Quick Answer: STD rashes usually develop days to weeks after exposure and may include sores, blisters, or systemic symptoms. Allergic rashes often appear quickly after contact with a product like latex, lubricant, or soap and typically improve once the irritant is removed.
Why So Many People Confuse Allergic Reactions With STDs
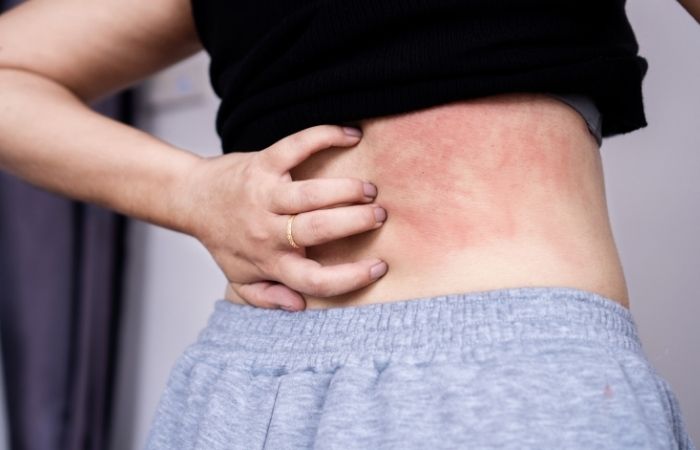
Skin is the body's first alarm system. When something irritates it, the reaction can look dramatic: redness, swelling, itching, bumps, or a burning sensation. Unfortunately, these same symptoms can also appear during early stages of certain sexually transmitted infections.
Dermatologists and sexual health clinicians see this confusion constantly. Someone notices irritation after sex and assumes infection. Another person ignores early STD symptoms because they think it's just a skin reaction. Both situations are common because the body only has a limited number of ways to signal that something is wrong.
There are three major reasons the two conditions get mixed up so often.
First, timing can overlap. An allergic reaction from a condom, lubricant, body wash, or spermicide may show up minutes or hours after exposure. But infections like Herpes or Syphilis may appear days later, which can make people connect symptoms to the wrong event.
Second, the genital area is sensitive. Friction, shaving, tight clothing, and moisture can all cause skin irritation that looks alarming even when it is harmless.
Third, online symptom searches tend to show worst-case scenarios. Someone types “rash after sex” into a search engine and suddenly every image looks like an infection.
The goal isn’t to panic or dismiss symptoms. It’s to understand how allergic reactions and infections behave differently.
What an Allergic Rash Usually Looks and Feels Like
An allergic rash happens when the immune system reacts to something that touched the skin. The trigger might be latex, lubricants, soaps, spermicides, fragrances, laundry detergents, or even certain fabrics.
In sexual health clinics, latex condom sensitivity is one of the most common triggers. People often discover it after switching condom brands or trying a product with new additives.
Unlike infections, allergic reactions tend to appear quickly after exposure. Many people notice itching, redness, or burning within minutes or a few hours after contact.
Another key feature is location. Allergic reactions usually appear exactly where the irritant touched the skin. If a condom caused the reaction, irritation may appear along the shaft of the penis or inside the vagina. If lubricant triggered it, redness might spread more broadly.
| Symptom | What It Often Feels Like | Typical Timing |
|---|---|---|
| Redness | Warm or flushed skin | Minutes to hours after contact |
| Itching | Persistent urge to scratch | Often begins quickly |
| Swelling | Mild puffiness in the affected area | Within hours |
| Small bumps or rash | Raised irritation patches | Within hours |
| Burning sensation | Stinging or irritation | Usually soon after exposure |
Most allergic reactions improve once the trigger disappears. Cleaning the area, staying away from the product, and giving the skin time to heal usually makes things better in one to three days.
However, if irritation continues for several days or worsens, it may not be a simple allergy. That is where testing and medical evaluation become important.
People are also reading: What to Order When You’re Not Sure: STD Tests by Situation
How STD Rashes Tend to Develop Differently
Sexually transmitted infections behave differently from allergic reactions because they involve microorganisms entering the body and multiplying. This process takes time, so symptoms don't usually show up right away after being exposed.
For example, early symptoms of Herpes often appear between two and twelve days after contact. Syphilis sores can appear about three weeks later. Chlamydia and gonorrhea are two other infections that may not cause a rash but can cause discharge, burning when you pee, or pain in the pelvic area.
