Quick Answer: Throat STD testing is usually done with a simple throat swab that collects cells from the back of the throat. Doctors test that sample for infections like gonorrhea and chlamydia using lab analysis. Many routine STD screenings do not include throat testing unless you specifically request it.
The STD That Lives Quietly in the Throat
One of the biggest misunderstandings about sexually transmitted infections is that they always cause obvious symptoms. In reality, throat infections are often silent. You could carry oral Gonorrhea or Chlamydia for weeks, or even months, without feeling anything unusual.
Doctors call these infections “oropharyngeal STIs,” meaning the bacteria live in the throat rather than the genitals. They’re usually transmitted through oral sex, although rarely they can also spread through deep kissing if sores or infections are present.
A patient once described it this way during a clinic visit:
“I thought I just had seasonal allergies. I only tested because my partner tested positive for gonorrhea. I had zero symptoms.”
This scenario is incredibly common. According to public health research, throat infections often go unnoticed because the throat doesn’t always react strongly to these bacteria.
Even when symptoms do appear, they tend to mimic ordinary illnesses:
| Symptom | How Common It Is | What It Can Feel Like |
|---|---|---|
| Sore throat | Occasional | Scratchy or irritated throat similar to mild strep |
| Swollen lymph nodes | Uncommon | Tender glands under the jaw |
| Redness in the throat | Sometimes | Inflamed throat seen during examination |
| No symptoms at all | Very common | Many people feel completely normal |
Because these symptoms overlap with everyday illnesses, doctors rarely diagnose throat STDs based on symptoms alone. Testing is the only reliable way to know.
How Doctors Actually Test the Throat for STDs
When people imagine STD testing, they usually picture blood tests or urine samples. Those tests work well for many infections, but they don’t always detect bacteria living in the throat.
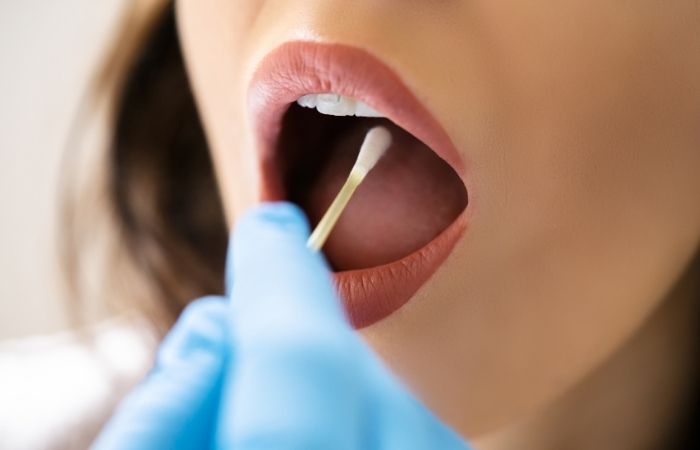
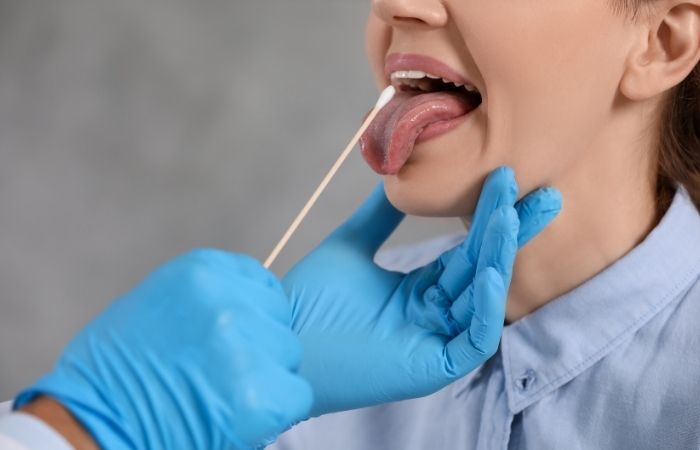
Instead, clinicians rely on a simple procedure called a throat swab.
The process doesn't take long, and most people say it feels like a strep test. A clean cotton swab gently touches the back of the throat and tonsils to get cells and fluid. Then, the sample is sent to a lab where molecular testing methods are used to find bacterial DNA.
In most clinics, the entire swabbing process takes less than ten seconds.
