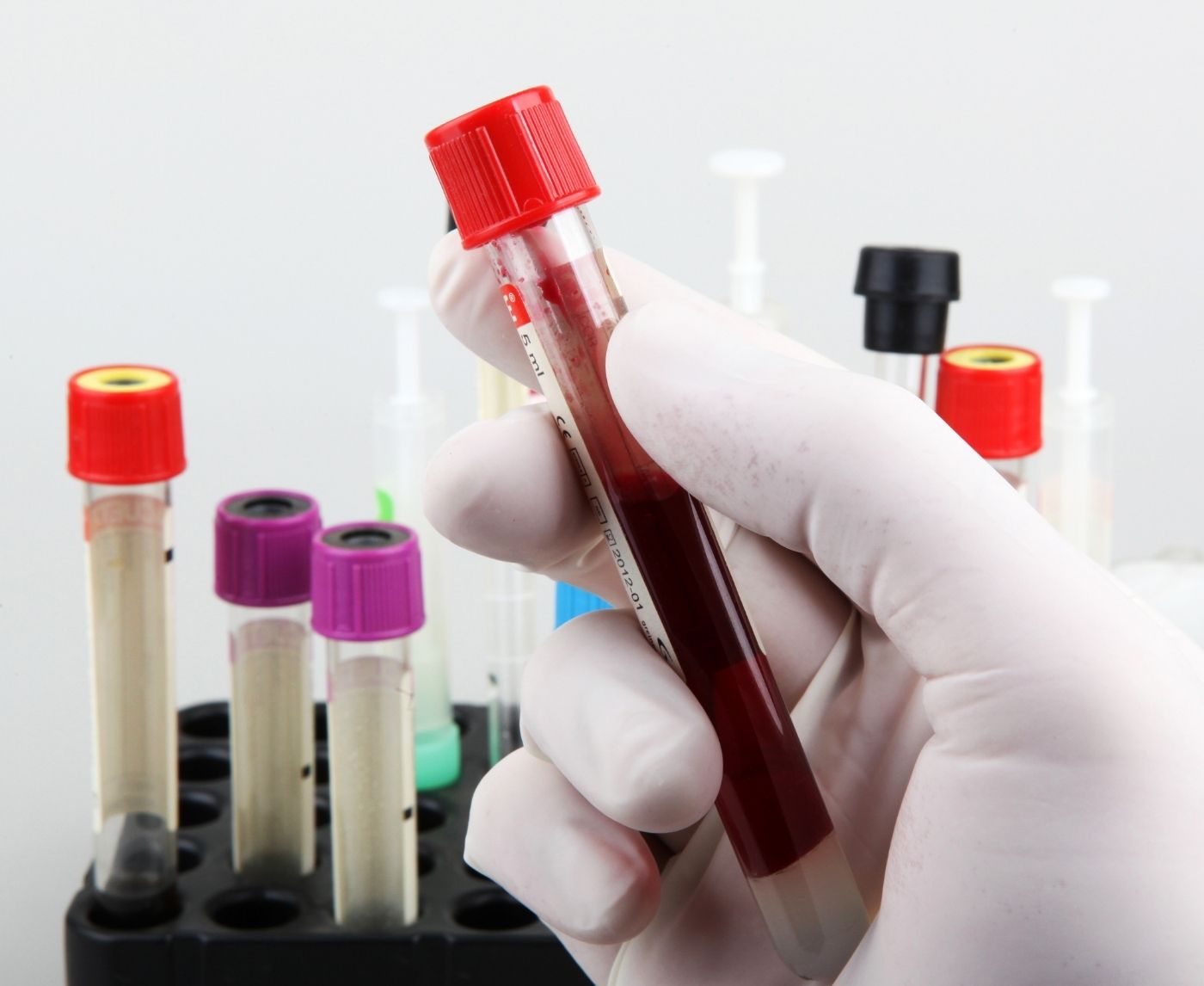
Quick Answer: Doctors test for multiple STDs at once because symptoms overlap, co-infections are common, and many STDs show no symptoms at all. Testing broadly protects you from missed diagnoses and delayed treatment.
One Symptom Doesn’t Equal One Infection
Here’s what most people assume: one exposure leads to one infection. One symptom means one disease. That’s how colds work. That’s how strep throat works.
