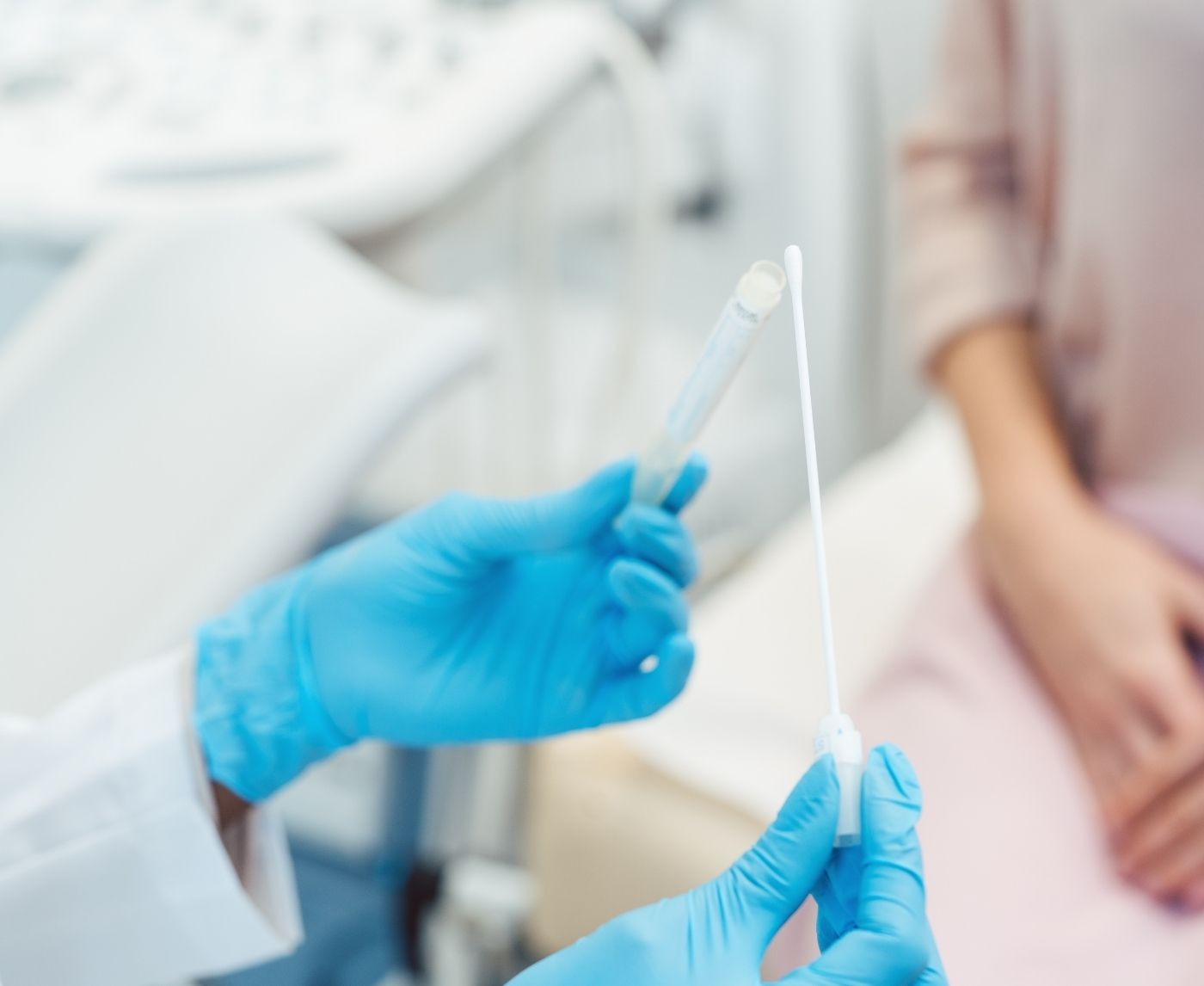
Quick Answer: A “full STD panel” often misses infections like Herpes, Trichomoniasis, or Mycoplasma genitalium, unless you specifically ask for them. Even with testing, timing, window periods, and test types can impact results.
