Quick Answer: Symptoms after condom sex can still happen because condoms don’t protect against all infections, irritation and allergies are common, and some STDs may already have been present before sex.
This Is the Part Nobody Explains About “Safe Sex”
There’s a quiet assumption baked into sex education: use a condom, and you’re covered. And yes, condoms dramatically reduce risk. But they don’t create a force field around your entire genital area. Skin still touches skin. Fluids can still get close to areas not covered. And your body can still react in ways that have nothing to do with infection.
A lot of people only realize this after the fact. One person described it like this: “I kept thinking, this doesn’t make sense. We used protection. So why do I feel anything at all?” That confusion is valid, but it’s also where misinformation starts creeping in.
So before jumping to worst-case scenarios, it helps to understand the main categories of what’s actually happening when symptoms show up after protected sex.
What Your Body Might Be Reacting To (And What It Means)
Not all post-sex symptoms point to the same cause. In fact, most fall into a few predictable buckets, some harmless, some worth testing, none worth ignoring.
| Cause | What It Feels Like | When It Shows Up | Risk Level |
|---|---|---|---|
| Friction / irritation | Burning, soreness, redness | Same day or next day | Low |
| Latex or lube reaction | Itching, swelling, rash | Within hours | Low |
| Pre-existing STD | Discharge, pain, irritation | Days later | Moderate |
| Skin-to-skin STD | Sores, bumps, lesions | Days to weeks | Moderate |
The key takeaway here is timing and type of symptom. A burning sensation right after sex tells a very different story than a sore that appears a week later. Your body gives clues, you just need to know how to read them.
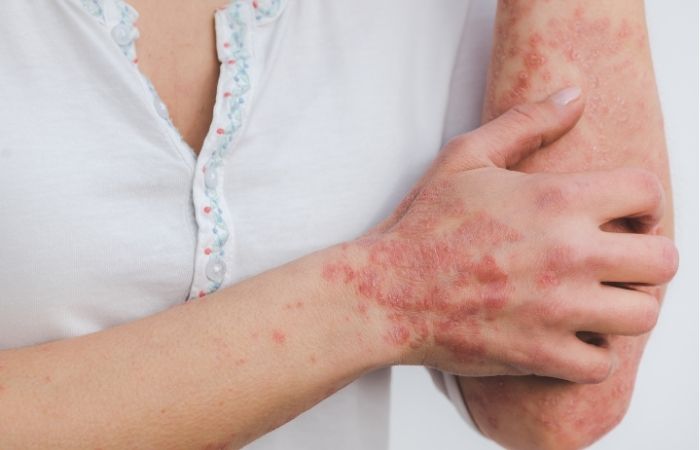
People are also reading: Rash After Sex: STD, Allergy, or Something Else?
Sometimes It’s Not an STD at All (And That’s More Common Than You Think)
Let’s start with the least scary, but most overlooked, cause: irritation. Sex, even good sex, is still friction. If there wasn’t enough lubrication, or if things lasted longer than usual, your skin can get inflamed. That can feel like burning or sensitivity, especially during urination afterward.
Then there’s the material itself. Latex condoms are safe for most people, but not everyone. Some bodies react subtly, just a little itch or warmth. Others react more dramatically, with visible redness or swelling. Add in flavored or scented lubricants, and suddenly your skin is dealing with chemicals it didn’t ask for.
One patient once said, “It felt exactly like an infection. I was convinced. Turned out I just needed a different brand of condoms.” That happens more often than people realize.
These reactions usually improve within a couple of days. If symptoms fade instead of worsen, that’s a strong sign you’re dealing with irritation, not infection.
But Yes, You Can Still Get an STD With a Condom
This is the part people don’t like hearing, but it’s important: condoms reduce risk significantly, but they don’t eliminate it entirely. Especially when it comes to infections that spread through skin contact.
Conditions like herpes, HPV, and syphilis don’t require fluid exchange. They spread through contact with infected skin, areas a condom might not cover. That includes the base of the genitals, surrounding skin, or even thighs during close contact.
That doesn’t mean condoms “don’t work.” They absolutely do. They just aren’t a full-body barrier.
There’s also real-world use to consider. Condoms can slip, shift, or be put on slightly late. None of this means you did anything wrong, it just means biology isn’t perfect.