But STDs don’t play by that logic.
Chlamydia and gonorrhea often look nearly identical in the body. Both can cause burning urination, discharge, pelvic pain, or absolutely nothing at all. Trichomoniasis can mimic yeast infections. Early syphilis can look like a harmless sore. HIV can resemble the flu.
And here’s the part no one explains clearly: you can absolutely have more than one STD at the same time.
Co-infection isn’t rare. It’s common enough that public health screening guidelines routinely recommend testing for multiple infections when one is suspected. Why? Statistically, if someone has one bacterial STD, their chances of getting another one go up a lot because of shared risk pathways.
It’s not about judgment. It’s about probability.
Why Doctors Prefer a Panel Instead of a Single Test
When you ask for “just a chlamydia test,” your provider is thinking bigger than that moment. They’re thinking about missed diagnoses, untreated infections, and silent transmission.
Let’s look at what happens if testing is too narrow.
| Scenario | What the Patient Thinks | Clinical Risk | What Broader Testing Prevents |
|---|---|---|---|
| Burning urination | “It must be chlamydia.” | Could also be gonorrhea or trichomoniasis | Missed co-infection and reinfection risk |
| Genital sore | “It’s probably irritation.” | Could be herpes or early syphilis | Delayed treatment and transmission |
| No symptoms but new partner | “I feel fine.” | Asymptomatic infection | Silent spread to partners |
| One positive result | “That explains everything.” | Second infection untreated | Comprehensive treatment plan |
This is why the phrase “STD panel vs single test” matters. A panel doesn’t assume. It checks.
From a public health perspective, comprehensive testing reduces long-term complications like pelvic inflammatory disease, infertility, and chronic infection. From your perspective, it prevents that awful moment three weeks later when symptoms don’t resolve because something was missed.
People are also reading: I Think I Gave My Partner Chlamydia, What Do I Say Now?
Yes, You Can Have Multiple STDs at Once
A 24-year-old patient once said, “I tested positive for gonorrhea. They told me I also had chlamydia. I thought that was impossible.” It wasn’t.
Chlamydia and gonorrhea frequently co-occur. Studies consistently show overlapping infection rates because they spread the same way, infect the same tissues, and often travel together through sexual networks. If exposure happens, exposure rarely comes labeled with a single pathogen.
And it’s not limited to bacterial infections.
Someone with genital herpes can also contract chlamydia. A person with untreated syphilis may also carry HIV. In fact, certain infections increase biological susceptibility to others because inflammation makes transmission easier.
That’s the clinical reality behind the question “can you have more than one STD?” The answer isn’t dramatic. It’s simply yes.
The Overlap Problem: Symptoms Don’t Stay in Their Lane
Here’s where things get messy.
Most STD symptoms overlap. Discharge doesn’t come color-coded by pathogen. Burning doesn’t identify itself. A rash doesn’t announce whether it’s viral or bacterial.
Many people Google “symptoms of multiple STDs” because their experience doesn’t fit neatly into one description. That confusion is valid. Overlapping STD symptoms are the rule, not the exception.
And sometimes there are no symptoms at all.
Up to the majority of chlamydia cases can be asymptomatic. Gonorrhea can be silent, especially in women and people with cervixes. Early HIV can look like a mild viral illness and disappear before testing even crosses someone’s mind.
When doctors test broadly, they are responding to this uncertainty, not accusing you of anything.
Co-Infections Are More Common Than People Realize
Let’s strip away the fear and just talk biology.
Sexual contact exposes you to ecosystems, not single organisms. If a partner carries one infection, the behaviors and network that allowed that infection to spread can allow others to spread too. That’s not a moral statement. It’s epidemiology.
In clinical settings, co-infection between chlamydia and gonorrhea is common enough that many providers automatically test for both together. The tissues they infect overlap. The transmission routes are identical. And when one is present, the statistical probability of the other increases.
But it goes further than bacterial pairing.
Inflammation from one STD can increase vulnerability to another. For example, untreated syphilis or genital herpes can create microtears or sores that make HIV transmission biologically easier. That’s one reason why doctors think in panels instead of silos.
It’s not overtesting. It’s pattern recognition.
How Testing Narrowly Can Backfire
Imagine this scenario.