How a “Negative” Test Isn’t Always the End of the Story
Let’s be honest, getting an STD test feels like checking a box on your adulting checklist. You book it, pee in a cup, maybe give a blood sample, then wait for that clean confirmation: “Everything came back negative.”
But here’s the catch no one tells you when you Google “STD testing near me” at 2AM: not all infections are automatically included. In fact, some of the most common ones, like Herpes or Trichomoniasis, are deliberately excluded unless you explicitly request them. Others might not even be testable unless symptoms are present or unless the lab you chose offers it.
For Madi, that “clean panel” didn’t include Trichomoniasis. Her provider hadn’t even mentioned it. The test result said “comprehensive,” but it had left a few very common infections off the list, because many do.
STD Tests Don’t All Work the Same Way
There’s no such thing as a universal STD test, just a group of individual tests bundled together. That bundle might vary by provider, lab, location, or even insurance coverage. And if you’re using an at-home test kit? The accuracy and scope can change drastically between brands.
Think of it like ordering a combo meal: it looks complete, but unless you check the ingredients, you might miss that it comes without fries. Here’s a look at what’s typically included (and what’s often missing):
| STD | Included in Standard Panel? | Requires Special Request? | Why It’s Often Missed |
|---|---|---|---|
| Chlamydia | Yes | No | Core panel inclusion |
| Gonorrhea | Yes | No | Core panel inclusion |
| Syphilis | Sometimes | Yes | Often skipped in low-risk groups |
| HIV | Yes | No | Standard in most tests |
| Herpes (HSV-1/2) | No | Yes | Blood test has low predictive value if no symptoms |
| Trichomoniasis | Rarely | Yes | Typically symptom-triggered only |
| Mycoplasma genitalium | No | Yes | Newer test, limited availability |
Table 1: What’s in a standard STD panel, and what might be left out.
This reality means that even if you tested recently and got a clean bill of health, there are real gaps in that sense of security. And those gaps are how people like Madi fall through the cracks.
People are also reading: The Chlamydia Crisis: America’s Most Common STD Isn’t Going Away
The Herpes Loophole: Why It's Almost Never Automatically Tested
Here’s the wild part: Herpes is one of the most common sexually transmitted infections globally, and yet it’s not included in most “routine” STD tests. The CDC doesn’t recommend it for general screening unless symptoms are present or there’s a known exposure.
Why? Because herpes blood tests can detect antibodies but can’t tell you when you were infected or if it’s currently active. And false positives are not uncommon. The result is a lot of emotional distress over something that might have never caused symptoms in the first place.
But here’s the flip side: not testing doesn’t mean it’s not there. You could carry and transmit HSV-2 without knowing, especially if you’ve never had a recognizable outbreak.
For Alex, a 29-year-old queer man in Los Angeles, this was a hard lesson. After a sore appeared on his groin, he assumed it was a friction blister. His previous tests had all been clean. A clinic swab confirmed Herpes. The reaction? Anger, and confusion.
“I felt lied to by the system. I thought I was being safe and responsible.”
He wasn’t wrong to be upset. The system doesn’t always empower people with information about what tests they are, and aren’t, getting.
Timing Matters: The STD Window Period Problem
Even if you request every possible test, you’re still battling another invisible factor: time. Every infection has a “window period,” or the time between exposure and when a test can reliably detect it. Testing too early may yield a false negative, giving a false sense of security.
For example, a test taken 3 days after a risky encounter may not show any infection, even if one is brewing in your body. Depending on the type of test, the sensitivity, and the infection itself, you might need to wait a week, or even a month, for an accurate result.
| Infection | Minimum Detection Window | Best Time to Test |
|---|---|---|
| Chlamydia | 5–7 days | 14 days |
| Gonorrhea | 5–7 days | 14 days |
| Syphilis | 3 weeks | 6 weeks+ |
| HIV (4th gen) | 2–4 weeks | 4–6 weeks |
| Trichomoniasis | 5–28 days | 2–3 weeks |
| Herpes (HSV antibodies) | 4–6 weeks | 12–16 weeks |
Table 2: Window periods vs. best testing timelines.
Testing too early was exactly what happened to Carmen, who took an at-home test kit three days after a condom broke. Her test came back negative across the board. Two weeks later, painful urination sent her to urgent care, where a provider swabbed for Trichomoniasis. Positive.