One sexual health nurse explained it this way:
“People expect something invasive, but it’s literally the same kind of swab we use to check for strep throat. It’s fast and painless.”
Once the sample reaches the lab, it’s typically tested using a method called a nucleic acid amplification test (NAAT). This technology looks for tiny fragments of bacterial genetic material and is extremely sensitive.
| Test Type | How It Works | What It Detects |
|---|---|---|
| Throat swab (NAAT) | Collects cells from throat and analyzes bacterial DNA | Gonorrhea, chlamydia |
| Culture test | Grows bacteria in a lab sample | Gonorrhea confirmation |
| Blood test | Detects antibodies | Syphilis, HIV (not throat-specific) |
Because throat infections are location-specific, doctors often recommend testing multiple body sites when someone may have been exposed.
That means screening might include samples from the throat, genitals, and rectum depending on the type of sexual contact.
People are also reading: Most People With an STD Don’t Feel Sick, Here’s Why
The Thing Most STD Tests Don’t Tell You
A common misconception is that “getting tested for everything” automatically includes the throat. In reality, many routine STD panels only test urine or genital samples unless a throat swab is specifically requested.
This can lead to missed infections.
A sexual health physician once shared a conversation that happens frequently in clinics:
“Patients say they were tested recently and everything was negative. Then we ask if a throat swab was done, and the answer is almost always no.”
This matters because infections can exist in one location but not another. Someone could test negative in a urine test yet still have oral gonorrhea.
Public health experts refer to this as “extragenital testing,” meaning testing areas outside the genitals where infections can hide.
Throat screening is particularly important for people who have oral sex with multiple partners or who are part of communities where extragenital infections are more common.
If you’re unsure whether your last STD test included the throat, it’s perfectly reasonable to ask your healthcare provider directly. Many clinics will add the swab immediately if there’s any potential exposure.
Can You Test for a Throat STD at Home?
Clinic testing remains the gold standard, but at-home testing options have expanded dramatically in recent years. Many modern testing kits allow users to collect their own samples and send them to a laboratory.
The biggest difference is that some kits rely on urine samples, while others include swabs for throat or rectal testing.
This method can make it easier for people who want privacy or convenience to take tests.
A college student once explained why he chose a home kit:
“I wasn’t embarrassed about testing, I just didn’t want to sit in a waiting room for two hours. Doing it at home felt simpler.”
If you’re exploring this option, it’s important to choose a reputable test provider that uses certified laboratories. You can learn more about available testing options on the STD Rapid Test Kits homepage, which explains different types of at-home tests and how they work.
Some kits, like the Combo STD Home Test Kit, check for more than one infection at a time. These kits put together a number of screenings into one package. These can be helpful for people who want to get a general idea of their sexual health after getting a new partner.
The key thing to remember is that not all home tests include throat swabs. If oral exposure is a concern, the testing kit must specifically include a swab designed for throat sampling.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
Timing Matters: When to Test After Oral Sex
Another common question is when throat STD testing should happen after possible exposure. Testing too early can sometimes produce false negatives because the bacteria haven’t multiplied enough to be detected.
Doctors refer to this delay as the “window period.”
| Infection | Earliest Reliable Test | Best Testing Window |
|---|---|---|
| Gonorrhea | 3–5 days | 1–2 weeks |
| Chlamydia | 5–7 days | 1–2 weeks |
| Syphilis (oral lesions) | 3 weeks | 4–6 weeks |
If symptoms appear sooner, like severe throat pain or unusual lesions, doctors usually recommend testing immediately.
But in many cases, people test simply because they want peace of mind after a new partner or unprotected oral sex. Waiting about a week after exposure generally produces more accurate results for bacterial infections.
What Happens If a Throat STD Test Is Positive?
Finding out you have an infection in your throat can feel unsettling at first. But the good news is that the most common throat STDs are treatable.
Most of the time, doctors give people antibiotics to treat gonorrhea. Most of the time, you get these as an injection and then take them by mouth. People usually take oral antibiotics for a few days to get rid of chlamydia.
Most of the time, doctors tell patients not to have sex until their treatment is over. They may also tell them to take the test again to make sure the infection is gone.
Partner notification is also important. That conversation can feel awkward, but it’s a critical step in preventing reinfection and protecting others.
A physician who works in sexual health clinics put it simply:
“Most people assume oral sex is lower risk, but bacteria don’t really care where they live. The good news is we can detect and treat these infections easily once people know to test.”