The Timing Trap: Why Symptoms Don’t Always Mean What You Think
Here’s where anxiety tends to spike: symptoms show up, and your brain immediately connects them to the last sexual encounter. But the body doesn’t always work on that timeline.
| Timing | Most Likely Explanation |
|---|---|
| Within 24 hours | Friction or allergic reaction |
| 2–5 days later | Possible bacterial infection like chlamydia or gonorrhea |
| 1–3 weeks later | Possible herpes or syphilis symptoms |
This is where people get misled. You might feel symptoms days after condom sex and assume that moment caused it. But infections like chlamydia can exist quietly before that encounter and only become noticeable later.
In other words, timing can trick you into blaming the wrong event.
What You Should Actually Do Next (Without Spiraling)
First, pause the panic. Not every symptom equals a diagnosis. But don’t ignore your body either.
If symptoms are mild and fade quickly, it’s reasonable to monitor. If they persist, worsen, or include things like discharge, sores, or pain when urinating, it’s time to get clarity.
You don’t need to wait in uncertainty. You can start with a discreet, at-home option like a STD rapid test kit, which allows you to check for common infections without the stress of a clinic visit.
If you want broader coverage, a combo STD home test kit can screen for multiple infections at once, especially helpful if you’re not sure what you’re dealing with.
One person put it simply: “The worst part wasn’t the symptoms. It was not knowing.” Testing replaces that uncertainty with facts.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
When It Feels Like Something More Than Irritation
There’s a difference between your body being a little irritated and your body trying to tell you something is off. The tricky part is that early STD symptoms can feel subtle, almost easy to dismiss if you’re hoping it’s nothing.
If what you’re feeling is persistent, specific, or getting worse instead of better, it’s worth paying closer attention. Not in a panic way, just in a grounded, informed way.
People often describe that moment as a shift. “At first I thought it was just soreness. But by day three, it didn’t feel normal anymore.” That’s usually your cue to stop guessing and start getting answers.
Symptoms That Deserve a Second Look
Some symptoms are more likely to point toward an infection rather than simple irritation. These don’t mean you definitely have an STD, but they do mean it’s time to take things seriously.
| Symptom | Why It Matters |
|---|---|
| Unusual discharge | Common with chlamydia or gonorrhea |
| Pain when urinating | Often linked to bacterial infections |
| Sores or blisters | Can indicate herpes or syphilis |
| Persistent itching (days) | Less likely to be simple friction |
| Pelvic or testicular pain | Possible deeper infection |
If you’re scanning that table and recognizing something, don’t jump to conclusions, but don’t ignore it either. This is where testing becomes less of a “maybe” and more of a smart next step.
The Mental Spiral Is Real, Here’s How to Stay Grounded
Let’s talk about the part no one puts in medical guides: the mental side of this. The moment you notice symptoms after sex, even protected sex, your brain can go into overdrive. You replay everything. You question every detail. You start googling things at 2 a.m. that only make you more anxious.
That spiral is incredibly common. It doesn’t mean something is seriously wrong, it means you’re human and trying to make sense of uncertainty.
One person described it like this: “I went from ‘it’s probably nothing’ to diagnosing myself with everything in one night.” That jump is fueled by fear, not facts.
What actually helps is shifting from guessing to clarity. Symptoms alone are not a reliable diagnosis. Even doctors don’t rely on symptoms alone, they test.
Why Waiting Too Long Can Make Things More Confusing
There’s a temptation to wait it out. To see if symptoms disappear. To hope your body just “fixes it.” And sometimes, yes, if it’s irritation, it will resolve on its own.
But if it’s an infection, waiting can do two things: it can prolong symptoms, and it can make timelines harder to interpret. You lose the ability to clearly connect exposure, symptoms, and testing windows.
This is especially true for infections that can be silent at first. By the time symptoms become obvious, the infection may have already been present longer than you think.
Getting tested early doesn’t just give you answers, it gives you a timeline you can actually trust.
Testing Without the Awkwardness (And Why More People Are Choosing It)
Let’s be honest: for a lot of people, it’s not the test itself that’s the barrier, it’s everything around it. The waiting room. The conversations. The feeling of being judged, even when no one is actually judging you.