Skin symptoms caused by STDs also tend to have patterns that allergic reactions don't usually have.
| Possible Symptom | Why It Matters |
|---|---|
| Blisters or fluid-filled sores | Common in herpes outbreaks |
| Painless ulcers | Often linked to syphilis |
| Clusters of sores | Instead of an allergy, suggest a viral infection. |
| Flu-like symptoms | Some infections make you tired or give you a fever. |
| Symptoms lasting longer than a week | Allergic reactions typically subside more quickly. |
Another clue is progression. Rashes from allergies usually stay the same for a while and then go away. Symptoms of STDs often change over time. A small irritation could turn into blisters, ulcers, or scabs over the course of a few days.
When symptoms change like that, clinicians begin thinking about infection rather than irritation.
If you're unsure, discreet testing can provide clarity. Many people choose a private option such as an at-home STD testing kit, which allows them to check for common infections without scheduling a clinic visit.
Knowing your status removes guesswork. And when symptoms are ambiguous, guessing is rarely helpful.
Timing Tells a Story: When Allergic Reactions Appear vs STD Symptoms
If there is one clue clinicians rely on more than anything else, it is timing. The human body reacts to allergens almost immediately, while infections take time to develop. That difference is often the first sign of what might be going on.
When the immune system sees something as irritating, it releases inflammatory chemicals like histamine. This is what happens during an allergic reaction. This reaction can happen a few minutes or a few hours after being exposed. A lot of people notice that their skin is itchy or red before they even get out of bed.
Sexually transmitted infections follow a different biological timeline. Bacteria or viruses must first enter the body, replicate, and trigger an immune response. That process creates what doctors call an incubation period. During this time, a person can have no visible symptoms at all.
| Condition | When Symptoms Usually Appear | Typical Pattern |
|---|---|---|
| Allergic reaction (latex, lubricant, soap) | Minutes to a few hours after contact | Sudden itching, redness, irritation |
| Herpes | 2–12 days after exposure | Blisters, sores, or tingling sensations |
| Syphilis | 10–90 days after exposure | Painless ulcer or sore |
| Chlamydia | 1–3 weeks after exposure | Often mild or no symptoms |
| Gonorrhea | 2–10 days after exposure | Discharge, burning urination |
Understanding this timeline helps many people rule things out. If irritation started within an hour of trying a new lubricant or condom, an allergic reaction becomes much more likely. If symptoms appear several days after sexual contact, infection moves higher on the list of possibilities.
Still, timing alone cannot confirm the cause. Some allergic reactions are delayed, and some infections stay silent for weeks.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
Situations Where People Commonly Misread Symptoms
Sexual health clinics often hear the same kinds of stories. The symptoms are real, but the interpretation is wrong because the trigger isn't obvious at first.
Consider what happened to Daniel, a 28-year-old who noticed redness and itching the morning after sex with a new partner. His first thought was that he had picked up an infection.
“I woke up the next day and everything felt irritated,” he explained later. “I spent hours looking at STD pictures online and convinced myself something was wrong.”
After a clinic visit, the explanation turned out to be much simpler. The irritation was caused by a scented lubricant his partner had recently purchased. Once he stopped using it, the symptoms disappeared within two days.
Another situation happens in the opposite direction. Someone assumes their rash is harmless irritation and delays testing.
Ana, 31, initially believed she had a reaction to a new body wash after noticing small sores several days after sex.
“I thought maybe it was shaving or soap,” she later said. “But the spots started turning into painful blisters.”
Her symptoms were eventually diagnosed as Herpes, something she might have caught earlier if she had recognized the delayed timing.
Stories like these highlight why guessing rarely works. Symptoms can overlap, and personal assumptions often fill in the wrong explanation.
Everyday Triggers That Cause Allergic Reactions During Sex
Not every rash that appears after sex has anything to do with infection. In fact, dermatologists say contact irritation is extremely common, especially in sensitive skin areas.
Some of the most frequent triggers include:
| Trigger | Why It Can Cause Irritation | Typical Symptoms |
|---|---|---|
| Latex condoms | Some people develop sensitivity to natural latex proteins | Redness, itching, swelling |
| Lubricants | Fragrances, warming agents, or preservatives irritate skin | Burning or stinging |
| Spermicides | Chemicals designed to kill sperm may irritate tissue | Inflammation or rash |
| Soaps or body washes | Strong fragrances disrupt the skin barrier | Dryness, redness |
| Friction | Extended sexual activity can irritate delicate skin | Chafing or mild rash |
When irritation is caused by contact with a product, symptoms usually appear exactly where the product touched the skin. Switching to fragrance-free lubricants or non-latex condoms often resolves the issue completely.
But you should never ignore symptoms that don't go away or sores, blisters, or strange discharge that show up.
When Testing Becomes the Smart Next Step
A lot of people don't want to get tested because they are embarrassed or unsure. But taking a test doesn't mean that something is wrong. It's just a way to turn unknowns into facts.