People are also reading: Can You Tell If Someone Has an STD Just by Looking?
Which STDs Can Actually Infect the Throat?
When people hear “throat STD,” they often assume there must be dozens of possibilities. In reality, only a handful of infections regularly show up in the throat. Two bacteria dominate the conversation: Gonorrhea and Chlamydia.
Both infections can settle into the tissues at the back of the throat after oral sex with an infected partner. The bacteria attach to mucous membranes and quietly replicate there, often without causing obvious symptoms. Because the throat has a different immune environment than genital tissue, infections sometimes stay mild or invisible.
That doesn’t mean they’re harmless. Even without symptoms, these infections can still spread to partners or move to other parts of the body through sexual contact.
| Infection | How It Reaches the Throat | Typical Symptoms | Testing Method |
|---|---|---|---|
| Gonorrhea | Oral sex with an infected partner | Often none, sometimes sore throat or redness | Throat swab (NAAT test) |
| Chlamydia | Oral contact with infected genital tissue | Usually no symptoms | Throat swab or lab analysis |
| Syphilis | Contact with sores during oral sex | Painless lesions or ulcers in mouth | Blood test and lesion swab |
| Herpes (HSV-1 or HSV-2) | Kissing or oral contact with active sores | Cold sores, mouth ulcers | Swab of lesion or blood test |
In practice, most throat screenings focus primarily on gonorrhea and chlamydia because they are both common and easy to miss. Viral infections like herpes or syphilis tend to show clearer physical signs such as sores or lesions, which usually prompt testing right away.
The important takeaway is that throat infections exist on a spectrum. Some cause visible symptoms, others remain silent. Testing fills the gap between those two realities.
Why Throat STDs Are So Easy to Miss
One of the most frustrating things about oral infections is how subtle they can be. Unlike genital infections, which sometimes cause discharge, pain, or burning, throat infections often blend into everyday sensations.
A mild scratchy throat might be written off as dehydration. Swollen glands might be blamed on a cold. Even doctors sometimes overlook throat STDs unless they know a patient has had oral exposure.
Part of the reason lies in how the throat works. The tissues in the oropharynx are always in contact with bacteria, bits of food, and things that cause irritation in the environment. Because of this, the immune system there is used to tolerating microbes rather than reacting dramatically to them.
That biological tolerance can allow infections like Gonorrhea to linger quietly.
Researchers studying sexual health clinics have found that a large percentage of throat infections are discovered only during routine screening rather than because someone noticed symptoms.
“Most people we diagnose had no idea anything was wrong,” one clinician explained. “They tested because a partner suggested it or because they were doing routine screening.”
This is why many modern sexual health guidelines recommend testing based on exposure rather than symptoms alone. If oral sex was part of the encounter, adding a throat swab simply closes a diagnostic blind spot.
Think of it less as assuming something is wrong and more as completing the full picture. When testing includes all possible exposure sites, results become far more reliable.
Check Your STD Status in Minutes
Test at Home with Remedium8-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $149.00 $392.00
For all 8 tests
Common Testing Mistakes That Can Lead to Missed Throat STDs
Most missed throat infections don’t happen because testing failed. They happen because the throat was never tested in the first place. This is one of the most common blind spots in sexual health screening.
Many people assume that if they “got tested for everything,” the throat must have been included. In reality, most standard panels rely on urine samples or genital swabs unless a provider specifically adds extragenital testing. If oral sex was involved, skipping the throat swab leaves a gap in the results.
Another issue is timing. Testing the day after a new encounter can feel reassuring, but infections need time to become detectable. The bacteria that cause Gonorrhea and Chlamydia usually need several days to multiply before laboratory tests can reliably detect them.
A sexual health nurse once explained it in practical terms:
“People want certainty immediately after exposure, which is completely understandable. But testing too early can give a false sense of security. Waiting about a week makes the results much more dependable.”
Self-collection errors can also affect results when testing at home. Throat swabs need to touch the back of the throat and tonsil area where bacteria typically live. A quick swipe along the tongue won’t collect the right cells for analysis.
Finally, people sometimes skip testing because they assume symptoms would be obvious if something were wrong. Throat infections challenge that assumption. Many people with oral gonorrhea or chlamydia feel perfectly normal.
