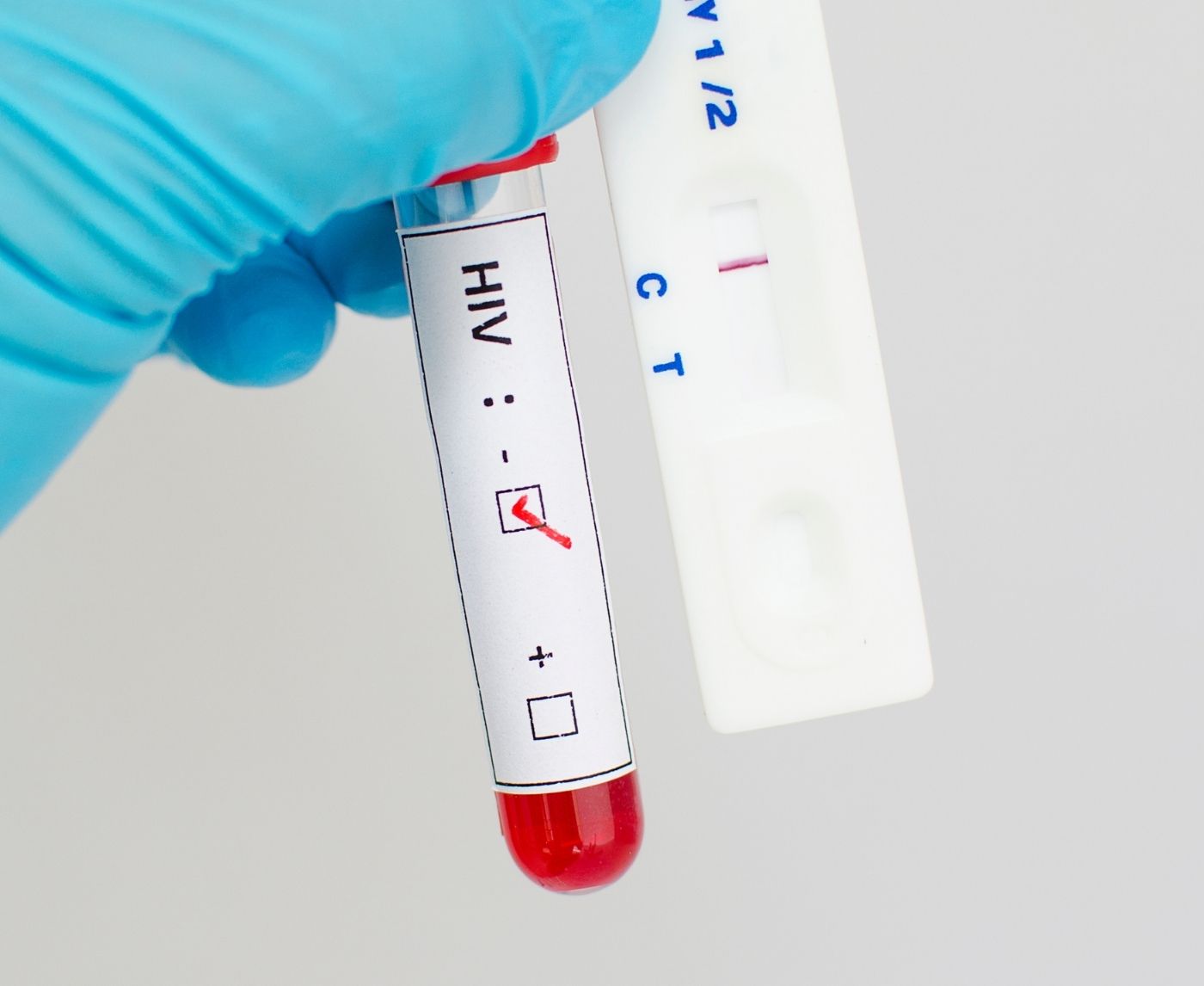
Quick Answer: Antivirals don't often give false negatives on STD tests, but they can change the time frame for some infections, like HIV or herpes. If you test too soon, especially if you're on PrEP, PEP, or suppressive therapy, you may need to take another test to be sure.
This Fear Is More Common Than You Think
“I tested negative, but I’m on PrEP. What if it delayed the result?”
“I started valacyclovir right away. Did that mess up my herpes blood test?”
“I took antibiotics before I got tested for chlamydia. Did I ruin the test?”
I hear versions of this weekly. The fear usually isn’t about the science, it’s about control. People want certainty. They want to know their negative result means negative, not “maybe negative.”
