Quick Answer: A faint line on an STD rapid test usually still counts as a positive result if it appears within the official reading time and the control line is visible. Rapid tests detect biological markers, and even small amounts can produce a lighter line. When in doubt, repeat the test or confirm with a lab test.
The Moment People Notice the Faint Line
Rapid STD tests are designed to be simple. You collect a sample, apply it to the cassette, wait the recommended time, and read the lines. In theory, it’s straightforward. In reality, thousands of people every day stare at a result that isn’t perfectly clear.
One of the most common things people say when they see a faint line is: “It’s probably just a shadow.” That reaction is understandable. A faint line feels uncertain. It doesn’t carry the visual confidence of a dark stripe that leaves no room for interpretation.
But rapid tests don’t work like a light switch. They work more like a chemical signal that grows stronger depending on how much of a specific marker is present in the sample. If the amount is lower, the line can appear lighter. The test is still reacting to something real.
“I kept tilting the test under the bathroom light,” said one patient during a clinic intake interview. “It looked like a ghost line. I thought maybe my eyes were playing tricks on me.”
This moment of uncertainty is incredibly common, especially with at-home tests. The key is understanding what those lines actually represent.
What the Lines on a Rapid STD Test Actually Mean
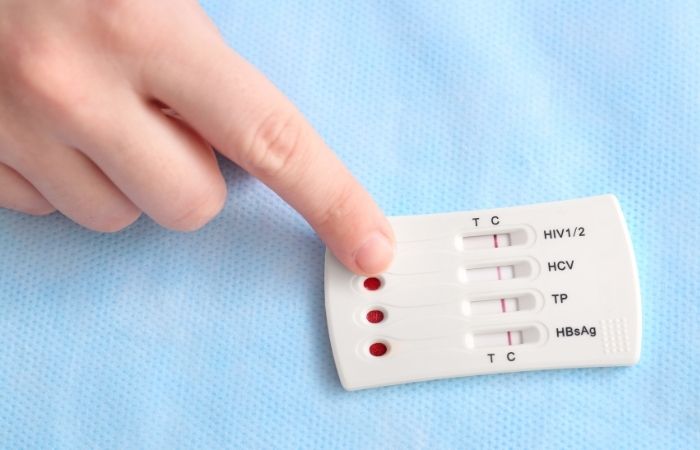
Most rapid STD tests use what scientists call a lateral flow immunoassay. The concept sounds technical, but the visual design is simple: one line confirms the test worked, and the other line reacts to markers linked to infection.
| Line | What It Means | Why It Matters |
|---|---|---|
| Control Line (C) | Shows the test worked properly | The test result is not valid without it. |
| Test Line (T) | Shows up when the test finds markers that are linked to infection | Even a faint line could mean a positive reaction. |
The control line is like a built-in safety check. It shows that the liquid moved through the test strip correctly and that the chemistry inside the cassette is working.
The test line is where things become emotionally loaded. That line reacts when the strip encounters antibodies, antigens, or other molecules associated with specific infections. If those markers are present, even in small quantities, the test chemistry can produce a faint signal.
“The darkness of the line doesn’t measure how infected someone is,” explained a laboratory technologist during a training workshop. “It simply reflects how strong the reaction was in that specific sample.”
That means a faint line doesn’t necessarily mean an early infection, and a dark line doesn’t mean a worse one. The test isn’t grading severity. It’s detecting presence.
People are also reading: TikTok Said It Was Just a Rash. My Doctor Said Herpes.
Why a Positive Line Can Look Faint
Several completely normal factors can make a rapid STD test line appear lighter than expected. None of them automatically mean the result is wrong.
The most common reason is simply concentration. The test looks for a biological marker, and if the sample has less of it, the chemical reaction makes a lighter signal. The test still sees the marker, but it doesn't react as strongly.
Timing also plays a role. Rapid tests must be read within a specific window, often between 10 and 20 minutes depending on the kit. Within that time frame, a faint line can be a legitimate positive signal. After the window passes, evaporation artifacts may appear and confuse interpretation.
Another factor is sample variability. Even with proper technique, two samples from the same person can contain slightly different concentrations of antibodies or antigens. That variation can change how bold the line appears.
