Quick Answer: HPV symptoms often appear in women as visible genital warts or abnormal cervical cells, while men may carry the virus without any symptoms at all. Men can transmit HPV even without knowing they have it.
Why This Matters More Than Most People Think
If you’re in a relationship where one person has tested positive for HPV or noticed symptoms while the other hasn’t, you might feel confused, or betrayed. This article is for people caught in that moment. Maybe you're rethinking your last few hookups, or you're in a long-term relationship and wondering what this diagnosis means about fidelity. Maybe you're a guy who feels fine but just got told your partner has HPV, and you're wondering, “Do I need to worry too?”
HPV doesn’t play fair. It’s the most common sexually transmitted infection globally, and yet testing, detection, and symptoms show up differently depending on your anatomy, your immune system, and even the type of HPV. And that matters, because misunderstandings around symptoms and visibility can lead to false blame, missed testing, delayed treatment, or emotional distance between partners. This isn’t about who’s “clean” and who’s “not.” It’s about understanding how HPV operates, and how to protect each other, even when nothing looks wrong.
The Visibility Gap: Why Symptoms Appear in Women First
Let’s be blunt: HPV is often invisible in men. That doesn’t mean it’s harmless, but it does mean men are less likely to know they’re infected. For women, the virus tends to reveal itself through abnormal Pap smears or visible genital warts. Men may not show any symptoms, or they may show up in places that are harder to check, like inside the urethra, under the foreskin, or in the throat.
Consider this: in a 2022 CDC surveillance report, over 42% of women between 18 and 59 had evidence of genital HPV. But the percentage of men with visible symptoms? Far lower. Not because men don’t get HPV, but because the virus often flies under the radar in male bodies, making them silent carriers. Meanwhile, women are more likely to be routinely screened through Pap tests, which pick up on HPV’s cellular damage even when no external warts are present.
The imbalance here isn’t biological cruelty, it’s medical infrastructure. Women get screened early and often; men typically don’t. That’s changing slowly, especially as rates of HPV-related throat cancer in men rise, but we’re not there yet.
| Group | Common Detection Method | Visibility of Symptoms | Routine Screening Available? |
|---|---|---|---|
| Women | Pap smear, HPV DNA test, visual wart inspection | High – abnormal cells, visible warts | Yes – cervical screening is standard |
| Men | Visual inspection, biopsy (only if symptomatic) | Low – often asymptomatic or hidden | No – no standard screening for most men |
Table 1. Why women often get diagnosed before men. Symptom visibility and access to screening play a critical role.
People are also reading: The Syphilis Timeline How Long After Sex Can You Really Test?
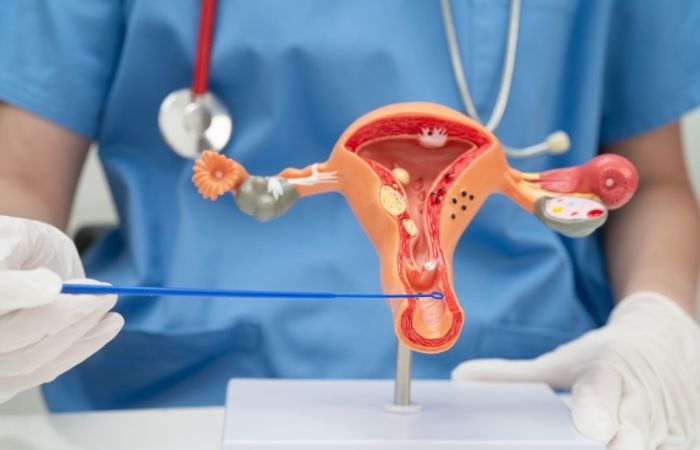
What HPV Looks Like in Women
HPV in women can take multiple forms, some obvious and others completely silent. The most visible sign is genital warts, which may appear as soft, flesh-colored bumps around the vulva, vagina, anus, or cervix. These may be raised or flat, and often show up in clusters. They don’t usually itch or hurt, which is why some women miss them until a gynecologist points them out.
