Quick Answer: Painful ejaculation can happen because of prostatitis, infections such as chlamydia or gonorrhea, pelvic floor muscle tension, urethral inflammation, or prostate disorders. If ejaculation suddenly becomes painful, especially alongside burning urination or pelvic discomfort, doctors often recommend medical evaluation and STD testing.
When Pleasure Turns Sharp Instead
A man named Daniel once described the moment he first noticed it. He had been seeing someone new for a few weeks, and everything felt normal until one night when orgasm came with a sudden burning sensation that ran through the penis and into the lower abdomen. It was brief but strong enough to make him pause and wonder if something had gone wrong.
Over the next few days the sensation appeared again during masturbation. It was not unbearable, but it was uncomfortable enough to turn a routine moment into something filled with quiet concern. By the time Daniel searched online for “why does ejaculation hurt,” he had already convinced himself it might be an STD.
This reaction is extremely common. Ejaculation involves the coordinated contraction of muscles, the prostate gland, seminal vesicles, and the urethra. When any part of that chain gets angry or inflamed, the body can think of the contraction as pain instead of pleasure.
Doctors often explain that ejaculation is actually a complex reflex involving nerves in the pelvis and spinal cord. Semen moves through several structures during orgasm, and inflammation anywhere along that pathway can create discomfort. Understanding those pathways helps explain why painful ejaculation can have multiple causes rather than a single diagnosis.
The Anatomy Behind Ejaculation Pain
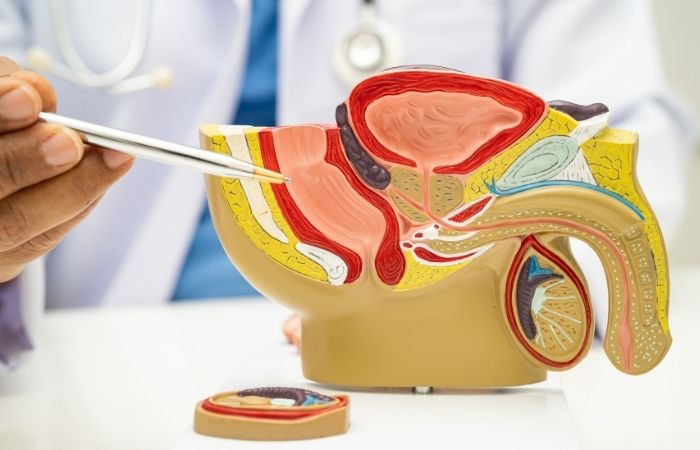
It helps to picture what the body is doing during orgasm to understand why ejaculation can hurt. The prostate gland contracts in a rhythmic way, which pushes semen into the urethra. The muscles in the pelvic floor contract in waves, which helps push out semen. At the same time, nerves all over the pelvis quickly send signals to muscles to move and feel.
If one component of this system becomes irritated, the contractions that normally feel pleasurable can trigger pain instead. Inflammation inside the prostate can create pressure during those contractions. Infection in the urethra can cause burning as semen passes through. Tight pelvic muscles can squeeze nerves or tissues that are already sensitive.
Doctors sometimes describe painful ejaculation as a signal rather than a disease itself. The symptom tells you that something in the pelvic system is inflamed, irritated, or under stress. Identifying which structure is involved is the key step toward solving the problem.
The table below summarizes several of the most common causes doctors investigate when someone reports pain during orgasm.
| Condition | What Happens in the Body | Typical Symptoms |
|---|---|---|
| Prostatitis | Inflammation of the prostate gland | Pelvic pain, painful ejaculation, urinary discomfort |
| Urethritis | Inflammation of the urethra often from infection | Burning urination, discharge, ejaculation pain |
| Sexually transmitted infections | Bacterial infection affecting reproductive tract | Painful ejaculation, discharge, testicular discomfort |
| Pelvic floor dysfunction | Chronic tension in pelvic muscles | Pelvic pressure, painful orgasm, urinary symptoms |
| Prostate disorders | Structural changes or enlargement | Pelvic pressure, ejaculation discomfort |
One important detail often surprises people. Not all instances of painful ejaculation are associated with sexually transmitted infections. Many patients assume that discomfort automatically means they caught something during sex, but inflammation from prostate issues or pelvic muscle tension can produce nearly identical symptoms.
Still, infections remain a key possibility, which is why doctors usually rule them out early. Testing provides clarity and prevents untreated infections from causing further irritation in the reproductive tract.