That’s why at-home testing has become such a game-changer. It removes the social friction and replaces it with something simple: privacy and control.
With a discreet at-home STD test, you can check what’s going on without turning it into a whole event. No waiting rooms. No awkward explanations. Just information.
And if you're not sure what's wrong, like itching, mild burning, or something that just doesn't feel right, a broader option like a combo STD test kit can help you check for a lot of things at once.
This isn’t about assuming the worst. It’s about removing uncertainty so you can move forward, whether that means relief or treatment.
People are also reading: I Thought I Was Fine, Until It Burned to Pee
The Truth Most People Learn the Hard Way
Condoms are one of the best tools we have in sexual health. They prevent countless infections and give people real control over their risk. But they’re not a guarantee of zero symptoms, and they’re not meant to be.
The real goal isn’t perfection, it’s awareness. Knowing that symptoms can still happen. Knowing the difference between irritation and infection. Knowing when to wait, and when to act.
Because the people who handle this best aren’t the ones who never have symptoms. They’re the ones who know what to do when they do.
So… Was It the Condom, the Sex, or Something Else?
By this point, you’ve probably realized something important: symptoms after condom sex don’t come from one single cause. It’s rarely as simple as “it worked” or “it failed.” Most of the time, it’s a mix of biology, timing, and how your body reacts to what just happened.
And that’s where people get stuck. Not because the situation is dangerous, but because it’s unclear. Uncertainty is what makes everything feel worse than it actually is.
One person summed it up perfectly: “I didn’t even care what it was anymore, I just wanted to know.” That’s the shift. Moving from fear to clarity.
What People Often Misinterpret (And Why It Causes So Much Stress)
There are a few patterns that come up again and again. Misinterpretations that turn manageable situations into full-blown anxiety spirals.
One of the biggest is assuming that timing equals cause. It makes sense to blame that encounter if symptoms appear after having sex with a condom. But infections don't follow emotional logic; they follow biological timelines.
Another common trap is assuming all symptoms mean the same thing. A mild burn, a rash, a bump, these can come from completely different causes, many of which are harmless.
And then there’s the “I used protection, so this shouldn’t be happening” belief. When reality doesn’t match that expectation, it creates confusion and fear. Not because something terrible happened, but because no one explained the nuance.
How to Read Your Body Without Jumping to Worst-Case Scenarios
Your body isn’t trying to scare you, it’s giving you data. The goal isn’t to panic or ignore it. It’s to interpret it correctly.
If symptoms are mild, short-lived, and improving, your body is likely recovering from irritation or sensitivity. That’s a normal response, especially if sex was intense, longer than usual, or involved new products.
If symptoms are specific, persistent, or evolving, like discharge, sores, or increasing discomfort, your body is asking for attention. Not panic. Just attention.
This is where people often wish they had a simple rulebook. But the closest thing to that is this: patterns matter more than isolated symptoms.
A single sensation doesn’t tell the full story. But how it behaves over time? That’s where clarity starts to form.
You’re Not “Overreacting”, You’re Responding to Uncertainty
There’s a subtle kind of shame that shows up in situations like this. People think, “Maybe I’m overthinking it.” Or worse, “I shouldn’t be worried because we used a condom.”
But worry isn’t the problem. Staying stuck in uncertainty is.
You’re allowed to want answers. You’re allowed to check what’s going on in your own body. That’s not anxiety, that’s self-awareness.
And the truth is, most people who take that step feel better quickly, not because something was wrong, but because they stopped guessing.
Check Your STD Status in Minutes
Test at Home with Remedium8-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $149.00 $392.00
For all 8 tests
The Quiet Confidence That Comes From Knowing
There’s a noticeable shift that happens once you replace assumptions with facts. Whether the result is negative or something that needs treatment, the emotional weight drops almost immediately.
Because the hardest part of this experience isn’t usually the outcome, it’s the unknown.
Getting tested, especially early, gives you something solid to work with. It turns a vague situation into a clear one. And from there, everything becomes more manageable.
That’s the part people don’t talk about enough: clarity isn’t just medical, it’s emotional.
What This Really Comes Down To
You can use a condom and still feel symptoms. That doesn’t mean you failed. It doesn’t mean something serious happened. It means your body reacted, and now you have a chance to understand why.