But many high-risk HPV types don’t produce warts. Instead, they alter cervical cells in ways only detectable through a Pap smear or HPV DNA test. That means you could feel totally normal and still have a strain linked to cervical cancer. This disconnection between symptoms and severity is why routine screening is crucial, even if everything feels fine.
In some cases, women report subtle symptoms like post-sex bleeding, discharge changes, or pelvic discomfort. These signs aren't specific to HPV but may warrant testing, especially if combined with an abnormal Pap result or known exposure.
One woman we interviewed, Ana (28), said it like this:
“My doctor said I had high-risk HPV from a routine Pap. I didn’t even know I had it. I felt totally fine, no warts, no pain, nothing. And my boyfriend? He didn’t even get tested. He didn’t have to.”
This asymmetry leads many women to internalize the infection as their fault. It’s not. It’s biology, and lack of equal testing access.
Check Your STD Status in Minutes
Test at Home with RemediumPapillomavirus (HPV) Test
 For Women
For Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $33.99 $49.00
What HPV Looks Like in Men
In men, HPV often hides in plain sight, or deep inside. You can get genital warts on your penis, scrotum, anus, or thigh. They can be small or big, flat or raised, and most of the time people don't notice them unless they itch or grow. Warts can be hard to see because of things like circumcision status, skin folds, and even hair growth.
But most men with HPV never develop visible warts. Their immune systems clear the virus silently over 6 to 24 months. That doesn’t mean they’re not contagious. During this period, known as subclinical infection, they can pass HPV to partners through skin-to-skin contact, even without penetration. Condoms reduce but don’t eliminate this risk.
Oral HPV is another layer of complexity. Men are three times more likely than women to develop HPV-related oropharyngeal cancers, often years after initial infection. Symptoms here are subtle: sore throat, hoarseness, or a persistent lump in the neck. Most don’t connect these signs to a past sexual encounter, which delays diagnosis.
Josh (34) described his experience like this:
“I had a wart once in college, got it frozen off, and didn’t think about it again. Years later, my girlfriend tested positive for high-risk HPV. I felt like I had nothing to do with it. Now I’m wondering if I gave it to her without knowing.”
This is the cycle HPV creates: silent infection in men, visible consequence in women, and confusion in both.
| HPV Location in Men | Symptoms (if any) | Challenges in Detection |
|---|---|---|
| Genitals (penis, scrotum, perineum) | Visible or hidden warts, itching, irritation | May be under foreskin or too small to notice |
| Anal region | Warts, bleeding, discomfort (rare) | Often misattributed to hemorrhoids or ignored |
| Throat (oral HPV) | Sore throat, hoarseness, lump in neck | No routine screening; often diagnosed late |
Table 2. Where HPV hides in male bodies, and why it often goes unnoticed.
Why One Partner Shows Symptoms, and the Other Doesn’t
This is the part where relationships can get rocky. When one partner has visible symptoms, or a positive result, and the other insists they’re fine, it often leads to a quiet war of assumptions. Who brought it in? Who’s lying? But here’s the truth: HPV doesn’t follow fairness. It can live undetected for years, remain dormant, or disappear without treatment. This doesn't mean your partner is lying; they could just be asymptomatic and not know it.
Biologically, women are more likely to develop noticeable symptoms like genital warts or abnormal Pap results because the vaginal and cervical tissues are more susceptible to HPV-induced cellular changes. Men, with external skin and fewer moist mucosal surfaces, may carry the virus without those changes becoming visible. Hormonal changes and differences in the immune system also affect how the body reacts to HPV in men and women.
This asymmetry creates what researchers call “clinical mismatch.” One partner carries symptoms, sees a doctor, gets a name for it. The other partner never notices a thing. And yet both may have been infected for months, or years, without knowing.
