Quick Answer: Jock itch (ringworm) is a fungal infection that can spread through skin contact during sex but is not a true STD. Treatment usually involves antifungal creams for 2–4 weeks, and symptoms should improve within days if treated correctly.
This Is Where Most People Spiral (And Why It Makes Sense)
A rash after sex hits differently. It’s not just physical, it’s emotional. You replay everything. Who you were with. Whether you used protection. Whether you missed something. And suddenly, a patch of irritated skin feels like a full-blown life event.
One patient once told me, “I didn’t even care that it itched, I just needed to know if my life was about to change.” That’s the real weight behind this kind of symptom. It’s not just discomfort. It’s uncertainty.
Here’s the grounding truth: not every rash after sex is an STD. In fact, a large percentage of these cases turn out to be fungal infections, especially something called jock itch, which is basically ringworm in the groin area.
What You’re Actually Looking At: Fungus vs STD Rash
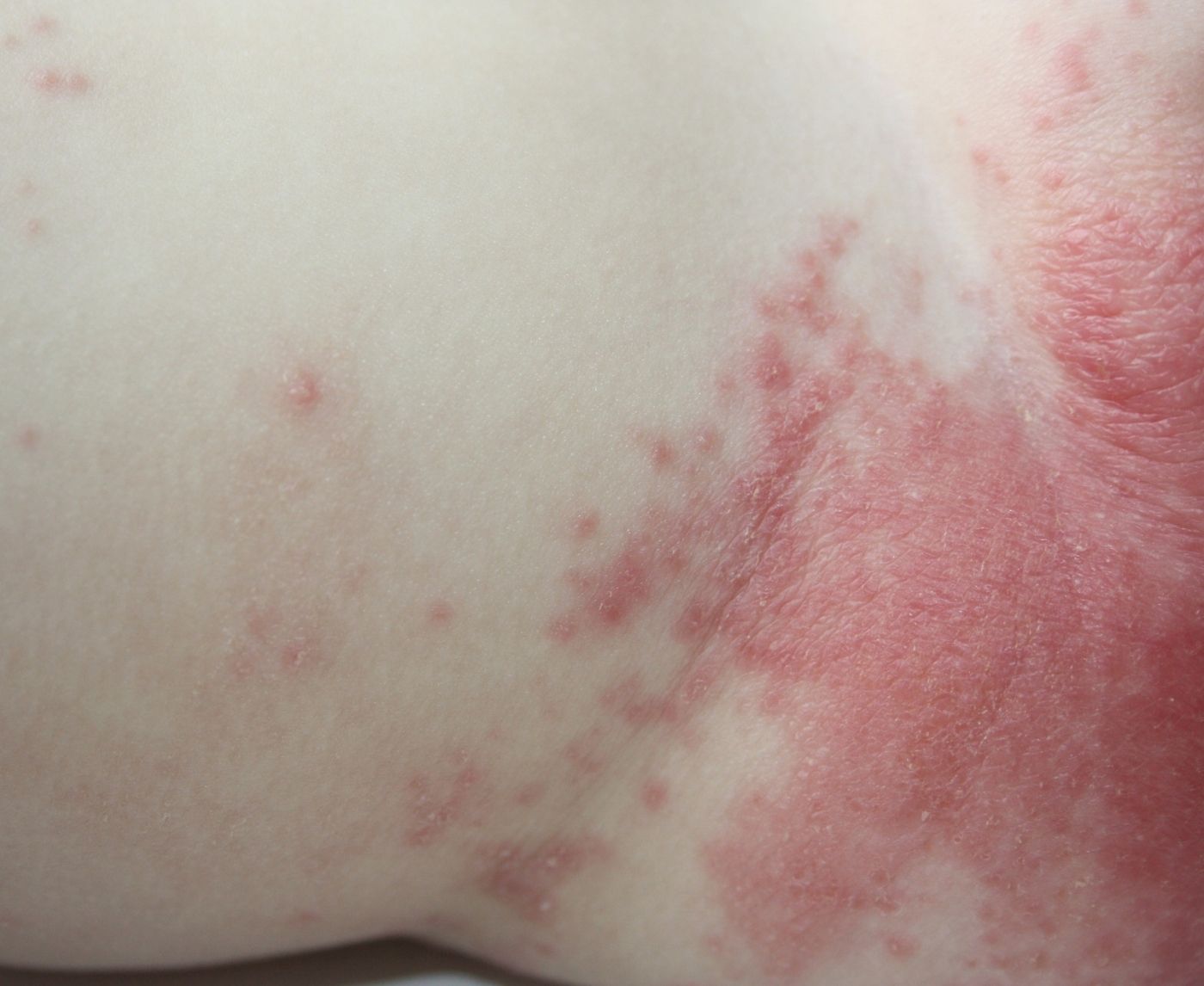
Let’s slow this down and look at what’s happening on your skin. Because visually, fungal infections and some STDs can overlap just enough to confuse people, but the patterns are different once you know what to look for.