Here’s the grounded truth: modern STD testing, especially NAAT (nucleic acid amplification tests) for bacterial infections and antigen/antibody testing for HIV, is highly sensitive. Antivirals and antibiotics generally do not create false reassurance out of thin air. But the timing of when you test, especially during active treatment or immediately after exposure, can affect how early an infection becomes detectable.
Let’s break it down clearly, without panic and without oversimplification.
How STD Tests Actually Detect Infection (And Why Timing Matters)
There are different ways to find different kinds of infections. Some tests look for genetic material from the virus or bacteria themselves. Others look for your body’s immune response, antibodies that develop over time. This difference is why window periods exist at all.
When people ask about STD test accuracy while on medication, they’re usually thinking about one of three categories:
| Infection Type | Common Test Type | What the Test Detects | Could Antivirals Affect Timing? |
|---|---|---|---|
| Chlamydia & Gonorrhea | NAAT / PCR | Actual bacterial DNA | Rarely; antibiotics may clear infection before testing |
| HIV | Antigen/Antibody or RNA | Viral protein (p24), antibodies, or viral RNA | Possible minor timing shifts on PrEP, PEP, or ART |
| Herpes (HSV-1 & HSV-2) | Swab PCR or antibody blood test | Viral DNA (swab) or antibodies (blood) | Antivirals may reduce viral shedding but rarely block antibody formation |
| Hepatitis B & C | Antibody & antigen tests | Immune response or viral markers | Antivirals typically do not prevent detection |
Table 1. How different STD tests detect infection and whether antivirals meaningfully alter detection timing.
The key insight here: medications do not usually “hide” infections. They may reduce viral replication or bacterial load, but modern tests are designed to detect very small amounts of genetic material or immune response.
The bigger issue? Testing before your body, or the pathogen, has reached detectable levels.
People are also reading: Think It’s Just a Cold Sore? Why It Might Be Genital Herpes
HIV: The Situation Where Timing Questions Get Loudest
If you’re on PrEP, PEP, or HIV treatment (ART), your question makes sense. These medications directly suppress viral replication. So could they delay detection?
Here’s what we know from current infectious disease guidance and published studies:
PrEP does not prevent HIV antibodies from forming if infection occurs, but it may delay the earliest stages of viral replication. That means extremely early RNA detection could theoretically shift by days to a couple of weeks. It does not make long-term infection invisible.
PEP is different. Because it’s started after potential exposure, it can suppress early viral replication if taken correctly. Testing is therefore scheduled at specific intervals, often immediately, then at 4–6 weeks, and again at 3 months, to rule out delayed seroconversion.
ART (treatment for people already diagnosed) suppresses viral load to undetectable levels, but that does not cause false negative antibody tests. Antibodies remain present even if viral load becomes undetectable.
| Scenario | Does It Cause False Negatives? | Retest Recommendation |
|---|---|---|
| On PrEP, tested 10 days after exposure | Possible early false reassurance if too soon | Retest at 4–6 weeks and 3 months |
| Completed 28 days of PEP | Unlikely long-term false negative, but delayed detection possible | Test at 4–6 weeks post-PEP and at 3 months |
| On long-term ART | No false negative antibody tests expected | Routine viral load monitoring per provider |
Table 2. HIV testing timing considerations while on PrEP, PEP, or ART.
This is why “false negative HIV test on PrEP” searches spike online. It’s not that the medication hides infection. It’s that people often test during the window period, sometimes within days of exposure, when no test on Earth could confidently detect it yet.
If you’re in that window and your anxiety is climbing, structured retesting, not repeated daily testing, is what gives clarity.
If you need private testing that fits those retesting intervals, you can explore options at STD Rapid Test Kits, including discreet at-home options designed around recommended windows.
Herpes Antivirals: Do Acyclovir or Valacyclovir Affect Test Results?
If you’ve ever typed “does acyclovir affect herpes test?” into Google at midnight, you’re not alone. Herpes anxiety has a unique emotional charge because symptoms can be subtle, sporadic, or nonexistent. When someone starts suppressive therapy quickly, especially after a new exposure, they often worry they interfered with the test.
Let’s separate the two types of herpes testing, because this is where confusion explodes.
Swab tests (PCR) detect actual viral DNA from a sore. Blood tests detect antibodies your immune system produces after exposure. Antivirals like acyclovir or valacyclovir reduce viral replication and shedding, which can shorten outbreaks. But they do not erase antibodies once your body has produced them.
