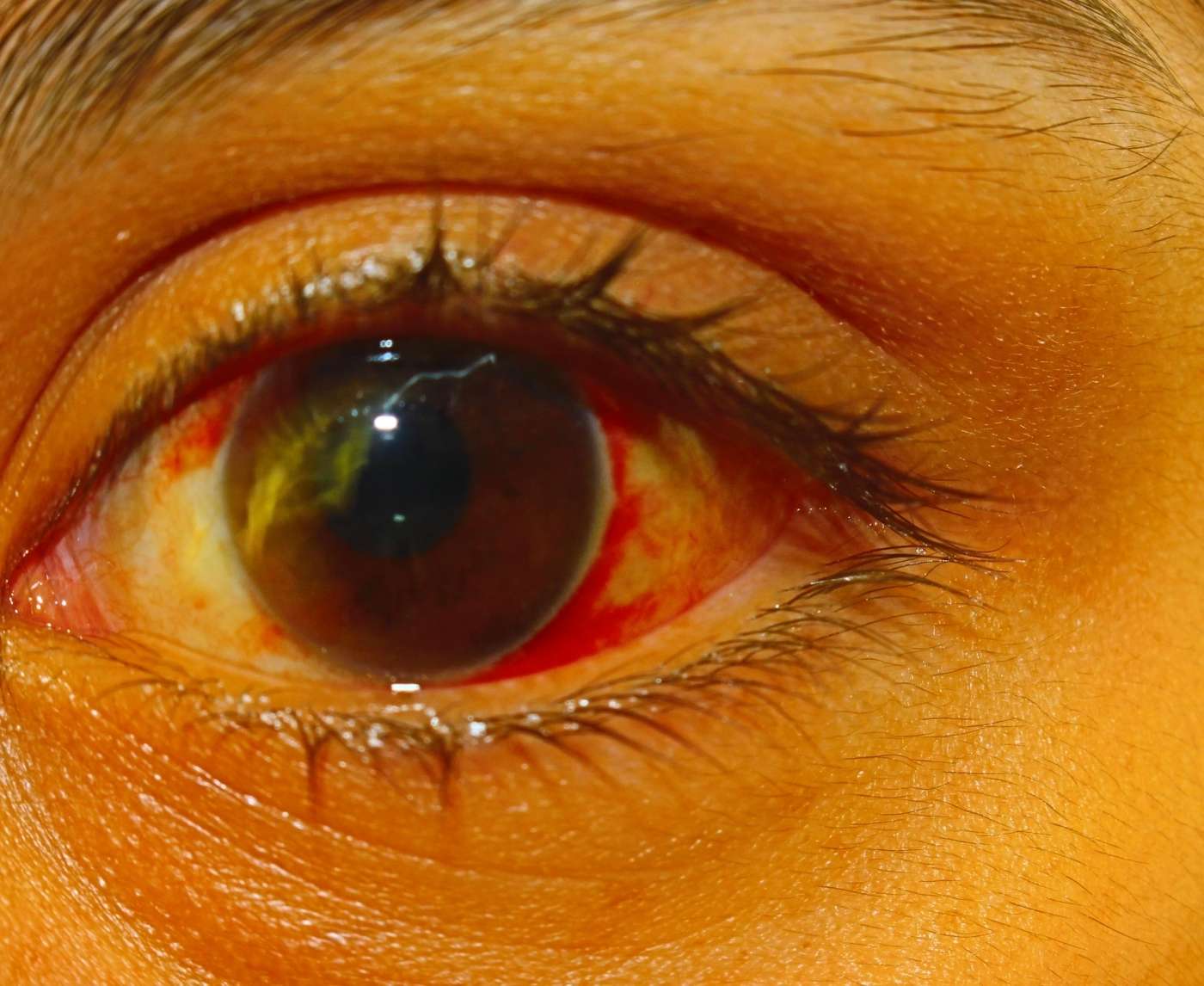
Quick Answer: Pink eye and STDs can both cause red, burning, watery eyes after oral sex. If symptoms include thick discharge, severe swelling, or worsen within 1–3 days after fluid exposure, testing for gonorrhea or chlamydia is recommended around 7–14 days after exposure for accurate results.
First, Let’s Separate Panic From Possibility
Not every red eye after sex is an STD. In fact, most aren’t. Eyes are sensitive. Semen can irritate the surface of the eye even without infection. So can friction from rubbing, leftover makeup, or simply sleeping in contact lenses after a long night. Your body doesn’t need an infection to react.