People are also reading: Sharing Razors, Cuts, and STD Fears: What’s Real and What’s Not
The Role of Prostatitis in Painful Ejaculation
Among the most common explanations doctors find is prostatitis. The prostate gland sits just below the bladder and surrounds part of the urethra, making it a central structure during ejaculation. When the prostate becomes inflamed, every contraction during orgasm can press against irritated tissue.
Prostatitis is a broad term that refers to a variety of issues. In some cases, bacteria cause the problem, and in others, long-term inflammation without a clear infection does. In both cases, the gland becomes sensitive, and doing things that involve the prostate can hurt.
A patient once described it as a deep ache that arrived right before ejaculation and lingered afterward. Another explained that orgasm felt normal at first, then suddenly turned into a sharp pressure behind the penis. Doctors recognize these descriptions immediately because they appear so frequently in prostatitis cases.
Researchers estimate that prostatitis symptoms affect millions of men worldwide. The condition can appear in younger adults as well as older patients, and it often overlaps with urinary symptoms such as burning during urination, difficulty starting a stream, or persistent pelvic tension.
While the symptoms can feel alarming, most cases respond well to treatment. Antibiotics may be used if bacteria are present, while anti-inflammatory therapies, hydration, and pelvic floor relaxation techniques can help reduce irritation in non-infectious cases.
What makes prostatitis tricky is that it sometimes appears without obvious warning signs. Someone may feel completely healthy except for a sudden change in how ejaculation feels. That is one reason doctors take painful orgasm seriously even when other symptoms are mild.
When an Infection Is the Hidden Cause
For many people, the first fear after painful ejaculation is the possibility of a sexually transmitted infection. That fear is understandable. Several infections can inflame the urethra or reproductive tract, and when semen passes through those irritated tissues, the result can be burning, stinging, or pressure during orgasm.
Doctors often consider infections early in the diagnostic process because they are both common and treatable. Bacteria such as Chlamydia and Gonorrhea can infect the urethra, prostate, or epididymis. When those tissues swell, the pathways that semen travels during ejaculation become irritated, making the final moment of orgasm feel unexpectedly painful.
A man named Luis once walked into a clinic after noticing that ejaculation had begun to sting sharply near the tip of his penis. At first he assumed it was dehydration or irritation from friction. But when the burning sensation appeared during urination as well, he realized something else might be happening.
Testing eventually revealed urethritis caused by Chlamydia. After treatment with antibiotics, the burning sensation disappeared within weeks. Stories like this are one reason doctors often recommend testing when painful ejaculation appears suddenly, especially after a new sexual partner.
The infections most often associated with ejaculation pain affect the urethra or prostate. When inflammation develops, the muscular contractions that normally move semen through the reproductive tract can cause irritation in already sensitive tissue.
| Infection | How It Causes Pain | Other Possible Symptoms |
|---|---|---|
| Chlamydia | Inflames the urethra and reproductive tract | Burning urination, discharge, pelvic discomfort |
| Gonorrhea | Causes urethral inflammation and infection | Painful urination, discharge, testicular pain |
| Trichomoniasis | Irritates the urethra and genital tract | Itching, mild discharge, urinary irritation |
| Prostate infection | Inflammation within the prostate gland | Pelvic pain, painful ejaculation, urinary difficulty |
It is important to understand that infections do not always cause obvious symptoms right away. Many people carry bacteria for days or weeks before noticing anything unusual. In those situations, painful ejaculation may be one of the first clues that inflammation has begun inside the reproductive tract.
Testing helps remove the uncertainty. A discreet home test kit or clinic test can detect infections quickly, allowing treatment to begin before the irritation spreads or worsens.
If you are worried about infection after experiencing symptoms, you can learn more about testing options at STD Rapid Test Kits. Their at-home combo STD test kit screens for several common infections, helping people get answers privately without waiting for a clinic appointment.
For a lot of patients, just ruling out infections can be a huge relief. If tests show that bacteria are present, doctors can start treatment or look into other possible causes if the results come back negative.
Pelvic Floor Tension: The Cause People Rarely Expect
Not every case of painful ejaculation begins with infection or prostate disease. In fact, many doctors now recognize pelvic floor tension as a surprisingly common contributor. The pelvic floor is a group of muscles that support the bladder, rectum, and reproductive organs. Those muscles contract in a rhythm during orgasm to help get rid of sperm.