| Feature | Fungal (Jock Itch / Ringworm) | STD-Related Rash |
|---|---|---|
| Shape | Ring-shaped, defined edges | Blisters, sores, or irregular patches |
| Itching | Common, often intense | Variable |
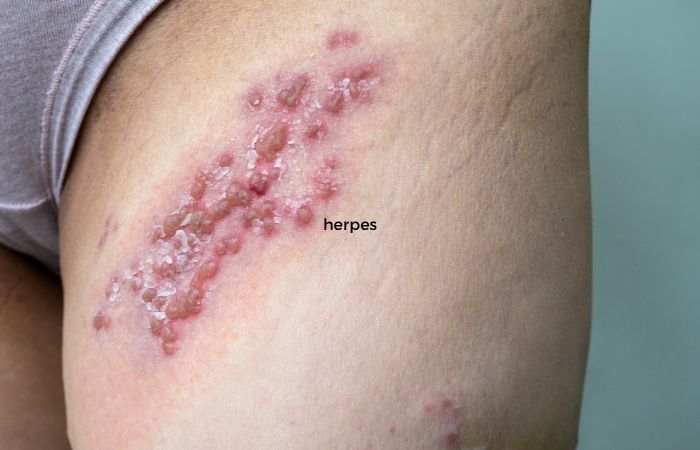
| Pain | Mild irritation | Often painful (especially herpes) |
| Spread pattern | Expands outward | Clustered lesions or ulcers |
Here’s the key insight: fungal infections tend to look organized. They expand in a circular way, almost like your skin is drawing boundaries. STDs, especially viral ones, tend to look more chaotic, clusters, blisters, or open sores.
But, and this matters, visual guesses are not diagnosis. If there’s any doubt, testing is how you take control of the situation, not Google.
People are also reading: Price, Privacy, and Peace of Mind: Your 2025 STD Test Comparison Guide
How Ringworm Ends Up “Sexually Transmitted”
This is where language trips people up. Ringworm isn’t classified as a sexually transmitted disease, but it absolutely can spread during sex. Skin-to-skin contact, warmth, moisture, all of that creates a perfect environment for fungi to move from one body to another.
Think of it less like an STD and more like a contact infection that just happens to thrive in intimate situations. The groin area stays warm and slightly damp, which is basically a five-star hotel for fungal organisms.
“I thought I caught something serious,” another patient said. “Turns out it was just something my body picked up from skin contact. Still sucked, but way less scary once I knew.”
That’s the shift. Same symptom, completely different emotional outcome once you understand what you’re dealing with.
What Actually Clears It: Real Treatment That Works
Let’s get practical, because this is the part most people want immediately. If this is jock itch or ringworm, treatment is straightforward, but only if you do it correctly and consistently.
The biggest mistake? Stopping too early. The rash fades, you think it’s gone, and then it comes back louder. That’s because fungus lingers under the surface longer than it looks like it does.
| Treatment | How It Works | Timeline |
|---|---|---|
| Clotrimazole / Miconazole | Kills surface fungus | 2–4 weeks |
| Terbinafine | Stronger antifungal action | 1–2 weeks |
| Oral antifungals | For stubborn or widespread cases | Doctor prescribed |
Apply the cream beyond the visible rash. Wash and dry the area thoroughly before applying. And keep going even after the skin looks normal again. That last part is what prevents recurrence.