Most of the time, doctors will tell you to get tested if your symptoms don't get better after a few days, if you get sores or blisters, or if you had sex without protection and want to be sure.
For those who prefer privacy, testing from home is an option. A discreet kit like the Combo STD Home Test Kit allows individuals to screen for multiple infections without waiting for a clinic appointment.
Testing doesn’t just answer the immediate question. It also protects partners and helps people make informed decisions about their health. And sometimes, the result provides peace of mind that a rash is simply irritation rather than infection.
People are also reading: Burning After Sex but No STD? It Could Be BV, Yeast, or Trich
What Doctors Actually Look For During an STD or Rash Evaluation
When someone visits a clinic with genital irritation, the first thing clinicians do is slow the story down. Instead of jumping straight to tests, they ask detailed questions about timing, symptoms, and recent exposures. This conversation often reveals clues that a quick internet search cannot.
When you go to the doctor with a rash, they usually want to know when it started, if you used any new products, if you used protection during sex, and if any other symptoms appeared. Before a physical exam even starts, these details help narrow down the options.
The appearance of the rash also matters. Skin irritation from allergies tends to look flat, red, or slightly bumpy, while certain infections have very recognizable patterns. A trained clinician can often distinguish between these patterns in just a few minutes.
| Observation | What It May Suggest |
|---|---|
| Uniform redness with itching | Often allergic or contact irritation |
| Clusters of fluid-filled blisters | Common sign of herpes infection |
| Single painless sore | Possible early syphilis symptom |
| Widespread rash on body | Possible secondary syphilis stage |
| Rash that fades within days | Often allergic or friction related |
Sometimes the evaluation ends there. If the symptoms are clearly irritation and go away quickly, you may not need to do anything else. If the rash looks strange or doesn't go away, the best thing to do is get tested.
Why Waiting Too Long to Test Can Create Confusion
One problem with sexually transmitted infections is that they don't always show up right away. A person might feel completely normal for days or weeks after exposure. During this time, the infection is present but invisible.
This time between exposure and symptoms often leads to wrong conclusions. Someone might see a rash after having sex and think that the two things are related, even if the rash came from something else, like shaving or detergent.
Other times, the opposite happens. A mild symptom appears days later and is dismissed as irritation when it actually signals infection. Because of this overlap, many clinicians encourage testing whenever symptoms appear after sexual contact.
The goal is not to create anxiety. It is simply to remove uncertainty. Knowing the answer allows people to move forward rather than replaying possibilities in their head.
Myths That Make STD Symptoms Harder to Recognize
Many people grow up hearing simplified messages about sexually transmitted infections. These messages are often meant to discourage risky behavior, but they sometimes leave adults with misleading ideas about how symptoms actually appear.
One of the most common myths is that STD symptoms always look dramatic. People expect severe pain, large sores, or obvious discharge. In reality, early symptoms can be subtle or even invisible.
Another myth is that allergic reactions cannot happen during sex. In reality, contact irritation is extremely common. The genital area contains delicate skin that reacts easily to friction, chemicals, and new products.
A third misconception is that condoms eliminate every possible reaction. Condoms make it much less likely that you will get an infection, but some people may be more sensitive to latex. In those cases, using polyurethane or polyisoprene condoms instead often works.
The takeaway is simple: symptoms alone rarely provide a complete answer. A rash might be harmless irritation, or it might be the body signaling infection.
Testing provides the clarity that guesswork cannot.
Check Your STD Status in Minutes
Test at Home with Remedium8-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $149.00 $392.00
For all 8 tests
How People Quietly Take Back Control of the Situation
For many people, the hardest part of sexual health is the uncertainty. Not knowing whether symptoms matter can create days of anxiety, late-night searches, and uncomfortable conversations.
The good news is that testing has become far more accessible and private than it used to be. Instead of waiting weeks for appointments, many people now choose discreet testing options that allow them to check their health from home.
A confidential resource like STD Rapid Test Kits gives individuals a way to screen for common infections without clinic waiting rooms or awkward scheduling. Results arrive quickly, and the process can be completed entirely in private.
This kind of testing is not about assuming the worst. It is about replacing uncertainty with information. Once people know their status, they can focus on solutions rather than speculation.
FAQs
1. Could an STD rash really look like a simple allergic reaction?
Absolutely. Skin only has so many ways to complain, and redness or itching is one of its favorite moves. Early symptoms of infections like Herpes or Syphilis can start off looking surprisingly mild, just a patch of irritation or a few bumps. The giveaway is usually what happens next: allergic reactions calm down once the irritant disappears, while infections tend to evolve into sores, blisters, or other changes.