In long-term relationships, this often sparks suspicion: “If I just got diagnosed, and you don’t have anything, you must have cheated.” In reality, the virus could’ve been dormant in either partner from a past encounter. There’s no easy way to trace who had it first. This uncertainty isn't just annoying; it's also upsetting. We need to be more understanding when we talk about HPV, especially when we talk to our partners.
HPV Can Be Dormant, For Months or Even Years
One of the most confusing facts about HPV is that it can lie dormant for a long time. You can have it, show no symptoms, and then suddenly develop warts or get a positive test result years after your last sexual partner. This latency is why HPV doesn’t always follow predictable timelines.
Studies have shown that most people clear the virus within 1–2 years, especially if they’re young and have healthy immune systems. But in some cases, the virus sticks around quietly, especially if it’s one of the high-risk strains. In women, that can mean no symptoms until a Pap smear flags an abnormality. In men, it might never show up unless a visible wart forms or throat cancer symptoms appear down the line.
Here’s how long HPV can behave in both men and women:
| HPV Status | Typical Duration in Women | Typical Duration in Men |
|---|---|---|
| Low-risk HPV (wart-causing) | 6 to 18 months (often clears) | 6 to 24 months (often asymptomatic) |
| High-risk HPV (cancer-linked) | Can persist for years undetected | Often unnoticed unless throat symptoms arise |
| Dormant infection (no symptoms) | Detected by Pap or HPV test | Rarely detected unless warts appear |
Table 3. HPV behavior over time: Even when it disappears, it can reemerge under the right conditions.
This dormancy explains why someone might test positive now even if their last sexual encounter was a year, or five, ago. The virus doesn’t always cause immediate symptoms, and it doesn’t need to in order to spread. That’s what makes it so hard to track, treat, and talk about.
Why There’s No Routine HPV Test for Men (Yet)
Here’s a medical injustice: there’s no approved HPV test for men unless symptoms appear. That’s right, unless you have warts, lesions, or signs of anal or oral complications, most healthcare providers won’t test you for HPV. This isn’t because men don’t get it. It’s because the tests we have aren’t FDA-approved for general screening in males.
For women, the story is different. Pap smears and HPV DNA tests are a normal part of sexual health care that starts in your 20s. These tests look for changes in cervical cells that are caused by high-risk HPV. Men, on the other hand, are usually left out unless they request testing through a specialist or are part of high-risk populations (e.g., men who have sex with men, or those with HIV).
This testing gap makes it easy for male partners to say, “I’m negative,” even if they’ve never been tested. It’s not necessarily deception, it’s a blind spot in the system. Without visible symptoms or proactive healthcare, many men simply never know they’re carriers. That’s why so many women feel blindsided after a diagnosis.
Instead of blame, we need better access, equal screening protocols that don’t wait for visible symptoms or life-threatening complications.
What It Feels Like: HPV Beyond the Body
HPV isn’t just a physical diagnosis, it’s emotional. When symptoms appear in one partner, and not the other, the psychological fallout can be just as intense as the infection itself. Women, in particular, often report feelings of shame, confusion, or betrayal. Men may feel helpless, or dismissive, especially if they’ve never had symptoms and think it “isn’t a big deal.”
Olivia (32) described her reaction after being told she had high-risk HPV:
“I felt dirty. I’d been with my boyfriend for almost two years. He told me he was tested before we got serious. But now I’m the one with abnormal cells. It felt like a betrayal, even though I know that’s not fair.”
Ryan (29) shared the opposite experience:
“When my partner showed me the warts, I felt panic. Not because of the warts, but because I realized I could’ve given it to her without knowing. I felt responsible but totally out of control.”
These reactions aren’t overreactions. They’re real consequences of how we teach people about STDs, through fear, judgment, and silence. HPV is common, manageable, and often temporary. But without good communication and accurate education, it becomes a wedge between people who otherwise care about each other.
How HPV Spreads, Even Without Symptoms or Sex
Most people assume HPV spreads only through penetrative sex. That’s a myth. HPV spreads through skin-to-skin contact, including genital contact without penetration, oral sex, and even mutual masturbation if the virus is on the skin. This means a condom doesn’t fully protect you, though it does lower the risk.
