Quick Answer: A rash that appears right after sex is more often irritation, friction, heat rash, or an allergic reaction than an STD. Most STD-related rashes have specific timelines, patterns, or additional symptoms, and many do not appear immediately after exposure.
First, Breathe: Most Post-Sex Rashes Aren’t STDs
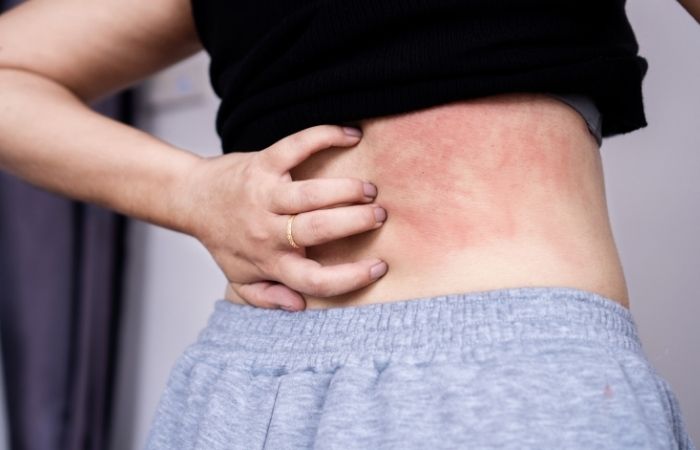
I’m going to say something that might calm your nervous system: your skin is dramatic. It reacts quickly to friction, moisture, shaving, sweat, new products, and new partners. It does not need an infection to get irritated.
After sex, your genital skin has often been exposed to heat, rubbing, bodily fluids, lubrication, latex, and sometimes microtears you can’t even see. That combination alone can create redness or bumps within hours. STDs, on the other hand, usually follow biological timelines that involve incubation periods.
Translation: if a rash appeared within a few hours, it is far more likely to be mechanical or allergic than infectious. That doesn’t mean ignore it. It means evaluate it calmly.
What STDs Actually Cause Rashes?
Not all sexually transmitted infections cause visible rashes. In fact, many of the most common ones, including Chlamydia and Gonorrhea, typically do not cause external skin rashes at all. They are internal infections affecting the urethra, cervix, throat, or rectum.
When people search “STD rash,” they are usually worried about a small group of infections known for skin involvement: Herpes (HSV-1 and HSV-2), Syphilis, and sometimes early HIV. Each has a different timeline and appearance.
| Infection | Typical Onset After Exposure | What It Usually Looks Like | Pain or Itch? |
|---|---|---|---|
| Herpes | 2–12 days | Clusters of fluid-filled blisters that break into sores | Often painful or tingling |
| Syphilis | 3–6 weeks | Single painless sore (first stage); later, widespread rash including palms/soles | Usually not itchy |
| HIV (acute phase) | 2–4 weeks | Flat red rash with flu-like symptoms | Typically not itchy |
If your rash appeared the same night or the next morning, that timeline alone makes infections like syphilis or HIV extremely unlikely. Biology doesn’t move that fast.
People are also reading: Tops, Bottoms, and Atlanta’s HIV Crisis: What Really Drives the Numbers
The Usual Suspects: Irritation, Heat, and Allergic Reactions
Now let’s talk about what causes most “rash after sex” scares.
Friction burn is incredibly common. Longer sessions, less lubrication, or vigorous movement can create red patches that feel raw or tender. These usually improve within 24–72 hours if you avoid further irritation.
Heat rash can appear as tiny red bumps in areas where sweat gets trapped, inner thighs, groin folds, under the scrotum, around the vulva. If you were sweating, in tight clothing, or didn’t shower right away, this becomes more likely.
Allergic reactions can happen to latex condoms, lubricants, spermicides, or even a partner’s body wash. These often show up as redness, itching, or small raised bumps fairly quickly after contact.
Notice the theme: fast onset usually points to contact irritation.
Timing Is Everything: A Side-by-Side Comparison
| When It Appeared | Most Likely Causes | Less Likely Causes |
|---|---|---|
| Within hours | Friction, heat rash, allergic reaction | Herpes (rarely that fast), syphilis, HIV |
| 2–7 days later | Herpes, yeast, irritation | Syphilis, HIV |
| 3–6 weeks later | Syphilis (primary stage) | Friction or heat-related issues |
One of the biggest mistakes people make is assuming anything that happens after sex must have been caused by that specific encounter. Sometimes timing is coincidence. Skin reacts to dozens of variables.