If the pelvic muscles remain chronically tight or overactive, those contractions can squeeze surrounding nerves and tissues. Instead of smooth rhythmic pulses, the body experiences a sensation closer to cramping or pressure.
A patient named Kareem once described it as a deep ache that appeared right before ejaculation and lingered afterward. His tests for infection were completely normal. Eventually a urologist suggested pelvic floor therapy, which focuses on teaching the muscles to relax instead of constantly tightening.
After a few weeks of focused physical therapy, the pain went away. Kareem later said that he had been clenching his pelvic muscles for years without realizing it during stressful days at work and hard workouts. He didn't realize that the tension had slowly crept into their sexual activity.
This kind of muscular tension often develops gradually. Stress, heavy lifting, cycling, and prolonged sitting can all contribute. The pelvic floor gets too protective over time and tightens even when it would be better to let go.
Doctors increasingly refer patients with unexplained pelvic pain or ejaculation discomfort to pelvic floor specialists. These therapists use breathing exercises, manual therapy, and posture adjustments to help muscles release chronic tension.
The concept can feel surprising at first. Many people expect sexual pain to come from infection or injury, not from muscles that have quietly stayed tight for too long. But once patients understand how the pelvic floor participates in orgasm, the connection begins to make sense.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
When Ejaculation Pain Appears Suddenly
Sudden pain during ejaculation often creates the most anxiety. When something changes quickly in the body, people worry that a serious condition may be developing. While that possibility should never be ignored, doctors emphasize that abrupt symptoms often have manageable explanations.
Temporary inflammation from dehydration, intense sexual activity, or mild irritation can occasionally cause short-term discomfort. For example, someone who has not ejaculated in a long time may experience stronger contractions that feel unusual or slightly uncomfortable.
However, persistent or recurring pain deserves attention. When symptoms continue for days or weeks, doctors begin investigating patterns. Does the pain appear only during ejaculation, or does it also occur during urination? Is there pelvic pressure afterward? Has there been a recent sexual exposure that could introduce infection?
These questions help narrow down possible causes. In a lot of cases, a few simple tests and a physical exam can quickly figure out if the problem is an infection, inflammation of the prostate, or muscle tension.
Most importantly, painful ejaculation is rarely something people need to simply tolerate. The body is signaling irritation somewhere in the pelvic system, and identifying that signal early can prevent longer-term discomfort.
Other Medical Conditions Doctors Sometimes Find
While prostatitis, infections, and pelvic muscle tension account for many cases, doctors occasionally uncover other conditions when investigating painful ejaculation. The reproductive system is complex, and several structures participate in the process of orgasm. When even one of those structures becomes irritated, the sensation can change dramatically.
One possible contributor is inflammation of the seminal vesicles. These small glands sit behind the prostate and produce a large portion of the fluid that becomes semen. When they become inflamed, the pressure created during ejaculation can feel uncomfortable or sharp. The pain may appear deep in the pelvis rather than directly in the penis.
Another possibility involves the epididymis, the coiled tube attached to each testicle that stores and transports sperm. If the epididymis becomes inflamed, the discomfort may radiate into the testicles or lower abdomen during orgasm. Some patients describe a heavy, aching sensation that develops shortly after ejaculation.
Occasionally doctors also evaluate whether medications or nerve irritation might play a role. Certain drugs can alter nerve signaling in the pelvis, and rare neurological conditions can change how orgasmic contractions are perceived. These cases are far less common, but they remain part of the broader diagnostic picture when symptoms do not fit the usual patterns.
Most patients feel relieved once a doctor explains how many structures participate in ejaculation. What initially feels mysterious begins to make sense once the anatomy and nerve pathways are understood.
| Condition | What Happens | Where Pain May Be Felt |
|---|---|---|
| Seminal vesicle inflammation | Glands producing semen become irritated | Deep pelvic pain during ejaculation |
| Epididymitis | Inflammation in sperm storage tubes | Testicular ache or pressure after orgasm |
| Nerve irritation | Pelvic nerves transmit pain signals | Sharp or electric pelvic sensations |
| Medication side effects | Certain drugs alter nerve responses | General pelvic discomfort during orgasm |
Although these conditions appear less frequently than prostatitis or infection, they highlight an important point. Painful ejaculation is not a single disease. Instead, it is a symptom that signals irritation somewhere along the pathway semen travels during orgasm.