In heterosexual couples, one partner may contract it from oral sex, or from a previous relationship. In same-sex couples, shared toys or skin-to-skin friction can also transmit the virus. It’s not about recklessness, it’s about how the virus works. That’s why so many people who’ve had just one or two partners still end up with HPV.
What makes this even more complex is that people often stop using protection in long-term relationships. If one partner has dormant HPV and the other doesn’t, the transmission may not happen until immunity shifts or a flare-up occurs, months or even years into monogamy. It’s not infidelity. It’s biology.
This is why couples need tools, not blame. Testing, communication, vaccines, and shared responsibility go a lot farther than guilt trips ever could.
So You Have Symptoms, What Should You Do?
If you’re the partner with visible signs of HPV, genital warts, abnormal bleeding, or an unusual Pap result, it can feel like you’re holding the evidence while the other person walks away symptom-free. The first step? Take a breath. Most cases of HPV are treatable, and many clear on their own with no long-term impact. But if symptoms are showing up, it’s time to act, not panic.
If you have warts, a healthcare provider can confirm whether they’re caused by HPV (most often, they are). Treatments include topical solutions, freezing (cryotherapy), or minor surgical removal. These are outpatient, quick, and usually covered by insurance. Warts can come back, but managing them early reduces discomfort and helps prevent transmission.
Your doctor may recommend additional testing, such as a biopsy or colposcopy, if the results of your Pap test were abnormal. But this doesn't mean you have cancer. Most of the changes HPV makes to the cervix go away on their own, but you should still keep an eye on them. The earlier you catch abnormal cells, the easier they are to manage.
If you’re a man with visible symptoms, warts, throat discomfort, or anal pain, don’t wait. Ask for a physical exam, even if your provider doesn’t immediately suggest HPV testing. Early intervention makes a huge difference in both comfort and outcomes.
This is also the moment to loop your partner in, calmly, without blame. It’s not about accusations. Moving forward, it's all about being aware, safe, and sharing responsibility.
What If You Have No Symptoms, but You're Still Worried?
This is where a lot of people get stuck. You feel fine. You’ve had no warts, no abnormal tests. But your partner just got diagnosed with HPV, and now you’re not sure what to do. Should you test? Should you assume you have it? Should you stop having sex?
Here’s the deal: if you’re a man without symptoms, you likely won’t be tested unless you specifically ask, and even then, options are limited. That’s because there’s still no universal screening test for HPV in males. But you can still take action.
Talk to your healthcare provider about your partner’s diagnosis. Share any possible symptoms, even if they seem minor (like throat irritation or a single bump). If your partner’s diagnosis involves a high-risk strain, you may want to monitor your own health more closely and consider discussing anal or oral screening with a specialist.
If you’re a woman whose partner was diagnosed, and you’ve never been tested for HPV, it’s time to schedule a Pap and HPV co-test. This will give you a baseline. If you’ve had normal results in the past, you’re still not immune, but you’re informed.
And if you’ve been vaccinated? Great. But remember, vaccines prevent certain strains, not all. That’s why monitoring and honesty still matter after vaccination.
Vaccination: It's Not Just for Teens
Most people think the HPV vaccine is for kids. It’s true, it’s most effective before sexual debut, which is why it’s offered to preteens. But what many don’t know is that you can still get vaccinated as an adult, up to age 45 in some countries.
The HPV vaccine (Gardasil 9) protects against the strains most likely to cause genital warts and cancers, including cervical, throat, and anal cancers. Even if you’ve already been exposed to one strain, the vaccine may protect you from others. It doesn’t cure existing infections, but it strengthens your defense moving forward.
We’ve spoken with people in their 30s and 40s who said getting vaccinated post-exposure helped them feel proactive, and gave their partners peace of mind.