But here’s where the investigator voice kicks in: if infectious fluid containing bacteria makes direct contact with the eye, transmission is biologically possible. Gonorrhea is particularly aggressive in mucous membranes. The same bacteria that infects the throat or genitals can infect conjunctival tissue. Chlamydia can as well, though it often presents more gradually.
So the question isn’t “Can this happen?” It can. The real question is: “Does what I’m feeling match what that looks like?”
What STD Eye Infections Actually Feel Like
Ava noticed her eye was gritty the morning after oral sex with a new partner. She assumed it was allergies. By that evening, it was red and producing thick yellow discharge that glued her lashes together. She woke up the next day and couldn’t fully open it without wiping it first. That detail matters.
Classic viral pink eye tends to produce watery discharge and mild irritation. STD-related eye infections, especially from gonorrhea, often escalate fast. Swelling can become pronounced. Discharge may turn thick, yellow, or green. Pain can intensify rather than stabilize.
With chlamydia, symptoms may be more subtle at first. Persistent redness. Mucus strands. A feeling like something is stuck in the eye that won’t rinse out. It doesn’t always explode overnight, which is why people sometimes miss it.
| Feature | Viral/Bacterial Pink Eye | Gonorrhea Eye Infection | Chlamydia Eye Infection |
|---|---|---|---|
| Onset Speed | Gradual (1–2 days) | Rapid (12–48 hours possible) | Gradual to moderate |
| Discharge | Watery or mild mucus | Thick, yellow/green, heavy | Mucus-like, persistent |
| Swelling | Mild | Often significant | Mild to moderate |
| Pain Level | Irritating but tolerable | Can be painful or intense | Often mild discomfort |
| Exposure History | Cold, contact spread | Direct sexual fluid contact | Direct sexual fluid contact |
None of these signs alone confirm an STD. But when severe discharge pairs with recent oral exposure, testing stops being overreacting and starts being smart.

People are also reading: Testicle Pain and Swelling? Don’t Ignore Signs of Orchitis
How STDs Reach the Eye in the First Place
The eye is a mucous membrane. So are the genitals, throat, and rectum. Bacteria that thrive in warm, moist tissue don’t care whether they’re in the urethra or the conjunctiva. If infected fluid touches your eye and isn’t rinsed quickly, transmission becomes possible.
This can happen during oral sex if semen or vaginal fluid splashes or is transferred by fingers. It can happen if someone touches their genitals and then rubs your eye. It can even happen accidentally during cleanup.
It doesn’t require ejaculation directly into the eye. It requires exposure to infected fluid. That nuance matters, because many people panic even when there was minimal contact. Risk depends on whether the partner actually had an untreated infection.
Most people who Google “semen in eye STD risk” don’t know their partner’s status. That uncertainty is what fuels the anxiety spiral. Testing answers that question more reliably than guessing symptoms.
Timing: When Testing Actually Makes Sense
Here’s where we slow the panic down and bring in timing science. Testing too early can produce false reassurance. Testing too late just prolongs stress. The sweet spot matters.
Most nucleic acid amplification tests (NAATs) for gonorrhea and chlamydia become reliable about 7 days after exposure, with the best accuracy coming closer to 14 days. Symptoms may appear earlier, but detectable bacterial levels take time to build.
If your eye started burning 24 hours after exposure, that doesn’t mean testing on day two will be accurate. It means symptoms can appear before test sensitivity peaks.
| Days Since Exposure | What’s Happening Biologically | Testing Guidance |
|---|---|---|
| 1–3 Days | Possible early irritation or symptom onset | Too early for reliable testing unless severe symptoms require medical care |
| 4–7 Days | Bacterial levels rising | Testing may detect infection but retest at 14 days increases confidence |
| 7–14 Days | Window period closing | Ideal time for accurate testing |
| 14+ Days | Peak detection accuracy | Test now if not already done |
If discharge is heavy, pain is worsening, or vision is affected, don’t wait for the perfect window. Seek urgent care. Gonococcal eye infections can escalate quickly and require prescription antibiotics.
If symptoms are mild and stable, testing at home around day 7–14 gives you clarity without sitting in a clinic lobby replaying your weekend decisions.
Peace of mind matters. If your brain keeps replaying the moment, you can order a discreet test directly from STD Rapid Test Kits and handle it privately. Results are yours. No awkward explanations.
What If It’s Not Just the Eye? The Clues People Miss
Marcus thought he had seasonal allergies. His right eye was red and watery two days after oral sex. He figured maybe it was pollen, or maybe he slept funny. What he didn’t think about was the sore throat that followed three days later. Or the mild burning when he peed that he brushed off as dehydration.