Also, skip steroid creams unless prescribed. They can temporarily reduce redness while making the fungal infection worse underneath. It’s a short-term illusion that leads to a longer problem.
When It’s Not Just a Rash Anymore
There are moments when you shouldn’t wait it out. If the rash becomes painful, starts blistering, or doesn’t improve after a couple of weeks of antifungal treatment, it’s time to pivot.
This is where testing comes in, not as a panic move, but as a clarity move. Because if there’s even a small chance this could be something like herpes or another infection, knowing early changes everything about how you manage it.
You can start with something discreet and fast like an at-home STD test if you’re not ready for a clinic visit. It’s a simple way to rule things out and stop guessing.
“I wish I had just tested instead of stressing for a week,” someone once said. That’s usually how it goes, uncertainty is the hardest part, not the result.
What to Do Right Now (Without Overthinking It)
If you’re dealing with a rash after sex, you don’t need to solve everything in one moment. You just need a plan that moves you forward.
Start with antifungal treatment if it looks like jock itch. Keep the area dry. Avoid friction. Give your skin space to heal. And at the same time, stay honest with yourself, if something feels off or doesn’t match typical fungal patterns, get tested.
That balance is everything. Calm action instead of panic reaction.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
“I Thought It Was an STD”, A Real Moment Most People Don’t Talk About
Jordan, 27, noticed the rash the morning after a weekend hookup. It wasn’t dramatic at first, just a faint red patch near the inner thigh. But by day two, it itched. By day three, it had a defined edge. And by day four, Google had already convinced him it might be Herpes.
“I kept zooming in on photos online, trying to match what I had. Every image made me more anxious. I didn’t even know fungal infections could look like that.”
What he had was classic jock itch. But the emotional experience? That was very real. The waiting, the guessing, the mental spiral, it’s something a lot of people go through quietly.
This is why understanding the difference matters. Because the sooner you recognize what’s likely fungal, the faster you can treat it, and the less time you spend imagining worst-case scenarios.
Why It Happened After Sex (Even If You’re “Clean”)
This part catches people off guard. They assume that if something shows up after sex, it must be sexually transmitted in the traditional sense. But fungal infections don’t follow those rules.
They’re opportunistic. They take advantage of conditions, heat, friction, moisture, not identity or “cleanliness.” You can shower daily, use protection, and still end up with jock itch after sex simply because the environment was right.
During sex, especially longer sessions, your skin experiences:
- Friction: which slightly irritates and weakens the skin barrier
- Moisture: sweat and natural fluids create a humid environment
- Contact: prolonged skin-to-skin exposure allows fungi to transfer
That combination is enough. It doesn’t mean anyone did anything wrong. It just means your skin encountered something it reacted to.
One person put it simply: “It felt unfair. Like I did everything right. But bodies don’t run on fairness, they run on biology.”
The Timeline No One Explains Clearly
One of the biggest clues in figuring this out is timing. When symptoms show up can tell you a lot about what you’re dealing with.
| Condition | Typical Onset After Exposure | What It Feels Like |
|---|---|---|
| Fungal (Jock Itch) | 1–5 days | Itching, redness, spreading rash |
| Herpes | 2–12 days | Pain, blisters, sores |
| Syphilis | 10–90 days | Painless ulcer |
If something shows up quickly and itches more than it hurts, fungal causes climb higher on the list. If it’s painful, blistering, or ulcer-like, that’s when you stop guessing and get evaluated or tested right away.
Timing isn’t diagnosis, but it’s a strong clue that helps you decide your next move.
Where People Go Wrong With Treatment
There’s a pattern I see constantly. Someone starts treatment, sees improvement, and then stops too soon. A week later, the rash is back, and now it’s more stubborn.
Fungal infections don’t just live on the surface. They sit deeper in the skin layers, even when things look clear. So stopping early is like leaving the job half done.
Another common mistake is mixing treatments without knowing what you’re treating. Using antibacterial creams, steroid creams, or random home remedies can actually make things worse or mask symptoms.
“I tried three different creams before I realized I needed one specific thing,” someone once admitted. “Once I used the right one consistently, it finally cleared.”
Consistency beats variety here. Pick the right antifungal, and stick with it.