Maria (38) shared:
“I already had HPV when I got vaccinated. But my doctor said it could still help. It made me feel like I had some control again.”
If your partner has HPV, getting vaccinated together can be an act of care, not just prevention. It shows you're protecting each other, not blaming each other.
Talking to Your Partner (Without Blame)
HPV often enters a relationship quietly, but it doesn’t have to explode it. The hardest part is usually not the diagnosis, it’s the conversation. Telling a partner that you tested positive, or that you noticed a wart, can feel vulnerable. It's real to be afraid of being judged, blamed, or left behind. But here's the truth: being honest usually makes people trust you more than not saying anything at all.
Start by separating the diagnosis from morality. HPV is a virus, not a verdict. Over 80% of sexually active people will contract it at some point. Framing it this way can defuse tension and make space for empathy instead of panic.
Share the facts: what type you were diagnosed with (if known), what your doctor said, what the plan is. Invite your partner into the process. This isn’t “your problem.” It’s shared. Even if only one of you has symptoms, both of you deserve support and information.
One couple we interviewed decided to get tested together, even though only one partner had symptoms. The experience strengthened their relationship, not because of the results, but because of the transparency.
If you’re on the receiving end of that disclosure, breathe before reacting. Your partner isn’t accusing you. They’re including you. That’s what real intimacy looks like.

People are also reading: Can You Catch an STD from a Hotel Towel?
You Can Still Have Sex (Here’s How to Do It Safely)
Contrary to fear-based myths, an HPV diagnosis doesn’t mean you have to stop having sex. But it does mean rethinking how you approach it. The virus is most contagious when symptoms are present, but can still be transmitted even when invisible. Condoms reduce risk, but they don’t eliminate it. Skin-to-skin contact outside the barrier is still enough for transmission.
If warts are visible, it’s generally advised to hold off on sex until they’re treated and healed. That lowers the risk of spreading the virus or causing discomfort. If you and your partner both already have HPV, you may not be protecting each other from reinfection, but using protection is still wise, especially if you’re not sure which strain each of you has.
Here’s what matters most: informed consent. Talk about it. Make rules. Decide together what feels safe. HPV is manageable, but only when both people are part of the plan.
Check Your STD Status in Minutes
Test at Home with Remedium10-in-1 STD Test Kit

 For Women
For Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $189.00 $490.00
For all 10 tests
Protecting Each Other Without Panic
HPV isn’t about who’s clean and who’s not. It’s about bodies doing their thing, sometimes quietly, sometimes visibly. If you’re the one with symptoms, you’re not dirty. If your partner doesn’t have symptoms, they’re not innocent or guilty. You're both just navigating a virus that more than 80% of adults encounter at some point.
Protecting each other means getting tested, talking openly, and making proactive decisions, like vaccination or choosing a combo STD home test if you're worried about more than just HPV. It means remembering that a virus doesn’t define your value, your loyalty, or your future.
You’re not alone. And you’re not doomed. You’re just informed now, which makes you powerful.
FAQs
1. Can guys really have HPV and not even know it?
Yep, happens all the time. Most men with HPV don’t have symptoms, don’t get tested, and may never realize they were even exposed. No pain, no bumps, no clue. That doesn’t mean they’re not contagious, it just means the virus can live quietly in their system, especially in areas like the scrotum, penis shaft, or anus. That’s one reason so many women find out first.
2. What does HPV actually look like “down there”?
It depends. If you’ve got low-risk HPV, you might notice fleshy, cauliflower-like bumps (genital warts). They can be tiny or clustered, flat or raised. But here’s the twist: some strains don’t cause any visible signs at all. That’s why so many people walk around thinking they’re in the clear, until a Pap smear or a surprise diagnosis changes the story.
3. If I just tested positive, does that mean my partner cheated?
Not necessarily. HPV can hide out for months, even years, before making a scene. So it could be from a past relationship, a dormant infection, or yes, recent exposure. The problem is, you can’t carbon-date HPV. There’s no way to know exactly when it entered your body. That’s frustrating, but it’s also a reason to approach this with curiosity, not accusations.