This is where context matters. Eye symptoms after oral sex sometimes travel with other subtle signs. Gonorrhea and chlamydia can infect the throat without obvious pain. They can infect the genitals without dramatic discharge. So when someone searches “STD without genital symptoms,” they’re often surprised to learn that yes, you can have an infection localized in one area while barely noticing another.
If you’re experiencing red eyes after oral sex and also noticing unusual discharge, throat irritation, pelvic discomfort, or urinary burning, that cluster strengthens the case for testing. It doesn’t confirm anything. But it shifts the situation from “probably allergies” to “worth checking.”
On the other hand, if your only symptom is mild watery irritation that improved within 48 hours and there was no known exposure to an infected partner, the probability leans toward simple conjunctivitis or irritation. Your body can react strongly to friction and still not be infected.
Why Gonorrhea in the Eye Gets So Much Attention
There’s a reason “gonorrhea in eye” trends higher than “chlamydia eye infection.” Gonorrhea can be aggressive. In rare cases, untreated gonococcal conjunctivitis can threaten vision. That sounds terrifying, and it should be taken seriously. But it is also treatable when caught early.
The bacteria responsible for gonorrhea, Neisseria gonorrhoeae, adheres efficiently to mucosal tissue. When it infects the eye, symptoms often escalate fast. Swelling can become dramatic. Discharge can be profuse. Pain may intensify rather than stabilize. If you’re asking yourself whether your eye burning after semen exposure is “normal irritation,” pay attention to speed and severity.
Contrast that with viral pink eye. Viral conjunctivitis often spreads from one eye to the other. It may accompany cold symptoms. It produces tearing more than thick pus. It feels uncomfortable but rarely alarming.
Speed is the tell. Severe swelling within 24–48 hours after direct fluid exposure should not be ignored.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
The Emotional Spiral: Why This Feels Bigger Than It Is
Here’s the part nobody talks about enough. When symptoms follow a sexual encounter, they carry moral weight. Even if you logically support casual sex. Even if you use protection. Even if you are sex-positive and informed. The body reaction becomes a narrative.
“I shouldn’t have done that.” “I knew better.” “Now I’m paying for it.”
This inner dialogue amplifies fear. A red eye becomes a symbol. But infections are biological events, not character judgments. If you were exposed, you were exposed. Shame doesn’t change incubation timelines.
Testing reframes the story. Instead of guessing, you gather data. Instead of spiraling, you act. That shift from speculation to clarity reduces anxiety more than symptom Googling ever will.
When to Seek Immediate Care Instead of Waiting to Test
Most eye irritation can wait a few days for clarity. Some cannot. If you experience intense pain, sensitivity to light, vision changes, or copious thick discharge that worsens rapidly, urgent medical evaluation matters more than perfect test timing.
Gonococcal eye infections can require prescription antibiotic drops or systemic antibiotics. They are not situations for watchful waiting. This is not about panic. It’s about respecting severity.
Ella described it as “waking up with my eye sealed shut and throbbing.” That is not subtle irritation. That’s escalation. In cases like that, emergency care or urgent care is appropriate regardless of exposure timeline.
Home Testing vs Clinic Testing: What Makes Sense Here?
If symptoms are moderate and stable, many people prefer discreet at-home testing. It avoids the uncomfortable conversation at urgent care where you explain, “Well, it was oral sex and maybe fluid got in my eye.” Privacy can be a powerful reason to test from home.
Modern NAAT-based tests are highly accurate within the proper window period. A properly collected sample after day seven gives strong detection reliability. By day fourteen, sensitivity is typically at peak for gonorrhea and chlamydia.
If you need eye-specific swabs or your symptoms are very bad, you may need to go to the clinic for testing. But for a lot of people who may have been exposed, using a discreet kit to screen them gives them quick and private answers.
| Scenario | Best Option | Why |
|---|---|---|
| Mild symptoms, stable, day 7–14 after exposure | At-home NAAT test | High accuracy, maximum privacy |
| Severe swelling, pain, or vision changes | Urgent clinic care | Immediate evaluation and prescription treatment |
| Uncertain exposure but high anxiety | At-home screening | Quick reassurance reduces stress |
| Symptoms spreading to other areas | Clinic or comprehensive test panel | May require multi-site evaluation |
If you want a discreet option that screens for common bacterial STDs, you can explore available kits directly at STD Rapid Test Kits. Testing is not an admission of guilt. It’s an act of clarity.
What Happens If You Test Positive?