You test positive for gonorrhea. You take antibiotics. The burning improves. You assume it’s handled. But two weeks later, you still feel “off.” You retest and discover untreated chlamydia was there the entire time.
Now you’ve had extended inflammation, extended anxiety, and potentially extended transmission risk, all because the initial testing wasn’t broad enough.
Doctors have seen this play out repeatedly. That experience shapes how they order tests.
Here’s how comprehensive testing changes outcomes.
| Testing Approach | Detection Scope | Risk of Missed Co-Infection | Likelihood of Retesting Later | Peace of Mind |
|---|---|---|---|---|
| Single Infection Test | One pathogen only | Moderate to High | Higher | Conditional reassurance |
| Comprehensive STD Panel | Multiple common STDs | Significantly Lower | Lower | Broader clarity |
When people search “why did my doctor order more STD tests,” what they’re really asking is: do they think something worse is going on?
Usually, the answer is no. They’re preventing something worse from being missed.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
The Silent Factor: Asymptomatic STDs Change Everything
This is the part that surprises most people.
You can feel completely normal and still carry an infection. In fact, asymptomatic STD testing is standard practice precisely because so many infections do not cause early warning signs.
A person can have chlamydia with no discharge. Gonorrhea without burning. HIV without obvious symptoms after the initial flu-like phase. HPV without visible warts.
If doctors only tested based on symptoms, countless infections would go untreated.
That’s why comprehensive screening guidelines recommend panel testing for sexually active individuals with new or multiple partners, even if they “feel fine.” It’s preventative medicine, not suspicion.
STD Panel vs Single Test: What’s Actually Included?
Not all panels are identical, and that’s important to understand.
In clinical settings, a standard screening panel often includes testing for chlamydia, gonorrhea, syphilis, and HIV. Depending on symptoms and risk factors, providers may also include trichomoniasis, hepatitis B, or hepatitis C.
At home, comprehensive options exist as well. A discreet combo STD home test kit allows you to screen for multiple infections at once without stepping into a waiting room.
For many people, especially those in rural areas or those who simply want privacy, an at-home STD panel provides both control and clarity. And the logic is the same as in a clinic: test broadly so nothing slips through.
If you’re unsure where to start, you can explore options directly at STD Rapid Test Kits. Peace of mind doesn’t require a fluorescent exam room.
When One Positive Result Triggers More Testing
Another moment that feels scary is when you test positive for one STD and your doctor immediately orders additional tests.
It can feel like escalation. It’s actually protocol.
If someone tests positive for gonorrhea, additional screening for chlamydia is routine. If someone tests positive for syphilis, HIV testing is typically recommended. Not because disaster is assumed, but because co-infections are statistically linked.
This layered testing protects long-term health. Untreated infections can cause complications like infertility, chronic pelvic pain, neurological damage in advanced syphilis, or immune system compromise in untreated HIV.
Early detection interrupts that trajectory.
Why “Just Test Me for One Thing” Can Be Risky
Sometimes patients push back. “I only want to test for chlamydia.” Or, “I’m sure it’s just gonorrhea.”
Doctors hear that request a lot. But narrowing testing based on self-diagnosis can create blind spots.
Symptoms don’t reliably differentiate infections. Even clinicians can’t look at discharge color and definitively label a pathogen without testing. That’s why laboratory confirmation exists.
There’s also a timing issue. Different STDs have different window periods, the time between exposure and reliable detection. If someone tests too early for one infection but not another, they may get a false sense of security.
Broad testing helps reduce that risk.
The Emotional Side No One Talks About
Let’s pause the science for a second.
When your provider orders multiple STD tests, it can feel personal. It can feel like they’re assuming something about your sex life. People have said things like, “Do they think I’m reckless?” or “Why are they testing me for everything?”
That reaction makes sense. Sexual health still carries stigma. Even responsible, condom-using, communicative adults can feel a spike of shame when they hear the word “panel.”
But testing broadly isn’t a character judgment. It’s harm reduction.
A nurse once told a patient who was embarrassed about a full screen, “I test my own partner for everything every year. It’s standard care.” That quiet normalization matters. STD screening is maintenance, like checking cholesterol or blood pressure.
And in fact, most infections happen within ordinary, everyday sexual lives, not dramatic outlier situations. Long-term relationships, new partners after a breakup, oral sex that felt low-risk, a condom that slipped. Real life is messy. Medicine adapts to that mess.