4. Can you really get HPV from going down on someone?
For sure. HPV spreads easily through skin-to-skin contact, even mouth-to-genital contact. And while oral HPV is often symptomless, in some cases it can lead to throat cancer down the line, especially in men. No, that doesn’t mean you should stop having oral sex. But it does mean you should be aware, get vaccinated if you can, and talk to partners about risk.
5. Why do doctors test women for HPV but not men?
It's less about fairness and more about infrastructure. There’s no FDA-approved HPV test for general use in men right now. Women, on the other hand, get Pap smears and HPV DNA testing as part of regular reproductive care. So yes, that makes it look like women get “caught” with HPV more often, but that’s only because someone’s actually looking.
6. I’ve already had sex, does the HPV vaccine still do anything for me?
Absolutely. It works best before you get HPV, but it can still protect you from strains you haven't had sex with yet. Gardasil 9 covers nine types, including the ones most likely to cause cancer and warts. So even if you’ve had one strain, the vaccine still helps shield you from others. It’s a “better late than never” situation.
7. Can we still have sex if one of us has HPV?
You can, but talk about it first. If warts are present, it’s a good idea to hold off until treatment is complete to reduce transmission risk. If neither of you have symptoms, using condoms or dental dams can help, but they’re not foolproof. HPV can live on skin outside the areas they cover. The real MVP here? Communication and informed consent.
8. So… does this mean I have HPV forever?
Probably not. In most people, the immune system clears HPV naturally within 6 to 24 months. But it can also go dormant and reappear under stress or immune changes. That’s why regular screening (like Pap smears or follow-ups after wart treatment) matters. You might not “see” it anymore, but your body remembers.
9. I don’t want to pass this to my partner, what can I actually do?
Start with honesty. Tell them what you’ve been diagnosed with and what your doctor said. Use protection, even if you’re both infected, it can still reduce the chance of spreading or reactivating a different strain. And consider getting vaccinated together. Turning treatment into teamwork can actually bring couples closer, not tear them apart.
10. Do I need to tell every past partner?
That’s up to you, and depends on timing and type. If it’s a recent diagnosis and you’ve had unprotected sex with someone, a heads-up is fair. If it’s been years, and you’re not in contact, the public health risk is probably low. Remember, most people will get HPV at some point, and we don’t report every cold we get. Still, if you're in doubt or want help crafting the conversation, your doctor or a telehealth provider can guide you through it.
You Deserve Answers, Not Assumptions
Getting an HPV diagnosis, especially when your partner shows no signs, can be isolating. But remember: symptoms don’t tell the full story. The virus behaves differently in every body. One partner’s silence doesn’t mean immunity, and one person’s diagnosis doesn’t mean blame. HPV is common, confusing, and often misunderstood, but it’s also manageable.
Whether you're the one with visible symptoms or just grappling with the emotional fog of an unexpected diagnosis, you have options. You can ask questions. You can get tested. You can talk to your partner. You can take control.
Don’t wait and wonder, get clarity. This discreet at-home combo test kit checks for the most common STDs, including those that often hide like HPV.
How We Sourced This Article: We combined current guidance from leading medical organizations with peer-reviewed research and lived-experience reporting to make this guide practical, compassionate, and accurate.
Sources
1. CDC – Genital HPV Infection Fact Sheet
3. World Health Organization – HPV and Cervical Cancer
4. Planned Parenthood – What Is HPV?
5. HPV infection - Symptoms & causes (Mayo Clinic)
6. Human Papillomavirus Epidemiology and Prevention (NCBI)
7. How to Protect Against HPV (American Cancer Society)
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a no-nonsense, sex-positive approach and is committed to expanding access for readers in both urban and off-grid settings.
Reviewed by: L. Sharma, MPH | Last medically reviewed: December 2025
This article is only for informational purposes and should not be taken as medical advice.