You breathe out first. Because both gonorrhea and chlamydia can be treated. When you take antibiotics as directed, they work well to get rid of bacterial infections. Early treatment stops problems from happening and lowers the risk of spreading.
You contact a healthcare provider for confirmation and treatment guidance if needed. You notify recent partners so they can test and treat as well. That conversation feels uncomfortable, but it’s an act of care.
And then you move forward. Most people who test positive once never experience long-term consequences because they handled it promptly. The story ends with antibiotics and a follow-up test, not permanent damage.
Ignoring symptoms prolongs anxiety. Addressing them shortens it.
People are also reading: Red Bumps, Burning, or Just Shaving? What Vaginal Spots Really Mean
Incubation, Window Periods, and Why Your Brain Wants Instant Answers
Here’s the frustrating part. Your eye can start burning within a day of exposure, but reliable testing may require waiting a full week. That gap between symptom and certainty is where anxiety grows teeth.
Incubation refers to the time between exposure and symptom onset. Window period refers to the time between exposure and when a test can reliably detect infection. They are not the same thing. You can feel something before a test turns positive. You can also have zero symptoms and still test positive later.
With gonorrhea, symptoms in the eye can appear quickly, sometimes within 2–5 days. With chlamydia, it may take a week or longer. Testing accuracy, however, improves significantly after day seven and peaks closer to day fourteen for most nucleic acid tests.
Jordan tested on day three because he couldn’t stand the uncertainty. It came back negative. He felt relief for about twelve hours. Then he started wondering if it was too early. He retested at day twelve and felt calmer not because the result changed, but because the timing made sense.
Sometimes the emotional relief doesn’t come from the result alone. It comes from knowing the science supports it.
If It’s Just Pink Eye, What Should Happen?
Most viral or non-STD bacterial conjunctivitis improves within several days to a week. Discharge decreases. Swelling softens. The eye feels irritated but not aggressively painful. Vision remains stable. Symptoms may spread to the other eye in viral cases.
Warm compresses help. Avoiding contact lenses helps. Not rubbing the eye helps. Improvement is gradual but noticeable.
If symptoms are steadily improving by day three or four and there are no other signs of systemic infection, the likelihood of an STD-related cause drops. That doesn’t mean testing is forbidden. It means the probability curve shifts.
The key question becomes: Is this stabilizing or escalating?
If It’s an STD, What Happens Without Treatment?
Untreated gonorrhea in the eye can worsen. Severe inflammation can damage the cornea if not treated promptly. That’s why severe cases require urgent antibiotics. This is not meant to scare you. It’s meant to reinforce that bacterial infections are treatable when addressed early.
Chlamydia in the eye can become chronic if untreated. It may cause persistent redness and irritation. Again, treatable. The issue is delay, not inevitability.
What makes people delay? Embarrassment. Minimization. Hoping it will resolve. Telling yourself it’s probably nothing. But if your body keeps signaling, listen.
Testing is faster than weeks of wondering.
Check Your STD Status in Minutes
Test at Home with Remedium6-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $119.00 $294.00
For all 6 tests
The Scenario Most People Don’t Consider
Sometimes the eye symptoms aren’t from the partner you’re worried about. Sometimes they’re from you. If you had an untreated throat or genital infection and touched your own eye after contact, self-transfer can occur. That possibility often surprises people.
Testing isn’t about accusing someone else. It’s about understanding your own status. If you haven’t screened in a while and had new partners, this moment might simply be the reminder your body needed.
Many people who search “eye infection after oral sex” discover they were asymptomatic carriers in another site. That realization isn’t shameful. It’s informative.
Retesting and Follow-Up: When Is It Necessary?
If you test negative at day seven but symptoms persist or worsen, retesting at day fourteen increases confidence. If you test positive and complete antibiotic treatment, follow your provider’s recommendation regarding retesting. Some guidelines suggest retesting for reinfection several weeks to months later, especially if new exposure occurs.
If symptoms resolve quickly and testing is negative within the appropriate window, no additional testing may be required. Context matters. Risk level matters. Your comfort level matters.
Sexual health isn’t a single event. It’s ongoing maintenance.
Let’s Address the Question You’re Really Asking
“Did I mess up?”
No. You engaged in consensual sex. Exposure can happen even when you’re careful. Even when you trust someone. Even when protection is used in other ways. Eyes are simply less talked about in risk discussions.
You’re not reckless for being here. You’re responsible for wanting clarity.
If you’re within the 7–14 day window after exposure and your eye symptoms are lingering or intense, consider ordering a discreet screening kit from STD Rapid Test Kits. Private shipping. Clear instructions. Direct answers.