The takeaway? You can’t fast-forward your way to a reliable result. Patience is uncomfortable, but essential.
Check Your STD Status in Minutes
Test at Home with Remedium6-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $119.00 $294.00
For all 6 tests
Marketing vs Reality: What “Comprehensive” Really Means
Many testing services, especially at-home STD kits, use the word “comprehensive” as a marketing term. But comprehensive doesn’t mean complete. It usually refers to a panel that includes Chlamydia, Gonorrhea, Syphilis, HIV, and sometimes Hepatitis B and Hepatitis C. That’s it.
Unless you specifically order expanded tests or select a kit labeled “14-panel” or “Full spectrum” (and even those vary), you’re likely missing common culprits like Herpes, Trichomoniasis, or Mycoplasma genitalium.
That’s how Ty, 33, got caught off guard. After a breakup, he ordered an at-home STD test kit from a well-reviewed brand. The sleek box, discreet shipping, and fast results felt empowering. The results? All negative.
But when a new partner mentioned they had tested positive for Mycoplasma genitalium, Ty asked his doctor about it. Turns out, his test hadn’t included it at all. The doctor didn’t blame him, but he did order a separate urine PCR. It came back positive.
“I felt dumb, honestly. Like I’d done all the right things, but still missed something huge.”
That’s the emotional cost of misleading simplicity. Good marketing should never substitute for transparent testing scopes. That’s why it’s so important to ask questions before you swab or submit your sample.
Do You Need to Test Again? Absolutely, Here’s Why
Testing isn’t a one-and-done moment. It’s a snapshot. If you’ve had new partners, experienced a condom failure, or started having symptoms, a retest is often warranted, even if your last results were clean. Especially if those results came back suspiciously fast or didn’t include the right infections.
Think of it this way: would you trust a security system that only monitored half your doors and windows? Testing should be tailored to your exposure history, your symptoms, and your peace of mind, not just what a basic kit provides.
Plus, symptoms can evolve. Some STDs, like Herpes, Trichomoniasis, or Syphilis, can lie low for weeks or even months before surfacing. That means today’s “all clear” could be tomorrow’s missed diagnosis.
If you’ve tested once and still feel off, or you just want certainty, retesting is not paranoia. It’s protection. It's agency. It's care.
This at-home combo STD test kit offers a broader range of detection than most “basic” options and ships discreetly anywhere in the U.S. Whether it’s reassurance or real-time answers, one retest could clear the confusion.
Trichomoniasis: The Most Skipped STD in America
Trichomoniasis, or “Trich,” infects an estimated 2 to 3 million Americans per year, and many don’t know they have it. It’s not deadly. It’s not talked about. And it’s almost never included in routine screening unless symptoms are present or requested.
This means millions may be walking around with a treatable but transmissible infection without ever being offered the test. Even more frustrating? Many clinics don’t offer a rapid test for it, only lab swabs, which must be processed offsite. And many at-home kits skip it entirely unless labeled as expanded.
In women and people with vaginas, Trich can cause foul-smelling discharge, itching, or burning. In men, it’s often silent, but can still be passed on. Testing involves a swab (or sometimes a urine sample), and treatment is a single antibiotic dose.
So why is it so frequently left out?
Stigma, lack of awareness, and outdated testing protocols. And unless patients push for it, most doctors won’t suggest it without symptoms, despite its high prevalence.
This makes Trich a textbook case of an “invisible infection.” One that doesn’t show up in your test results because it was never looked for in the first place.
Herpes Isn't Just Skin Deep, It’s Often Emotionally Overlooked
Beyond biology, Herpes carries a weight most other STDs don’t. There’s stigma. Panic. Shame. Even though the CDC estimates over 1 in 6 people have genital herpes, most people never know it, because they were never tested.
And if you do ask for a herpes test? You might face pushback. Many clinicians don’t want to screen asymptomatic people for it due to the chance of false positives and the emotional fallout that can come from a misunderstood result.
But here's the thing: that doesn’t mean the infection isn’t present. It just means the system has decided that not knowing is better than possibly overreacting to a borderline lab value. For people like Leila, that logic can feel deeply dismissive.