People are also reading: TikTok STD Myths You Shouldn’t Trust With Your Body
The Public Health Angle: It’s Not Just About You
Here’s the bigger picture.
When doctors test for multiple STDs, they’re also thinking about transmission networks. Untreated infections don’t just stay contained to one person. They move quietly through communities.
Comprehensive testing shortens that chain.
For example, untreated chlamydia can lead to pelvic inflammatory disease, which increases the risk of infertility. Untreated syphilis can progress to neurological complications. Untreated HIV can weaken the immune system significantly. Early detection protects individual health, but it also reduces community spread.
That’s why screening guidelines emphasize regular panel testing for sexually active adults with new or multiple partners. It’s preventative medicine operating at scale.
What If Your Tests All Come Back Negative?
This is a question people don’t ask enough.
If you’re tested for multiple STDs and everything is negative, that doesn’t mean the testing was unnecessary. It means the system worked. It ruled out the most common infections and gave you clarity.
Clarity has value.
And if symptoms persist despite negative results, that information also guides next steps. It may point toward non-STD causes like urinary tract infections, bacterial vaginosis, yeast infections, or dermatologic conditions.
Testing broadly narrows the field. It doesn’t create problems, it eliminates them.
Choosing At-Home Panel Testing Without Guesswork
Some people avoid clinics entirely because of time, privacy, or anxiety. That’s real. Not everyone has easy access to care, and not everyone feels comfortable discussing sexual history face-to-face.
An at-home panel can offer the same comprehensive logic without the waiting room.
A multi-STD combo test kit allows you to screen for the most common infections in one step. Instead of guessing which single test to order, you reduce the margin for error.
Your results stay private. Your decisions stay yours. And you’re applying the same strategy doctors use, test broadly, treat accurately, move forward confidently.
So Why Doctors Test for Multiple STDs, Even If You Only Have One Symptom
Let’s bring this home.
Doctors test for multiple STDs because infections overlap. Because co-infections are common. Because symptoms don’t reliably point to a single diagnosis. And because many infections show no symptoms at all.
They do a lot of tests to make sure that diagnoses aren't missed, treatment isn't delayed, and complications don't last a long time. They test broadly because experience has taught them that single-test assumptions fail people.
It isn’t about assuming the worst. It’s about covering the full picture.
When you understand that, the panel stops feeling like suspicion and starts feeling like protection.
Check Your STD Status in Minutes
Test at Home with Remedium8-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $149.00 $392.00
For all 8 tests
What Doctors See That Patients Don’t
There’s something else happening in that exam room that most people never consider.
Doctors aren’t just reacting to your symptom. They’re reacting to patterns they’ve seen hundreds, sometimes thousands, of times before. They’ve seen the patient who tested for one infection and came back two weeks later still uncomfortable. They’ve seen the person who treated gonorrhea only to discover untreated chlamydia was still present. They’ve seen the quiet, asymptomatic infection uncovered only because someone agreed to a full panel instead of “just the one test.”
That experience changes how clinicians think.
When someone says, “Can’t we just test for one thing?” the provider isn’t dismissing them. They’re remembering every case where narrow testing delayed answers. Medicine is pattern recognition layered over probability. If infections commonly overlap, testing reflects that reality.
It’s not about assuming worst-case scenarios. It’s about reducing blind spots.
There’s also a practical layer most people don’t see: treatment decisions depend on complete information. If two infections are present and only one is treated, inflammation may persist. Symptoms may partially improve, then rebound. Anxiety lingers. Trust in the medical process erodes. Comprehensive testing up front prevents that cascade.
And here’s something deeply human: doctors would rather tell you everything is negative than call you back to say, “We missed something.”
Comprehensive testing protects both of you from that moment.
Broad Testing Is About Control, Not Catastrophe
When people hear “we’re going to run a full STD panel,” their brain sometimes jumps to worst-case thinking. Why so many tests? Is something really wrong?
But panel testing isn’t escalation. It’s strategy.
Think about it this way: if you’re checking smoke in a house, you don’t inspect one room and assume the rest are fine. You check the whole structure because problems spread quietly. Sexual health works the same way.
Testing broadly gives you control. It replaces speculation with data. It allows treatment to be targeted and complete. And if everything comes back negative, you walk away with something incredibly valuable, certainty.