But here’s the investigator voice kicking in: if symptoms persist, worsen, blister, ulcerate, or are paired with fever or swollen lymph nodes, it’s time to consider testing.
Look Closer: What the Rash Actually Looks and Feels Like
When someone types “STD rash vs irritation” into a search bar at 1:17 a.m., what they’re really asking is: Does this look dangerous? So let’s slow it down and examine texture, sensation, and pattern, because those details matter more than panic.
A friction-related rash usually looks like flat redness or chafed skin. It may feel tender, almost like a carpet burn, especially during urination or when fabric rubs against it. There are no fluid-filled blisters, no deep ulcers, and no spreading clusters.
Herpes, on the other hand, typically starts with tingling or burning before visible lesions appear. Then come small, grouped blisters filled with clear fluid. They break open, forming shallow, painful sores. That clustered blister pattern is a major clue.
Syphilis in its first stage doesn’t look like a rash at all. It usually presents as a single, firm, painless sore called a chancre. Many people miss it because it doesn’t hurt. Weeks later, secondary syphilis can produce a more generalized rash, sometimes even on the palms of the hands or soles of the feet, which is a distinctive feature.
An allergic reaction tends to be itchier than infectious rashes. It may appear symmetrical where the contact occurred, for example, exactly where a condom touched or where lubricant was applied. It can also spread slightly beyond the genital area if your immune system is reacting strongly.
Pain, Itch, or Nothing at All?
Here’s a counterintuitive truth: some of the scariest-sounding infections don’t itch much. Early HIV rash, for example, is often described as flat, red, and not especially itchy, and it usually appears with flu-like symptoms such as fever, sore throat, or body aches.
If your rash is intensely itchy and improves with antihistamines or cool compresses, that leans toward allergic or heat-related causes. If it burns sharply, especially with small grouped blisters, that’s more consistent with herpes. If it doesn’t hurt at all and looks like a firm sore, that’s when syphilis testing becomes important.
And then there’s the category of “barely there.” Mild redness without bumps, without pain, and without progression often resolves on its own within a couple of days. That pattern alone lowers the likelihood of an STD significantly.
Check Your STD Status in Minutes
Test at Home with Remedium6-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $119.00 $294.00
For all 6 tests
Location Tells a Story
Where the rash appears can narrow things down further.
A rash confined to inner thighs or skin folds often suggests heat rash or sweat irritation. If bumps are directly on the shaft of the penis, labia, or around the anus, especially if clustered, herpes becomes more plausible. A single sore on the genitals that feels firm but painless is classic for primary syphilis.
But here’s the reassuring reality: irritation respects friction zones. It shows up where skin rubs skin or where tight clothing traps moisture. Infections tend to follow predictable biological patterns.
One patient once told me, “I convinced myself it was herpes because it burned, but I’d just shaved and then had sex for an hour.” Two days of gentle care and the redness faded completely. Context matters.
When Testing Actually Makes Sense
This is the part most people skip to: Do I need an STD test?
If your rash appeared within hours and is already improving, testing immediately is unlikely to change anything. Most infections have incubation periods, the time between exposure and detectability, that are longer than a day.
Here’s a simplified testing guidance table grounded in standard medical timelines.
| Scenario | Testing Recommendation |
|---|---|
| Painful blisters within 2–12 days of exposure | Test for Herpes (PCR swab if active lesion) |
| Single painless sore 3–6 weeks later | Blood test for Syphilis |
| Rash + fever 2–4 weeks after high-risk exposure | Consider HIV testing (Ag/Ab test) |
| Rash improving within 72 hours, no other symptoms | Monitor; testing optional unless other risk factors exist |
If you’re in that gray zone, unsure, anxious, replaying the encounter in your head, testing can provide clarity. Not because panic demands it, but because certainty reduces spiraling.
You can explore discreet options through STD Rapid Test Kits, including combination panels that screen for multiple infections at once. If you’re specifically worried about herpes, there are targeted options like this Herpes HSV-1 & HSV-2 Rapid Test Kit designed for privacy and quick answers.
Testing isn’t an admission of guilt. It’s an act of control.
People are also reading: My STD Symptoms Disappeared, Am I Still Infected?
How Long Should a Post-Sex Rash Last?