The bottom line is simple: faint lines happen because chemistry is sensitive, not because the test is malfunctioning.
Positive, Negative, and Invalid Results Compared
Understanding the difference between these three outcomes removes most of the anxiety people feel when reading rapid test results. The lines themselves provide the clues.
| Result | What You See | What It Means |
|---|---|---|
| Negative | Control line only | No detectable markers in the sample |
| Positive | Control line plus a test line (even faint) | Markers associated with infection detected |
| Invalid | No control line | The test didn't work right or was done wrong. |
If the control line doesn't show up, you can't trust the test. It means that the fluid didn't move right, the reagents didn't work, or the test wasn't done right.
If the control line appears and a second line is visible, even faintly, the test chemistry has detected something. That’s why most instructions clearly state that any visible test line within the reading window should be considered positive.
This rule exists because early or low-level signals still matter. Ignoring faint lines would cause many real infections to be missed.
Faint Lines vs Evaporation Lines
One reason people doubt faint results is the internet myth about evaporation lines. These lines can appear on some rapid tests after the official reading time passes, especially if the strip dries out.
Evaporation lines usually look different from true positive lines. They often appear gray, uneven, or colorless rather than pink or purple like the control line.
The biggest difference is timing. If the faint line appears within the official reading window, it is much more likely to be a true reaction. If it appears thirty minutes later while the cassette sits on the counter, it may be an artifact of drying.
“People sometimes stare at tests for hours,” one sexual health nurse explained. “But the instructions usually give a very clear reading window for a reason.”
Following that timing guideline prevents most confusion.
Check Your STD Status in Minutes
Test at Home with Remedium8-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $149.00 $392.00
For all 8 tests
Common Mistakes That Make Results Harder to Read
Rapid tests are designed to be user-friendly, but small errors can still affect how results appear. Fortunately, these mistakes are easy to avoid once you know what they are.
- Reading too early: Lines may not fully develop yet.
- Reading too late: Evaporation artifacts may appear.
- Too little sample: Weak fluid flow can produce unclear lines.
- Incorrect buffer amount: The reaction may not complete properly.
Another surprisingly common issue is lighting. Bathroom lighting can cast shadows across the cassette window, making faint lines harder to see. Looking at the test under brighter neutral light can clarify what’s actually there.
None of these mistakes automatically invalidate a test, but they can create confusion about the result.
If You See a Faint Line, Here’s the Calm Next Step
The first thing to remember is that faint lines are not rare. They happen frequently with rapid tests, and most manufacturers specifically warn users not to ignore them.
If a faint test line appears within the correct reading window and the control line is present, the safest interpretation is that the result may be positive. That doesn’t mean panic is required, but it does mean confirmation is a good idea.
Many people choose to repeat the test after the appropriate window period or confirm with a laboratory test. Clinics and telehealth services can help verify results and discuss treatment options if needed.
If you prefer privacy, many people start by ordering discreet kits through STD Rapid Test Kits, which allow testing at home before deciding whether to pursue clinical follow-up.
What matters most is clarity. Testing exists to replace guesswork with real information.
Why Timing Matters When Reading a Rapid STD Test
People often forget about the reading window when they get a quick STD test. Every quick test has a certain amount of time after which the result is no longer valid. The kit could take 10, 15, or even 20 minutes to work.
Within that window, the chemistry inside the test strip is actively reacting to the sample. Colored particles move across the strip and bind to specific molecules if they are present. This is when the test line develops and becomes visible.
After that window passes, the chemistry is no longer actively controlled. The strip begins to dry, and faint artifacts can appear. These marks are often what people refer to as evaporation lines.
This is why test instructions almost always include a sentence similar to: “Do not read the test after the specified time.” It isn’t a random rule. It exists to protect you from misinterpreting a drying test strip.

People are also reading: I Asked Reddit About My STD Symptoms. Here’s What Happened
How Rapid STD Tests Detect Infection
If you know how these tests work, you can better understand results that are hard to understand. Rapid STD tests look for biological signs that show someone has an infection. Depending on the test, the markers could be antibodies that your immune system makes or antigens that come from the pathogen itself.