Sometimes it’s friction. Sometimes it’s sensitivity. Sometimes it’s timing. And yes, sometimes it’s an infection that needs attention.
But in every case, the next step is the same: stop guessing, and get clear.
Because once you know what’s actually going on, everything else, treatment, relief, peace of mind, falls into place.
FAQs
1. Wait… so I used a condom and I can still get an STD?
Yeah, uncomfortable truth, but yes. Condoms do a really good job, especially for fluid-based infections, but they don’t cover everything. If skin outside the condom comes into contact, like with herpes or HPV, there’s still a small window for transmission.
2. It burns a little after sex, did I mess up?
Probably not. That light burning feeling right after sex is super common and usually comes down to friction, especially if things got a little intense or dry. If it chills out within a day or two, your body’s just recovering, not sending you a diagnosis.
3. Why does it itch after using a condom? That feels… suspicious.
Totally get why your brain goes there. But itching is often your skin reacting, not an infection announcing itself. Latex, lube, even friction can trigger that “something’s off” feeling, especially if your body’s sensitive.
4. How do I know if it’s irritation or something real?
Look at the pattern, not just the symptom. Irritation shows up fast and fades. Infections tend to stick around, evolve, or come with extras, like discharge, pain when peeing, or visible sores. If it’s lingering or escalating, that’s your sign to check it out.
5. The condom didn’t break though… so why am I dealing with this?
Because “didn’t break” doesn’t mean “nothing happened.” Condoms reduce risk, they don’t erase it. Also, not everything you feel after sex is about infection. Sometimes your body’s just reacting to the experience itself.
6. Could I have already had something before this?
Honestly? That’s very possible. A lot of STDs don’t show symptoms right away, so they kind of sit quietly until something triggers your awareness. Then it feels like it came from the most recent hookup, even if it didn’t.
7. I feel weird, but not “sick.” Do I still need a test?
If your gut is nudging you, it’s worth listening. You don’t need dramatic symptoms to justify testing. A quick check can either rule things out or catch something early, both are wins.
8. How long should I wait before I actually test?
Timing matters more than people think. Some infections show up in a few days, others take a couple of weeks to be detectable. If you’re unsure, testing now and retesting later is a smart, low-stress approach.
9. Is it bad if I keep having sex while I’m not sure?
It’s not about “bad”, it’s about risk. If something’s unclear, pressing pause protects both you and your partner. Once you know what’s going on, you can move forward without that question hanging over you.
10. Be honest, am I overthinking this?
You’re not overthinking, you’re reacting to uncertainty. Big difference. Most people in your position would feel the same way. The goal isn’t to shut that feeling down, it’s to replace it with actual answers.
You Deserve Clarity, Not Guesswork
You used a condom. That matters. But your body still felt something, and now you’re stuck in that weird space between “it’s probably nothing” and “what if it’s not?” That tension? That’s what actually makes this stressful, not the symptom itself.
The goal isn’t to panic over every itch or sensation. It’s to figure out what deserves attention and what doesn’t. If symptoms fade quickly, your body likely just needed a reset. If they stick around, evolve, or feel off in a way you can’t ignore, that’s your cue to stop guessing and get clarity.
Don’t wait and wonder. If there’s even a small chance something’s going on, start with a discreet screen like the Combo STD Home Test Kit. No awkward conversations. No second-guessing. You can move on without that question hanging over you now that you have real answers.
How We Sourced This Article: We built this guide using a mix of medical research, public health guidance, and real-world symptom patterns people report every day. That includes how condoms actually perform, how infections spread, and why your body might react after sex, even when you did everything “right.”
Sources
1. Centers for Disease Control and Prevention – STD Prevention
2. World Health Organization – Sexually Transmitted Infections Fact Sheet
3. Mayo Clinic – STD Symptoms and Causes
5. Planned Parenthood – STDs and Safer Sex
6. National Institutes of Health – STI Research Database
About the Author
Dr. F. David, MD is a board-certified infectious disease doctor who specializes in preventing, diagnosing, and treating STIs. His direct, sex-positive style puts privacy, patient empowerment, clinical accuracy, and clarity at the top of the list.
Reviewed by: Dr. Samuel Ortega, MD | Last medically reviewed: March 2026
This article is meant to give you information, not medical advice.