People are also reading: Are STD Risks in Public Bathrooms Real? Let’s Break Down the Facts
When Should You Get Checked?
Many people hesitate before speaking to a doctor about sexual symptoms. The topic can feel awkward, and some worry they might be overreacting to a temporary issue. But physicians who specialize in urology and sexual health consistently emphasize that painful ejaculation is a legitimate reason to seek evaluation.
One patient once told his doctor he waited nearly three months before mentioning the symptom. During that time he avoided intimacy, searched endlessly online, and quietly worried about serious illness. When he finally scheduled an appointment, the diagnosis turned out to be mild prostatitis that responded quickly to treatment.
Situations like this happen frequently because people underestimate how common pelvic health issues are. In reality, doctors discuss symptoms like painful ejaculation every day. The conversation is routine from a medical perspective, even if it feels personal for the patient.
There are a few times when doctors strongly suggest getting a medical evaluation. If you have pain that doesn't go away after a week or two, you should see a doctor. If you have fever, burning in your urine, pelvic pressure, or strange discharge, you should get help right away.
Another important moment to seek testing is after a new sexual exposure. If ejaculation suddenly becomes painful following unprotected sex or contact with a new partner, doctors often recommend screening for infections to rule out treatable causes.
Testing today is much easier than many people realize. Clinics offer quick urine or swab tests, and some individuals prefer the privacy of home testing kits that allow them to collect samples discreetly and mail them to certified laboratories.
Understanding when to test can help remove uncertainty. The table below summarizes typical situations where doctors recommend screening for infection when ejaculation becomes painful.
| Situation | Why Testing Helps | What Doctors Look For |
|---|---|---|
| Pain after new sexual partner | Possible exposure to infection | Chlamydia, gonorrhea, other bacterial STDs |
| Pain with burning urination | Urethral inflammation may be present | Urethritis or urinary infection |
| Discharge or genital irritation | Common symptom of infection | Bacterial STDs or trichomoniasis |
| Persistent unexplained symptoms | Ruling out infection clarifies diagnosis | Multiple infections affecting the urethra |
Once testing is complete, the next steps become clearer. If an infection is present, treatment can begin quickly. If tests return negative, doctors can shift their focus toward prostate inflammation, pelvic muscle tension, or other noninfectious causes.
The uncertainty that often comes with painful ejaculation starts to go away when guesswork is replaced with reliable information.
What Usually Helps Painful Ejaculation Improve
Once doctors identify the likely cause of painful ejaculation, treatment often becomes straightforward. The most important change for many patients is realizing that their bodies are reacting to inflammation and not permanent damage. Most of the time, the tissues that are involved are just irritated, not broken.
If infection is present, antibiotics typically resolve symptoms once the bacteria are cleared. Patients often say that the burning or sharp feeling goes away a few days after they start treatment. Even if your symptoms get better quickly, it's still important to finish the whole course of medication. This is because infections that aren't completely healed can come back.
If prostatitis is to blame, doctors may suggest a mix of anti-inflammatory drugs, drinking a lot of water, and sometimes short courses of antibiotics, depending on the type. Taking warm baths and doing pelvic relaxation exercises can also help lower the pressure in the prostate and the tissues around it.
Pelvic floor dysfunction requires a slightly different approach. Patients often do better with specialized physical therapy that focuses on retraining the muscles of the pelvis instead of just taking medicine. The goal is to teach those muscles to relax instead of getting tighter all the time.
Mateo, a patient, once said that the most surprising thing about therapy was learning how much stress he had in his body. He didn't realize it, but sitting at a desk for long hours had made his pelvic muscles tighter. The pain during ejaculation slowly went away after he started doing breathing exercises and specific stretches.
These experiences reinforce an important message: painful ejaculation is usually a solvable problem once the cause becomes clear. Identifying that cause simply requires a willingness to investigate the body’s signals instead of ignoring them.
Check Your STD Status in Minutes
Test at Home with Remedium8-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $149.00 $392.00
For all 8 tests
The Emotional Side of Sexual Symptoms
Physical symptoms rarely exist in isolation. Sexual health concerns often carry emotional weight as well, especially when the symptom appears suddenly. Pain during ejaculation can make intimacy feel stressful, even for people who normally feel confident about their sexual health.
Some individuals begin avoiding sex or masturbation entirely while trying to figure out what is happening. Others quietly search the internet late at night, comparing symptoms and imagining worst-case scenarios. That anxiety is understandable, but it can also amplify physical tension in the body.