Here’s the nuance: if someone starts antivirals extremely early, during a first-ever infection, there is limited evidence suggesting antibody development could be slightly delayed. Not prevented. Delayed. That means testing very early after exposure (for example, 2–3 weeks) might not show antibodies yet, whether or not medication was involved.
In practical terms, suppressive therapy rarely causes a long-term false negative herpes blood test. The more common issue is testing before the standard 12–16 week window when antibodies reliably appear.
One patient once told me, “I started valacyclovir the day I felt tingling. My blood test at six weeks was negative. I thought the medication hid it.” When she retested at 16 weeks, the result was clear. The medication didn’t hide anything. The timing simply hadn’t matured.
This is why retesting schedules matter more than panic testing.
Antibiotics and Bacterial STDs: Can Treatment Hide Infection?
Now let’s talk about chlamydia and gonorrhea. NAAT or PCR tests, which look for bacterial genetic material directly, usually find these bacterial infections. So, can antibiotics make an STD test come back negative when it shouldn't?
Yes, but not the way people think.
You might be able to get rid of the infection completely or partially if you take antibiotics that work against the bacteria before the test. That could lead to a negative result, not because the test failed, but because the infection was treated. This is different from an antiviral masking a virus.
The real complication here is premature retesting. Testing too soon after finishing antibiotics can detect leftover bacterial fragments and produce confusing results. That’s why most guidelines recommend retesting for cure after about three weeks if clinically indicated, and routine retesting at three months due to reinfection risk.
Medication doesn’t “hide” these infections. It treats them. But incomplete treatment or reinfection can complicate interpretation.
And here’s the piece people don’t talk about enough: antibiotics may relieve symptoms before you ever test. That can create the illusion that you “imagined it.” Relief does not equal proof you were negative. It may simply mean the medication worked.
Check Your STD Status in Minutes
Test at Home with Remedium6-in-1 STD Rapid Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $119.00 $294.00
For all 6 tests
Can Medication Mask Symptoms but Not the Test?
This is one of the most important distinctions in this entire article.
Medications, antivirals, antibiotics, even anti-inflammatory drugs, can absolutely change how your body feels. They can reduce pain, suppress sores, shorten discharge duration, and calm swelling. That can make you think nothing was ever there.
But modern molecular tests are not reading your symptoms. They’re detecting viral RNA, bacterial DNA, or antibodies in your bloodstream. Symptom suppression does not equal test suppression.
In other words, medication may calm the surface story without changing the laboratory reality.
This is especially relevant for people on long-term herpes suppressive therapy. Daily valacyclovir reduces outbreaks and transmission risk, but it does not eliminate the underlying virus. If antibodies are present, they remain detectable. If you test outside the proper window period, you may simply be testing too early, not “too medicated.”
The Real Culprit: Testing During the Window Period
When people ask whether antivirals cause false negative STD tests, what they’re usually encountering is the window period, the time between exposure and when a test becomes reliably positive.
Here’s what that looks like in real life:
You had sex on a Saturday. By Wednesday, anxiety is peaking. You test on Friday. It’s negative. You’re on PrEP, so now you worry the medication interfered. But biologically, your body simply hasn’t had enough time to produce detectable markers.
This is why structured testing beats reactive testing.
| Infection | Earliest Possible Detection | Optimal Testing Window | Medication Impact? |
|---|---|---|---|
| Chlamydia | 7 days | 14 days | Antibiotics treat; do not mask NAAT if present |
| Gonorrhea | 7 days | 14 days | Similar to chlamydia |
| HIV | 10–14 days (RNA) | 4–6 weeks (Ag/Ab), 3 months definitive | PrEP/PEP may slightly delay earliest detection |
| Herpes | Swab during outbreak | 12–16 weeks (antibody) | Antivirals rarely delay antibodies significantly |
Table 3. Typical window periods and whether medication meaningfully alters detection.
Notice the pattern? The variability lies in timing, not concealment.
When Retesting Is the Smart Move
If you tested within the earliest possible detection window while on antivirals, the responsible next step is not spiraling, it’s scheduling a follow-up at the optimal window.
Retesting is especially important if:
You tested for HIV within two weeks of exposure while on PrEP or PEP. You tested for herpes antibodies before 12 weeks. You took antibiotics before testing for chlamydia or gonorrhea and aren’t sure whether infection cleared. Or you simply cannot calm your anxiety despite a negative early result.
Peace of mind sometimes requires confirmation.
If you need a discreet way to follow recommended retesting intervals, the Combo STD Home Test Kit allows structured follow-up testing without clinic scheduling delays. Clarity should be accessible, not complicated.