Time is one of the most honest diagnostic tools we have. Irritation behaves differently than infection, and your skin will usually tell you which direction things are heading if you watch it calmly for a couple of days.
A friction burn or heat rash typically improves within 24 to 72 hours once the area is kept clean, dry, and free from further rubbing. Redness fades. Tenderness softens. The skin may lightly peel as it heals. That trajectory, steady improvement, is reassuring.
Herpes lesions, by contrast, follow a more defined arc. Tingling or burning may come first, then visible blisters, then open sores, then crusting over several days. The full cycle often lasts 7 to 14 days during an initial outbreak. It does not usually disappear in two days.
Syphilis sores can linger for three to six weeks if untreated, even if they are painless. That’s part of why they’re missed. The absence of discomfort can create false reassurance.
If your rash is already fading by day two or three, that strongly favors irritation over infection.
Red Flags That Deserve Immediate Attention
This is where the no-nonsense investigator voice steps in. While most post-sex rashes are benign, certain patterns warrant quicker evaluation.
If you notice rapidly spreading redness, significant swelling, pus, severe pain, or fever, that is not a “wait and see” situation. Those symptoms could signal a bacterial skin infection unrelated to STDs, or a complication that needs antibiotics.
If you develop painful urination, unusual discharge, swollen lymph nodes in the groin, or flu-like symptoms alongside a rash, testing becomes more urgent. When systemic symptoms appear, it’s time to move from guessing to confirming.
And if you experienced a high-risk exposure, unprotected sex with a new partner, a known positive partner, or a condom break, testing provides clarity regardless of how mild the rash looks.
The Psychology of “It Must Be an STD”
Let’s talk about the part nobody says out loud. After sex, especially with a new partner, the mind scans for evidence of danger. Every tingle becomes suspicious. Every bump feels loaded with meaning.
One woman once told me, “I checked with a flashlight three times in one night. I was sure I’d ruined my life.” What she had was heat rash from tight jeans and a long Uber ride home. The rash faded in 48 hours. The anxiety lasted longer.
Shame amplifies sensation. If you already feel guilty or unsure about the encounter, your brain is primed to interpret normal skin variation as catastrophic. That doesn’t make you dramatic. It makes you human.
But here’s the grounding truth: STDs follow biological rules. They don’t appear instantly out of nowhere. They don’t vanish overnight. And they don’t punish you for pleasure.
What to Do Right Now (Instead of Spiraling)
First, give the skin a break. Avoid further friction. Wear loose, breathable clothing. Skip new soaps or scented products. Keep the area dry and clean with mild water.
Second, observe without obsessing. Check once or twice a day, not every fifteen minutes. You are looking for progression, not perfection.
Third, decide rationally about testing based on timeline and risk, not fear. If you are within a few days of exposure and have no blistering or systemic symptoms, waiting for the appropriate window period improves test accuracy.
If you are past the typical incubation window for infections like herpes or syphilis and symptoms align, that’s when a targeted test makes sense. Combination panels are useful when uncertainty is high. A comprehensive option like the Combo STD Home Test Kit can screen for multiple infections discreetly from home.
Peace of mind is not weakness. It’s health maintenance.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
Before You Label It, Ask These Three Questions
When people panic about a rash after sex, they usually skip straight to diagnosis. But slow medicine is better medicine. Before you label it an STD, or dismiss it completely, ask three grounding questions.
First: Is it changing? Irritation tends to peak quickly and then improve. Infectious rashes often evolve. Blisters form. Sores open. New spots appear. Stability or improvement within 48 hours is reassuring. Escalation is information.
Second: Does the timeline actually make biological sense? If you had sex last night and noticed redness this morning, infections like Syphilis or HIV are not realistic explanations. Their incubation periods are measured in weeks, not hours. Your anxiety might be immediate. Pathogens are not.
Third: What else was happening? Were you sweating? Shaved earlier that day? Used a new lubricant? Had longer or rougher sex than usual? Wore tight clothing afterward? Skin doesn’t react in a vacuum. Context often explains what fear tries to dramatize.
I once had a patient who was convinced a mild groin rash was a new infection. After talking it through, we realized he’d switched to a heavily scented body wash and then spent an hour in tight gym shorts post-hookup. Two days later, the rash was gone. The infection he feared never existed.
This is the part where the compassionate voice matters: noticing your body doesn’t make you paranoid. It makes you attentive. The key is pairing attention with logic.