Peace of mind is not dramatic. It’s practical.
FAQs
1. Be honest, can you actually get gonorrhea in your eye from oral sex?
Yes. It’s not common, but it’s real. If infected fluids make direct contact with your eye, gonorrhea bacteria can attach to that tissue the same way they attach to the throat or genitals. Most exposures don’t lead to infection, but if symptoms escalate quickly after contact, that’s when testing stops being dramatic and starts being responsible.
2. How fast would I know if something’s wrong?
Sometimes faster than you’d like. With gonorrhea, symptoms can show up within a couple of days, redness, swelling, thick discharge that feels different from typical pink eye. Chlamydia tends to move slower. But remember: symptom timing isn’t the same as testing timing. Even if your eye burns on day two, reliable testing usually makes more sense closer to day seven or later.
3. What if it’s just watery and annoying, no thick discharge?
That leans more toward irritation or viral pink eye. STD-related eye infections often look more intense. Think heavier discharge, more swelling, sometimes more pain. If it’s mild, improving, and not escalating, the probability drops. If it’s getting worse instead of better, that’s your cue.
4. Okay but… semen got in my eye. Am I automatically infected?
No. Exposure is not the same thing as infection. The other person would need to have an active untreated infection for transmission to occur. Semen can absolutely irritate your eye without transmitting anything. Burning alone doesn’t equal bacteria.
5. If my partner says they tested negative recently, can I relax?
Maybe, but timing matters. If they tested very soon after their own exposure, their result might have been inside a window period. That’s not about mistrust. It’s about biology. If you’re feeling symptoms, testing yourself removes the guesswork.
6. What would make this an emergency?
Severe swelling. Intense pain. Light sensitivity. Vision changes. Discharge that’s heavy and worsening quickly. Those aren’t “wait and see” symptoms. Those are “get seen today” symptoms. Especially if exposure was recent.
7. If I test negative at day five, am I good?
Probably not definitively. Day five is often early for peak accuracy. A negative that early may need confirmation closer to day fourteen. The goal isn’t just a result, it’s a result you can trust.
8. Can herpes infect the eye too?
It can. Herpes in the eye usually presents differently, more pain, light sensitivity, sometimes a feeling like something sharp is stuck there. It’s less commonly linked to fluid splash exposure, but if symptoms are unusual or vision changes, a clinician should evaluate it.
9. If symptoms disappear, can I skip testing?
If they resolve quickly and you have low-risk exposure, you may not need further testing. But if your anxiety is lingering or you’re unsure about your partner’s status, screening can give you closure. Peace of mind counts.
10. Am I overreacting?
No. You noticed something. You’re asking questions. That’s what adults do when their body signals uncertainty. Overreacting would be spiraling without information. Getting tested, or deciding not to based on timing and symptoms, is informed action.
You Deserve Clarity, Not Catastrophizing
A red, burning eye after oral sex can feel like a flashing warning sign. Sometimes it’s simple irritation. Sometimes it’s viral pink eye. Occasionally, it’s an STD that needs antibiotics. The difference isn’t something you determine by fear alone. It’s determined by symptoms, exposure context, and timing.
If you’re in the 7–14 day window after possible exposure and symptoms haven’t clearly improved, testing gives you control back. You can order discreet screening directly from STD Rapid Test Kits and get answers privately. No waiting room. No explanations. Just data.
Sex happens. Exposure happens. Responsible follow-up is what protects you and your partners. That’s not shameful. That’s adult.
How We Sourced This Article: This guide was informed by current clinical guidance from leading public health authorities, peer-reviewed infectious disease research, and patient-centered reporting on ocular sexually transmitted infections. We looked at medical research on gonococcal and chlamydial conjunctivitis, how long it takes for symptoms to show up, and how accurate tests should be.
Sources
1. Centers for Disease Control and Prevention – Gonorrhea Fact Sheet
2. Centers for Disease Control and Prevention – Chlamydia Fact Sheet
3. American Academy of Ophthalmology – Conjunctivitis Overview
4. Mayo Clinic – Pink Eye (Conjunctivitis)
5. World Health Organization – Sexually Transmitted Infections Overview
6. CDC – 2021 STI Treatment Guidelines: Gonococcal Infections
7. American Academy of Family Physicians – Diagnosis and Management of Red Eye
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a direct, sex-positive approach to help readers make informed decisions without shame.
Reviewed by: L. Ramirez, PA-C | Last medically reviewed: February 2026
This article is only meant to give you information and should not be used instead of medical advice.