People are also reading: Using a Herpes Home Test Kit? Here’s How to Read the Results the Right Way
Edge Cases: When Antivirals Actually Can Shift Timing
Let’s talk about the scenarios that fuel the anxiety forums. Not the common ones, the rare ones. Because when someone Googles whether antivirals can cause a false negative STD test, they’re usually afraid they’re the exception.
There are a few clinical edge cases where timing shifts slightly. The key word is slightly.
HIV on PrEP or PEP: If exposure occurs while someone is taking PrEP inconsistently, or if PEP is started very early after exposure, viral replication may be partially suppressed in the earliest phase. This can delay RNA detection by days or, rarely, a few weeks. It does not erase infection long term. Antibody tests will still become positive if infection occurred.
Immediate Antiviral Use in Primary Herpes: Starting high-dose antivirals during the first-ever outbreak may, in rare cases, delay antibody development slightly. That means a 6-week blood test might be negative, while a 16-week test becomes positive. This is about immune timing, not test failure.
Immunosuppression: People with very weak immune systems, like those with advanced HIV who haven't gotten treatment yet, people who are getting chemotherapy, or people who have had a transplant, may not make antibodies for a long time. The delay is due to the immune system, not the antivirals themselves.
Notice the pattern again: these scenarios may shift detection timing. They do not permanently conceal infection from modern diagnostics.
What Infectious Disease Guidelines Actually Say
Instead of warning about how medications can make people invisible, major public health organizations always stress the importance of retesting at set times. The Centers for Disease Control and Prevention, the World Health Organization, and the most important infectious disease societies all say that people should get tested again after being exposed to HIV, especially because the window periods are different.
The language used in clinical guidance is careful. It focuses on delayed seroconversion in rare cases, not medication creating permanent false negatives. That distinction matters.
For example, HIV testing after PEP completion is recommended at 4–6 weeks and again at 3 months. This schedule accounts for theoretical delays in early detection, not evidence that antivirals hide infection indefinitely.
Similarly, herpes antibody testing is considered most reliable at 12–16 weeks post-exposure, regardless of suppressive therapy status.
The science community plans for timing variability. It does not operate on fear-based assumptions.
The Emotional Spiral: “What If I Messed Up My Test?”
Let’s pause the lab talk for a second.
I’ve had patients sit across from me and say, “I should’ve waited.” Or, “I shouldn’t have started medication.” Or, “I think I ruined the test.” The guilt is heavy. The self-blame is louder than the science.
You did not ruin your health by taking medication. You did not sabotage your diagnosis by seeking treatment. Acting quickly is responsible, not reckless.
Most false negative fears are about early testing, not about medication interference. When someone tests five or ten days after exposure and gets a negative result, their brain looks for an explanation if anxiety persists. Medication becomes the villain because it feels tangible.
But in reality, biology just needs time.
Check Your STD Status in Minutes
Test at Home with Remedium8-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $149.00 $392.00
For all 8 tests
How to Test Strategically While on Antivirals
If you’re currently on PrEP, PEP, suppressive herpes therapy, or even antibiotics, here’s what a structured testing approach looks like in practice.
| Situation | Immediate Action | Follow-Up Testing |
|---|---|---|
| Exposure while on PrEP | Test at 2–4 weeks | Repeat at 3 months for definitive result |
| Completed PEP | Test at end of PEP course | Repeat at 4–6 weeks and 3 months post-exposure |
| Started antivirals during first herpes outbreak | Swab active lesions if present | Blood test at 12–16 weeks |
| Took antibiotics before bacterial STD test | Wait at least 3 weeks before retesting for cure | Routine retest at 3 months |
Table 4. Structured testing timelines while on medication.
Notice that none of these rows say “testing won’t work.” They simply build in follow-up intervals that match biology.
If coordinating clinic visits feels overwhelming, especially during multi-step retesting, at-home options can make timing easier to control. Testing through STD Rapid Test Kits allows you to align testing with recommended windows without waiting room delays.
What a True False Negative Actually Looks Like
Let’s define this clearly. A true false negative means the infection is present and detectable, but the test fails to identify it despite proper timing. That scenario is rare with modern molecular testing.
Most “false negatives” fall into one of these categories:
Testing before the window period has closed. Testing the wrong site (for example, urine only when infection was oral). Not following test instructions correctly. Or testing after effective treatment cleared the infection.
Medication is usually not the cause.
Modern NAAT tests for chlamydia and gonorrhea are highly sensitive. Fourth-generation HIV tests detect both antigen and antibody. Herpes PCR swabs during active outbreaks are extremely accurate. These tools were designed to detect infection even at low levels.