If you’re unsure, monitor for 48 to 72 hours. If things worsen, blister, ulcerate, or align with known incubation timelines, test. If they fade, your skin was simply doing what skin does, reacting and healing.
FAQs
1. I noticed redness right after sex. Did I just catch something?
Probably not. Infections don’t usually work that fast. If it showed up the same night, especially if things were enthusiastic, dry, or involved shaving, irritation is the leading suspect. Your skin is reactive. It’s not delivering moral judgments.
2. It burns when I pee, does that automatically mean herpes?
Not automatically. Friction alone can make skin raw enough to sting during urination. Herpes tends to involve distinct clusters of blisters that open into sores, often with tingling beforehand. If you’re just dealing with generalized redness and no blisters, pause before jumping to worst-case scenarios.
3. What if it doesn’t itch at all? Isn’t that suspicious?
Not necessarily. Some irritation barely itches. Some infections don’t itch either. The real question is: is it evolving? Spreading? Turning into blisters? A stable patch of redness that fades in a couple of days tells a very different story than lesions that progress.
4. Can you get an STD rash without any other symptoms?
Yes, but it depends on the infection. A primary Syphilis sore can appear without pain. Early HIV rash usually comes with flu-like symptoms. Herpes often announces itself with tingling or sensitivity before sores appear. A completely isolated, mild rash that resolves quickly is less characteristic of these infections.
5. I shaved earlier that day. Could that really be the whole explanation?
Honestly? Yes. Shaving creates microscopic breaks in the skin. Add friction, sweat, and body fluids, and you’ve built the perfect environment for razor burn or folliculitis. It can look dramatic. It can feel dramatic. But it’s mechanical, not infectious.
6. If it was an allergic reaction, would it show up that fast?
Allergies are speedy. Latex, lubricant, or spermicide reactions can appear within minutes to hours. They’re often itchy, sometimes puffy, and usually line up exactly where contact happened. Switch products and the pattern often disappears.
7. How do I know when it’s time to stop monitoring and actually test?
If blisters form. If you see an open sore that doesn’t hurt but won’t go away. If you develop fever, swollen glands, or feel generally unwell. Or if your exposure risk was high and waiting is just fueling anxiety. Testing isn’t panic, it’s clarity.
8. My partner says they don’t have symptoms. Should I still worry?
Many STDs can be silent. That’s just biology, not dishonesty. The decision to test should be based on exposure and timing, not blame. Sexual health isn’t about catching someone. It’s about taking care of yourself.
9. What if it’s already fading, did I overreact?
You didn’t overreact. You responded to uncertainty. That’s human. If it’s improving within 48–72 hours and never developed into blisters or ulcers, irritation was the likely cause. Skin heals quickly when it’s given a break.
10. Be honest, how often is a “rash after sex” actually an STD?
Less often than people fear. In clinical practice, the majority of immediate post-sex rashes turn out to be friction, sweat, shaving irritation, or contact reactions. STDs have patterns. They follow timelines. They don’t usually appear out of nowhere the same night.
You Deserve Clarity, Not Catastrophizing
A rash after sex can feel like a verdict. But most of the time, it’s just skin reacting to friction, sweat, or contact. Your body is responsive, not accusatory.
If something doesn’t resolve, if blisters appear, if timing lines up with known incubation windows, or if you simply want certainty, testing is a calm, rational next step. You can explore discreet options through STD Rapid Test Kits, including comprehensive panels like the Combo STD Home Test Kit that screen for common infections privately at home.
You are not reckless for having sex. You are responsible when you choose clarity.
How We Sourced This Article: This guide was informed by current guidance from major public health organizations including the Centers for Disease Control and Prevention (CDC), Mayo Clinic, and the World Health Organization, alongside peer-reviewed infectious disease literature and clinical practice standards.
Sources
1. CDC – Genital Herpes Fact Sheet
4. Mayo Clinic: Signs and Reasons for Genital Herpes
5. World Health Organization – Sexually Transmitted Infections Fact Sheet
6. CDC – 2021 STI Treatment Guidelines: Genital Ulcer Disease
7. NHS – Genital Herpes Overview
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He combines clinical precision with a stigma-free, sex-positive approach to patient education and accessible testing.
Reviewed by: L. Carter, PA-C | Last medically reviewed: March 2026
This article is meant to give you information, not medical advice.