People are also reading: Herpes, HPV, or Just Irritation? Rash After Sex Symptoms Decoded
When You Should Pause and Consider STD Testing
Here’s the honest line: if your symptoms don’t behave like a typical fungal infection, don’t try to force the diagnosis. Your body doesn’t follow internet checklists perfectly.
Consider testing if:
- Pain: The rash hurts instead of just itching
- Blisters: You notice fluid-filled bumps or open sores
- No improvement: After 10–14 days of antifungal treatment
- Uncertainty: You simply don’t feel confident about what it is
This isn’t about assuming the worst. It’s about removing doubt.
If you want something discreet and immediate, a combo STD home test kit can check for multiple infections at once. It’s a way to get clarity without sitting in a waiting room replaying everything in your head.
And if everything comes back negative? That’s powerful. It lets you fully focus on treating what’s actually there.
Small Changes That Make a Big Difference During Healing
Treatment isn’t just about what you apply, it’s also about the environment you create for your skin. Fungus thrives in certain conditions, and healing means disrupting that environment.
Keep things dry. That’s the priority. After showering, take a moment to fully dry the area, even if it feels unnecessary. Moisture is what allows the infection to persist.
Wear looser clothing when possible. Tight fabrics trap heat and friction, which slows recovery. This isn’t forever, it’s just while your skin resets.
And maybe most overlooked: give your body a break from sexual activity until the rash clears. Not as punishment, but as protection, for both you and your partner.
“I rushed back too soon and it came right back,” one person shared. “The second time, I waited, and it actually stayed gone.”
What No One Tells You About Recurrence (Why It Keeps Coming Back)
This is the part that frustrates people the most. You treat it, it fades, you relax, and then a week or two later, it’s back like nothing ever happened. It feels personal, like your body is working against you.
But what’s actually happening is simpler. Fungal infections are persistent, and they don’t need much to restart. A little leftover fungus, a warm environment, a bit of friction, and it picks up where it left off.
That’s why prevention matters just as much as treatment. Not in a paranoid way, but in a practical one. You’re not trying to avoid life, you’re just making it harder for the fungus to come back.
| Cause | What’s Happening | What Helps |
|---|---|---|
| Stopping treatment early | Fungus remains under the skin | Continue 1–2 weeks after it looks clear |
| Moisture buildup | Creates ideal growth conditions | Dry thoroughly, breathable clothing |
| Re-exposure | Contact with infected skin or surfaces | Avoid sharing towels, pause intimacy |
This isn’t about being perfect. It’s about understanding patterns. Once you see how it behaves, it becomes much easier to manage, and much less stressful.
Check Your STD Status in Minutes
Test at Home with Remedium6-in-1 STD Rapid Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $119.00 $294.00
For all 6 tests
Before You Jump to Conclusions, Read Your Skin Like a Story
When something shows up on your body after sex, your brain wants a label immediately. Good or bad. Serious or nothing. But skin doesn’t work like that, it tells a story in patterns, not headlines.
A fungal rash usually unfolds gradually. It starts subtle, then becomes more defined. It itches in a way that’s persistent but not sharp. You might notice it spreading outward, almost like it’s drawing a boundary on your skin. That slow, expanding pattern is a clue most people miss when they’re focused on worst-case scenarios.
Compare that to infections like Herpes, where symptoms often feel more abrupt and intense. People describe it as “something feels wrong” before anything is even visible. Then come the blisters, the tenderness, the kind of discomfort that makes you very aware of the area even without touching it.
The goal isn’t to self-diagnose perfectly. It’s to notice patterns so you can respond instead of react. Treat what clearly looks fungal. Watch how it behaves over a few days. And if the story your skin is telling doesn’t match what you expected, that’s your cue to get clarity, not panic.
“I realized I was trying to skip steps,” someone once said. “I wanted an answer before I even gave my body time to show me what it was.” That’s the shift. You don’t need instant certainty, you need the next right move.
FAQs
1. So… can you actually get ringworm from sex, or is that just internet panic?
You can, but not in the way people think about STDs. It’s not living in bodily fluids, it’s just skin-to-skin contact doing its thing. If someone has a fungal infection and there’s enough contact, friction, and moisture, it can transfer. It’s less “you caught an STD” and more “your skin picked something up.”