After getting what she thought was a yeast infection, Leila’s symptoms didn’t improve with OTC meds. Her primary care doctor insisted she didn’t “need” a herpes test unless there were sores. But she pushed, and eventually got an IgG blood test.
Positive for HSV-2.
“At least now I know,” she said. “That knowledge let me take control.”
Herpes is not the end of the world. But not knowing? That can feel like a betrayal of your autonomy. Especially when you thought you’d tested for everything.

People are also reading: Chlamydia Threatens More Than Just YouIt Endangers Your Baby Too
False Security: When “Negative” Isn’t the Same as Safe
There’s a dangerous quiet that follows a negative test result, especially when you’re sure you’ve covered all your bases. Relief floods in, and confidence rebounds. You go back to your life. Maybe you hook up again. Maybe you stop worrying. Until symptoms sneak in, or a partner shares news, or something just doesn’t feel right anymore.
That’s how Cassie found herself sitting in a Planned Parenthood clinic three weeks after celebrating a negative full panel from an at-home brand she’d seen on TikTok. Her only symptom was a new, almost chalky discharge. “Yeast?” she guessed. The clinician nodded, but swabbed her anyway, just in case.
Three days later, the call came: Trichomoniasis. Her test kit hadn’t included it.
And like many people in her position, Cassie felt a swirl of betrayal and shame. Not from her partners, but from the system. She’d followed the rules. She’d ordered the kit. She’d trusted the result.
We don’t talk enough about the emotional toll of believing you’re protected, only to learn you were testing blind. That sense of false security can lead to more risk, more unknowing transmission, and deeper feelings of disempowerment when the truth finally surfaces.
How to Ask for the Right Tests (Even If You’re Nervous)
Asking for expanded testing doesn’t mean you’re paranoid, it means you’re informed. But it can be intimidating, especially in clinical settings that rush appointments or assume your risk level without asking. Here’s how to start that conversation without spiraling into shame:
“Can you walk me through exactly which infections this panel tests for?”
“I’d like to make sure I’m screened for Herpes and Trichomoniasis. Can we add those?”
“Is Mycoplasma genitalium included in this test, or do I need to request it separately?”
These are not “extra” questions. They’re basic patient advocacy. If you’re using an at-home test, look for the test menu on the product page. If it’s not clearly listed, skip it. Transparency matters.
Some providers may still discourage certain tests (like Herpes) based on outdated guidance or fear of patient distress. But you have the right to know. To test. To treat. To disclose, or not, based on actual information, not assumption.
Check Your STD Status in Minutes
Test at Home with Remedium7-in-1 STD Test Kit

 For Men & Women
For Men & Women Results in Minutes
Results in Minutes No Lab Needed
No Lab Needed Private & Discreet
Private & DiscreetOrder Now $129.00 $343.00
For all 7 tests
What Real Comprehensive Testing Looks Like
If you want to make sure you're truly covered, your testing strategy needs to go beyond a checkbox or a single package. True comprehensive testing should ideally include:
• Core STDs: Chlamydia, Gonorrhea, Syphilis, HIV, Hepatitis B, Hepatitis C
• Commonly missed infections: Trichomoniasis, Herpes (HSV-1 & HSV-2), Mycoplasma genitalium
• Retesting windows: A plan for follow-up if tested too early after exposure
• Exposure-based customization: Adding or skipping based on your specific risk, symptoms, and partner history
This is where at-home kits like the Combo STD Home Test Kit can be helpful, if they’re clear about what’s included and when to use them. Always check whether tests are FDA-approved, what type of test is used (PCR vs antibody vs antigen), and whether they list window periods.
You shouldn’t have to guess. You shouldn’t have to Google for hours. A comprehensive approach should be designed with you in mind, not just lab protocols.
Case Closure: What Happened to Madi?
Back to Madi, the one who started this story. After texting a nurse through a telehealth app, she was advised to get a swab for Trichomoniasis. She went to a walk-in clinic that afternoon and told the provider that she’d had a full panel recently, but still had symptoms.
The provider nodded and said something she wouldn’t forget:
“A lot of these infections hide in the gaps. You did the right thing testing. Now let’s finish the job.”