2. I noticed itching right after sex. Does that mean it’s probably an allergy?
Often, yes. When itching shows up within minutes or a couple of hours, it’s frequently the skin reacting to something it touched, latex, lubricant, or even a new body wash. Think of it like your skin saying, “No thanks, we’re not doing that again.” Infections almost never appear that quickly because the bacteria or virus needs time to settle in.
3. How long should an allergic rash last?
Most contact reactions fade pretty quickly once the trigger is gone. A day or two of redness or mild itching isn’t unusual, especially if friction or shaving irritated the skin. But if you’re still dealing with the same rash a week later, or it’s getting worse instead of better, that’s usually a sign something else might be going on.
4. Can condoms actually cause reactions that look like STD symptoms?
They can, and it surprises a lot of people. Some folks are sensitive to latex itself, while others react to the lubricant or spermicide coating the condom. The result can be itching, redness, or swelling right where the condom touched the skin. Switching to non-latex condoms usually fixes the problem almost immediately.
5. If the rash disappeared after two days, should I still worry about an STD?
Probably not, but context matters. Quick-disappearing irritation is more typical of allergies, friction, or shaving. That said, if the rash appeared a few days after sex or came with sores, fever, or strange discharge, it's still a good idea to get tested for peace of mind.
6. Could shaving bumps or ingrown hairs be mistaken for STD symptoms?
All the time. Shaving irritation can produce small red bumps that look suspiciously like something more serious. The difference is that ingrown hairs usually appear exactly where hair was shaved and may have a visible hair trapped under the skin. They also tend to improve as the skin heals.
7. Do all sexually transmitted infections cause visible rashes?
Not even close. Many infections are surprisingly quiet at first. Conditions like Chlamydia or Gonorrhea often cause burning during urination or unusual discharge instead of skin changes. Some people have no symptoms at all, which is why routine testing matters even when everything seems normal.
8. When is testing the safest choice?
If symptoms linger longer than a few days, change in appearance, or appear several days after sexual contact, testing is the safest way to get answers. It removes the guessing game. Instead of trying to diagnose yourself at midnight with search results and anxiety, you get a clear answer you can act on.
9. What if I’m embarrassed to go to a clinic?
You’re definitely not alone there. A lot of people feel the same way, which is why private at-home testing has become so popular. It lets you check your health discreetly without waiting rooms or awkward conversations, just straightforward answers.
10. What’s the biggest mistake people make when they notice a rash after sex?
If they already know what caused it. Some people panic and assume the worst. Others shrug it off as irritation even when symptoms are evolving. The smarter move is simple: watch how the rash behaves, give your skin a couple days to calm down, and if anything feels off, get tested so you’re working with facts instead of guesses.
You Deserve Clarity, Not Guesswork
Rashes in intimate areas trigger a special kind of anxiety. The mind goes straight to worst-case scenarios, scrolling through symptoms, comparing photos, trying to decode what your body might be saying. But most of the time, the situation is simpler than the internet makes it seem.
Skin irritation can come from countless things, latex, lubricant, friction, shaving, even a new laundry detergent. But infections follow patterns too, and when timing, symptoms, or exposure leave room for doubt, the smartest move is clarity rather than speculation.
If a rash appeared immediately after contact with a product, give your skin a chance to calm down. If symptoms show up days after sex, evolve into sores, or simply refuse to disappear, that’s when testing becomes the responsible next step.
Don’t sit with uncertainty. If infection is even a possibility, start with a discreet screen like the Combo STD Home Test Kit. Your results are private, the process is straightforward, and knowing the answer always feels better than guessing.
How We Sourced This Article: This guide blends current sexual health guidance with dermatology research on allergic contact reactions and sexually transmitted infections. We reviewed clinical materials from the CDC, WHO, and major medical institutions alongside peer-reviewed dermatology literature examining rash presentation and STD symptom timelines. The goal was to present medically accurate distinctions while keeping the explanation practical and understandable for people navigating real-world symptoms.
Sources
1. An Overview of Sexually Transmitted Diseases from the Centers for Disease Control and Prevention
2. Fact Sheet from the World Health Organization on Sexually Transmitted Infections
3. Planned Parenthood—Signs and Tests for STDs
4. NHS – Sexually Transmitted Infections Overview
5. DermNet NZ – Contact Dermatitis
6. Centers for Disease Control and Prevention – Genital Herpes Overview
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on sexually transmitted infection prevention, diagnosis, and patient education. His work combines clinical expertise with clear, stigma-free communication so people can make informed decisions about their sexual health.
Reviewed by: Board-Certified Sexual Health Specialist | Last medically reviewed: March 2026
This article is only for informational purposes and should not be used instead of professional medical advice, diagnosis, or treatment.