2. Why did this show up right after sex though?
That timing feels suspicious. Yeah, the timing messes with your head. But sex creates the perfect environment, heat, sweat, friction, and that’s exactly what fungus loves. It doesn’t mean your partner “gave you something serious,” it just means conditions lined up.
3. How can I tell if this is jock itch or something like herpes without freaking out?
Start with how it feels. If it itches like crazy and slowly spreads outward, fungal jumps higher on the list. If it hurts, burns, or turns into blisters or open sores, that’s when you stop guessing and get tested. Your body usually gives you clues, you just need to know which ones matter.
4. I started using cream and it looks better, can I stop now?
This is where people accidentally sign up for round two. Even if it looks gone, the fungus can still be hanging out under the surface. Give it another week or two after it clears. Think of it like finishing antibiotics, you don’t stop just because you feel better.
5. Is it okay to still hook up while I’m treating it?
Real answer? It’s better to pause. Not because you did anything wrong, but because it can spread through contact and slow your healing down. Give your skin a little break, it’s not forever, just until things settle.
6. What if I’ve been treating it and it’s just… not going away?
That’s your signal to pivot. Either it’s a stubborn fungal infection that needs stronger treatment, or it’s not fungal at all. If you’re two weeks in with no real improvement, it’s time to get a second opinion or test, no guessing game required.
7. Can I just use whatever cream I have at home?
Not all creams are created equal. Antifungal creams work, random antibacterial or steroid creams can actually make things worse or hide symptoms. If you’re treating fungus, you want something specifically labeled antifungal. Simple, but important.
8. Why does it itch more at night or after sweating?
Because fungus thrives in warmth and moisture. So when your body heats up or the area gets damp, it basically wakes up and gets more active. That’s why keeping things dry isn’t just advice, it’s part of the treatment.
9. If this looks like ringworm, do I really need an STD test?
Not all the time, but if there's even a small doubt, it's worth it for peace of mind. Especially if something seems wrong, looks strange, or doesn't get better with treatment. Testing isn’t about assuming the worst, it’s about closing the loop.
10. This feels embarrassing… is this something people actually deal with a lot?
Way more than you think. People just don’t talk about it openly. Rashes after sex are incredibly common, and a huge chunk turn out to be things like fungal infections, not STDs. You’re not weird, you’re just human with skin that reacts to stuff.
You Deserve Clarity, Not Guesswork
An itchy rash after sex can mess with your head fast. It’s not just the discomfort, it’s the meaning you attach to it. Suddenly you’re questioning decisions, replaying moments, and trying to diagnose yourself in a browser tab at midnight.
But most of the time, this isn’t about something life-altering. It’s about understanding what your skin is telling you. If it itches and spreads, treat it like a fungal infection and follow through completely. If something feels off, pain, blisters, no improvement, shift gears and get answers. Each step replaces panic with clarity.
Don’t sit in the uncertainty longer than you have to. If there’s even a small chance this could be something more, start with a discreet option like the Combo STD Home Test Kit. No waiting rooms, no guessing, just real answers so you can move forward.
How We Sourced This Article: From a clinical dermatology point of view, this guide has information about fungal infections. From a sexual health point of view, it has information about the patterns of STD symptoms. We checked the CDC, NHS, Mayo Clinic, and peer-reviewed dermatology research, as well as people's real-life experiences with symptoms, to make sure that this information is both medically correct and true to life.
Sources
1. Centers for Disease Control and Prevention – Ringworm (Tinea)
2. NHS – Ringworm Symptoms and Treatment
3. American Academy of Dermatology – Ringworm
4. PubMed – Dermatophyte Infection Research
5. World Health Organization – Sexually Transmitted Infections
6. DermNet NZ – Tinea Cruris (Jock Itch)
7. Planned Parenthood – STDs and Safer Sex Overview
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. His work blends clinical accuracy with a direct, stigma-free approach to sexual health education.
Reviewed by: Board-Certified Dermatology Specialist | Last medically reviewed: March 2026
This article is only meant to give you information; it is not a substitute for professional medical advice, diagnosis, or treatment.