Her swab was positive. She took the single-dose antibiotic that evening, let her partner know, and blocked off the weekend to rest, reflect, and reset. She also ordered a more complete test kit to use in a few weeks, just in case.
“I’m not mad at myself anymore,” she said. “I’m mad no one told me sooner.”
And that’s the reality of modern STD testing. Most of us assume it’s one simple step. But real sexual health care? It’s a series of conversations, retests, and honest check-ins with your body and your exposure. That’s how you stay empowered. Not by assuming you’re clean, but by knowing exactly what you were tested for, when, and what that really means.
FAQs
1. Wait, so my “full panel” might not have included everything?
Yup. That’s the part no one tells you. Most “full panels” only cover the basics: Chlamydia, Gonorrhea, maybe HIV and Syphilis. If you didn’t specifically ask for Herpes or Trichomoniasis, chances are they weren’t even on the radar.
2. Why would they leave out something like Herpes?
Because Herpes is messy, testing-wise and emotionally. The blood test can’t tell when you got it, and false positives happen. So many doctors won’t test unless you’re showing sores. But that doesn’t mean you’re in the clear. It just means no one looked.
3. I tested negative, but I still feel weird down there. Am I just being paranoid?
Nope, you’re listening to your body. That’s smart. If something feels off, itching, discharge, weird timing, it’s worth a retest. Some infections don’t show up right away, and others aren’t covered in routine screening at all. Trust your gut over the paperwork.
4. Can I get an STD even if we used a condom?
Unfortunately, yes. Condoms are great at reducing risk, but not all STDs play by the same rules. Herpes, HPV, and even Syphilis can spread through skin-to-skin contact outside the condom zone. And oral sex? That’s a whole other gateway.
5. Is Trichomoniasis really that common?
More than you'd think. It affects millions, mostly women and people with vaginas, but it’s wildly underdiagnosed because many folks don’t show symptoms, and routine panels skip it. One little protozoan, big sneaky impact.
6. My doctor didn’t even mention half these tests. What gives?
Doctors are humans too, and some follow outdated guidelines, make assumptions about your risk, or simply don’t have access to certain tests. That’s why being your own advocate matters. Asking isn’t rude. It’s responsible.
7. How long should I wait after exposure to get tested?
Depends on the infection. Some show up in tests after 5–7 days, others (like Syphilis or Herpes) might take weeks. If you test early, you might need to test again later. One-and-done is a myth, testing is a process.
8. What is Mycoplasma genitalium and do I need to worry about it?
It’s a mouthful and a menace. Mycoplasma genitalium is a lesser-known STD that’s been linked to pelvic pain and urethritis. It’s often silent, not usually tested for, and becoming more antibiotic-resistant. If you’re symptomatic and your usual tests came back clean, it’s worth asking about.
9. Should I test again even if nothing hurts?
If you’ve had a new partner, a broken condom, or you just feel unsure, yes. Many STDs have no symptoms at all. Peace of mind is priceless, and way better than waiting until something *does* hurt.
10. How do I bring this up with a partner without freaking them out?
Try honesty with a side of chill: “Hey, I tested recently but just found out it didn’t include everything. I’m getting a follow-up test, maybe we both should.” It’s not a confession. It’s a collaboration. You’re not dirty, you’re informed.
You Deserve Answers, Not Assumptions
You did the right thing. You got tested. But if you’re reading this, you might also feel confused, let down, or blindsided by a positive result, or by new symptoms despite a “clean” panel. That doesn’t mean you failed. It means the system didn’t give you the full picture.
Don’t wait and wonder, get the clarity you deserve. This at-home combo test kit checks for the most common STDs discreetly and quickly. It includes the infections most standard kits skip, and gives you the power to know for sure.
How We Sourced This Article: We combined current guidance from leading medical organizations with peer-reviewed research and lived-experience reporting to make this guide practical, compassionate, and accurate.
Sources
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a no-nonsense, sex-positive approach and is committed to expanding access for readers in both urban and off-grid settings.
Reviewed by: Dr. Kara Jenkins, MPH | Last medically reviewed: September 2025
This article is for informational purposes and does not replace medical advice.