The process starts when a liquid sample travels across the test strip. As the sample moves, it encounters tiny particles coated with molecules designed to bind to specific markers. If those markers exist in the sample, they attach to these particles and continue moving across the strip.
Further down the strip is the test line area. This section contains molecules designed to capture those complexes. When enough of them accumulate, they create a visible colored line.
The control line works similarly but reacts with particles that should always appear if the liquid moved correctly. That is why the control line must appear for the result to be considered valid.
What this means in practice is simple: the test line doesn’t appear randomly. It appears because a chemical reaction occurred.
Does a Darker Line Mean a Stronger Infection?
This is one of the most common things people get wrong about quick tests. A lot of people think that the darker the line, the worse the infection is. In reality, the line's intensity is not a good way to tell how bad the infection is.
A darker line simply means that more of the detectable marker was present in the sample at that moment. A lighter line means the concentration was lower. The test was never designed to measure severity or stage of infection.
There are a few normal things that can change how strong a line looks:
- Sample concentration: Different samples contain slightly different marker levels.
- Hydration levels: Dilution of the sample can affect the reaction strength.
- Early immune response: Antibody levels can rise gradually.
- Natural variation in test strips: The way they are made can cause small differences in how they look.
For this reason, healthcare professionals treat faint positive lines the same way they treat darker ones: as a signal worth confirming.
What Window Periods Have to Do With Faint Lines
Another factor that can influence rapid test results is the window period. This is the amount of time between a possible exposure and when a test can reliably detect infection.
During the earliest stage of infection, the biological markers that tests detect may still be building. If a test is taken during this early phase, the signal may appear faint because only a small amount of the marker is present.
This doesn't mean that the answer is wrong. It just shows where the infection is on its timeline.
| Infection | Typical Detection Window | Why Timing Matters |
|---|---|---|
| HIV | 2 to 6 weeks for most rapid antibody tests | Antibodies must develop before detection |
| Syphilis | 3 to 6 weeks | Immune response builds gradually |
| Hepatitis B | 4 to 8 weeks | Antigens and antibodies increase over time |
If testing occurs very early after exposure, repeating the test later can provide a clearer result.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
A Quiet Truth About STD Testing Anxiety
Rapid tests are designed to empower people. They give individuals the ability to check their health privately and quickly. But that same privacy can create a strange emotional moment when the result is not immediately obvious.
People often describe staring at the test cassette longer than they planned to. They tilt it under different lights, zoom in with their phone camera, or compare it to pictures online. That reaction isn’t irrational. It’s the natural response to uncertainty about something personal and important.
“I kept refreshing forums looking for photos that looked like mine,” one patient admitted during a sexual health consultation. “Everyone’s faint line looked slightly different.”
The reality is that faint lines vary from test to test. What matters is not the exact shade or thickness of the line but whether it appeared during the correct reading window.
Testing at Home vs Testing in a Clinic
Both at-home testing and clinic-based testing serve important roles in sexual health care. Rapid tests provide immediate answers and privacy, while clinical testing can provide confirmatory results and access to treatment.
Many people start with an at-home test because it feels easier emotionally. Opening a package in a private space often feels less intimidating than scheduling an appointment.
If the result is negative, it can provide peace of mind. If the result is positive or unclear, a clinic visit can provide confirmation and medical guidance.
For those who want the option to test discreetly first, many people begin with the Combo STD Home Test Kit, which checks for several common infections using rapid testing technology.
The most important step isn’t where the test happens. It’s that testing happens at all.
FAQs
1. I’m staring at a faint line right now. Does that count as positive?
If a second line shows up during the official reading time, even if it’s pale or barely there, most rapid STD tests consider that a positive reaction. The line doesn’t have to be bold to count. The chemistry in the strip only produces that line when it detects the marker it’s designed to find. When people feel unsure, the usual next step is simple: repeat the test or confirm it with a clinic test so you’re not left guessing.
2. Why would the line be so faint instead of dark?
Rapid tests react to how much of a marker is in the sample at that moment. If there’s less of it, the reaction can look lighter. Think of it like adding a drop of food coloring to water versus a full squeeze, the signal is still there, just softer. Hydration, sample variation, and where your immune system is in its response can all influence how bold that line appears.