Certainty reduces stress. Certainty improves communication with partners. Certainty lets you move forward without that low-level background hum of “what if?”
That’s why doctors test for multiple STDs at once. Not because your symptom is dramatic. Not because they suspect chaos. But because comprehensive answers are cleaner than partial ones.
And when it comes to your health, clean answers are worth it.
FAQs
1. Wait. You can actually have two STDs at the same time?
Yes. And I know that sounds dramatic, but it’s not rare. If two infections spread the same way and infect the same tissues, they can absolutely show up together. It’s not a “how did this happen?” moment. It’s biology doing what biology does.
2. If I only have one symptom, doesn’t that mean it’s just one infection?
Not necessarily. Burning urination doesn’t come with a name tag. Discharge doesn’t introduce itself. A sore doesn’t clarify whether it’s viral or bacterial. Symptoms overlap constantly, which is why doctors don’t rely on guesswork, they test broadly and let the lab do the sorting.
3. Why does it feel like my doctor is testing me for everything?
Because they are, and that’s a good thing. It’s not about assuming anything about your sex life. It’s about not missing something silent. Medicine is preventative by design. If there’s an opportunity to catch something early, providers take it.
4. Is it overkill to ask for a full STD panel?
No. If anything, it’s efficient. Testing for one infection today and another three weeks later because symptoms didn’t resolve? That’s the frustrating route. A comprehensive panel reduces second-guessing and second appointments.
5. What if I test positive for one STD, should I panic about the rest?
Take a breath. A positive result doesn’t automatically mean there are more. It simply means your provider may recommend additional screening to rule things out. Think of it as closing loops, not opening new disasters.
6. Can I just treat the one I tested positive for and ignore the rest?
Please don’t. If co-infections go untreated, symptoms can linger, and complications can develop quietly. Treatment works best when it’s complete. That’s why doctors connect the dots instead of treating infections in isolation.
7. If I feel completely fine, why would I need multiple STD tests?
Because many infections don’t announce themselves. Some people carry chlamydia or gonorrhea for months without obvious symptoms. Feeling fine isn’t proof of being infection-free. Testing is clarity, not confession.
8. Does having one STD make it easier to catch another?
Sometimes, yes. Infections that cause sores or inflammation can increase biological susceptibility to others. That’s one reason providers think in patterns instead of single events.
9. I’m embarrassed about asking for a full panel. Is that normal?
Completely normal. Sexual health still carries unnecessary stigma. But requesting comprehensive testing is responsible, not reckless. It says, “I care about myself and the people I’m intimate with.” That’s mature energy, not shameful energy.
10. What’s the safest move if I’m unsure?
When in doubt, test broadly. It removes the mental spiral. It replaces guessing with data. And it lets you move forward, whether that means treatment, reassurance, or simply peace of mind.
You Deserve Clarity, Not Guesswork
One symptom doesn’t always equal one infection. And one negative test doesn’t always tell the full story.
If you’re wondering whether you should test broadly, the safest answer is usually yes. Not because something terrible is assumed, but because certainty feels better than doubt.
You can explore comprehensive, discreet options directly at STD Rapid Test Kits. If you’d rather follow the same strategy doctors use in clinics, a combo STD home test kit allows you to screen for multiple common infections at once.
Your results are private. Your health decisions are yours. And testing broadly isn’t dramatic, it’s informed.
How We Sourced This Article: This article was informed by current screening recommendations from the Centers for Disease Control and Prevention, guidance from the World Health Organization, and clinical summaries from Mayo Clinic and NHS resources. We also looked at peer-reviewed studies on STD co-infection rates and how they spread to make sure that the explanations are based on current epidemiological evidence.
Sources
1. CDC – STD Screening Recommendations
2. World Health Organization – Sexually Transmitted Infections Fact Sheet
3. Mayo Clinic – Sexually Transmitted Diseases Overview
5. CDC – Chlamydial Infections Treatment Guidelines
6. CDC – Gonococcal Infections Treatment Guidelines
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a no-nonsense, sex-positive approach and is committed to expanding access to accurate sexual health information.
Reviewed by: Jordan M. Reyes, PA-C | Last medically reviewed: March 2026
This article is only meant to give you information and should not be used instead of medical advice.