The goal of testing isn’t to assume the worst. It’s simply to close the uncertainty gap. When testing includes the correct body sites and happens at the right time, results become far more meaningful, and a lot less stressful to interpret.
FAQs
1. Can you really get an STD in your throat from oral sex?
Yes. Bacteria like Gonorrhea and Chlamydia can live in the throat after oral sex with an infected partner. The tricky part is that most people feel completely normal, which is why throat infections often fly under the radar until someone gets tested.
2. If I had a full STD panel, wouldn’t that already check my throat?
Not necessarily. Many standard STD tests only use urine or genital swabs unless you specifically ask for throat testing. If oral sex was involved, it’s worth asking your provider directly, “Did we test my throat too?”
3. What does a throat STD test actually feel like?
It’s surprisingly boring, in a good way. A clinician swabs the back of your throat with a cotton tip, just like a strep test. The whole thing takes a few seconds, and most people say the worst part is the brief gag reflex.
4. I have a sore throat after oral sex. Should I panic?
Probably not. Most sore throats are caused by viruses, allergies, or dry air. But if the timing lines up with a new partner or exposure, testing is a smart move because throat STDs can occasionally cause irritation that feels similar.
5. How long should I wait before testing after oral sex?
About a week is usually a good window for bacterial infections like gonorrhea or chlamydia. Testing too early can miss an infection simply because the bacteria haven’t multiplied enough yet to show up in the lab.
6. Can you spread a throat STD to someone else?
Yes, it’s possible. Oral infections can pass to a partner’s genitals during oral sex. That's why doctors often tell people to stay away from sex until their treatment is over and their symptoms, if they had any, are gone.
7. Do throat STDs always cause symptoms?
No, and that’s what makes them sneaky. Many people with oral gonorrhea or chlamydia feel perfectly fine. Some only discover it after a partner tests positive or during routine screening.
8. Can at-home STD tests check the throat?
Some can, but not all. Kits that include a throat swab allow you to collect a sample yourself and send it to a lab. If oral exposure is part of your concern, make sure the test specifically mentions throat or “extragenital” testing.
9. What happens if a throat STD test comes back positive?
The good news is that antibiotics usually work for throat infections that are caused by bacteria. Your doctor will help you feel better, and they may want you to take another test later to make sure the infection is gone.
10. Is oral sex actually risky for STDs?
It’s lower risk than some forms of sex, but it’s definitely not risk-free. Bacteria and viruses don’t really care where they live, if they have a path to move between bodies, they’ll take it. Testing is simply the way we keep that reality from becoming a bigger problem.
You Deserve Clarity, Not Guesswork
A strange sore throat after a hookup can spiral quickly. Your brain runs through every possibility: allergies, a cold, maybe nothing at all. But sexual health works best when uncertainty gets replaced with information.
The reality is simple. Most throat infections from Gonorrhea or Chlamydia cause few symptoms, which is why testing matters more than speculation. A quick swab answers the question directly. No guessing, no late-night symptom spirals.
If recent oral sex leaves you wondering, start with a discreet screen like the Combo STD Home Test Kit. Your results are private. Your health decisions stay in your hands. And peace of mind beats uncertainty every time.
How We Sourced This Article: This article is based on current medical guidance for extragenital STD testing, peer-reviewed infectious disease research, and real-world experience from sexual health clinics. We examined studies on how doctors detect oropharyngeal gonorrhea and chlamydia, along with CDC screening recommendations and modern lab tests such as nucleic acid amplification tests (NAATs). Everything here is designed to keep the science accurate while explaining it in a way that’s clear, practical, and stigma-free.
Sources
1. Centers for Disease Control and Prevention – Gonorrhea Fact Sheet
2. Mayo Clinic: Symptoms and Causes of Gonorrhea
3. Planned Parenthood: Information about STDs and STIs
4. Fact Sheet on Sexually Transmitted Infections from the World Health Organization
5. Centers for Disease Control and Prevention – STI Screening Recommendations
6. Planned Parenthood – Gonorrhea Symptoms, Testing, and Treatment
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on sexually transmitted infection prevention, diagnosis, and treatment. His work emphasizes practical testing guidance, stigma-free sexual health education, and clear medical communication.
Reviewed by: Daniel K. Mercer, MD, Infectious Disease | Last medically reviewed: February 2026
This article is only for informational purposes and should not be used instead of professional medical advice, diagnosis, or treatment.