3. Could my eyes be tricking me?
Honestly, this happens a lot. People tilt the test under different lights, take phone photos, or hold it up to the window trying to figure out if the line is real. Good lighting helps, neutral light usually makes faint lines easier to see. If the line is visible without squinting and it appeared during the correct time window, it’s generally treated as a real result.
4. What if the line appeared later, like after half an hour?
That’s where things get murkier. Rapid tests are designed to be read within a specific time window, often around 10–15 minutes. After that, the strip starts drying out, and faint marks can appear that aren’t true reactions. Those are called evaporation lines, and they’re one reason instructions always warn people not to read the test too late.
5. Does a darker line mean the infection is worse?
No. A darker line doesn’t mean anything about severity. Rapid tests aren’t measuring how “bad” an infection is, they’re only detecting whether certain markers are present. Someone with a faint line and someone with a dark line could have the exact same infection.
6. I tested really soon after a hookup. Could that make the line faint?
It can. Many STDs have what’s called a window period, the time between exposure and when tests can reliably detect the infection. Early in that window, the markers tests look for may just be starting to appear. Sometimes that produces a lighter signal, which is why repeating the test later can provide confirmation.
7. What if my test only shows one line?
Most of the time, if you only see the control line and not the test line, the result is negative. The control line just shows that the test worked as it should have. If that control line doesn’t appear at all, though, the result is considered invalid and the test should be repeated.
8. How common are faint lines on rapid STD tests?
Honestly, it happens a lot. Rapid tests are built to be very sensitive, so they can catch even small amounts of the markers they’re looking for. That’s helpful for early detection—but it also means the line doesn’t always show up bold and unmistakable.
9. Should I panic if I see a faint line?
No. A faint line isn’t a crisis, it’s just a signal that deserves confirmation. Many people simply repeat the test or visit a clinic for a follow-up test. The goal isn’t to scare anyone; it’s to replace uncertainty with clear information.
10. What's the best thing to do next after a faint result?
Treat it as a result worth checking again. That might mean repeating the test after the recommended window period or confirming it with a clinic test. Most infections are manageable when caught early, and testing is the step that moves you from guessing to knowing.
You Deserve Clarity, Not Guesswork
Seeing a faint line on an STD rapid test can feel oddly unsettling. It’s not a bold answer, and it leaves your brain searching for certainty. But rapid tests aren’t designed to create dramatic visuals, they’re designed to detect biological signals. Even a subtle line is your body’s chemistry interacting with the test.
The goal isn’t to panic over every shade of pink. The goal is to remove uncertainty. If the line appeared within the reading window, treat it as a result worth confirming. Retest after the appropriate window period if needed, or follow up with a clinic test to get a definitive answer.
And if testing privately feels easier, start there. A discreet screen like the Combo STD Home Test Kit can check for several common infections without leaving home. Your results are private, your timeline is yours, and clarity almost always feels better than guessing.
How We Sourced This Article: This guide draws on clinical guidance for rapid diagnostic testing, standard protocols for STD screening, and peer-reviewed research on lateral flow tests. To keep everything accurate, we compared the information against medical studies and public health resources. We focused on how these tests work in real life—how long they take to detect infections, how reliable they are, and how to read the results correctly. The material comes from established research institutions and public health organizations that study infectious disease and diagnostic testing.
Sources
1. Centers for Disease Control and Prevention – Sexually Transmitted Infections Overview
2. Fact Sheet on Sexually Transmitted Infections from the World Health Organization
4. CDC: Guidelines for Treating Sexually Transmitted Infections
5. U.S. FDA – Home Use Diagnostic Tests Overview
6. World Health Organization – Guidelines on HIV Self-Testing and Rapid Diagnostics
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on sexually transmitted infection diagnosis, testing technology, and prevention. His work blends clinical accuracy with clear, stigma-free communication so readers can understand their sexual health without confusion or judgment.
Reviewed by: Board-Certified Infectious Disease Specialist | Last medically reviewed: March 2026
This article is only meant to give you information. It shouldn't be used instead of professional medical advice, diagnosis, or treatment.










