpes status. |
| If herpes mattered, doctors would automatically test for it | Screening guidelines prioritize infections with clear treatment pathways and straightforward detection. Herpes relies on antibody timing and interpretation, which is why it is often excluded from routine panels. |
| I would know if I had herpes because I would have symptoms | HSV can remain inactive in nerve cells or cause symptoms so mild they are misidentified. Asymptomatic viral shedding allows transmission without noticeable signs. |
| A positive test means I have an active infection | IgG blood tests detect past exposure, not active outbreaks. The result reflects immune memory, not current symptom status or timing of infection. |
| If I test negative once, I’m in the clear | If testing occurs before antibodies are detectable, the result can be a false negative. Testing from 6 weeks after exposure provides the first reliable signal, with confirmation at 12 weeks. |
The reason these misconceptions persist is simple: the system does not clearly communicate what is and is not included in testing. So people rely on assumptions that feel reasonable but don’t match how the biology and testing methods actually work.
Once you understand that herpes testing is separate, time-dependent, and antibody-based, the confusion disappears. What replaces it is a much more accurate question: not “Was I tested?”, but “Was I tested for herpes, at the right time?”
What Taking Control Actually Looks Like
Once you understand how herpes testing works, the next step is not complicated, but it does require being intentional. Testing should be based on exposure timing, not assumptions about what was included in a previous panel.
If you have had sexual contact with a new or untested partner, the correct approach is to align testing with the antibody window. Testing from 6 weeks after exposure provides the first reliable indication of HSV antibodies, and repeating the test at 12 weeks confirms whether the immune response is fully detectable. That two-step approach removes most of the uncertainty that comes from testing too early.
This same principle applies whether you are testing through a provider or using an at-home option. The difference is not in the biology, it is in control. When you choose to test intentionally, using options like the HSV-1 & HSV-2 rapid home test kit, you are no longer dependent on whether herpes is included in a standard panel.
For broader screening, especially if you want to remove uncertainty across multiple infections at once, a comprehensive option like the Complete STD home test kit package includes herpes alongside other major STDs, closing the gap that standard panels often leave open.
At that point, the situation changes completely. You are no longer guessing based on incomplete testing. You are working with actual data, aligned with how your body responds to infection, and making decisions from a position of clarity instead of assumption.

People are also reading: Is Discharge Without Pain a Sign of an STD?
If Your Doctor Won’t Test You, Here’s What to Do
At some point, a lot of people run into the same situation: they ask to be tested for herpes, and the answer is hesitation, pushback, or a flat-out no. That response is not random. It reflects how current screening guidelines are designed, but it does not mean testing is off the table.
If a provider declines to order a herpes test, the first step is to be specific. Request a type-specific IgG blood test for both HSV-1 and HSV-2. This matters because general or non-type-specific tests do not provide clear or useful results. Being precise about the test removes part of the ambiguity that leads to pushback.
If the answer is still no, the situation becomes straightforward. You are not required to rely on a single provider’s decision to understand your own health status. At that point, using an at-home option becomes the most direct path forward.
By using a rapid at-home test, you’re employing the same basic technology of antibody detection. The main difference is the timing. Instead of waiting to see if the testing facility offers the test in their panel of services, the key to using the rapid at-home test is the timing. The first indication of the body responding to the exposure occurs at the 6-week mark. The second indication of the body responding to the exposure occurs at the 12-week mark.
Options like the HSV-1 & HSV-2 rapid home test kit or the Genital HSV-2 rapid test allow you to test on your own timeline, without waiting for approval or navigating unclear testing panels.
This is where control shifts. Instead of asking whether herpes was included, you are making sure it is. Instead of relying on assumptions, you are working with actual results. And instead of leaving gaps in your testing, you are closing them intentionally.
FAQs
1. Why is herpes not included in standard STD testing?
Herpes testing is based on antibody testing, not direct testing for the virus. Antibody testing is less clear in people without symptoms.
2. Can I get tested for herpes even without symptoms?
Yes. You can ask for a type-specific IgG test for HSV-1 and HSV-2, or use an at-home test for the same antibodies.
3. How long after exposure can I get tested for herpes?
Testing at least 6 weeks after exposure is the first indication of the immune system's response to the herpes virus. Testing at 12 weeks after exposure will confirm the immune response is fully developed.
4. What does a negative herpes test mean?
A negative test means no antibodies have been detected at the time of testing. This could mean the test was performed too early after exposure, so the body has not yet developed antibodies, resulting in a false negative.
5. What does a positive herpes test mean?
A positive test for IgG means the body has developed antibodies for HSV-1 or HSV-2 at some time in the past. It does not mean the body is currently infected or when the infection occurred.
6. Can herpes be transmitted without symptoms?
Yes. This is possible because the virus on the skin surface will periodically reactivate and thus be transmitted even without the manifestation of symptoms.
7. What’s the difference between HSV-1 and HSV-2?
HSV-1 has a tendency to affect the mouth, while HSV-2 has a tendency to affect the genital area. However, the virus can affect the mouth or the genital area regardless of the type.
8. Are at-home herpes tests accurate?
If the tests are conducted within the appropriate time window, the accuracy of the results will be the same as those obtained in a clinical setting using a blood test.
9. Why do I need to retest at 12 weeks?
This is because the antibodies take time to build up. Retesting in the 12th week ensures the antibodies have had time to build up and thus the results will be accurate.
10. Can I request herpes testing even if my doctor says no?
Yes. You have the right to ask to be tested for the virus.
Take Control of Your Testing, Don’t Leave It to Assumptions
If herpes is not included in routine panels, the only way to know your status is to test for it intentionally. That means choosing the right test, timing it correctly, and making sure nothing is left out.
You can start with a targeted option like the HSV-1 & HSV-2 rapid home test kit, or use a broader panel like the Complete 7-in-1 STD home test kit to check multiple infections at once.
If you want to explore all available options, visit the STD Rapid Test Kits homepage and choose the test that fits your timeline and level of certainty.
Testing is not about panic. It is about clarity. And clarity is what allows you to make informed decisions about your health, your partners, and your next steps.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC, Genital Herpes Fact Sheet
2. USPSTF, Genital Herpes Screening Recommendation
3. WHO, Herpes Simplex Virus Overview
4. NCBI, HSV Epidemiology and Transmission
5. CDC, STI Treatment Guidelines: Herpes
6. NCBI, Herpes Simplex Virus Serologic Testing
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: STD Rapid Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.