The problem isn’t invisibility. It’s impatience.
FAQs
1. Okay, be honest. Can antivirals actually cause a false negative STD test?
Deep breath. In almost every real-world situation, no. Antivirals don’t magically cloak infections from modern lab technology. What they can do, very occasionally, is shift the earliest detection window by a bit. So if you tested super early, the issue probably isn’t the medication. It’s the calendar.
2. I’m on PrEP and tested negative 10 days after sex. Should I trust it?
At 10 days, even without PrEP, that’s early. PrEP doesn’t make HIV invisible, but it can slightly slow early viral replication. Translation? Test again at 4–6 weeks, then at 3 months. That’s not because something is wrong, it’s because biology has a schedule.
3. I started valacyclovir right away for a possible first herpes outbreak. Did I mess up my blood test?
You didn’t sabotage anything. Starting antivirals quickly is responsible. In rare first-time infections, antibody development can take longer, so a 6-week test might be negative while a 16-week test gives you the final answer. That’s timing, not test failure.
4. Can antibiotics hide chlamydia or gonorrhea from a test?
They don’t hide it, they treat it. If you took the right antibiotic, the bacteria may simply be gone by the time you test. That’s a cured infection, not a masked one. The bigger issue is retesting too soon after treatment and getting confusing results from leftover fragments.
5. What’s the biggest reason people think they have a false negative?
Testing inside the window period. It’s almost always that. You feel something. You panic. You test within days. It’s negative. Your brain goes, “It must be the medication.” Usually, it’s just that the infection, if present, wasn’t detectable yet.
6. Can medication reduce symptoms but not affect the test?
Absolutely. Antivirals can calm sores. Antibiotics can reduce discharge. Anti-inflammatory meds can dull pain. But PCR and antibody tests aren’t looking at how you feel, they’re looking for biological markers. Symptoms fading doesn’t equal infection disappearing overnight.
7. If I’m still anxious after a negative test, what’s the healthiest move?
Make a plan instead of retesting every few days. Pick the correct follow-up window. Put it on your calendar. Step away from symptom-googling. Structured retesting brings clarity. Panic testing fuels the spiral.
8. Does HIV treatment (ART) ever cause someone to test negative for antibodies?
No. Once antibodies are formed, they stay detectable, even if viral load becomes undetectable. Undetectable viral load means treatment is working, not that the immune response disappeared.
9. Is there any scenario where antivirals permanently hide an STD?
Not with modern testing. Medicine has evolved. Molecular diagnostics are extremely sensitive. The fear of permanent invisibility is understandable, but it’s not how the science works.
10. Why does this topic make people so anxious?
Because sexual health hits identity, trust, relationships, and shame all at once. Add a medication into the mix and it feels like you changed the outcome. You didn’t. You took care of yourself. Now you just need to test on the right timeline.
If You’re Still Worried, Here’s What Actually Helps
If you’ve made it this far, you’re probably not just curious, you’re anxious. Maybe you tested early while on PrEP. Maybe you started valacyclovir the second you felt tingling. Maybe you took antibiotics before you could get to a clinic. And now you’re wondering whether your negative result is solid.
Here’s the grounded reality: antivirals rarely create true false negative STD tests. What they can do, in limited situations, is shift early detection timing. That’s a planning issue, not a catastrophe. Structured retesting closes the gap.
You don’t fix anxiety by repeatedly testing inside the window period. You fix it by choosing the right window and sticking to it.
If you need a private, controlled way to retest according to recommended timelines, the Combo STD Home Test Kit allows you to follow up discreetly without waiting for appointments. Your health deserves clarity, not guesswork.
How We Sourced This Article: This guide combines the most up-to-date clinical advice from top public health organizations, peer-reviewed research on infectious diseases, and real-life experience giving patients advice.
Sources
2. CDC – Rules for Treating STDs
3. Fact Sheet on HIV from the World Health Organization
4. CDC – Recommendations for Managing Genital Herpes
5. CDC—Guidelines for Treating Chlamydia
6. CDC – Pre-Exposure Prophylaxis (PrEP)
7. CDC – Post-Exposure Prophylaxis (PEP)
8. Mayo Clinic – HIV Diagnosis and Treatment
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a no-nonsense, sex-positive approach and is committed to expanding access to accurate testing for all communities.
Reviewed by: A. Ramirez, PA-C | Last medically reviewed: March 2026
This article is only for information and should not be taken as medical advice.