Doctors who work in sexual health often remind patients that the body and mind influence each other closely. Anxiety can increase muscle tension in the pelvis, which in turn may worsen discomfort during orgasm. Breaking that cycle sometimes requires both medical care and reassurance.
Talking openly with a healthcare professional can make an enormous difference. Patients start to feel better when they learn that painful ejaculation has known causes and treatment options. What used to be a mystery is now a health problem that can be dealt with.
FAQs
1. Is painful ejaculation normal?
No, ejaculation should not typically cause pain. Occasional mild discomfort may happen temporarily, but persistent pain during orgasm often signals inflammation, infection, or pelvic muscle tension that should be evaluated.
2. Can an STD cause painful ejaculation?
Yes. Chlamydia and gonorrhea are two infections that can cause swelling in the urethra and reproductive tract. This can cause pain or a burning feeling when you get there.
3. Does prostatitis make ejaculation hurt?
It can. Prostatitis involves inflammation of the prostate gland, and the contractions that occur during orgasm can press against that irritated tissue, producing pain or pressure.
4. Why does ejaculation burn sometimes?
Burning during ejaculation often happens when the urethra is inflamed. This inflammation can result from infection, irritation, or sometimes prostate issues affecting the reproductive tract.
5. Can stress cause painful ejaculation?
Yes, in a way. Your pelvic floor muscles can get tight if you are stressed for a long time. These muscles are so tight that it might be hard for you to get up.
6. Should I get tested for an STD if ejaculation hurts?
You should get tested if you suddenly have painful ejaculation, especially if you just got a new sexual partner or if you have other symptoms like burning urination or discharge.
7. How long should painful ejaculation last before seeing a doctor?
If the pain doesn't go away after a week or two, you should see a doctor. If you have pain that won't go away, it could be a sign of infection or inflammation that you shouldn't ignore.
8. Can dehydration or frequent sex cause ejaculation pain?
Temporary irritation from dehydration or intense sexual activity can occasionally cause mild discomfort. However, recurring pain should still be evaluated to rule out infection or prostate inflammation.
9. Can pelvic floor therapy help painful ejaculation?
Yes. If tight pelvic muscles are making your symptoms worse, pelvic floor therapy can help relax those muscles and make orgasms less painful.
10. Can painful ejaculation go away on its own?
Sometimes it can. Dehydration, intense sexual activity, or mild inflammation may cause temporary irritation that goes away in a few days. But if the pain keeps returning or lasts longer than a week or two, doctors recommend getting checked to rule out infection, prostatitis, or pelvic floor tension.
You Deserve Answers, Not Uncertainty
Pain during ejaculation can feel confusing, even a little alarming. One moment everything feels normal, and the next your body sends a signal that something in the system isn’t quite right. The goal isn’t to panic about every new sensation. The goal is to understand what your body is trying to tell you.
If the pain appeared after a new sexual partner, testing can quickly rule out infections. Doctors often check for prostate inflammation or pelvic floor tension if STD tests come back negative but the pain doesn't go away. Each step narrows the possibilities and replaces guesswork with real answers.
You don’t have to wait in uncertainty. If infection could be part of the picture, start with a private screen like the Combo STD Home Test Kit. The process is discreet, the results are confidential, and understanding what’s happening in your body brings far more relief than wondering.
How We Sourced This Article: This article combines clinical guidance on painful ejaculation, prostatitis, and sexually transmitted infections with peer-reviewed urology research. We looked at medical research on urethritis, pelvic floor dysfunction, and prostate inflammation, as well as advice from public health organizations. The goal was to give accurate medical information and explain the science in a way that is easy to understand and doesn't make people feel bad about themselves.
Sources
1. Centers for Disease Control and Prevention – Chlamydia Fact Sheet
2. Centers for Disease Control and Prevention – Gonorrhea Fact Sheet
3. Mayo Clinic – Prostatitis Overview
4. World Health Organization – Sexually Transmitted Infections Fact Sheet
5. Cleveland Clinic – Prostatitis
7. MSD Manual Consumer Version – Prostatitis
8. Merck Manual Professional Edition – Prostatitis
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. His work centers on making sexual health information accessible, stigma-free, and grounded in current clinical research.
Reviewed by: Michael R. Levin, MD, Urology | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.










